Professional Documents
Culture Documents
Objectives:: Clinical Relevance of MYC, BCL2 and BCL6 Rearrangements and Amplification in Diffuse Large B-Cell Lymphoma
Objectives:: Clinical Relevance of MYC, BCL2 and BCL6 Rearrangements and Amplification in Diffuse Large B-Cell Lymphoma
Uploaded by
Eddie CaptainOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Objectives:: Clinical Relevance of MYC, BCL2 and BCL6 Rearrangements and Amplification in Diffuse Large B-Cell Lymphoma
Objectives:: Clinical Relevance of MYC, BCL2 and BCL6 Rearrangements and Amplification in Diffuse Large B-Cell Lymphoma
Uploaded by
Eddie CaptainCopyright:
Available Formats
Clinical Relevance of MYC, BCL2 and BCL6 Rearrangements
and Amplification in Diffuse Large B-cell Lymphoma
GC Caponetti1, BJ Dave2, L Smith2, M Bast2, P Meyer2, P Bierman2, G Bociek2, J Vose2, J Armitage2, K Fu2, P Aoun3, TC Greiner2, WC Chan2 and DD Weisenburger3.
Creighton University Medical Center, Omaha, NE, USA; 2University of Nebraska Medical Center, Omaha, NE, USA; 3City of Hope National Medical Center, Duarte, CA, USA.
Objectives: The highly-variable clinical outcome seen in patients with diffuse large B-cell lymphoma (DLBCL) may be
due, at least in part, to various genetic abnormalities. BCL2 and BCL6 are often rearranged in DLBCL, and about 10% of
cases have rearrangement of MYC. These oncogenes play an important pathogenic role in DLBCL, and simultaneous
rearrangement or amplification of MYC, along with BCL2 and/or BCL6 (double hit) may have a synergistic effect leading
to poor survival. To test this hypothesis, we performed a retrospective analysis of DLBCL cases tested for translocations
and amplifications involving MYC, BCL2 and BCL6, and treated with CHOP- or R-CHOP-like therapies.
Methods:
We searched the database of the Nebraska Lymphoma Study Group for cases of de novo DLBCL with
available clinical data, patient consent, no prior treatment, and available conventional cytogenetics (CC) and/or FISH
results. Patients with a history of HIV infection or organ transplantation were excluded. CC and/or FISH reports were
reviewed to identify rearrangements of MYC, BCL2, and BCL6. Cases were classified into three groups according to the
rearrangement or amplification status of these three genes: 1) MYC- (with or without BCL2 or BCL6 rearrangement or
amplification); 2) MYC+/BCL2-/BCL6- or BCL6 unknown; and 3) MYC+/BCL2+ or BCL6+. A gene was considered
amplified if four or more copies were identified by FISH. The 5-year overall survival (OS) and event-free survival (EFS)
of the three groups were then compared.
1.0
0.9
0.8
|
|
MYCMYC+/BCL2-/BCL6MYC+/BCL2+ or BCL6+
| |
0.7
|
0.6
||
|
0.5
||
| |
Event-free Survival(%)
|
|
|
| |
| || |
0.4
|||
||
0.3
|| |
|
| | ||
0.2
|
|| |
||
|
0.1
||
0.8
|
|
0.7
0.6
10
Years
15
| |
20
0.5
0.4
| ||
| ||
| ||
0.3
| ||
| |
|| |
|
0.2
| | | |
|
||
||
Years
|
0.6
|
0.5
15
0.4
|
0.3
|
0.2
|
0.1
0.8
|
0.7
0.6
Test: p=0.023
0
10
Years
15
20
0.5
0.4
0.3
0.2
|
|
Test: p=0.0059
0.0
5
MYC+/BCL2-/BCL6MYC+/BCL2+ or BCL6+
| |
0.1
20
0.9
MYC+/BCL2-/BCL6MYC+/BCL2+ or BCL6+
| |
0.7
0.0
10
Test: p=0.010
0
0.8
|
|
0.0
5
0.9
MYCMYC+/BCL2-/BCL6MYC+/BCL2+ or BCL6+
0.1
Test: p=0.094
0.0
||
|
|
|
|
0.9
Overall Survival (%)
|
|
1.0
Event-free Survival(%)
1.0 |
1.0
Overall Survival (%)
10
15
Years
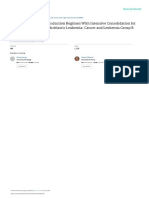
Figure 1 . Overall survival (A and C) and event-free survival (B and D) of patients with DLBCL according to the presence
or absence of rearrangement or amplification of the MYC, BCL2 and BCL6 genes.
Results: We identified 212 cases of DLBCL that met the study criteria, with a male to female ratio of 1:1 and a median
age of 67 years at diagnosis (range, 20-90 years). Based on the rearrangement and amplification status of the three
genes, 178 cases (85%) were classified as MYC- and had a 5-year OS of 47% and EFS of 38%; 17 cases (8%) were
MYC+/BCL2-/BCL6- or BCL6 unknown and had a 5-year OS of 76% and EFS of 71%; and 17 cases (8%) had a double
hit (MYC+/BCL2+ or BCL6+) with a 5-year OS of only 29% and EFS of 12%. No significant differences in clinical
characteristics were identified among these groups. However, a decreased complete remission rate (p=0.091) and
worse OS (p=0.064) and EFS (p=0.011) were found among double hit cases with MYC+/BCL2+ or BCL6+.
Conclusions:
MYC+ DLBCL cases without BCL2 or BCL6 rearrangements or amplification do not have a worse
survival when compared to cases without MYC abnormalities. However, MYC+ DLBCL cases with either BCL2 or BCL6
abnormalities have a poor clinical outcome and should be treated with aggressive or novel therapies.
20
You might also like
- Problem Solving in RheumatologyDocument293 pagesProblem Solving in RheumatologyGaudeamus IgiturNo ratings yet
- LinfomaDocument9 pagesLinfomaRocio HaroNo ratings yet
- Fphar 09 01497Document11 pagesFphar 09 01497Atina IraniNo ratings yet
- Research PaperDocument14 pagesResearch PaperlilisNo ratings yet
- PBC 24420Document7 pagesPBC 24420Nachapol JatNo ratings yet
- Leucemia GenomicaDocument14 pagesLeucemia GenomicaNathalie Soler BarreraNo ratings yet
- Gabriel Caponetti Et Al. - Clinical Significance of C-MYC Rearrangement in Diffuse Large B-Cell Lymphoma - Poster For USCAP 2011Document1 pageGabriel Caponetti Et Al. - Clinical Significance of C-MYC Rearrangement in Diffuse Large B-Cell Lymphoma - Poster For USCAP 2011Eddie CaptainNo ratings yet
- 1 s2.0 S0006497119353972 MainDocument3 pages1 s2.0 S0006497119353972 Mainmiltoncaballero5No ratings yet
- MR 25Document9 pagesMR 25Riko JumattullahNo ratings yet
- JCM 08 01175 v2 PDFDocument28 pagesJCM 08 01175 v2 PDFAs'har AnwarNo ratings yet
- Prognostic Factors For Chronic Lymphocytic LeukemiaDocument6 pagesPrognostic Factors For Chronic Lymphocytic LeukemiaJose AbadiaNo ratings yet
- How I Treat Double-Hit Lymphoma 2Document7 pagesHow I Treat Double-Hit Lymphoma 2abdul qayyumNo ratings yet
- Wall 2016Document15 pagesWall 2016Jose AbadiaNo ratings yet
- Mixed Phenotype Acute LeukemiaDocument10 pagesMixed Phenotype Acute LeukemiaMarco Aurélio SartoriNo ratings yet
- Multiparametric Flow Cytometry in Mixed Phenotype Acute LeukemiaDocument8 pagesMultiparametric Flow Cytometry in Mixed Phenotype Acute LeukemiaBhargav YagnikNo ratings yet
- How I Treat Newly Diagnosed Chronic Phase CMLDocument9 pagesHow I Treat Newly Diagnosed Chronic Phase CMLDenisse SarabiaNo ratings yet
- ZH 800607002314Document8 pagesZH 800607002314ekanovicaNo ratings yet
- Bosch2019 PDFDocument18 pagesBosch2019 PDFlengers poworNo ratings yet
- Reviews: Chronic Lymphocytic Leukaemia: From Genetics To TreatmentDocument18 pagesReviews: Chronic Lymphocytic Leukaemia: From Genetics To Treatmentlengers poworNo ratings yet
- Pages 4 7Document4 pagesPages 4 7andreas_251650No ratings yet
- Article Ang3Document9 pagesArticle Ang3Ayoub HajjarNo ratings yet
- Synchronous Presence of Chronic Lymphocytic Leukaemia and Breast Cancer in Nigerian Adult Females Case SeriesDocument5 pagesSynchronous Presence of Chronic Lymphocytic Leukaemia and Breast Cancer in Nigerian Adult Females Case SeriesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Associatio of SNP Rs5069 in APOA1 With Benign Breast Diseases in A Mexican PopulationDocument8 pagesAssociatio of SNP Rs5069 in APOA1 With Benign Breast Diseases in A Mexican PopulationRushali MoreNo ratings yet
- La Mellarin D2Document2 pagesLa Mellarin D2JESUS DAVID BOLA‹O JIMENEZNo ratings yet
- Chronic Lymphocytic Leukemia: A Clinical and Molecular Heterogenous DiseaseDocument14 pagesChronic Lymphocytic Leukemia: A Clinical and Molecular Heterogenous DiseaseCallisthenisLeventisNo ratings yet
- Gribben, 2011 AlemtDocument7 pagesGribben, 2011 AlemtveraffulNo ratings yet
- Regular ArticleDocument11 pagesRegular ArticleOmar FernándezNo ratings yet
- Parik H 2016Document35 pagesParik H 2016Jose Angel AbadíaNo ratings yet
- Regimen Calgb 8811Document14 pagesRegimen Calgb 8811ricardo_cheNo ratings yet
- Zeng 2016Document7 pagesZeng 2016Thanasis PapatheodorouNo ratings yet
- Review Article WHO Classification of Tumors of Hematopoietic and Lymphoid Tissues 4th EditionDocument8 pagesReview Article WHO Classification of Tumors of Hematopoietic and Lymphoid Tissues 4th EditionCat NhanNo ratings yet
- Non-Hodgkin Lymphoma of The Breast: MD MD MD PHD MDDocument6 pagesNon-Hodgkin Lymphoma of The Breast: MD MD MD PHD MDlPiNGUSlNo ratings yet
- 2016 Article 70Document8 pages2016 Article 70sawantleena62No ratings yet
- Rodrguez Vicente 2013Document14 pagesRodrguez Vicente 2013Jose AbadiaNo ratings yet
- 1548 FullDocument13 pages1548 FullsabarinaramNo ratings yet
- Ghalesardi 2021Document9 pagesGhalesardi 2021Riyadh Z. MawloodNo ratings yet
- Treatment of Infant Leukemias Challenge and PromiseDocument5 pagesTreatment of Infant Leukemias Challenge and PromiseSyifa SariNo ratings yet
- Paper Comparativa Sobrevida de PV, TE y MFPDocument7 pagesPaper Comparativa Sobrevida de PV, TE y MFPDani HaindlNo ratings yet
- Basophil-Biomarker-Fibrosis - PMF 2018Document8 pagesBasophil-Biomarker-Fibrosis - PMF 2018Banchob SripaNo ratings yet
- Revista de Mieloma MultipleDocument7 pagesRevista de Mieloma MultiplelevydarkNo ratings yet
- DHH-RHEBL1 Fusion Transcript A Novel Recurrent AML Ricardo, 2013Document9 pagesDHH-RHEBL1 Fusion Transcript A Novel Recurrent AML Ricardo, 2013mrkhprojectNo ratings yet
- A Case Report of Pediatric Acute Lymphoblastic Leukemia With E8a2 BCR/ABL1 Fusion TranscriptDocument6 pagesA Case Report of Pediatric Acute Lymphoblastic Leukemia With E8a2 BCR/ABL1 Fusion TranscriptArdiles Robinson Rohi LagaNo ratings yet
- 179 227 1 SMDocument5 pages179 227 1 SMRadinal MauludiNo ratings yet
- Adult Acute Lymphoblastic Leukemia: Concepts and StrategiesDocument12 pagesAdult Acute Lymphoblastic Leukemia: Concepts and StrategiesdrravesNo ratings yet
- Ol 27 2 14210 PDFDocument11 pagesOl 27 2 14210 PDFafzaahmad212No ratings yet
- Citometria 2005Document8 pagesCitometria 2005Leslie AraujoNo ratings yet
- From The Experts: How I Treat Older Patients With Acute Myeloid LeukemiaDocument12 pagesFrom The Experts: How I Treat Older Patients With Acute Myeloid LeukemiaWillyPeñaNo ratings yet
- Acute Lymphoblastic Leukemia in Children and Adolescents: Prognostic Factors and Analysis of SurvivalDocument7 pagesAcute Lymphoblastic Leukemia in Children and Adolescents: Prognostic Factors and Analysis of SurvivalAbdurrahman HasanuddinNo ratings yet
- Pediatric Blood Cancer - 2023 - Abstracts From The 39th Annual Meeting of The Histiocyte SocietyDocument64 pagesPediatric Blood Cancer - 2023 - Abstracts From The 39th Annual Meeting of The Histiocyte SocietySeham GoharNo ratings yet
- Cho Et Al-2019-International Journal of CancerDocument12 pagesCho Et Al-2019-International Journal of Cancerlouisehip UFCNo ratings yet
- Study of Correlation Between Imatinib Mesylate Plasma-LinkDocument7 pagesStudy of Correlation Between Imatinib Mesylate Plasma-LinkIvonne Mercedes Gutierrez AtapaucarNo ratings yet
- BR J Haematol - 2016 - Kritharis - How I ManageDocument6 pagesBR J Haematol - 2016 - Kritharis - How I ManageMarco Aurélio SartoriNo ratings yet
- A Study On Tuberculosis in Elderly Patients: Medical OfficerDocument5 pagesA Study On Tuberculosis in Elderly Patients: Medical OfficerJoan FloRevzNo ratings yet
- INFLAMMATORY Breast CancerDocument20 pagesINFLAMMATORY Breast CancerbencleeseNo ratings yet
- Central Nervous Disease in Pediatric Patients LLADocument5 pagesCentral Nervous Disease in Pediatric Patients LLAlaura rangelNo ratings yet
- Article AngDocument12 pagesArticle AngAyoub HajjarNo ratings yet
- Relapsed Acute Myeloid Leukemia in Children and Adolescents: Current Treatment Options and Future StrategiesDocument10 pagesRelapsed Acute Myeloid Leukemia in Children and Adolescents: Current Treatment Options and Future StrategiesYo MeNo ratings yet
- Acute Lymphoblastic Leukemia in Adolescent and Young AdultsDocument27 pagesAcute Lymphoblastic Leukemia in Adolescent and Young AdultsKarol CriscuoloNo ratings yet
- General Medicine: Open AccessDocument6 pagesGeneral Medicine: Open AccesssnNo ratings yet
- Cancer de ColonDocument7 pagesCancer de ColonAlex MoraNo ratings yet
- Demystifying The Diagnosis and Classification of Lymphoma - Gabriel C. Caponetti, Adam BaggDocument6 pagesDemystifying The Diagnosis and Classification of Lymphoma - Gabriel C. Caponetti, Adam BaggEddie CaptainNo ratings yet
- Gabriel Caponetti Et Al. - Clinical Significance of C-MYC Rearrangement in Diffuse Large B-Cell Lymphoma - Poster For USCAP 2011Document1 pageGabriel Caponetti Et Al. - Clinical Significance of C-MYC Rearrangement in Diffuse Large B-Cell Lymphoma - Poster For USCAP 2011Eddie CaptainNo ratings yet
- Gabriel Caponetti Et Al. - Utility of Immunohistochemistry To Diagnose Cat Scratch Disease - Poster For USCAP 2007Document1 pageGabriel Caponetti Et Al. - Utility of Immunohistochemistry To Diagnose Cat Scratch Disease - Poster For USCAP 2007Eddie CaptainNo ratings yet
- Detection of The BRAF c.1799T A (V600E) Mutation in MelanomaDocument1 pageDetection of The BRAF c.1799T A (V600E) Mutation in MelanomaEddie CaptainNo ratings yet
- Detection of The BRAF c.1799T A (V600E) Mutation in MelanomaDocument1 pageDetection of The BRAF c.1799T A (V600E) Mutation in MelanomaEddie CaptainNo ratings yet
- CBSE Class 9 Science Worksheet - Fundamental Unit of LifeDocument2 pagesCBSE Class 9 Science Worksheet - Fundamental Unit of LifeThe Shikshak100% (2)
- Nurs 3020 Clinical EvaluationDocument14 pagesNurs 3020 Clinical Evaluationapi-456466614No ratings yet
- Molecules, of The Immune SystemDocument39 pagesMolecules, of The Immune SystemFaith MbasaniNo ratings yet
- Cracking Cancer Toolkit Slides June 19 Jeffrey Dach Mitch Ghen 2021 AA2Document97 pagesCracking Cancer Toolkit Slides June 19 Jeffrey Dach Mitch Ghen 2021 AA2André Amorim67% (3)
- The Best Brain FoodDocument3 pagesThe Best Brain Foodanima1982No ratings yet
- Biology 2019Document12 pagesBiology 2019Jyoti RaniNo ratings yet
- Common Tests During PregnancyDocument7 pagesCommon Tests During Pregnancyrraja2k2No ratings yet
- Chorea Curs CompletDocument101 pagesChorea Curs CompletMarian GeorgeNo ratings yet
- 3edited My Class Note 1 On Blood BankDocument46 pages3edited My Class Note 1 On Blood BankmatewosNo ratings yet
- Reading Questions AP PsychDocument56 pagesReading Questions AP Psychasomisetty11No ratings yet
- Acceptance Letter CsuDocument3 pagesAcceptance Letter CsuRufaq UllahNo ratings yet
- Liver Function Tests: When Should Lfts Be Ordered? What Do The Results Mean?Document3 pagesLiver Function Tests: When Should Lfts Be Ordered? What Do The Results Mean?Anbaraj ArunNo ratings yet
- Lee CV PDFDocument33 pagesLee CV PDFAnonymous 2g7jW7No ratings yet
- IT.12 (YUL) - Male HypogonadismDocument23 pagesIT.12 (YUL) - Male HypogonadismMikhael JHNo ratings yet
- Khusbu Keyal 2017 PDFDocument10 pagesKhusbu Keyal 2017 PDFFelicia SutarliNo ratings yet
- Tuberculinum PDFDocument4 pagesTuberculinum PDFadi swara100% (1)
- Medallion: Congratulations 2013 Honors GraduatesDocument8 pagesMedallion: Congratulations 2013 Honors GraduatesjamwilljamwillNo ratings yet
- Genetic Engineering MindmapDocument1 pageGenetic Engineering Mindmapgihan1mohamed1ahmedNo ratings yet
- Olfactory Nerve - WikipediaDocument29 pagesOlfactory Nerve - Wikipediaراوند اعبيدNo ratings yet
- General Principles of Cell OrganisationDocument3 pagesGeneral Principles of Cell Organisation22194No ratings yet
- Jurnal 4 - Kasus SimpleDocument12 pagesJurnal 4 - Kasus SimpleKurnia SelaNo ratings yet
- History and Development of Antimicrobial Susceptibility Testing MethodologyDocument7 pagesHistory and Development of Antimicrobial Susceptibility Testing MethodologyTogu NaiposposNo ratings yet
- MCQ Breeding and Farm AnimalsDocument10 pagesMCQ Breeding and Farm AnimalsvishnuNo ratings yet
- ADPKDDocument75 pagesADPKDVenkataramanan KrishnamoorthyNo ratings yet
- g6pd Group 5 A2Document39 pagesg6pd Group 5 A2Kristian CadaNo ratings yet
- Cloning Lesson For High School ClassesDocument9 pagesCloning Lesson For High School Classesmartin pontNo ratings yet
- Trisomie 21 AnglaisDocument34 pagesTrisomie 21 AnglaisKatia Hareb-CherfaouiNo ratings yet
- Lab Manual GeneticsDocument15 pagesLab Manual Geneticsapi-319985329100% (1)
- Chemistry Class 12 Chemical Kinetics ProjectDocument11 pagesChemistry Class 12 Chemical Kinetics ProjectNich TeniNo ratings yet