Professional Documents
Culture Documents
Genetic Aspect of Growth and Puberty
Genetic Aspect of Growth and Puberty
Uploaded by
Chesy Viviandra0 ratings0% found this document useful (0 votes)
24 views34 pagesThis document discusses the genetic factors that influence human growth and puberty. It covers several key points:
1) Height is highly influenced by genetics, with heritability estimated at 60-80%. Hundreds of genetic syndromes are associated with abnormal growth.
2) Mutations in genes involved in the somatotropic axis like GH, its receptor, and transcription factors can cause short stature. Bone growth genes like FGFR3 and COL1A1 can also be mutated.
3) The SHOX gene on the X and Y chromosomes is frequently involved in growth disorders like Langer syndrome, Turner syndrome, and idiopathic short stature due to mutations or deletions.
4
Original Description:
Original Title
genetic aspect of growth and puberty.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses the genetic factors that influence human growth and puberty. It covers several key points:
1) Height is highly influenced by genetics, with heritability estimated at 60-80%. Hundreds of genetic syndromes are associated with abnormal growth.
2) Mutations in genes involved in the somatotropic axis like GH, its receptor, and transcription factors can cause short stature. Bone growth genes like FGFR3 and COL1A1 can also be mutated.
3) The SHOX gene on the X and Y chromosomes is frequently involved in growth disorders like Langer syndrome, Turner syndrome, and idiopathic short stature due to mutations or deletions.
4
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
24 views34 pagesGenetic Aspect of Growth and Puberty
Genetic Aspect of Growth and Puberty
Uploaded by
Chesy ViviandraThis document discusses the genetic factors that influence human growth and puberty. It covers several key points:
1) Height is highly influenced by genetics, with heritability estimated at 60-80%. Hundreds of genetic syndromes are associated with abnormal growth.
2) Mutations in genes involved in the somatotropic axis like GH, its receptor, and transcription factors can cause short stature. Bone growth genes like FGFR3 and COL1A1 can also be mutated.
3) The SHOX gene on the X and Y chromosomes is frequently involved in growth disorders like Langer syndrome, Turner syndrome, and idiopathic short stature due to mutations or deletions.
4
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 34
The genetic aspect
of growth and puberty
dr. Yulia Ariani, Sp.A
Departemen Biologi Kedoktera FKUI
Growth
• Growth : gain of body weight (BW), body
height (BH), or head circumference (HC)
• Growth is influenced by environment and
genetic factors
• Body height is highly heritable high genetic
contribution, polygenic and multifactorial
• Heritability index for BH 0,6 – 0,8
A genetic map of the genes affecting height.
• Hundreds of syndrome in OMIM (Online
Mendelian Inheritance in Men) registry are
associated with growth disturbance
• Most cases are delayed growth due to
endocrine abnormality and linked to growth
hormone (GH) deficiency (isolated or combine
with other hypophyseal hormone deficiencies)
or with a lack of activity
Genes
• Mutations of genes expressed along the
somatotropic axis (GH coding gene, its
receptor, etc) and transcription factors
(HESX1, LHX3, LHX4, PROP1, POU1F1, SOX3,
SOX2, etc)
• Mutation of genes involved in bone formation
(FGFR3, COLI-A1)
• Anomalies of SHOX gene, located in sex
chromosome most frequent
SHOX gene
• SHOX gene is located at the tip of both sex
chromosome inside the telomeric part of
pseudoautosomal region I (PAR I) which
comprises around 2,6Mb
• There is no difference between SHOX (X) dan
SHOX (Y)
• This region is a hotspot for very frequent
recombination events
• SHOX gene function is dosage dependent
loss of function of one SHOX allele growth
failure
SHOX gene abnormality
• Idiopathic short stature
• Turner syndrome
Idiopathic short stature
• Loss of function of one SHOX allele due to
mutation
• Most frequent is deletion of SHOX gene in a
different size account for around 80% of all
mutations
• Prevalence of SHOX mutations in children with
idiopathic short stature is estimated around 2
– 15%
Turner syndrome
• Turner syndrome (TS) is almost always
associated with the loss of one SHOX gene
because of the numerical or structural
aberration of the X chromosome
• female with absence of one X chromosome
Incidence: 1 in 1200 – 2500 females (90% of
them undergo spontaneous abortion)
• Short stature (57 inches average)
• Hormone therapy may increase height
- Intelligence is often near average, although with severe
deficits in spatial ability and directional sense (perhaps
due to smaller amounts of brain tissue — grey & white
matter in parietal lobes; Reiss, 1995).
• Loss of both SHOX alleles causes complete
lack of SHOX and extreme phenotype called
Lange syndrome
• The gain of 1 or 2 additional copies of SHOX
due to structural abberations can be asociated
with tall stature
Severe growth anomalies
• On going studies
• Genes are responsible: LH-β (β-Luteinizing
Hormone), COLI A1(Collagen I A1), VDR (Vitamin
D Receptor), ESR1 (Estrogen Receptor 1), DRD2
(Dopamine Receptor D2), IGF-1 (Insulin-like
Growth Factor 1), CYP17 (Cytochrome P450c17a),
CYP19 (Aromatase), Y chromosome, PTHR1
(PTH/PTHrP Receptor), GH1 (Growth Hormone 1),
PPARγ (Peroxisome Proliferator-Activated
Receptor-γ)
Puberty
• Puberty corresponds to the activation of the
hypothalamo-hypophyseal-gonadal function
full development of sexual characteristics,
final height, reproductive function and fertility
• Stages in pubertal were classified according
Tanner classification, focussing on secondary
sexual characterisrics
• First sign of puberty in girls is the
development of breast glands
• Average age 10,5-11 y.o
• Followed by the growth of pubic and axillary
hair
• Ends by the occurrence of menarche, around
the age of 13 (2-2,5 years after the first sign of
puberty) mean 10 – 15,5 y.o
• First sign of puberty in boys is an increase in
the volume of the testicles in average
occurs between 12-13 years of age
• Followed by the growth of pubic and axillary
hair, increase in the size of glans penis
• Genetics factors have contribution in the
occurrence of puberty and determine the age
of onset of puberty
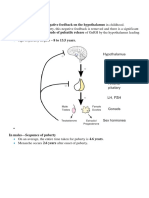
• Puberty depends of the reactivation of
gonadotropic axis (around 7-8 years of age)
• The absence of reactivation of this
reactivation is responsible for the delayed
puberty or even the complete absence of
puberty
• Acceleration of this reactivation is responsible
for precocious puberty
• It is now established that the onset of puberty is
determined by the events that take place in the
brain leads to a synchronized increase of GnRH
in hypothalamus
• The secretion of GnRH stimulates the synthesis
and release of LH and FSH
• LH and FSH reach the gonad and regulate gonad
development and secretion on gonad steroids
promote the growth of secondary sex hormone
and trigger the onset of sexual dimorphisms
(distribution of fats, muscle mass, breast
development, tone, voice)
Turner syndrome
• Sometimes is undetectable until puberty, as
secondary sex characteristics and menstruation
are not appearing
• Ovaries (gonad) do not develop prenatally leads
to high level of FSH and LH in early childhood
hypergonadrotropic hypogonadism
• Hormone therapy may induce menstruation
nevertheless it does not work for pregnancy
purpose
Kallmann syndrome
• KS is a combination of congenital hypogonadrotropic
hypogonadism disorder and decrease/absent sense of
smell (anosmia)
• Caused by disturbance of intrauterine migration of GnRH
neurons from the olfactory placodes to hypothalamus
insufficient/absent of GnRH insufficient of FSH/LH
hypogonadism
• Clinically and genetically heterogenous, most cases are
sporadic (60%)
• Genes involved are vary
• In familial cases mode of inheritance is vary (autosomal
recessive, autosomal dominant, X-linked recessive,
oligogenic)
KS genes
• KAL1 ???
• FGFR1 in 10% - 30% of KS cases
• FGF8
• PROK2
• PROKR2
• WDR11
KAL 1 gene FGFR 1 gene
You might also like
- MeningitisDocument9 pagesMeningitisNader Smadi88% (8)
- Advice Sheet A12 - Infection Control in Dentistry - Identist - 2 PDFDocument31 pagesAdvice Sheet A12 - Infection Control in Dentistry - Identist - 2 PDFizeldien5870No ratings yet
- Luise Hay Symptoms ListDocument12 pagesLuise Hay Symptoms Listmaviladin100% (2)
- Hahn, R. 1995. Sickness and Healing - An Anthropological Perspective. Chap 4 - The Role of Society and Culture in Sickness and HealingDocument24 pagesHahn, R. 1995. Sickness and Healing - An Anthropological Perspective. Chap 4 - The Role of Society and Culture in Sickness and HealingJenny Gill67% (3)
- Neurology Fam Med CiricullumDocument381 pagesNeurology Fam Med CiricullumbajariaaNo ratings yet
- Common Genetic DisordersDocument44 pagesCommon Genetic DisordersHamza Ali50% (2)
- Aditiawati - No Signs of Puberty PDFDocument43 pagesAditiawati - No Signs of Puberty PDFJayantiNo ratings yet
- PubertyDocument50 pagesPubertyDeepanshu KumarNo ratings yet
- Approach To Delay PubertyDocument33 pagesApproach To Delay PubertyRaja Iqbal Mulya HarahapNo ratings yet
- Sexuality and IntersexualityDocument23 pagesSexuality and IntersexualityManu BharadwazNo ratings yet
- Endo Part IVDocument40 pagesEndo Part IVChippy RabeNo ratings yet
- Dian Ais EditDocument41 pagesDian Ais EditDian SiregarNo ratings yet
- Disorder of Determination and Sex DifferentiationDocument62 pagesDisorder of Determination and Sex DifferentiationSYAFIRA INAYAHNo ratings yet
- Reproduction Block (Puberty) Khairun Nisa Bagian Fisiologi FK Unila 216Document28 pagesReproduction Block (Puberty) Khairun Nisa Bagian Fisiologi FK Unila 216Redina AndiniNo ratings yet
- Pubertal Disorders LectureDocument60 pagesPubertal Disorders LectureRawabi rawabi1997No ratings yet
- Growth Hormone DeficiencyDocument11 pagesGrowth Hormone DeficiencyIgor VasićNo ratings yet
- Mendelian Genetics in ManDocument33 pagesMendelian Genetics in ManIndian Military Academy, DehradunNo ratings yet
- Lec 1Document9 pagesLec 1ardevanaNo ratings yet
- Hypogonadotropic Hypogonadism: Lawrence C. Layman, MDDocument14 pagesHypogonadotropic Hypogonadism: Lawrence C. Layman, MDPrasanth VargheseNo ratings yet
- Disorders of PubertyDocument28 pagesDisorders of PubertySujit KoiralaNo ratings yet
- 8-Acromegaly & DwarfismDocument79 pages8-Acromegaly & DwarfismsweyamkulimaNo ratings yet
- Pemicu 3: Siklus Hidup 2014Document54 pagesPemicu 3: Siklus Hidup 2014exxxxooooNo ratings yet
- Alternative Mechanisms of Signal Transduction: The Cellular and Molecular Basis of DevelopmentDocument32 pagesAlternative Mechanisms of Signal Transduction: The Cellular and Molecular Basis of DevelopmentDon MARSHALNo ratings yet
- Puberty: Dr. Valérie M. SchwitzgebelDocument66 pagesPuberty: Dr. Valérie M. SchwitzgebelJoshua RomeroNo ratings yet
- Puberty PDFDocument66 pagesPuberty PDFnenyNo ratings yet
- Puberty PDFDocument66 pagesPuberty PDFnenyNo ratings yet
- Puberty: Dr. Valérie M. SchwitzgebelDocument66 pagesPuberty: Dr. Valérie M. SchwitzgebelnenyNo ratings yet
- Human Disease Genes or Human Genetic DiseaseDocument23 pagesHuman Disease Genes or Human Genetic Diseasebalkrishn joshiNo ratings yet
- Genetics Mendelian Disorder Three (Autosaved)Document87 pagesGenetics Mendelian Disorder Three (Autosaved)OROKE JOHN EJENo ratings yet
- Amenorrhea WilliamsDocument26 pagesAmenorrhea WilliamsGregorius Juan GunawanNo ratings yet
- Pediatrics - Endocrine System (Part1)Document150 pagesPediatrics - Endocrine System (Part1)Gen XNo ratings yet
- Inheritance of Autosomal Dominant and XlinkedDocument43 pagesInheritance of Autosomal Dominant and XlinkedBabak NamiNo ratings yet
- Biochemical Investigation of Infertile Couple-My PresentationDocument91 pagesBiochemical Investigation of Infertile Couple-My PresentationOlukoyejo OluwaboriNo ratings yet
- HypogonadismDocument37 pagesHypogonadismCristy BelleNo ratings yet
- Approach To Short StatureDocument71 pagesApproach To Short StatureOmar HamwiNo ratings yet
- 2 - Fragile X SyndromeDocument4 pages2 - Fragile X Syndromechenelyn_15No ratings yet
- Genetic & Deve PathDocument9 pagesGenetic & Deve PathRichard Ndung'uNo ratings yet
- Identification and Management of Ambiguous GenitaliaDocument31 pagesIdentification and Management of Ambiguous Genitaliateslimolakunleraji100% (1)
- Testicular Feminization Syndrome: SGD B-3Document29 pagesTesticular Feminization Syndrome: SGD B-3Jessica LinNo ratings yet
- Patterns: OF InheritanceDocument45 pagesPatterns: OF InheritanceMary Grace SunioNo ratings yet
- Residency Preparation: Video Topic: GeneticsDocument22 pagesResidency Preparation: Video Topic: GeneticsKanis FatemaNo ratings yet
- Infertility in Males and FemalesDocument18 pagesInfertility in Males and FemalesKiprotich Titus NgetichNo ratings yet
- UntitledDocument45 pagesUntitledMary Grace SunioNo ratings yet
- By Shveta Jaishankar and Swathi Jain GCM III YearDocument37 pagesBy Shveta Jaishankar and Swathi Jain GCM III YearShveta Jaishankar IyerNo ratings yet
- Patient Family GuidelinesDocument16 pagesPatient Family GuidelinesClaudia IrimieNo ratings yet
- 14 Male InfertilityDocument13 pages14 Male InfertilityShenina KnightleyNo ratings yet
- 14 Male Infertility PDFDocument13 pages14 Male Infertility PDFShenina KnightleyNo ratings yet
- Precocious Puberty: ObjectiveDocument16 pagesPrecocious Puberty: ObjectiveZafar JavedNo ratings yet
- Kallmann SyndromeDocument12 pagesKallmann SyndromeCristi PopoviciNo ratings yet
- Gender Identity Disorder Not Otherwise SpecifiedDocument4 pagesGender Identity Disorder Not Otherwise SpecifiedJona AddatuNo ratings yet
- Sex & Love SlidesDocument45 pagesSex & Love SlidesJennifer Isom Schmidtke, Ph.D.No ratings yet
- Common Genetic Disease Related Hormonal and Metabolism: DR Erna Mirani, M.Si - MedDocument63 pagesCommon Genetic Disease Related Hormonal and Metabolism: DR Erna Mirani, M.Si - MedFahmi Nur ZamanNo ratings yet
- Hypothalamic-Pituitary-Gonadal AxisDocument82 pagesHypothalamic-Pituitary-Gonadal AxisIiiNo ratings yet
- 0127「小兒遺傳及代謝」講師陳燕彰醫師Document114 pages0127「小兒遺傳及代謝」講師陳燕彰醫師許懷朔No ratings yet
- Adol Health - DR FransiscaDocument60 pagesAdol Health - DR FransiscaJohanna FreddaNo ratings yet
- Ambiguous Genitalia - An ApproachDocument35 pagesAmbiguous Genitalia - An ApproachWindy MuldianiNo ratings yet
- Assesment of Amen or RheaDocument49 pagesAssesment of Amen or Rheakhadzx100% (2)
- 1 - Short StatureDocument45 pages1 - Short StatureAmmar AlnajjarNo ratings yet
- Normal and Abnormal PubertyDocument37 pagesNormal and Abnormal Pubertyhazab1968100% (1)
- Reproductive HormonesDocument43 pagesReproductive HormonesMunchkin Celina100% (1)
- Fragile X SyndromeDocument23 pagesFragile X SyndromeVincent ScorsinniNo ratings yet
- PSYC20008 2024 Lecture 5 Human Genetics 2 - UploadDocument27 pagesPSYC20008 2024 Lecture 5 Human Genetics 2 - UploadrevilomartinNo ratings yet
- Adolescent Sexual - Reproductive Health Including Pubertal Changes - DR - ASIRIFI (Autosaved)Document52 pagesAdolescent Sexual - Reproductive Health Including Pubertal Changes - DR - ASIRIFI (Autosaved)Max ZealNo ratings yet
- Male Infertility, Diagnosis and Recent ManagementDocument77 pagesMale Infertility, Diagnosis and Recent ManagementDR SHASHWAT JANINo ratings yet
- Enzyme Linked Immunosorbent Assay (ELISA)Document16 pagesEnzyme Linked Immunosorbent Assay (ELISA)Kuzhandai VeluNo ratings yet
- Comprehensive Exam in Ethics A. Strengths and Weaknesses of The Filipino CharacterDocument6 pagesComprehensive Exam in Ethics A. Strengths and Weaknesses of The Filipino CharacterPrincess Lheakyrie CasilaoNo ratings yet
- Effects of Fertilizers, Manure and Poluthene On The Rate of Elongfation of HypocotylDocument6 pagesEffects of Fertilizers, Manure and Poluthene On The Rate of Elongfation of Hypocotylmusic madissNo ratings yet
- Tech Note Medonic m32 Analyzer Procedures For Optimized System Performance TNM 33227 2Document8 pagesTech Note Medonic m32 Analyzer Procedures For Optimized System Performance TNM 33227 2عبد القادر زيدوNo ratings yet
- New Microsoft Office Word DocumentDocument16 pagesNew Microsoft Office Word DocumentDavid LeeNo ratings yet
- Immunology MCQ BY: Dr. AlgassimDocument4 pagesImmunology MCQ BY: Dr. AlgassimmohamedNo ratings yet
- Giatric NurseDocument5 pagesGiatric NurseKim TanNo ratings yet
- The History of The ConciergerieDocument1 pageThe History of The ConciergerieAnnoying DogNo ratings yet
- Abstract BookDocument168 pagesAbstract BookPawanKaushikNo ratings yet
- Mechanism of ToxicityDocument35 pagesMechanism of ToxicityrinirhynNo ratings yet
- A Culturally Competent Model of Care For African Americans: Josepha Campinha-BacoteDocument6 pagesA Culturally Competent Model of Care For African Americans: Josepha Campinha-BacoteEE KMNo ratings yet
- Draft Reflection Paper in MC 102 LabDocument4 pagesDraft Reflection Paper in MC 102 LabHAZEL SANDRONo ratings yet
- Residual Ridge ResorptionDocument13 pagesResidual Ridge ResorptionsankarNo ratings yet
- Transfusion Related Immunomodulation (Trim) : By/ Aymen OmerDocument14 pagesTransfusion Related Immunomodulation (Trim) : By/ Aymen OmeraymenNo ratings yet
- Study Identification: Clinicaltrials - Gov PrsDocument5 pagesStudy Identification: Clinicaltrials - Gov PrsDolly Nurdin LubisNo ratings yet
- Read Online Textbook The Stolen Hours Karen Swan Ebook All Chapter PDFDocument22 pagesRead Online Textbook The Stolen Hours Karen Swan Ebook All Chapter PDFbetty.lumpkin102100% (5)
- Ayushannualreportfinal 22348189Document69 pagesAyushannualreportfinal 22348189Anil KumarNo ratings yet
- Final Nutrition in COPDDocument30 pagesFinal Nutrition in COPDAnimesh AryaNo ratings yet
- Villareal - NCMA216 Drug StudyDocument10 pagesVillareal - NCMA216 Drug StudyRozen VillarealNo ratings yet
- Case MalariaDocument2 pagesCase MalariaRaju NiraulaNo ratings yet
- DDU (General) Syllabus: Diploma of Diagnostic Ultrasound (DDU)Document19 pagesDDU (General) Syllabus: Diploma of Diagnostic Ultrasound (DDU)MitchNo ratings yet
- Rabbit From Farm To TableDocument3 pagesRabbit From Farm To Tablekarthik kumar100% (1)
- (Pharma-B) 6s-1-Draft - Experiment C & eDocument3 pages(Pharma-B) 6s-1-Draft - Experiment C & eKim RamosNo ratings yet
- Sweet Potato LeavesDocument3 pagesSweet Potato LeavesAlexanderLopezNebresNo ratings yet
- Laws Affecting Community Health Nursing Practice in The PhilippinesDocument2 pagesLaws Affecting Community Health Nursing Practice in The PhilippinesAndrei Borata100% (1)