Professional Documents
Culture Documents
Treatment in Pediatric Cancer
Treatment in Pediatric Cancer
Uploaded by
Lamria Maloni Siahaan0 ratings0% found this document useful (0 votes)
20 views35 pagesThe document summarizes treatment approaches for several types of pediatric cancer, including leukemia, retinoblastoma, and lymphoma. Chemotherapy is described as the primary treatment for most childhood cancers. Specific chemotherapy drugs and protocols are outlined for different cancers. Side effects of chemotherapy are also discussed. Other approaches like surgery and radiation therapy play roles in some cancer types. The goal of pediatric cancer treatment is typically to cure the cancer while preserving quality of life.
Original Description:
pediatric cancer
Original Title
treatment in pediatric cancer
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document summarizes treatment approaches for several types of pediatric cancer, including leukemia, retinoblastoma, and lymphoma. Chemotherapy is described as the primary treatment for most childhood cancers. Specific chemotherapy drugs and protocols are outlined for different cancers. Side effects of chemotherapy are also discussed. Other approaches like surgery and radiation therapy play roles in some cancer types. The goal of pediatric cancer treatment is typically to cure the cancer while preserving quality of life.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
20 views35 pagesTreatment in Pediatric Cancer
Treatment in Pediatric Cancer
Uploaded by
Lamria Maloni SiahaanThe document summarizes treatment approaches for several types of pediatric cancer, including leukemia, retinoblastoma, and lymphoma. Chemotherapy is described as the primary treatment for most childhood cancers. Specific chemotherapy drugs and protocols are outlined for different cancers. Side effects of chemotherapy are also discussed. Other approaches like surgery and radiation therapy play roles in some cancer types. The goal of pediatric cancer treatment is typically to cure the cancer while preserving quality of life.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 35
Treatment in Pediatric Cancer
Department of Child Health
Faculty of Medicine
University of HKBP Nommensen
Leukemia
Chemotherapy
Chemotherapy (chemo) is the main treatment for nearly all
childhood leukemias
This is treatment with anti-cancer drugs that are given into a
vein, into a muscle, into the cerebrospinal fluid (CSF), or
taken as pills
Except when given into the CSF, chemo drugs enter the
bloodstream and reach all areas of the body, making this
treatment very useful for cancers such as leukemia
Chemotherapy
The treatment of leukemia uses combinations of several
chemo drugs
Doctors give chemo in cycles, with each period of treatment
followed by a rest period to give the body time to recover
In general, treatment for acute myeloid leukemia (AML) uses
higher doses of chemo over a shorter period of time (usually
less than a year), and acute lymphocytic leukemia (ALL)
treatment uses lower doses of chemo over a longer period of
time (usually 2 to 3 years)
Chemotherapy
Readiness for patient will get chemotherapy :
Clinically good
Laboratory findings
Nutritional state
Pshycological state
Chemotherapy
Some of the drugs used to treat childhood leukemia include:
Vincristine
Daunorubicin, also known as daunomycin
Doxorubicin
Cytarabine, also known as cytosine arabinoside or ara-C
L-asparaginase , PEG-L-asparaginase
Etoposide
Teniposide
6-mercaptopurine
6-thioguanine
Methotrexate
Mitoxantrone
Cyclophosphamide
Prednisone
Dexamethasone
Chemotherapy
The side effect of chemo depend on the type and dose of drugs given
and the length of treatment. These side effects can include:
Hair loss
Mouth sores
Loss of appetite
Diarrhea
Nausea and vomiting
Increased risk of infections (because of low white blood cell
counts)
Bruising and bleeding easily (from low platelet counts)
Fatigue (caused by low red blood cell counts)
Chemotherapy
The side effects above usually go away when treatment is finished.
There are often ways to reduce these side effects drugs can be
given to help prevent or reduce nausea and vomiting
Tumor lysis syndrome
another possible side effect of chemotherapy
patients who had large numbers of leukemia cells in the body
When chemo kills these cells, they break open and release their
contents into the bloodstream kidneys, which aren’t able to get rid
of all of these substances at once
Making sure the child gets lots of fluids during treatment and by
giving certain drugs, such as bicarbonate, allopurinol, and
rasburicase, which help the body get rid of these substances
Surgery
Surgery has a very limited role in treating childhood
leukemia
Because leukemia cells spread throughout the bone marrow
and to many other organs through the blood, it’s not possible
to cure this type of cancer by surgery
Surgery rarely has any role even in the diagnosis, since a bone
marrow aspirate and biopsy can usually diagnose leukemia
State After Treatment
Remission
A remission (or complete remission) is usually defined as having no
evidence of leukemia after the 4 to 6 weeks of induction
treatment. This means:
The bone marrow contains fewer than 5% blast cells,
The blood cell counts are within normal limits, and
There are no signs or symptoms of the disease
A molecular complete remission means there is no evidence of
leukemia cells in the bone marrow, even when using very
sensitive lab tests, such as polymerase chain reaction (PCR).
Even when leukemia is in remission, this does not always mean
that it has been cured
Minimal residual disease
Minimal residual disease (MRD) is a term used after treatment when
leukemia cells can’t be found in the bone marrow using standard lab
tests (such as looking at cells under a microscope), but they can still be
detected with more sensitive tests (such as flow cytometry or PCR). In
general, children with MRD during or after induction chemotherapy are
more likely to have the leukemia relapse (come back) and therefore may
need more intense treatment. Children with more MRD have a greater
risk of relapse than those with less MRD.
Active disease
Active disease means that either there is evidence that the leukemia is
still present during treatment or that the disease has relapsed (come
back) after treatment. For a patient to have relapsed, more than 5% of
the marrow must be made up of blast cells
Retinoblastoma
Children with retinoblastoma are treated by a team of doctors
that often includes:
A pediatric ophthalmologist: a doctor who treats eye
diseases in children
An ocular oncologist: a doctor (usually an
ophthalmologist) who treats cancers of the eye
A pediatric oncologist: a doctor who treats children with
cancer
A radiation oncologist: a doctor who treats cancer with
radiation therapy
The goals of treatment for retinoblastoma are:
To get rid of the cancer and save the child’s life
To save the eye if possible
To preserve as much vision as possible
To limit the risk of second cancers later in life, which can be
caused by treatment, particularly in children with hereditary
retinoblastoma
The most important factors that help determine treatment are:
Whether the tumor is just in one eye or both
How good the vision in the eye is
Whether the tumor has extended outside the eye
The main types of treatment for retinoblastoma are:
Surgery
Radiation therapy
Photocoagulation (using lasers to kill small tumors or the
blood vessels that feed them)
Cryotherapy (using cold to freeze and kill small tumors)
Thermotherapy (using a type of laser to apply heat to kill
small tumors)
Chemotherapy
High-dose chemotherapy and stem cell transplant
Chemotherapy
Chemo can be given in different ways :
Systemic chemotherapy
Periocular (subtenon) chemotherapy
Intra-arterial chemotherapy
doctors can use much smaller doses of chemo drugs (less
than 10% of the doses used for systemic chemo)
Intravitreal chemotherapy
Chemotherapy
Some of the drugs used to treat children with retinoblastoma
include:
Carboplatin
Cisplatin
Vincristine
Etoposide
Cyclophosphamide
Topotecan
Doxorubicin
Most often, 2 or 3 drugs are given at the same time. A standard
combination used to shrink intraocular retinoblastomas is
carboplatin, vincristine, and etoposide, although for very small
tumors, only carboplatin and vincristine may be enough
Chemotherapy
Along with those listed above, certain chemo drugs can cause specific side
effects
Cisplatin and carboplatin can affect the kidneys. Giving the child plenty
of fluids during treatment can help reduce this risk. These drugs can also
cause hearing loss in young children, especially in babies younger than 6
months.Your child’s doctor may check your child’s hearing with tests
during or after treatment. When carboplatin is injected directly into the
tissues near the eye (periocular chemotherapy), it can cause redness and
swelling in the area.
Vincristine can damage nerves. Some children may feel tingling and
numbness, particularly in their hands and feet.
Some drugs, such as etoposide, doxorubicin, and cyclophosphamide, can
increase the risk of developing a cancer of white blood cells known
as acute myeloid leukemia (AML) later in life. Fortunately, this is not
common.
Chemotherapy
Doxorubicin can damage the heart. The risk of this happening
goes up with the total amount of the drug given. Doctors try
to limit this risk as much as possible by not giving more than
the recommended doses and by checking the heart with an
echocardiogram (an ultrasound of the heart) during
treatment.
Cyclophosphamide can damage the bladder, which can cause
blood in the urine. This risk can be lowered by giving this
drug along with plenty of fluids and with a drug called
mesna, which helps protect the bladder.
Surgery ( Enucleation )
Surgery is not needed for all retinoblastomas, especially for
smaller tumors. But if a tumor gets quite large before it is
found, vision in the eye has often already been destroyed,
with no hope of getting it back
The most obvious side effect of enucleation is the loss of
vision in that eye, although most often the vision has already
been lost because of the cancer.
Removing the eye also can affect the future growth of bone
and other tissues around the eye socket, which can make the
area look somewhat sunken. Using an orbital implant can
sometimes lessen this effect
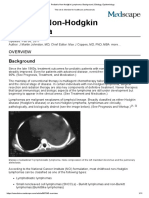
Lymphoma
Chemotherapy
Chemotherapy (chemo) is the main treatment for non-
Hodgkin lymphoma (NHL) in children. Chemo uses anti-
cancer drugs that are usually given into a vein or taken by
mouth
These drugs enter the bloodstream and reach all areas of the
body, making this treatment very useful for cancers that tend
to spread widely, such as NHL
In some cases where the lymphoma may have reached the
brain or spinal cord, chemo may also be given into the
cerebrospinal fluid (known as intrathecal chemo)
Chemotherapy
Children with NHL get a combination of several chemo drugs
over a period of time
The number of drugs, their doses, and the length of treatment
depend on the type and stage of the lymphoma
Doctors give chemo in cycles. Each chemo cycle generally lasts
for several weeks
A period of treatment is followed by a rest period to allow the
body time to recover
Most chemo treatments are given on an outpatient basis (in the
doctor’s office or clinic or hospital outpatient department), but
some – especially at the start of treatment – may need to be given
while the child stays in the hospital
Some of the drugs commonly used to treat
childhood lymphoma include:
Cyclophosphamide
Vincristine
Doxorubicin
Prednisone
Dexamethasone
Cytarabine
Methotrexate
L-asparaginase, PEG-L-asparaginase
Etoposide
6-mercaptopurine
Ifosfamide
Surgery
Surgery often has a limited role in treating lymphoma since it’s
unlikely to cure it by itself, and normal organs might be damaged
in the process
Surgery is sometimes used as the first treatment for early-stage
Burkitt lymphoma that is in only one area (such as part of the
intestine) to try to remove as much of the tumor as possible
before chemotherapy.
If the lymphoma can be removed completely, doctors might be
able to give a less intensive chemotherapy regimen
Other uses of surgery include: To get biopsy samples for lab tests
to determine the exact type of lymphoma if non-surgical
procedures (needle biopsy, bone marrow biopsy, etc.) could not
get enough tissue
Radiation Therapy
Sequential nodal spread of disease, usually from neck to
pelvis, allows for cure with radiation therapy to the involved
and contiguous nodal regions but requires accurate staging of
the disease
Radiation therapy was the first curative modality used for
Hodgkin lymphoma (HL) in the early 1960s. However, the
doses and fields used for the treatment of adult Hodgkin
lymphoma caused profound musculoskeletal retardation,
cardiac toxicity, and increased incidence of secondary
malignancies in the radiation field
Radiation Therapy
Radiation protocols are used as an adjuvant treatment after
chemotherapy
To reduce complications, risk-adapted or response-based, low-
dose, involved-field, or extended-field radiation is administered
In current pediatric trials, the use of nodal conformal radiation is
being evaluated to further decrease the burden of radiation to
other tissues
In addition, in some protocols the field for radiation has changed,
from the involved areas at the time of diagnosis to the residual
disease present at the time of response to therapy evaluation
Palliative Care
Pediatric Palliative care (pronounced pal-lee-uh-tiv) is
specialized medical care for children with serious illnesses. It
focuses on providing relief from the symptoms, pain, and
stress of a serious illness—whatever the diagnosis. The goal is
to improve quality of life for both the child and the family.
Pediatric palliative care is provided by a team of doctors,
nurses and other specialists who work together with a child’s
other doctors as an extra layer of support. It is appropriate at
any age and at any stage of an illness and can be provided
along with treatment meant to cure.
Pediatric palliative care addresses a serious medical
conditions, including genetic disorders, cancer, prematurity,
neurologic disorders, heart and lung conditions and others.
It relieves the symptoms of these diseases, such as pain,
shortness of breath, fatigue, constipation, nausea, loss of
appetite and difficulty sleeping. In short, it helps the child
and the family gain the strength to carry on with daily
life.
Pediatric palliative care is family-centered. Families are
better able to choose options that are in line with their
values, traditions and culture. This improves the well-being of
the entire family
s
THANK YOU
You might also like
- Case 32 QuestionsDocument9 pagesCase 32 Questionsapi-532124328No ratings yet
- Medical Student Clinical Assessment Form: (Mm/dd/yy) (Mm/dd/yy)Document4 pagesMedical Student Clinical Assessment Form: (Mm/dd/yy) (Mm/dd/yy)Natasha Reddy0% (1)
- NCP Acl TearDocument2 pagesNCP Acl TearEd Pascasio100% (2)
- Non Hodgkin Lymphoma in ChildrenDocument4 pagesNon Hodgkin Lymphoma in ChildrenMilzan MurtadhaNo ratings yet
- PICOT QuestionDocument1 pagePICOT Questionmelodia gandezaNo ratings yet
- Leukemia in ChildrenDocument44 pagesLeukemia in ChildrenSami ShouraNo ratings yet
- Chikungunya in Children 2015Document3 pagesChikungunya in Children 2015Douglas UmbriaNo ratings yet
- HerniaDocument67 pagesHerniaياسر نعيم الربيعي100% (2)
- Pediatric Non-Hodgkin Lymphoma - Background, Etiology, EpidemiologyDocument11 pagesPediatric Non-Hodgkin Lymphoma - Background, Etiology, EpidemiologytopNo ratings yet
- Pediatric Hiv/Aids: Kussia.A (MD)Document62 pagesPediatric Hiv/Aids: Kussia.A (MD)Yemata HailuNo ratings yet
- Measles: Note Prepared By: Arpana Khanal Dibyata Khatiwada Swastika Manandhar Dipak Mandal Amrit NeupaneDocument29 pagesMeasles: Note Prepared By: Arpana Khanal Dibyata Khatiwada Swastika Manandhar Dipak Mandal Amrit NeupaneTaufik KhanNo ratings yet
- Acute Hepatic Failure: Dr. Idit Segal December 2003Document25 pagesAcute Hepatic Failure: Dr. Idit Segal December 2003ZeusKimNo ratings yet
- Pediatric TuberculosisDocument126 pagesPediatric TuberculosisSherly CanceritaNo ratings yet
- HYDROCEPHALOUSDocument25 pagesHYDROCEPHALOUSSuman PoudelNo ratings yet
- 1.nutritional Disorder With KeyDocument9 pages1.nutritional Disorder With KeykarthicpraveenNo ratings yet
- Scale For Assessment of Pain in Infants, Neonates and ChildrenDocument4 pagesScale For Assessment of Pain in Infants, Neonates and Childrenfuka priesleyNo ratings yet
- Pediatric DMDocument39 pagesPediatric DMmy Lord JesusNo ratings yet
- Childhood Depression Presentation OutlineDocument7 pagesChildhood Depression Presentation Outlineapi-290018716No ratings yet
- Newborn Screening and Other Child Health ProgramDocument2 pagesNewborn Screening and Other Child Health ProgramPamela Joy Rico UnayNo ratings yet
- Rheumatic Heart DiseaseDocument15 pagesRheumatic Heart DiseaseAica AnisNo ratings yet
- Nutritional Needs of ChildrenDocument68 pagesNutritional Needs of ChildrenRani G SNo ratings yet
- Celiac Disease PresentationDocument24 pagesCeliac Disease Presentationmurali_bharadwazNo ratings yet
- Seminar On Choanal AtresiaDocument16 pagesSeminar On Choanal AtresiaGreeshma ShajiNo ratings yet
- Eating DisordersDocument6 pagesEating DisordersKarthik SathyanNo ratings yet
- Disorders of NewbornDocument4 pagesDisorders of NewbornBRUELIN MELSHIA MNo ratings yet
- 1905 Pediatric Cardiac Critical Care: Anthony - Lee@Utsouthwestern - EduDocument5 pages1905 Pediatric Cardiac Critical Care: Anthony - Lee@Utsouthwestern - EduShahzad Muneer ShahzadNo ratings yet
- Choanal AtresiaDocument32 pagesChoanal AtresiaGreeshma ShajiNo ratings yet
- ObesityDocument14 pagesObesityapi-338453738No ratings yet
- Numeric Rating ScaleDocument1 pageNumeric Rating ScaleGem Nicole P. Abrasaldo100% (1)
- Paediatric CardiologyDocument15 pagesPaediatric CardiologyAaron Nameer Abrar RahmanNo ratings yet
- Manova: Multivariate Analysis of Variance: Maaria JahangirDocument12 pagesManova: Multivariate Analysis of Variance: Maaria JahangirMaariaJahangirNo ratings yet
- Procedure File Front PageDocument37 pagesProcedure File Front PageShilpa sharmaNo ratings yet
- Acute Flaccid Paralysis (AFP) : Dr. Muhammad Haroon Resident Fcps Ii Trainee Deptt. of Pediarics KksDocument47 pagesAcute Flaccid Paralysis (AFP) : Dr. Muhammad Haroon Resident Fcps Ii Trainee Deptt. of Pediarics KksharoonNo ratings yet
- Congenital Diaphragmatic Hernia UptodateDocument16 pagesCongenital Diaphragmatic Hernia UptodateArmando CustodioNo ratings yet
- Neonatal Seizure 1Document5 pagesNeonatal Seizure 1Rayhanun MardhatillahNo ratings yet
- Nephrotic SyndromeeDocument28 pagesNephrotic SyndromeeRiteka SinghNo ratings yet
- Understanding Depression in Children and Adolescents: Bachelor's Thesis Degree Programme Nursing 2011Document52 pagesUnderstanding Depression in Children and Adolescents: Bachelor's Thesis Degree Programme Nursing 2011Maysoun AtoumNo ratings yet
- 6-Role of FBNC in Reducing IMR in J&KDocument22 pages6-Role of FBNC in Reducing IMR in J&KRicha MishraNo ratings yet
- The Integrated Management of Childhood IllnessesDocument32 pagesThe Integrated Management of Childhood IllnessesKrishna PhulpagarNo ratings yet
- Acute Liver Failure in Children 2008Document15 pagesAcute Liver Failure in Children 2008nevermore11No ratings yet
- 1.basic Final McqsDocument78 pages1.basic Final McqsPrabhat KcNo ratings yet
- Cold Chain & Immunisation ScheduleDocument18 pagesCold Chain & Immunisation ScheduleAman GoelNo ratings yet
- Pertussis: 1. Disease ReportingDocument18 pagesPertussis: 1. Disease Reportingzenagit123456No ratings yet
- Pediatric Respiratory Disorders General InterventionsDocument2 pagesPediatric Respiratory Disorders General Interventionscayla mae carlosNo ratings yet
- Coagulation DisordersDocument14 pagesCoagulation Disorderssusan_grace123No ratings yet
- Multiple Regression in SPSSDocument17 pagesMultiple Regression in SPSSVishal SharmaNo ratings yet
- Congenital Anomalies of Kidney and Ureter 2161 0940 1000190Document10 pagesCongenital Anomalies of Kidney and Ureter 2161 0940 1000190Indra JayaNo ratings yet
- Paediatrics - Febrile Convulsions Assessment, Treatment and Education PDFDocument12 pagesPaediatrics - Febrile Convulsions Assessment, Treatment and Education PDFPalash NagdeoteNo ratings yet
- PoliomyelitisDocument50 pagesPoliomyelitisJohn John TorresNo ratings yet
- Pediatric CardiologyDocument7 pagesPediatric CardiologyMaikka IlaganNo ratings yet
- Hemophilia & Other Hereditary Bleeding Disorders: Djajadiman Gatot Novie Amelia CDocument34 pagesHemophilia & Other Hereditary Bleeding Disorders: Djajadiman Gatot Novie Amelia CpiniNo ratings yet
- Pediatric Drug CalculationDocument22 pagesPediatric Drug Calculation11 - JEMELYN LOTERTENo ratings yet
- HIV Infection in PediatricDocument36 pagesHIV Infection in PediatricFatima SaghezliNo ratings yet
- Febrile Convulsions in ChildrenDocument2 pagesFebrile Convulsions in ChildrenMagdalena Dwiyani HutajuluNo ratings yet
- The Family With A Toddler ToddlerDocument5 pagesThe Family With A Toddler ToddlerReyna Mee AhiyasNo ratings yet
- Revised University Manual - 1Document144 pagesRevised University Manual - 1Nazish AbidNo ratings yet
- Offer Letter - Ahmed HussainDocument1 pageOffer Letter - Ahmed HussainRafiq AfridiNo ratings yet
- HydrocephalussDocument32 pagesHydrocephalussElvisNo ratings yet
- Disaster Management Module 4Document15 pagesDisaster Management Module 4Anil MNo ratings yet
- Fluid and Electrolyte NewDocument54 pagesFluid and Electrolyte NewSelam Tesfaye ShebaNo ratings yet
- Preterm Complications..Document89 pagesPreterm Complications..UdayBhaskar ChinthaNo ratings yet
- 4 MumpsDocument18 pages4 MumpsNamira Caroline ErchoNo ratings yet
- Congenital Diaphragmatic HerniaDocument29 pagesCongenital Diaphragmatic Herniapaddy9980No ratings yet
- The Ideal Neutropenic Diet Cookbook; The Super Diet Guide To Replenish Overall Health For A Vibrant Lifestyle With Nourishing RecipesFrom EverandThe Ideal Neutropenic Diet Cookbook; The Super Diet Guide To Replenish Overall Health For A Vibrant Lifestyle With Nourishing RecipesNo ratings yet
- Somatic Sensation: Dr. Debby Mirani Lubis, M.BiomedDocument34 pagesSomatic Sensation: Dr. Debby Mirani Lubis, M.BiomedLamria Maloni SiahaanNo ratings yet
- Somatic Sensation: Dr. Debby Mirani Lubis, M.BiomedDocument34 pagesSomatic Sensation: Dr. Debby Mirani Lubis, M.BiomedLamria Maloni SiahaanNo ratings yet
- Atopic MarchDocument7 pagesAtopic MarchLamria Maloni SiahaanNo ratings yet
- Diabetic Emergencies Case StudiesDocument32 pagesDiabetic Emergencies Case StudiesLamria Maloni Siahaan0% (1)
- Sistem Metabolisme: Jenny Novina SitepuDocument21 pagesSistem Metabolisme: Jenny Novina SitepuLamria Maloni SiahaanNo ratings yet
- Mendoza Resume ST Marys BHRNDocument1 pageMendoza Resume ST Marys BHRNapi-621792232No ratings yet
- CHEMISTRY and PharmacologyDocument577 pagesCHEMISTRY and PharmacologyIurieUngureanu100% (2)
- New Advanced in RadiotherapyDocument49 pagesNew Advanced in RadiotherapyIndonesian Journal of CancerNo ratings yet
- Covid 19 Health and Safety StandardsDocument3 pagesCovid 19 Health and Safety StandardsMaPhee BernadetteNo ratings yet
- Mental Illness SSKDocument4 pagesMental Illness SSKAnonymous 7WJJxPdENo ratings yet
- Metodologia de Admitere 2018 - Limba EnglezaDocument27 pagesMetodologia de Admitere 2018 - Limba EnglezaoscarapaNo ratings yet
- Adrenaline (Anaethesia Tutorial of The Week)Document8 pagesAdrenaline (Anaethesia Tutorial of The Week)Raisa AriesthaNo ratings yet
- Hmis in Blood BanksDocument35 pagesHmis in Blood BanksDrPriyanka Prashant PawsheNo ratings yet
- ESIC Maharashtra MTS - ResultDocument8 pagesESIC Maharashtra MTS - Resultwww.myemploymentportal.comNo ratings yet
- Point of Care TestingDocument80 pagesPoint of Care TestingInternational Medical Publisher100% (1)
- P8 Anrad APGDocument14 pagesP8 Anrad APGLia NurNo ratings yet
- Benzo Withdrawal SyndromeDocument7 pagesBenzo Withdrawal SyndromeWernerNo ratings yet
- Abusive RelationshipsDocument10 pagesAbusive RelationshipsGiulia Nădășan-CozmaNo ratings yet
- Speech & Language Therapy in Practice, Autumn 1999Document32 pagesSpeech & Language Therapy in Practice, Autumn 1999Speech & Language Therapy in PracticeNo ratings yet
- Case Study - Intestinal Resection and Anastomosis in A DogDocument13 pagesCase Study - Intestinal Resection and Anastomosis in A Dogapi-301746262No ratings yet
- History of First AidDocument10 pagesHistory of First AidnihalNo ratings yet
- (Presentation) PhobiaDocument40 pages(Presentation) PhobiaJajaMeowNo ratings yet
- BTL-6000 Super Inductive SystemDocument67 pagesBTL-6000 Super Inductive SystemromikatmNo ratings yet
- Acute Ischemic Stroke: Clinical PracticeDocument8 pagesAcute Ischemic Stroke: Clinical PracticeDorina FrunzeNo ratings yet
- Febrile SeizureDocument32 pagesFebrile SeizureShiva Valeska ArdhaniswariNo ratings yet
- Nursing Care For Child With Autoimmune Diseases & GI DisordersDocument4 pagesNursing Care For Child With Autoimmune Diseases & GI Disordersbunso padillaNo ratings yet
- Bronchial HygieneDocument37 pagesBronchial HygieneRayan MohhamadNo ratings yet
- Management of Relapsed Endometrial Cancer After First-Line Chemotherapy - Bradley MonkDocument49 pagesManagement of Relapsed Endometrial Cancer After First-Line Chemotherapy - Bradley Monkinfo7615No ratings yet
- Case Study: Cushing and AddisonDocument4 pagesCase Study: Cushing and AddisonJeff ValdezNo ratings yet
- Chapter 1: Introduction To Operative DentistryDocument11 pagesChapter 1: Introduction To Operative DentistryMariam AdnanNo ratings yet
- Lithium: Mimicry, Mania, and Muscle Relaxants: Simon Flood MRCP FRCA Andrew Bodenham FRCADocument4 pagesLithium: Mimicry, Mania, and Muscle Relaxants: Simon Flood MRCP FRCA Andrew Bodenham FRCARizwan AhmedNo ratings yet