Professional Documents
Culture Documents
Jurnal Breast Rekon Presentasi 10 Okt 18 Revisi
Jurnal Breast Rekon Presentasi 10 Okt 18 Revisi
Uploaded by
Febriadi R0 ratings0% found this document useful (0 votes)
21 views57 pagesThis document discusses different surgical approaches for breast cancer, including breast-conserving therapy (BCT), mastectomy, and reconstruction techniques. It provides a brief history of approaches from radical mastectomy to BCT. It describes oncoplastic breast surgery combining tumor removal with breast reconstruction. Techniques discussed include skin-sparing and nipple-sparing mastectomy, as well as immediate and delayed reconstruction using implants, tissue expanders, and flaps. Complications of different approaches are also summarized.
Original Description:
breast rekon
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses different surgical approaches for breast cancer, including breast-conserving therapy (BCT), mastectomy, and reconstruction techniques. It provides a brief history of approaches from radical mastectomy to BCT. It describes oncoplastic breast surgery combining tumor removal with breast reconstruction. Techniques discussed include skin-sparing and nipple-sparing mastectomy, as well as immediate and delayed reconstruction using implants, tissue expanders, and flaps. Complications of different approaches are also summarized.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
0 ratings0% found this document useful (0 votes)
21 views57 pagesJurnal Breast Rekon Presentasi 10 Okt 18 Revisi
Jurnal Breast Rekon Presentasi 10 Okt 18 Revisi
Uploaded by
Febriadi RThis document discusses different surgical approaches for breast cancer, including breast-conserving therapy (BCT), mastectomy, and reconstruction techniques. It provides a brief history of approaches from radical mastectomy to BCT. It describes oncoplastic breast surgery combining tumor removal with breast reconstruction. Techniques discussed include skin-sparing and nipple-sparing mastectomy, as well as immediate and delayed reconstruction using implants, tissue expanders, and flaps. Complications of different approaches are also summarized.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
You are on page 1of 57
Presentan : dr Mohamad Riza EL Anshori
Traine : dr Yopi SpB
Pembimbing : dr Ahmad Kurnia SpB(K)Onk
introduction
Breast cancer the leading cause of cancer
death.
Its surgical approach less mutilating in the
last decades.
Nowadays individualized at its best,
consideration not only the oncological aspects
of the tumor, neo/adjuvant treatment & genetic
predisposition
its timing (immediate vs delayed)
patient’s condition & wish
history
William Halsted radical mastectomy
(end 19th century)
Patey mastectomy (M. pectoralis major
preservation)
Fisher (1985) BCT lumpectomy
(segmental mastectomy) + adjuvant
radiotherapy (stage I and II breast cancer)
Oncoplastic breast surgery
breast cancer screening programs were initiated
breast centers offering an interdisciplinary and
comprehensive therapeutical approach for breast
cancer were established.
increased detection & treatment of predominantly
early breast cancers
improved survival rates and superior esthetic
outcome.
BCT :
safe treatment for most women with early-stage
breast cancers
safely applied in 70–80% of the cases requiring
surgical tumor removal.
The primary goal to preserve shape the
contralateral breast.
Thereby, one should take into account that
postoperative radiotherapy may result in some
extent of tissue shrinkage
BCT :
Although ,decreasing over the last two
decades, the rate of mastectomy has again
increased lately due to:
the detection of multifocal tumors
tumors with an extended in situ proportion
that is difficult to delimit
unfavorable breast-to-tumor size ratio in
rather thin patients with small-to-
intermediate sized breasts.
BCT ;
Awareness in the female population and the
relatively frequent detection of a genetic
predisposition to breast cancer (i.e., BRCA-1, BRCA-
2, p53) this trend toward an increased rate of
mastectomy, be it curative or prophylactic.
the absolute gold standard for surgical breast
cancer treatment, many women must or wish to
undergo mastectomy.
Consequently, reconstruction of the breast must be
offered, particularly in young patients.
MASTECTOMY
Nowadays, basically two ways of mastectomy
1. preserves the breast’s skin envelope as
possible, including NAC (skin-sparing , areola-
sparing , nipple-sparing , skin-reducing
mastectomy)
2. total ablation of the breast (complete removal
breast skin & glandular breast tissue)
biopsy scars and skin overlying a tumor or
even infiltrated by the tumor are excised in
order to reduce the risk of local recurrence.
BCT :
skin-sparing mastectomy equal oncological local
safety & improved esthetic outcome
(compared MRM)
the need for secondary surgery to adjust the
contralateral breast to achieve symmetry after
skin-sparing mastectomy, particularly if autologous
reconstruction with flaps is used.
Prophylactic bilateral
mastectomy
due to the increased detection of patients
carrying a genetic mutation or predisposition to
develop breast cancer (e.g., BRCA-1, BRCA-2, p53).
high demands to the esthetic outcome that can be
overcome with nipple-sparing mastectomy the
gold standard in prophylactic mastectomies.
Skin & nipple sparing
mastectomies complication
high rate of ischemia-related wound & necrosis of
up to 54%
consequence of a critically impaired blood supply
of the distant areas of the often very thin skin flap.
Various approaches described to decrease
ischemia-associated complications of the
mastectomy skin flap, including :
1. surgical skin reduction of the mastectomy flap
2. temporary insertion of an expandable implant
3. local application of vasodilators.
RECONSTRUCTiON TECHNIQUES
OF THE BREAST
BR the type of mastectomy & classified :
reconstruction type & time point.
delayed & immediate breast reconstruction.
IBR advantage of reducing the total
number of surgical procedures.
3 different approaches of breast
reconstruction may be considered:
(1) breast reconstruction using implants and skin expanders
(2) breast reconstruction using flaps
(vascularized autologous tissue)
(3) breast reconstruction using non-vascularized
lipoaspirate autologous fat.
BR Using implants and Skin
expanders
the first “implant”-based (1895) by Vincenz
Czerny (used a patient’s lipoma from the lumbar
region to reconstruct a post-surgical asymmetry
after tumor removal).
Cronin & Gerow fathered the modern era of
silicone gel filled breast implants and so allowed
DBR
5th generation silicone gel-filled breast implants
that contain a highly viscous & more or less
form-stable gel are usually used.
BR Using implants and Skin
expanders
The use of implants and skin expanders is not only
the oldest way to reconstruct a breast but also the
quickest and presumably easiest method of breast
reconstruction.
implant-based (the most often used technique)
implant-based’s prerequisite adequate skin
envelope covering the implant introduced in a
submuscular plane detaching the medial insertions
of the pectoralis major muscle from the ribs.
BR Using implants
Implant-based BR local complications 10 years with
a risk for a reoperation of 70% .
25 - 35% diagnosed with severe capsular contracture
& implant rupture.
high complication rate results from the thin skin
envelope remaining after mastectomy, not provide
coverage of the implant.
complication rate does neither consider breast shape
deformity and asymmetry in the context of mild to
moderate capsular contracture nor does it consider
an even worse outcome in implant-based breast
reconstruction with irradiated skin.
BR Using implants
De facto BR implants may yield very nice long-term
results
the implant will always remain more or less fixed to the
thoracic wall and consequently the breast maintains a
unique shape, indepen-dently from the patient’s
posture.
implant-based not allow recreating a naturally
shaped ptotic breast in most patients
often requires adaptive surgery of the contralateral
breast to achieve symmetry
BR Using implants
prevents from “collateral damage,” such as :
scars
contour deformity
muscular weak-ness
might be seen after flap harvesting for flap-
based BR (Figure 3).
Expander-Based Breast Reconstruction
first by Radovan (1976) to recreate the amount of
lost skin after mastectomy stepwise expansion of
the remaining chest skin.
Ideally, the contralateral breast volume should not
exceed a volume of 300–400 g.
Typically, patients with pre-expansion of the breast
skin undergo secondary breast reconstruction with
implants.
Expander-Based Breast Reconstruction
in young and skinny patients with
insufficient skin laxity,
yet enough adipose tissue to
reconstruct a breast mound of ~300–
350 g,
one might pre expand the breast skin
after mastectomy in order to
substitute the expander with an
autologous flap.
particularly helpful in patients who are sure to
get adjuvant radiotherapy of the skin and/or the
thoracic wall.
However, we currently do not know at what
extent the flap will indurate and shrink at long-
term follow-up.
BR with Acellular Dermis The use of acellular
dermal matrices in implant & expander based
Matrices of human, porcine, or bovine origin.
to improve esthetic outcome & reduce implant-
related morbidity, such as :
1. decreased rate of capsular contracture
2. an improved tolerance to radiotherapy
3. more natural anatomical reconstruction of the
inframammary fold and final breast contour.
Nahabedian a high safety & excellent
results use acellular dermis in a 12-year follow-
up (reconstruction after infection or
radiotherapy)
several matrix-related complications :
hematoma
Infection
seromas .
Lardi et al complications related to
patient characteristics and a learning curve,
patient selection
technical principles.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
The myocutaneous flaps for breast
reconstruction
Louis Ombredanne ( France, 1906 )-> the first
pedicled pectoralis muscle flap for IBR.
Ombredanne was the first reconstruct the skin
defect + the breast mound (at that time a
“luxury” procedure with limited indications).
Tanzani (Italy) first the pedicled myocutaneous
latissimus dorsi flap
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
Flap surgery for BR
the mid 70s, flaps from the abdomen &
thoracoepigastric, need several surgical stages.
The initial not to reconstruct the breast mound
primarily aimed resurfacing the thoracic
wall’s defects after radical mastectomy.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
Bostwick myocutaneous LD flap + silicone
implant adequate skin coverage to restore
the breast mound.
The advantage LD flap consistent
anatomy + easy flap harvest.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
flap transfer from the back can be associated :
highly visible scars
contour deformity of the thorax ventrally
the back dorsally as well as animation of the
skin/muscle-implant complex of the
pectoralis major respectively latissimus
dorsi muscle due to innervation of the latter
one (Figure 4).
the muscle undergoes atrophy of 50–75% of
its volume requiring an implant to restore
volume (unless the patient is rather thin
(Figure 5))
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
Tarantino 57% patients with a LD flap +
implants :
revisional surgery for implant replacement or
implant removal after a mean follow-up of 10
years
the indication for this procedure should be
restricted to patients who do not qualify for
either implant-based or flap-based BR
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
Hokin & Silfverskiold (1987) an extended
latissimus dorsi flap to avoid the use of an
implant.
The flap’s volume was significantly increased
by dissecting the subcutaneous fat
surrounding the skin island .
donor site morbidity increased
1. prolonged seroma
2. wound dehiscence rate
3. contour deformity.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
To overcome lack of the donor site of the
pedicled TRAM flap
Arnez et al
popularized the free TRAM flap
i.e., the microvascular anastomosis of at
least one artery & one vein of the flap to
recipient vessels.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
the authors limited harvest of the rectus
abdominis muscle, a safer transfer due to
improved perfusion originating from the
larger caudal pedicle (deep inferior
epigastric artery instead of deep superior
epigastric artery )
improved medial breast contour due to the
lack of tunneling of the flap’s cranial
pedicle.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
“perforator flap” or DIEP flap
revolutionized BR by :
1. maximizing the amount of safe tissue
transfer
2. minimizing donor site morbidity.
Abdominal tissue suitable for BR since
many patients have a certain abdominal
excess of skin and fat.
autologous BR using a DIEP (deep inferior
epigastric perforator) flap the gold
standard.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
lymphedema of the arm after sentinel lymph
node biopsy, axillary lymph node dissection and
or/radiotherapy of the lymph node basins, one
can surgically using lymphaticovenous
anastomosis or microvascular lymph node
transfer.
Combined with a DIEP flap, since the flap mostly
consists of the lymph nodes in the groin area
lateral to the femoral vessels and depends on
the pedicle originating from the superficial
inferior epigastric vessels .
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
microvascular flap to best personalize BR :
This included:
1. the superior gluteal artery perforator (sGAP) flap
2. the inferior gluteal artery perforator (iGAP) flap
from the gluteal region
3. the fasciocutaneous infragluteal (FCI) flap
4. the profunda femoral artery perforator (PAP) flap
from the infragluteal region
5. the transverse myocutaneous gracilis (TMG) flap
from the inner thigh region .
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
the internal mammary artery and its
concomitant vein used as the recipient
vessels.
the arterial branches originating from the
subscapular artery (e.g., thoracodorsal
artery, circumflex scapulae artery) or sternal
perforators arising through the pectoral
muscle are used.
Breast Reconstruction Using Flaps
(vascularized Autologous Tissue)
BR using autologous flap tissue allows a natural
& durable result
flap harvest will cause a “collateral damage” at
the flap’s donor site, including surgery
complications:
1. Scars
2. contour deformity
3. functional decreased.
microvascular flap-based BR is not only
technically more demanding, but also requires
more infrastructures within a BR , as compared
to implant-based BR (Table 1).
Fat Graft-Based BR Using Non vascularized
Lipoaspirate Fat
Autologous fat grafting (AFG; lipografting, lipofilling)
using liposuction followed by its reinjection into the
tissue to be corrected or augmented.
Fat grafting to the breast > 100 years old since
Holländer corrected a retracted scar after mastectomy
by injecting parceled fat into the scar.
AFG to the breast has become a popular tool over the
last 20 years, both in esthetic and reconstructive
surgery.
Fat Graft-Based BR Using Non
vascularized Lipoaspirate Fat
Regarding the breast, AFG proven effective
to correct post-surgical irregularities:
1. contour deformities and volume
asymmetries after BCT
2. “rippling” after implant-BR
3. improvement of the transition zone
between flap and skin in the neckline, as
well as the preparation of the
postmastectomy irradiated chest wall prior
to implant placement.
4. BR by means of AFG promising results.
Fat Graft-Based BR Using Non
vascularized Lipoaspirate Fat
AFG a “natural” filler, & unlike synthetic
fillers will neither induce any foreign body
reaction nor be resorbed completely.
to be structural, injection of the fat in
small aliquots using blunt cannulas in
multiple directions & multiple layers.
This approach maximizes the fat-to-tissue
contact, thereby the exposition of non
vascularized fat to vascularized host tissue .
Fat Graft-Based BR Using Non
vascularized Lipoaspirate Fat
Consensus fat may not be injected into
the glandular tissue of the breast.
60–70% of the injected fat is engrafted to
the host tissue.
Fat necrosis and oil cysts are common
complications after AFG and occur in
~5% .
Fat Graft-Based BR Using Non
vascularized Lipoaspirate Fat
fat grafting to the breast is controversially
discussed
presence of remaining glandular breast tissue,
as, for example, after BCT.
Grafted fat that naturally contains progenitor &
stem cells associated with breast cancer
progression & metastasic spread in an
experimental setting .
REFINEMENT SURGERY AFTER
BREAST RECONSTRUCTION
After BR, particularly if BR is performed
unilaterally, refinement surgery may be necessary
to reach symmetry of the breasts with regard to
shape, contour, and size.
The procedures usually consist of mastopexy,
breast reduction, or breast augmentation using
implants.
AFG is often used to correct small volume
asymmetries and contour deformities.
CONCLUSION
Breast cancer is the leading cause of cancer
death in women.
Its surgical approach has become less and
less mutilating, allowing for 70–80% of the
operated cases to undergo (BCT) that has
proven to be as safe as mastectomy with
regard to overall survival.
20–30% of the operated women are subjected
to mastectomy.
CONCLUSION
Since ~25 years, SSM alternative
to ablation for better esthetic results
due to preservation of the breast’s
skin envelope, from an oncological
point of view as safe as mastectomy.
SSM needs IBR not to lose the
skin envelope that unreconstructed
will inevitably retract and shrink to
the level of the thoracic wall.
CONCLUSION
BR should be personalized at its best, first of all
taking into consideration not only the oncological
aspects of the tumor, neo-/adjuvant treatment
and genetic predisposition, but also its timing
(IBR versus DBR), as well as the patient’s
condition and wish.
CONCLUSION
the overall number of breast reconstruction has
lately considerably increased.
BR itself can basically be classified into three
categories, including
1. implant and expander-based breast
reconstruction
2. flap-based breast reconstruction (vascularized
autologous tissue), a combination of both (flap
and implant)
3. breast reconstruction using fat grafting (non-
vascularized autologous lipoaspirate fat).
CONCLUSION
fat grafting to refine post-reconstructive
asymmetries.
importance that every woman having a high risk
(family history) diagnosed with a genetic
mutation affected breast cancer gets the
possibility to be presented to a multidisciplinary
board of a certified breast center prior to
surgery to be informed about all treatment
modalities, various modalities of BR.
CONCLUSION
The goal of this multidisciplinary
board is to best personalize breast
reconstruction, of course putting to
the fore the adequate oncological
treatment.
Thank you
You might also like
- PhilHealth Circular No. 0035, s.2013 Annex 2 List of Procedure Case RatesDocument98 pagesPhilHealth Circular No. 0035, s.2013 Annex 2 List of Procedure Case RatesChrysanthus Herrera50% (2)
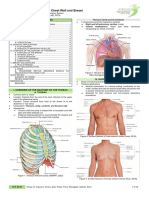
- 06 - 07 - Anatomy of The Chest Wall and BreastDocument16 pages06 - 07 - Anatomy of The Chest Wall and Breastbo gum parkNo ratings yet
- BCS Concepts Version XDocument44 pagesBCS Concepts Version XKumar KaushikNo ratings yet
- Mammoplasty Nottingham (6028)Document13 pagesMammoplasty Nottingham (6028)imtinanNo ratings yet
- Chen 2011 Chapter Oncoplastic Techniques For BreastDocument10 pagesChen 2011 Chapter Oncoplastic Techniques For BreastJohn TusselNo ratings yet
- Oncological Safety of Prophylactic Breast Surgery: Skin-Sparing and Nipple-Sparing Versus Total MastectomyDocument9 pagesOncological Safety of Prophylactic Breast Surgery: Skin-Sparing and Nipple-Sparing Versus Total MastectomynariecaNo ratings yet
- Review: Benjamin O Anderson, Riccardo Masetti, Melvin J SilversteinDocument13 pagesReview: Benjamin O Anderson, Riccardo Masetti, Melvin J SilversteinsanineseinNo ratings yet
- BreastReconstruction Review 2016Document9 pagesBreastReconstruction Review 2016Mohammed FaragNo ratings yet
- MastectomyDocument6 pagesMastectomyJustinAlmedaNo ratings yet
- JBC 15 350Document6 pagesJBC 15 350Andres VasquezNo ratings yet
- S. A. Robertson., 2014Document13 pagesS. A. Robertson., 2014ajeng hefdeaNo ratings yet
- Clough K Oncoplasty BJSDocument7 pagesClough K Oncoplasty BJSkomlanihou_890233161No ratings yet
- Breast Reconstruction After Bilateral ProphylacticDocument9 pagesBreast Reconstruction After Bilateral ProphylacticDirk BucknerNo ratings yet
- 10.1007@s12609 019 0305 3Document8 pages10.1007@s12609 019 0305 3Yefry Onil Santana MarteNo ratings yet
- 03 AnatomyDocument9 pages03 AnatomymaytorenacgerNo ratings yet
- MastopexyDocument10 pagesMastopexyMei WanNo ratings yet
- Letter A incision periareolar mastopexy with breast implant augmentation-dr. kamal hussein saleh-consultant cosmetic surgeon-al emadi hospital-qatar-doha,زرق ابر البوتوكس,جراحة التجميل,تجميل الانف,تجميل الثدي,تكبير الثدي,تكبير الارداف,مستشفى العمادي,قطر,دبيDocument5 pagesLetter A incision periareolar mastopexy with breast implant augmentation-dr. kamal hussein saleh-consultant cosmetic surgeon-al emadi hospital-qatar-doha,زرق ابر البوتوكس,جراحة التجميل,تجميل الانف,تجميل الثدي,تكبير الثدي,تكبير الارداف,مستشفى العمادي,قطر,دبيDR. KAMAL HUSSEIN SALEH AL HUSSEINY100% (1)
- Sili Kono MaDocument4 pagesSili Kono MaDella Rahmaniar AmelindaNo ratings yet
- Incision in Breast Oncoplastic SurgeryDocument26 pagesIncision in Breast Oncoplastic Surgeryccmcshh surgeryNo ratings yet
- MastopexyDocument15 pagesMastopexyLuiggi FayadNo ratings yet
- Atlas of Breast DeformityDocument17 pagesAtlas of Breast Deformitykomlanihou_890233161No ratings yet
- OncoplasticDocument14 pagesOncoplasticYefry Onil Santana MarteNo ratings yet
- Nava 2006Document8 pagesNava 2006Pasquale ProvaNo ratings yet
- Prepectoral Breast Reconstruction With Tiloop Bra Pocket: A Single Center Prospective StudyDocument9 pagesPrepectoral Breast Reconstruction With Tiloop Bra Pocket: A Single Center Prospective StudyFlorina PopaNo ratings yet
- Mastectomy (Case Analysis)Document7 pagesMastectomy (Case Analysis)Lester_Ocuaman_2248No ratings yet
- Mammography PresentationDocument84 pagesMammography Presentationsarose bhandari67% (3)
- Revision in Autologous Breast ReconstructionDocument24 pagesRevision in Autologous Breast ReconstructionJose Mauricio Suarez Becerra100% (1)
- Partial Mastectomy ReconstructionDocument12 pagesPartial Mastectomy ReconstructionJose Mauricio Suarez BecerraNo ratings yet
- Gox 8 E2966Document10 pagesGox 8 E2966michael atlanNo ratings yet
- Clinical Study: Extreme Oncoplastic Surgery For Multifocal/Multicentric and Locally Advanced Breast CancerDocument9 pagesClinical Study: Extreme Oncoplastic Surgery For Multifocal/Multicentric and Locally Advanced Breast CancerAsti DwiningsihNo ratings yet
- Tzeng 2011 Chapter MastectomyDocument14 pagesTzeng 2011 Chapter MastectomyDewa AnggaNo ratings yet
- Mastectomy,,osmayDocument5 pagesMastectomy,,osmayREj LolueNo ratings yet
- Safety of Fat Grafting in Secondary Breast ReconstructionDocument7 pagesSafety of Fat Grafting in Secondary Breast ReconstructionAlexander VigenNo ratings yet
- 14 Central Quadrant TechniqueDocument10 pages14 Central Quadrant TechniquemaytorenacgerNo ratings yet
- Oncoplastic Breast SurgeryDocument20 pagesOncoplastic Breast SurgeryGeorge Yacoup100% (1)
- Breast Reconstruction - Current TechniquesDocument288 pagesBreast Reconstruction - Current Techniquesamirekhalili1100% (1)
- Oncoplastic Breast SurgeryDocument27 pagesOncoplastic Breast SurgeryReem Amr El-DafrawiNo ratings yet
- Surgical Correction of Gynecomastia With Minimal Scarring: Multimediamanuscript AestheticDocument5 pagesSurgical Correction of Gynecomastia With Minimal Scarring: Multimediamanuscript AestheticAngga Putra Kusuma KusumaNo ratings yet
- Oncologic Safety of Conservative Mastectomy in The Therapeutic SettingDocument10 pagesOncologic Safety of Conservative Mastectomy in The Therapeutic SettingIdaamsiyatiNo ratings yet
- 2 StageprepecDocument10 pages2 StageprepecsalyouhaNo ratings yet
- Breast Reconstruction: Rekonstrukcija DojkeDocument7 pagesBreast Reconstruction: Rekonstrukcija DojkeJuwita Dewi PratiwiNo ratings yet
- Breast Reconstruction, AlmominDocument58 pagesBreast Reconstruction, Almominlayla alyamiNo ratings yet
- Early Breast Cancer TherapyDocument20 pagesEarly Breast Cancer TherapyIpseet MishraNo ratings yet
- Direct-To-Implant Breast ReconstructionDocument3 pagesDirect-To-Implant Breast ReconstructionCarlos Javier SolorzaNo ratings yet
- Breast Reconstruction With Microvascular MS-TRAM and DIEP FlapsDocument8 pagesBreast Reconstruction With Microvascular MS-TRAM and DIEP FlapsisabelNo ratings yet
- General Principle of MastectomyDocument35 pagesGeneral Principle of MastectomyScorpion NusNo ratings yet
- 3D Mammometric Changes in The Treatment of Idiopathic Joban 2019Document9 pages3D Mammometric Changes in The Treatment of Idiopathic Joban 2019Wildan Satrio WemindraNo ratings yet
- Sciencedirect: Improving Outcomes in Breast Reconstruction: From Implant-Based Techniques Towards Tissue RegenerationDocument5 pagesSciencedirect: Improving Outcomes in Breast Reconstruction: From Implant-Based Techniques Towards Tissue RegenerationRita DiabNo ratings yet
- Modified Radical MastectomyDocument6 pagesModified Radical Mastectomymetch isulatNo ratings yet
- Modified Radical MastectomyDocument10 pagesModified Radical MastectomynekNo ratings yet
- Chun 2011Document6 pagesChun 2011Radityo Budi LeksonoNo ratings yet
- BR 17102023Document19 pagesBR 17102023Maxi AbalosNo ratings yet
- Immediate Versus Delayed ReconstructionDocument12 pagesImmediate Versus Delayed ReconstructionJose Mauricio Suarez BecerraNo ratings yet
- Oncoplastic and Reconstructive BreastDocument14 pagesOncoplastic and Reconstructive BreastYefry Onil Santana Marte100% (1)
- Dermis 2 en MamaDocument11 pagesDermis 2 en MamaErika Rodriguez MarteNo ratings yet
- Feasibility and Early Cosmetic Outcome of Modified Lateral Intercostal Artery Perforator Flap After Breast Conservative SurgeryDocument11 pagesFeasibility and Early Cosmetic Outcome of Modified Lateral Intercostal Artery Perforator Flap After Breast Conservative Surgeryhaytham1412No ratings yet
- 1 s2.0 S174868151730181X MainDocument9 pages1 s2.0 S174868151730181X MainChiara BoccalettoNo ratings yet
- Internal MastopexyDocument7 pagesInternal MastopexyfumblefumbleNo ratings yet
- Breast ReconstructionDocument58 pagesBreast ReconstructionSumi TranNo ratings yet
- Gox 8 E2578Document12 pagesGox 8 E2578Ade Triansyah EmsilNo ratings yet
- Sinmasta CorreccionDocument6 pagesSinmasta CorreccionEugenia KowriginNo ratings yet
- Oncoplastic Breast Surgery Techniques for the General SurgeonFrom EverandOncoplastic Breast Surgery Techniques for the General SurgeonNo ratings yet
- Cosmetic and Reconstructive Surgery PolicyDocument13 pagesCosmetic and Reconstructive Surgery PolicyBrian AndrewNo ratings yet
- BreasteDocument60 pagesBreastemalathiNo ratings yet
- Case RatesDocument306 pagesCase RatesCyril DaguilNo ratings yet
- Treating Breast Cancer: Local TreatmentsDocument99 pagesTreating Breast Cancer: Local Treatmentssuci triana putriNo ratings yet
- 2019E 09 - Oncoplastic and Reconstructive SurgeryDocument22 pages2019E 09 - Oncoplastic and Reconstructive Surgeryrusgal8992No ratings yet
- Early Complications in Prepectoral Tissue Expander Based Breast ReconstructionDocument11 pagesEarly Complications in Prepectoral Tissue Expander Based Breast ReconstructionBruno Mañon0% (1)
- Five Steps To Internal Mammary Vessel Preparation in Less Than 15 MinutesDocument3 pagesFive Steps To Internal Mammary Vessel Preparation in Less Than 15 MinutesGökhan AkçiçekNo ratings yet
- Factors in Uencing Patient Decision-Making Between Simple Mastectomy and Surgical AlternativesDocument7 pagesFactors in Uencing Patient Decision-Making Between Simple Mastectomy and Surgical AlternativesDewi PaatNo ratings yet
- Scientific Events Distribution PDFDocument9 pagesScientific Events Distribution PDFCodrin FodorNo ratings yet
- Breast Reconstruction - Perspectives, Outcomes and Potential Complications (2017)Document191 pagesBreast Reconstruction - Perspectives, Outcomes and Potential Complications (2017)Sudip Shakya100% (2)
- The Pedicled TRAM Flap in Breast ReconstructionDocument22 pagesThe Pedicled TRAM Flap in Breast ReconstructionJose Mauricio Suarez BecerraNo ratings yet
- Obesity and Breast Reconstruction: Complications and Patient-Reported Outcomes in A Multicenter, Prospective StudyDocument10 pagesObesity and Breast Reconstruction: Complications and Patient-Reported Outcomes in A Multicenter, Prospective StudyMehmet SürmeliNo ratings yet
- Breast MCQDocument13 pagesBreast MCQMahmoud Abouelsoud100% (1)
- Robotics in Plastic SurgeryDocument15 pagesRobotics in Plastic SurgeryRaúl MartínezNo ratings yet
- Safety of Fat Grafting in Secondary Breast ReconstructionDocument7 pagesSafety of Fat Grafting in Secondary Breast ReconstructionAlexander VigenNo ratings yet
- Breast Reconstruction and MastectomyDocument3 pagesBreast Reconstruction and Mastectomysina bayat shahbaziNo ratings yet
- Assessment and Management of Patients With Breast Disorders Assessment and Management of Patients With Breast DisordersDocument36 pagesAssessment and Management of Patients With Breast Disorders Assessment and Management of Patients With Breast DisordersMozart OlarioNo ratings yet
- Questions and Rationale 2Document152 pagesQuestions and Rationale 2Ma. Louise Lovely RosalesNo ratings yet
- Prepectoral Breast Reconstruction With Tiloop Bra Pocket: A Single Center Prospective StudyDocument9 pagesPrepectoral Breast Reconstruction With Tiloop Bra Pocket: A Single Center Prospective StudyFlorina PopaNo ratings yet
- Day 4 L2Document90 pagesDay 4 L2yousif.05001467No ratings yet
- Breast Self ExaminationDocument81 pagesBreast Self ExaminationAudrie Allyson Gabales100% (1)
- Best New Flaps and Tips For Success in MicrosurgeryDocument12 pagesBest New Flaps and Tips For Success in MicrosurgeryDwi WicaksonoNo ratings yet
- Reoperative Plastic Surgery of The Breast (PDF)Document507 pagesReoperative Plastic Surgery of The Breast (PDF)Sang Trần100% (1)
- Free Flap PresentationDocument22 pagesFree Flap PresentationedabreoNo ratings yet
- Nipple-Areolar Complex ReconstructionDocument680 pagesNipple-Areolar Complex ReconstructionStephania Torres Pastrana y Rivera100% (2)
- A New Simple Technique For Neoumbilicoplasty: Vertical Incision and Partial Skin GraftDocument5 pagesA New Simple Technique For Neoumbilicoplasty: Vertical Incision and Partial Skin GraftJorge Luis MarcosNo ratings yet
- Master Degree in Plastic Surgery ThesisDocument117 pagesMaster Degree in Plastic Surgery ThesisMohamed Ahmed El-RoubyNo ratings yet
- (Download PDF) Plastic Surgery Craniofacial Head and Neck Surgery Pediatric Plastic Surgery 4Th Edition Geoffrey C Gurtner Full Chapter PDFDocument69 pages(Download PDF) Plastic Surgery Craniofacial Head and Neck Surgery Pediatric Plastic Surgery 4Th Edition Geoffrey C Gurtner Full Chapter PDFpjesmenessro100% (4)