Professional Documents
Culture Documents
Lewis Et Al. Chapter 30 Jessica Stoefen, MN, RN, CCRN
Lewis Et Al. Chapter 30 Jessica Stoefen, MN, RN, CCRN
Uploaded by
faiza0 ratings0% found this document useful (0 votes)
94 views64 pagesanemia
Original Title
Anemia
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentanemia
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
94 views64 pagesLewis Et Al. Chapter 30 Jessica Stoefen, MN, RN, CCRN
Lewis Et Al. Chapter 30 Jessica Stoefen, MN, RN, CCRN
Uploaded by
faizaanemia
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 64
Lewis et al.
Chapter 30
Jessica Stoefen, MN, RN, CCRN
Copyright © 2017, Elsevier Inc. All Rights Reserved.
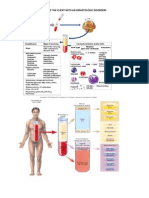
• A deficiency in
• Number of erythrocytes (RBCs)
• Quantity of hemoglobin
• Volume of packed RBCs (hematocrit)
Copyright © 2017, Elsevier Inc. All Rights Reserved.
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• RBC function
• Transport oxygen (O2) from lungs to
systemic tissues
•Carry carbon dioxide from tissues to lungs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Not a specific disease
• Manifestation of a pathologic process
• Diagnosed based on
• Complete blood count (CBC)
• Reticulocyte count
•Peripheral blood smear
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Classified as
• Morphologic
• Cellular characteristics
• Descriptive, objective laboratory information
• Etiologic
• Underlying cause
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Caused by body’s response to tissue
hypoxia
• Manifestations vary based on rate of
development, severity of anemia,
presence of co-existing disease
• Hemoglobin (Hgb) levels are used to
determine severity of anemia
Copyright © 2017, Elsevier Inc. All Rights Reserved.
7
• Pallor
• ↓ Hemoglobin
• ↓ Blood flow to the skin
• Jaundice
• ↑ Concentration of serum bilirubin
• Pruritus
• ↑ Serum and skin bile salt concentrations
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Result from additional attempts by
heart and lungs to provide adequate O2
to tissues
• Cardiac output maintained by
increasing heart rate and stroke
volume
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Subjective Data
• Important health information
• Past health history
• Medications
• Surgery or other treatments
• Dietary history
•Functional health patterns
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Objective Data
• General
• Integumentary Lewis et al. Table
• Respiratory 30-4
• Cardiovascular
•Gastrointestinal
• Neurologic
• Diagnostic findings
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Fatigue
• Imbalanced nutrition: Less than body
requirements
• Ineffective health management
• Assume normal activities of daily living
•Maintain adequate nutrition
• Develop no complications related to
anemia
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Patients with fatigue
• Alternate rest and activity
• Prioritize activities
• Accommodate energy levels
• Maximize O2 supply for vital functions
• Provide assistance to minimize risk for
injury
• Evaluate nutritional needs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Nursing care varies
• Numerous causes of anemia
• Patient specific needs
See Lewis et al. p. 607
Table 30-1 & 30-2
classifications of
anemias
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Anemia is not normal
• More common in the 70s and beyond
• Often related to an underlying cause
• Signs and symptoms may go
unrecognized
•Other health issues
• May be mistaken for normal aging
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Erythropoietin (EPO) is a glycoprotein
primarily produced in the kidneys (10%
in liver)
•↑ Number of stem cells committed to RBC
production
• Shortens time to mature RBCs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Life span of an RBC is 120 days
• Three alterations in erythropoiesis may
decrease RBC production:
• Decreased hemoglobin synthesis
• Defective DNA synthesis in RBCs
•Diminished availability of erythrocyte
precursors
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Most common nutritional disorder in
the world
• Most susceptible
• Very young
• Poor diet
•Women in reproductive years
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Inadequate dietary intake
• 5% to 10% of ingested iron is absorbed
• Malabsorption
• Iron absorption occurs in the duodenum
• Diseases or surgery that alter, destroy, or
remove absorption surface of this area of
intestine cause anemia
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Blood loss
• 2 mL whole blood contain 1 mg iron
• Major cause of iron deficiency in adults
• Chronic blood loss most commonly
through GI and GU systems
• Hemolysis
• Pregnancy contributes to this condition
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• General manifestations of anemia
• Pallor is most common
• Glossitis is second
• Inflammation of tongue
• Cheilitis is also found
• Inflammation of lips
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Laboratory findings
• Hgb, Hct, MCV, MCH, MCHC,
reticulocytes, serum iron, TIBC, bilirubin,
platelets
• Stool occult blood test
• Endoscopy
• Colonoscopy
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Goal
• Treat underlying disease causing reduced
intake or absorption of iron
• Replace iron
• Nutritional therapy
• Oral iron supplements
• Transfusion of packed RBCs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Oral iron
• Inexpensive
• Convenient
• Factors to consider
• Enteric-coated or sustained-release capsules
are counterproductive
• Daily dose is 150 to 200 mg
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Oral iron
• Factors to consider
• Best absorbed as ferrous sulfate in an acidic
environment
• Liquid iron should be diluted and ingested
through a straw
• Side effects
• Heartburn, constipation, diarrhea
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Parenteral iron
• Indicated for malabsorption, oral iron
intolerance, need for iron beyond normal
limits, poor patient compliance
• Can be given IM or IV
• IM may stain skin
• Z-track
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• At-risk groups
• Premenopausal women
• Pregnant women
•Persons from low socioeconomic
backgrounds
• Older adults
•Individuals experiencing blood loss
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Diet teaching
• Supplemental iron
• Discuss diagnostic studies
• Emphasize compliance
• Iron therapy for 2 to 3 months after
Hgb levels return to normal
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• A group of diseases involving
inadequate production of normal Hgb
• Results in decreased erythrocyte
production
• Problem with globulin protein
•Abnormal Hgb synthesis
• Hemolysis occurs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Autosomal recessive genetic basis
• One thalassemic gene
• Thalassemia minor
• Two thalassemic genes
• Thalassemia major
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Thalassemia minor
• Frequently asymptomatic
• Moderate anemia
• Microcytosis
• Hypochromia
• Body adapts to reduction of Hgb – thus no
treatment is indicated
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Thalassemia major
• Life-threatening
• Physical and mental growth often
retarded
• Pale and jaundiced
• Splenomegaly, hepatomegaly, and
cardiomyopathy
• Symptoms develop in childhood
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Thalassemia major
• As the bone marrow responds to the
deficit of O2 -carrying capacity of the
blood, RBC production is stimulated, and
marrow becomes packed with immature
erythroid precursors that die
•Chronic bone marrow hyperplasia
• Hepatitis C
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• No specific drug or diet is effective in
treating thalassemia
• Thalassemia major
• Blood transfusions or exchange
transfusions with chelating agents that
bind to iron to reduce iron overloading
• Splenectomy
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Group of disorders
• Caused by impaired DNA synthesis
• Presence of megaloblasts
• Majority result from deficiency in
• Cobalamin (vitamin B12)
•Folic acid
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Intrinsic factor (IF)
• Protein secreted by parietal cells of gastric
mucosa
• IF is required for cobalamin absorption
in the distal ileum
• If IF is not secreted, cobalamin will not be
absorbed
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Most commonly caused by pernicious
anemia
• Which is caused by an absence of IF
•Insidious onset
• Begins in middle age or later
• Predominant in Scandinavians and African
Americans
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Can also occur:
• GI surgery
• Chronic diseases of the GI tract
• Excessive alcohol or hot tea ingestion
• Smoking
•Long-term users of H2-histamine receptor
blockers and proton pump inhibitors
• Strict vegetarians
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• General manifestations of anemia
develop slowly due to tissue hypoxia
• GI manifestations:
• Sore tongue, anorexia, nausea, vomiting, and
abdominal pain
• Neuromuscular manifestations:
• Weakness, paresthesias of feet and hands,
↓ vibratory and position senses, ataxia, muscle
weakness, and impaired thought processes
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Macrocytic RBCs have abnormal shapes and
fragile cell membranes
• Serum cobalamin levels are decreased
• Normal serum folate levels and low
cobalamin levels suggest megaloblastic
anemia is due to cobalamin deficiency
• Upper GI endoscopy with biopsy of gastric
mucosa
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Parenteral or intranasal administration
of cobalamin is treatment of choice
• Patients will die in 1-3 years without
treatment
•This anemia can be reversed with ongoing
treatment but long-standing
neuromuscular complications may not be
reversible
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Also a cause of megaloblastic anemia
• Folic acid is required for DNA synthesis
• RBC formation and maturation
• Clinical manifestations are similar to
those of cobalamin deficiency, but
absence of neurologic problems
differentiates them
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Common causes
• Dietary deficiency
• Malabsorption syndromes
• Drugs
• Increased requirement
•Alcohol abuse and anorexia
• Loss during hemodialysis
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Serum folate level is low
• Normal is 3 to 16 mg/mL (7 to 36 mol/L)
• Serum cobalamin level is normal
• Treated by replacement therapy
• Usual dose is 1 mg per day by mouth
• Encourage patient to eat foods with
large amounts of folic acid
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Early detection and treatment
• Ensure safety
•Diminished sensations to heat and pain
from neurologic impairment
• Focus on compliance with treatment
• Regular screening for gastric cancer
Copyright © 2017, Elsevier Inc. All Rights Reserved.
At an outpatient clinic, K.L.’s 78-year-old grandma is found
to have a Hgb of 8.7 g/dL (87 g/L) and a Hct of 35%. Based
on the most common cause of these findings in the older
adult, the nurse collects information regarding
a. a history of jaundice and black tarry stools.
b. a 3-day diet recall of the foods the patient has eaten.
c. any drugs that have depressed the function of the bone
marrow.
d. a history of any chronic diseases such as cancer or renal
disease.
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Caused by
• Chronic inflammation
• Autoimmune and infectious disorders
• HIV, hepatitis, malaria
• Heart failure
• Malignant diseases
• Bleeding episodes
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Associated with
• Underproduction of RBCs
• Mild shortening of RBC survival
• Normocytic, normochromic, and
hypoproliferative RBCs
• Usually a mild anemia but can become
severe if the underlying disorder is
untreated
Copyright © 2017, Elsevier Inc. All Rights Reserved.
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Anemia of chronic disease findings
• ↑ Serum ferritin
• ↑ Iron stores
• Normal folate and cobalamin levels
• Treating underlying cause is best
•Rarely blood transfusions
• Conservative use of erythropoietin
therapy
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Pancytopenia
• Decrease in all blood cell types
• Red blood cells (RBCs)
• White blood cells (WBCs)
• Platelets
• Hypocellular bone marrow
• Ranges from chronic to critical
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Rare
• Annual rate of 2-5 new cases/million/year
• Usually acquired
• Idiopathic
• An autoimmune basis is presumed
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Abrupt or gradual development
• Symptoms caused by suppression of
any or all bone marrow elements
• General manifestations of anemia
• Fatigue, dyspnea
•Cardiovascular and cerebral responses
• Neutropenia
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Diagnosis confirmed by laboratory
studies
• Low Hgb, WBC, and platelet values
•Low reticulocyte count
• Elevated serum iron and TIBC
• Hypocellular bone marrow with increased
fat content (yellow marrow)
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Identify and remove causative agent
(when possible)
• Provide supportive care until
pancytopenia reverses
• Prevent complications from infection
• Prevent hemorrhage
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Prognosis of severe untreated aplastic
anemia is poor
• Advances in treatment options have
significantly improved outcomes
•Immune therapies and bone marrow
transplantation can be curative
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Anemia resulting from blood loss may
be caused by either acute or chronic
problems
•Acute blood loss occurs as a result of
sudden hemorrhage
• Sources of chronic blood loss are similar to
those of iron-deficiency anemia
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Causes of sudden hemorrhage
• Trauma
• Complications of surgery
• Conditions or diseases that disrupt
vascular integrity
• Hypovolemic shock
• Compensatory increased plasma volume with
diminished O2 -carrying RBCs
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Caused by body’s attempts to maintain
adequate blood volume and meet
oxygen requirements
• Clinical signs and symptoms are more
important than laboratory values
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Pain
• Internal hemorrhage
• Tissue distention, organ displacement, nerve
compression
• Retroperitoneal bleeding
• Numbness
• Pain in lower extremities
• Shock is major complication
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• With sudden blood volume loss, values
may seem normal or high for 2 to 3
days
• Once plasma volume is replaced, low
RBC concentrations become evident
• Low RBC, Hgb, and Hct levels show up and
reflect actual blood loss
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Replacing blood volume to prevent
shock
• Identifying source of hemorrhage
and stopping blood loss
• Correcting RBC loss
• Providing supplemental iron
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• May be impossible to prevent if caused
by trauma
• Postoperative patients
• Monitor blood loss
• Administer blood products for anemia
• No need for long-term treatment
Copyright © 2017, Elsevier Inc. All Rights Reserved.
• Sources of chronic blood loss:
• Bleeding ulcer
• Hemorrhoids
•Menstrual and postmenopausal blood loss
• Management involves
• Identifying the source
• Stopping the bleeding
• Providing supplemental iron as needed
Copyright © 2017, Elsevier Inc. All Rights Reserved.
You might also like
- Krause's Food & The Nutrition Care Process 13.UnitedVRG - HTD Digestión Dietista PDFDocument1 pageKrause's Food & The Nutrition Care Process 13.UnitedVRG - HTD Digestión Dietista PDFlaura0% (4)
- Unit 8 Assignment 1 7713Document7 pagesUnit 8 Assignment 1 7713Ashley Fagundo100% (1)
- NCP Risk For Deficient Fluid Volume PotentialDocument4 pagesNCP Risk For Deficient Fluid Volume PotentialArian May Marcos100% (1)
- Blood Disorders Seminar No 7Document142 pagesBlood Disorders Seminar No 7Hysum Mushtaq100% (2)
- Virtual Family Health Assessment ProjectDocument4 pagesVirtual Family Health Assessment Projectfaiza0% (1)
- Omar's Family AssessmentDocument10 pagesOmar's Family AssessmentfaizaNo ratings yet
- Self-Transcendence Theory: Pamela.G.Reed (1952-Present)Document20 pagesSelf-Transcendence Theory: Pamela.G.Reed (1952-Present)faizaNo ratings yet
- N375 Critical Thinking Activity ExampleDocument6 pagesN375 Critical Thinking Activity ExamplefaizaNo ratings yet
- ., Critical Thinking Activity 1, Davies SDocument3 pages., Critical Thinking Activity 1, Davies Sfaiza100% (1)
- Concept MapDocument2 pagesConcept MapfaizaNo ratings yet
- Levels of Prevention and Modes of InterventionDocument22 pagesLevels of Prevention and Modes of Interventionachuth2983% (6)
- Bionic 880Document13 pagesBionic 880Ian Miller100% (1)
- What Is Misophonia? M001Document2 pagesWhat Is Misophonia? M001guyfitzm1100% (1)
- Sirs and ModsDocument28 pagesSirs and ModsJoemay Belle CabanelaNo ratings yet
- The Child With A Condition of The Blood, Blood-Forming Organs, or Lymphatic SystemDocument68 pagesThe Child With A Condition of The Blood, Blood-Forming Organs, or Lymphatic SystemKelly TayagNo ratings yet
- Pathophysiology LectureDocument73 pagesPathophysiology LectureJoyyNo ratings yet
- Hematologic DisorderDocument16 pagesHematologic DisorderZoe DorothyNo ratings yet
- Blooddisorders 21 230610142333 f4472c75Document114 pagesBlooddisorders 21 230610142333 f4472c75Nabeel TahirNo ratings yet
- Anemia 3Document23 pagesAnemia 3Dana AhmadNo ratings yet
- Hematologic DisorderDocument66 pagesHematologic DisorderKristel AnneNo ratings yet
- AnemiaDocument43 pagesAnemiaNithiya NadesanNo ratings yet
- Chapt 44 LiverDocument93 pagesChapt 44 Liverhossein boloorianNo ratings yet
- Dr. Pradeep Daniel Gainneos .R PG Student Dept. of PedodonticsDocument130 pagesDr. Pradeep Daniel Gainneos .R PG Student Dept. of PedodonticsPradeepDanielGainneos0% (1)
- Nutrients Involved in Fluid and Electrolyte Balance: © 2017 Pearson Education, IncDocument55 pagesNutrients Involved in Fluid and Electrolyte Balance: © 2017 Pearson Education, IncazzahwaauroraNo ratings yet
- Acute Kidney InjuryDocument65 pagesAcute Kidney InjuryMohamad HamzaNo ratings yet
- BloodDocument142 pagesBloodChelleyOllitroNo ratings yet
- AnaemiaDocument73 pagesAnaemiamedicoprakashNo ratings yet
- Nursing Care Management of Patients With Anemia - 01Document38 pagesNursing Care Management of Patients With Anemia - 01Sionur 00No ratings yet
- Practice Teaching On Anemia: Presented By: Mr. Hari Singh Nagar M. SC Nursing 1 YearDocument44 pagesPractice Teaching On Anemia: Presented By: Mr. Hari Singh Nagar M. SC Nursing 1 YearSundarNo ratings yet
- IB Blood CellsDocument31 pagesIB Blood CellsDeva SeenaNo ratings yet
- Pathophysiology of BloodDocument80 pagesPathophysiology of BloodISRAELNo ratings yet
- Anemia: Shannen Kate N. Tercenio PM401Document22 pagesAnemia: Shannen Kate N. Tercenio PM401Shannen Kate TercenioNo ratings yet
- Iron Deficiency AnaemiaDocument48 pagesIron Deficiency AnaemiarkNo ratings yet
- Bloodkb 160720181259Document129 pagesBloodkb 160720181259Jeena RajNo ratings yet
- CH 42 GastritisDocument24 pagesCH 42 GastritisNina Patricia OrbeNo ratings yet
- New CVDDocument77 pagesNew CVDRachael TheisenNo ratings yet
- AnaemiaDocument71 pagesAnaemiaREETHUNo ratings yet
- Anemia During PregnancyDocument39 pagesAnemia During PregnancyBhawna JoshiNo ratings yet
- Lecture 4 - Hematology-PedsDocument60 pagesLecture 4 - Hematology-PedsGelsey Gelsinator JianNo ratings yet
- Anaemia by Haider AliDocument38 pagesAnaemia by Haider AliAbdul SamadNo ratings yet
- Iron Deficiency AnemiaDocument30 pagesIron Deficiency AnemiaSiti Nursuhada binti Mohd AminNo ratings yet
- Anemia 090820015524 Phpapp01Document31 pagesAnemia 090820015524 Phpapp01Jeffrey Calicdan BucalaNo ratings yet
- AnaemiaDocument27 pagesAnaemiaEmmanuel UsikuNo ratings yet
- Inflammation of Gastric Mucosa One of Most Common Problems Affecting The StomachDocument24 pagesInflammation of Gastric Mucosa One of Most Common Problems Affecting The StomachMuhajir AbbasNo ratings yet
- Average Age of StudentDocument6 pagesAverage Age of StudentKenan Gawinan KekeNo ratings yet
- AnaemiaDocument32 pagesAnaemiafalodun miracleNo ratings yet
- Course Code: NSC 410 Course Title: Practicum and Teaching Methodology MATRIC NUMBER: 19001748Document6 pagesCourse Code: NSC 410 Course Title: Practicum and Teaching Methodology MATRIC NUMBER: 19001748Kenan Gawinan KekeNo ratings yet
- Pathology Slides 2023 (B&B) (Medicalstudyzone - Com)Document249 pagesPathology Slides 2023 (B&B) (Medicalstudyzone - Com)Carol de AndradeNo ratings yet
- Pediatric Hematology LectureDocument84 pagesPediatric Hematology LectureloitaNo ratings yet
- Physiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaDocument65 pagesPhysiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaRizal AbdurrahmanNo ratings yet
- Chapter 38 Agents To Control Blood Glucose LevelsDocument40 pagesChapter 38 Agents To Control Blood Glucose Levelsjanmishelle208No ratings yet
- HAP 2 CH 6 Endocrine SystemDocument70 pagesHAP 2 CH 6 Endocrine SystemCaamir Dek HaybeNo ratings yet
- FLec2ANEMIA1Disorders of Iron and Heme MetabolismDocument67 pagesFLec2ANEMIA1Disorders of Iron and Heme MetabolismFrancis ValdezNo ratings yet
- The Micronutrients & Water: Roxana Dev Omar DevDocument36 pagesThe Micronutrients & Water: Roxana Dev Omar Deverwan berhanNo ratings yet
- ProteinDocument23 pagesProteincharisma maya0% (1)
- MISDC AnaemiaDocument33 pagesMISDC AnaemiawanyNo ratings yet
- Anemia: Anurag B Patidar Lecturer, CON, DMCHDocument27 pagesAnemia: Anurag B Patidar Lecturer, CON, DMCHpreet kaurNo ratings yet
- Chapter 44: Nursing Care of The Client With An Hematologic DisordersDocument18 pagesChapter 44: Nursing Care of The Client With An Hematologic DisordersfLOR_ZIANE_MAENo ratings yet
- Hematologic DisordersDocument197 pagesHematologic DisordersDanica Mae BianitoNo ratings yet
- Anemia in ChildrenDocument34 pagesAnemia in ChildrensmpoojasubashNo ratings yet
- AnimiaDocument9 pagesAnimiaElkasmi HoudaNo ratings yet
- Student - Module 9 - Renal AlterationsDocument44 pagesStudent - Module 9 - Renal AlterationsHannaNo ratings yet
- Anemia سمنار 2023Document25 pagesAnemia سمنار 2023Hesham IbrahimNo ratings yet
- Chronic Kidney DiseaseDocument14 pagesChronic Kidney DiseaseGabrielle Frances FernandezNo ratings yet
- Human Disorder & Gene TherapyDocument14 pagesHuman Disorder & Gene Therapyulfh08152No ratings yet
- Anemia 130809044630 Phpapp01Document30 pagesAnemia 130809044630 Phpapp0114 zarwa hassanNo ratings yet
- CH 41: Hematological Assessment (Per Amendolair)Document28 pagesCH 41: Hematological Assessment (Per Amendolair)USC Upstate Nursing CoachesNo ratings yet
- L15 - Blood - CMDocument32 pagesL15 - Blood - CMAleandra LettNo ratings yet
- Clinical Hematological: Assist Prof. Dr. Mudhir S. ShekhaDocument31 pagesClinical Hematological: Assist Prof. Dr. Mudhir S. ShekhaAhmed. Masud.OthmanNo ratings yet
- Vitamins & Minerals & HerbalsDocument27 pagesVitamins & Minerals & HerbalsLydia Lopz MsnrncdNo ratings yet
- Chapter - 51 Diuretic AgentsDocument40 pagesChapter - 51 Diuretic Agentsjanmishelle208No ratings yet
- Types Of Hemolytic Anemia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandTypes Of Hemolytic Anemia, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Aghayedo, Elmi-Homework 6Document3 pagesAghayedo, Elmi-Homework 6faizaNo ratings yet
- Running Head: Family Health Assessment 1Document6 pagesRunning Head: Family Health Assessment 1faizaNo ratings yet
- Running Header: Teaching Plan Surname 1Document6 pagesRunning Header: Teaching Plan Surname 1faizaNo ratings yet
- N375 Literature Tables, Guideline and Grading RubricDocument7 pagesN375 Literature Tables, Guideline and Grading RubricfaizaNo ratings yet
- Example Health Promotion Teaching PlanDocument6 pagesExample Health Promotion Teaching PlanfaizaNo ratings yet
- 11 CLINICAL SITE - Geriatric AssessmentsDocument2 pages11 CLINICAL SITE - Geriatric AssessmentsfaizaNo ratings yet
- Please Welcome To The Women and Children's Unit .: NAMEDocument1 pagePlease Welcome To The Women and Children's Unit .: NAMEfaizaNo ratings yet
- Pharmacology ATI Study GuideDocument3 pagesPharmacology ATI Study Guidefaiza100% (1)
- ASSIGNMENT: Pediatric Group Project & Presentation: Assessment of A Preschool Age ChildDocument13 pagesASSIGNMENT: Pediatric Group Project & Presentation: Assessment of A Preschool Age ChildfaizaNo ratings yet
- Week Date Diet/workout 1 5/9: TopicDocument2 pagesWeek Date Diet/workout 1 5/9: TopicfaizaNo ratings yet
- 2017 SSS TRIO ApplicationDocument2 pages2017 SSS TRIO ApplicationfaizaNo ratings yet
- Impaired SwallowingDocument2 pagesImpaired SwallowingfaizaNo ratings yet
- Asthma: Jessica Stoefen, MN, RN, CCRNDocument71 pagesAsthma: Jessica Stoefen, MN, RN, CCRNfaizaNo ratings yet
- North Hennepin Community College Nursing Program Clinical ProfileDocument2 pagesNorth Hennepin Community College Nursing Program Clinical ProfilefaizaNo ratings yet
- Centered Nursing Process Approach (9th Ed.) - St. Louis, MO: ElsevierDocument1 pageCentered Nursing Process Approach (9th Ed.) - St. Louis, MO: ElsevierfaizaNo ratings yet
- Thehumanbody3-4 UnitguideDocument9 pagesThehumanbody3-4 UnitguidefaizaNo ratings yet
- 4 INDEPENDENT - Pediatric Group Project & PresentationDocument59 pages4 INDEPENDENT - Pediatric Group Project & PresentationfaizaNo ratings yet
- Pharmocology Drug Cards: InnovarDocument33 pagesPharmocology Drug Cards: InnovarfaizaNo ratings yet
- 'S Aide Position Due To Personal Reasons. My Last Day of Emp ' Notice of Resignation. I Regret Any Inconvenience This May Cause, But The SituationDocument1 page'S Aide Position Due To Personal Reasons. My Last Day of Emp ' Notice of Resignation. I Regret Any Inconvenience This May Cause, But The SituationfaizaNo ratings yet
- Geeks Lab 6 ButerflyDocument7 pagesGeeks Lab 6 ButerflyMatthew Spencer HoNo ratings yet
- Diagnostic ProcessDocument14 pagesDiagnostic ProcessHelvin Eka Putra100% (1)
- UCLAN Coursework Assessment Brief PJ2300 GI CS 21-22 Sit - VerifiedDocument5 pagesUCLAN Coursework Assessment Brief PJ2300 GI CS 21-22 Sit - VerifiedSeanNo ratings yet
- CPD Questions For Volume 21 Issue 3Document4 pagesCPD Questions For Volume 21 Issue 3KeeranmayeeishraNo ratings yet
- 06 Collection and Handling of Biopsy SpecimensDocument7 pages06 Collection and Handling of Biopsy SpecimensAudrey CobankiatNo ratings yet
- TDM Slides NicholsDocument39 pagesTDM Slides NicholsGordon BongNo ratings yet
- Antibiotics in Oral & Maxillofacial SurgeryDocument50 pagesAntibiotics in Oral & Maxillofacial SurgerysevattapillaiNo ratings yet
- MCQ Examples Jan 2016Document30 pagesMCQ Examples Jan 2016Arshad KhanNo ratings yet
- PIS Flaminal Forte 112013Document2 pagesPIS Flaminal Forte 112013Roi Levinzon100% (1)
- Codeine - Wikipedia, The Free EncyclopediaDocument13 pagesCodeine - Wikipedia, The Free EncyclopediakjhgkhgkjgkjgkjNo ratings yet
- Hepatic Encephalopathy and DkaDocument6 pagesHepatic Encephalopathy and Dkajames garciaNo ratings yet
- Supplement Watch Life PakDocument2 pagesSupplement Watch Life Pakcuongtalentccc100% (1)
- Obat Kausatif Infeksi: 6ggpo, 0shqwlget Grad Corporis Ult Hui Form 3DDocument5 pagesObat Kausatif Infeksi: 6ggpo, 0shqwlget Grad Corporis Ult Hui Form 3DMaulana Malik IbrahimNo ratings yet
- Stago Vol 5 Issue 2 2015Document10 pagesStago Vol 5 Issue 2 2015PABLO ZAMUDIONo ratings yet
- Duke University Nurse Anesthesia Program (Acct #7042) Montgomery, Kelly Barton (Semester 7) Is Logged inDocument3 pagesDuke University Nurse Anesthesia Program (Acct #7042) Montgomery, Kelly Barton (Semester 7) Is Logged inkellyb11No ratings yet
- Musculoskeletal Imaging - The Basics: Laurie Lomasney, MD Department of Radiology Loyola University Medical CenterDocument45 pagesMusculoskeletal Imaging - The Basics: Laurie Lomasney, MD Department of Radiology Loyola University Medical CenterJohnny CordayNo ratings yet
- Hildegard E. Peplau: Interpersonal Theory (Interpersonal Relations in Nursing)Document9 pagesHildegard E. Peplau: Interpersonal Theory (Interpersonal Relations in Nursing)Otaku ChanNo ratings yet
- Identification of Potentially Dangerous Spiders of KansasDocument2 pagesIdentification of Potentially Dangerous Spiders of KansasChao L. Wu (Chao "Jimmy" Wu)No ratings yet
- A Literature Review On De-Quervain's TenosynovitisDocument12 pagesA Literature Review On De-Quervain's TenosynovitisfricaNo ratings yet
- Nursing Skills Lab Equipment & SuppliesDocument199 pagesNursing Skills Lab Equipment & SuppliesMiriam100% (12)
- Food and Drug Administration (FDA) Act of 2009Document22 pagesFood and Drug Administration (FDA) Act of 2009Godofredo SabadoNo ratings yet
- Dokumen - Tips Prismaflex User ManualDocument287 pagesDokumen - Tips Prismaflex User ManualosamaNo ratings yet
- Motor Control and Motor LearningDocument5 pagesMotor Control and Motor Learningelayumven100% (1)
- Full Guide To Laser Tattoo Removal TreatDocument3 pagesFull Guide To Laser Tattoo Removal TreatDimas Candido FerreiraNo ratings yet