Professional Documents
Culture Documents
Pulmonary Coccidioidomycosis: Pictorial Review of Chest Radiographic and CT Findings
Pulmonary Coccidioidomycosis: Pictorial Review of Chest Radiographic and CT Findings
Uploaded by
deborapkphn0 ratings0% found this document useful (0 votes)
18 views16 pagesc
Original Title
Coccidioidomycosis
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentc
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
18 views16 pagesPulmonary Coccidioidomycosis: Pictorial Review of Chest Radiographic and CT Findings
Pulmonary Coccidioidomycosis: Pictorial Review of Chest Radiographic and CT Findings
Uploaded by
deborapkphnc
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 16
Pulmonary Coccidioidomycosis :
Pictorial Review of Chest Radiographic
and CT Findings
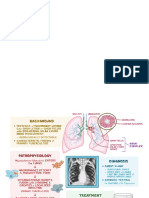
Coccidioidomycosis is a fungal The hyphal form highly infectious
infection caused by inhalation of spores (anthroconidia) inhalation
spores (anthroconidia ) from spherules rupture endospores
Coccidioides species (parasitic form) inflammation
The lungs are the target organ in Risk factors
coccidioidomycosis are involved - HIV infection
in a wide spectrum of clinical - Immunosuppressive medications
Imaging manifestations acute, - High-dose glucocorticoid
disseminated, or chronic disease administration
Diagnosis
• Sputum, bronchoalveolar lavage fluid, smear from cutaneous lesions, or
tissue biopsy samples.
• Serologic test Enzyme-linked immunoassays immunoglobulin M and
immunoglobulin G antibodies
• Bronchoscopy (Bronchoscopy is a useful diagnostic procedure if sputum
evaluation or serologic testing is not diagnostic)
• Biopsy transbronchial lung biopsy (bronkoskopi) and percutaneous
transthoracic needle biopsy with image guidance. Most biopsies are
currently performed with CT guidance.
Pulmonary Manifestations of
Coccidioidal Infection
• Acute Disease
• Disseminated
• Chronic forms
Acute Disease (primary coccidioidal infection)
Thoracic manifestations of acute coccidioidomycosis pulmonary parenchymal
abnormalities, intrathoracic adenopathy, and pleural effusion.
1. Pulmonary parenchymal abnomalities consolidation, nodules, cavities, and
peribronchial thickening
75% consolidation, (manifasting as) solitary or multiple areas of segmental or lobar
opacification . Unilateral with perihilar and basilar.
• Parenchymal opacification (varies from) a ground-glass appearance to
dense homogeneous consolidation
bacterial pneumonia
• A migratory pattern of parenchymal disease phantom infiltrates (in
which parenchymal consolidation) resolves at one site and reappears in a
different location
• 20% nodular opacities size or vary from 0.5 to 2.5 cm,
often multiple and well circumscribed, in the perihilar and
lower lung zones metastatic disease.
• Most nodules multiple and bilateral, with ill-defined
borders, and ranged between 0.5 cm and 3 cm.
• Most acute parenchymal abnormalities seen at chest radiography resolve
within 6 weeks.
2. Intrathoracic Adenopathy
Adenopathy results from regional spread of infection from pulmonary
parenchymal foci to hilar or mediastinal lymph nodes.
Hilar or mediastial adenopathy (chest radiography) ipsilateral
parenchymal consolidation, nodules, or peribronchial thickening
a. Frontal chest radiograph shows right hilar adenopathy (arrow).
b. Coronal CT image (soft-tissue window) shows extensive right hilar (white
arrow) and subcarinal (black arrow) adenopathy.
3. Pleural Effusion
15%- 20% of patients with acute coccidioidomycosis
Caused by contiguous spread of infection from adjacent parenchym
(pengaruh penyebaran infeksi dari parenkim paru).
Frontal chest radiograph shows a small right pleural effusion (arrowhead)
Disseminated Disease
Diagnosed by clinical symptoms, serologic findings, and tissue diagnosis.
Imaging of Disseminated fungemia and ARDS. Coccidioidomycosis
• miliary nodules caused by hematogenous spread
• Parenchymal consolidation
• Hilar and mediastinal adenopathy
• Extrapulmonary dissemination (occurs frequently and most commonly
involves the) skin, lymph nodes, bones and joints, central nervous
system (vertebral disease) and hematogen.
• Patients with AIDS are at increased risk of fungemia and ARDS
• Diffuse or dependent lung opacities may be seen with ARDS
Chronic Disease
Persist beyond 6 weeks
Imaging manifestations
• residual nodule,
• chronic cavity,
• persistent pneumonia with or without adenopathy,
• pleural effusion, and
• regressive changes.
Residual Pulmonary Nodule or Coccidioidoma
Chronic Coccidioidal Cavity
Differential diagnosis
primary lung malignancy
solitary metastasis
other granulomatous infection
You might also like
- Lung MycosisDocument80 pagesLung MycosisWisnu Omadi100% (2)
- Blood Pressure ChartDocument5 pagesBlood Pressure Chartmahajan1963100% (1)
- Course 5 Pleuro-Pulmonary Surgical SemiologyDocument23 pagesCourse 5 Pleuro-Pulmonary Surgical SemiologyvladutNo ratings yet
- Imaging Lung Manifestations of HIVDocument33 pagesImaging Lung Manifestations of HIVReyza HasnyNo ratings yet
- Imaging Tropical Disease 2019Document58 pagesImaging Tropical Disease 2019Rahmawati HamudiNo ratings yet
- Chronic Lower Respiratory Tract InfectionsDocument32 pagesChronic Lower Respiratory Tract Infectionsibnbasheer100% (2)
- L 5 - Lungs PathologyDocument128 pagesL 5 - Lungs PathologyDiana Popovici100% (1)
- Dr. Ali's Uworld Notes For Step 2 CKDocument40 pagesDr. Ali's Uworld Notes For Step 2 CKmarina shawkyNo ratings yet
- Lung Disease PicsDocument169 pagesLung Disease PicsDr-Mohammad Ali-Fayiz Al TamimiNo ratings yet
- Interstitial Lung Disease Diffuse Parenchymal Lung DiseaseDocument59 pagesInterstitial Lung Disease Diffuse Parenchymal Lung Diseaseapi-19641337100% (1)
- Villamor PIDSP-2019Document81 pagesVillamor PIDSP-2019April Rose Airoso - AramburoNo ratings yet
- Pneumonia Radiologi JurnalDocument6 pagesPneumonia Radiologi JurnalVania M DeviNo ratings yet
- PneumoniaDocument8 pagesPneumoniaCostescu ClaudiaNo ratings yet
- Interstitiallungdiseases VINOTH 2Document96 pagesInterstitiallungdiseases VINOTH 2podapodi870No ratings yet
- Lung AbscessDocument19 pagesLung Abscessvtyagi2377No ratings yet
- BRONKIEKTASIS BaruDocument23 pagesBRONKIEKTASIS BaruRamanda Cahya UmbarraNo ratings yet
- Respiratory MedicineDocument9 pagesRespiratory MedicineroseNo ratings yet
- Dapus 3Document10 pagesDapus 3Yan Agus AchtiarNo ratings yet
- BronchiectasisDocument25 pagesBronchiectasisDewi PermatasariNo ratings yet
- Approach To Interstitial Lung DiseasesDocument38 pagesApproach To Interstitial Lung Diseasesrahel solomonNo ratings yet
- B&lung AbscessDocument21 pagesB&lung Abscessnathan asfahaNo ratings yet
- Update Diagnosis and TherapyDocument29 pagesUpdate Diagnosis and TherapyRosi AmaliaNo ratings yet
- Radiology - Imaging of The ThoraxDocument49 pagesRadiology - Imaging of The Thoraxj.doe.hex_87No ratings yet
- Diseases of Respiratory OrgansDocument72 pagesDiseases of Respiratory OrgansEdi Kerina SembiringNo ratings yet
- Esti2015 P-0093Document36 pagesEsti2015 P-0093Irina Luciana DumitriuNo ratings yet
- Lung Abscess - Review - 2015Document13 pagesLung Abscess - Review - 2015Jonathan AiresNo ratings yet
- Journal Reading Divisi PulmonologyDocument11 pagesJournal Reading Divisi PulmonologySanrio NeuroNo ratings yet
- Imaging Pulmonary Infection, Classic Sign and Pattern PRESENTASIDocument84 pagesImaging Pulmonary Infection, Classic Sign and Pattern PRESENTASIMark Brown100% (1)
- BronchiectasisDocument60 pagesBronchiectasisArulNo ratings yet
- ANATPATH HIV 2021 S Singh With LG VoiceoverDocument59 pagesANATPATH HIV 2021 S Singh With LG VoiceoverSibabalwe DlovasheNo ratings yet
- Valeyre2015 Pulmonary SarcoidosisDocument11 pagesValeyre2015 Pulmonary SarcoidosisJohan ArocaNo ratings yet
- HIV AIDS Opportunistic InfectionsDocument26 pagesHIV AIDS Opportunistic InfectionsLaylee ClareNo ratings yet
- Nosocomial Infection. BPTDocument44 pagesNosocomial Infection. BPTAanchal GuptaNo ratings yet
- Syndrom of Consolidated Pulmonary Tissue. Pneumonia. Athelectasis. Andrei IchimDocument114 pagesSyndrom of Consolidated Pulmonary Tissue. Pneumonia. Athelectasis. Andrei IchimYan Sheng Ho100% (1)
- Aids Stuff Week 2Document4 pagesAids Stuff Week 2James MooreNo ratings yet
- Manifestations of Pulmonary Tuberculosis: Radiographic FindingsDocument24 pagesManifestations of Pulmonary Tuberculosis: Radiographic FindingsZuni TriyantiNo ratings yet
- Suppurative Lung Diseases.Document37 pagesSuppurative Lung Diseases.Salman KhanNo ratings yet
- CPC ShaDocument30 pagesCPC ShaskaruthuNo ratings yet
- Dr. Sana Bashir DPT, MS-CPPTDocument46 pagesDr. Sana Bashir DPT, MS-CPPTbkdfiesefll100% (1)
- DestructionDocument90 pagesDestructionMohamed HefnyNo ratings yet
- Enfermedad Pulmonar Cavitada: Poster No.: Congress: Type: AuthorsDocument24 pagesEnfermedad Pulmonar Cavitada: Poster No.: Congress: Type: AuthorsMarcela GarciaNo ratings yet
- Otolaryngological Manifestations of HIV/ AIDS: A ReviewDocument7 pagesOtolaryngological Manifestations of HIV/ AIDS: A ReviewFrinaensri DokiNo ratings yet
- Lung Abscess-Etiology, Diagnostic and Treatment Options: Review ArticleDocument11 pagesLung Abscess-Etiology, Diagnostic and Treatment Options: Review ArticleRickyNo ratings yet
- Study Guide 2Document16 pagesStudy Guide 2cNo ratings yet
- Interstitial Lung DiseaseDocument145 pagesInterstitial Lung DiseaseMaduka SanjeewaNo ratings yet
- Cystic and Cavitary Lung Diseases Focal and DiffuseDocument9 pagesCystic and Cavitary Lung Diseases Focal and DiffuseIndira DeviNo ratings yet
- Lung AbcessDocument11 pagesLung AbcessGul SapiNo ratings yet
- Viral Pneumoni Dari 18Document13 pagesViral Pneumoni Dari 18Yoyada SitorusNo ratings yet
- Pneumonia: Anjitha JosephDocument43 pagesPneumonia: Anjitha JosephanjithaNo ratings yet
- Cap PDFDocument23 pagesCap PDFriyaNo ratings yet
- Lung AbscessDocument40 pagesLung Abscessghhh100% (1)
- 2 Respiratory-InfectionsDocument61 pages2 Respiratory-InfectionsLana AiharaNo ratings yet
- Retropharyngeal AbscessDocument17 pagesRetropharyngeal AbscessLisa MoyoNo ratings yet
- Pulmonary TuberculosisDocument38 pagesPulmonary TuberculosisAhmed khanNo ratings yet
- Lung AbscessDocument40 pagesLung AbscessAmmad JavedNo ratings yet
- Acute Lung Abscesses. Definition of The Idea. Classification. Etiology and Pathogenesis. Clinical Picture. Diagnosis.Document6 pagesAcute Lung Abscesses. Definition of The Idea. Classification. Etiology and Pathogenesis. Clinical Picture. Diagnosis.Lucas Victor AlmeidaNo ratings yet
- Bronchiectasis OkDocument60 pagesBronchiectasis OkImmanuelNo ratings yet
- Opportunistic InfectionsDocument15 pagesOpportunistic InfectionsHimanshu MehtaNo ratings yet
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- S0022202X94976384 MainDocument4 pagesS0022202X94976384 MaindeborapkphnNo ratings yet
- Morphological Analysis of Dermatoporosis by in Vivo Reflectance Confocal Microscopy and UltrasonographyDocument9 pagesMorphological Analysis of Dermatoporosis by in Vivo Reflectance Confocal Microscopy and UltrasonographydeborapkphnNo ratings yet
- Imaging of The Post-Treatment Larynx: Suresh K. Mukherji, William J. WeadockDocument12 pagesImaging of The Post-Treatment Larynx: Suresh K. Mukherji, William J. WeadockdeborapkphnNo ratings yet
- The Association Between Skin Blood Flow and Edema On Epidermal Thickness in The Diabetic FootDocument8 pagesThe Association Between Skin Blood Flow and Edema On Epidermal Thickness in The Diabetic FootdeborapkphnNo ratings yet
- Ultrasonographic Assessment of Skin Structure According To AgeDocument8 pagesUltrasonographic Assessment of Skin Structure According To AgedeborapkphnNo ratings yet
- Ultrasonographic Subepidermal Low-Echogenic Band, Dependence of Age and Body SiteDocument7 pagesUltrasonographic Subepidermal Low-Echogenic Band, Dependence of Age and Body SitedeborapkphnNo ratings yet
- Iodinated Contrast Media and Their Adverse Reactions : Teleradiology Solutions, Bangalore, IndiaDocument7 pagesIodinated Contrast Media and Their Adverse Reactions : Teleradiology Solutions, Bangalore, IndiadeborapkphnNo ratings yet
- Neonatal Chest X-RayDocument31 pagesNeonatal Chest X-RaydeborapkphnNo ratings yet
- Giant Cell TumorDocument7 pagesGiant Cell TumordeborapkphnNo ratings yet
- LapDocument90 pagesLapdeborapkphnNo ratings yet
- A Rare Case of Chromophobe Renal Cell Carcinoma in A 55-Year-Old Female: A Case ReportDocument14 pagesA Rare Case of Chromophobe Renal Cell Carcinoma in A 55-Year-Old Female: A Case ReportdeborapkphnNo ratings yet
- Neonatal Chest X-RayDocument19 pagesNeonatal Chest X-RaydeborapkphnNo ratings yet
- PICODocument1 pagePICOdeborapkphnNo ratings yet
- MCQDocument102 pagesMCQsalamred92% (13)
- Okap Samson Uveitis PDFDocument12 pagesOkap Samson Uveitis PDFsharu4291No ratings yet
- Intravenous IbuprofenDocument13 pagesIntravenous Ibuprofenhumberto_freireNo ratings yet
- Free From Harm Final Report ResumenDocument4 pagesFree From Harm Final Report ResumenMiguel Armando Zúñiga OlivaresNo ratings yet
- Oropharyngeal and Nasopharyngeal SuctioningDocument2 pagesOropharyngeal and Nasopharyngeal SuctioningAlana Caballero100% (1)
- NiramayaDocument5 pagesNiramayaIam WaitNo ratings yet
- Jurnal - PPT Total Hip ReplacementsDocument11 pagesJurnal - PPT Total Hip ReplacementsEric GibsonNo ratings yet
- MRD Checklist: All Patient Sr. No. IPD ResponsibilitiesDocument1 pageMRD Checklist: All Patient Sr. No. IPD Responsibilitiesamit100% (5)
- New Initial Management in TraumaDocument69 pagesNew Initial Management in TraumaAhsan KhanNo ratings yet
- Chapter 1Document15 pagesChapter 1Joshua Yvan Ferrer Tordecilla100% (1)
- HCR 210 MASTER Teaching EffectivelyDocument24 pagesHCR 210 MASTER Teaching Effectivelyraj346No ratings yet
- Deviated Nasal SeptumDocument68 pagesDeviated Nasal Septumstudio53No ratings yet
- Gestational Trophoblastic DiseaseDocument37 pagesGestational Trophoblastic DiseaseOlisa 'phage' Onyebuchi100% (1)
- UNSW Response To Questions Raised Concerning Research Into The Compound DZ13Document2 pagesUNSW Response To Questions Raised Concerning Research Into The Compound DZ13ABC News OnlineNo ratings yet
- Principles of CT Scan AbdomenDocument101 pagesPrinciples of CT Scan Abdomenrajan kumar100% (16)
- TPB - List of Directory - Health and MedicalDocument21 pagesTPB - List of Directory - Health and MedicalMelai Delos Reyes CelesNo ratings yet
- Sirona Orthophos 3 Dental X-Ray - User Manual PDFDocument38 pagesSirona Orthophos 3 Dental X-Ray - User Manual PDFraeesNo ratings yet
- Skin Disease WartsDocument4 pagesSkin Disease WartsFatima Al MarzouqiNo ratings yet
- DR Balendra Pratap Singh BDS, MDS, Mams, Fisdr, Fpfa, Faamp, Icmr-If Assistant Professor Deptt. of ProsthodonticsDocument26 pagesDR Balendra Pratap Singh BDS, MDS, Mams, Fisdr, Fpfa, Faamp, Icmr-If Assistant Professor Deptt. of ProsthodonticsElavarasi GanesanNo ratings yet
- 17 - Toronto Notes 2011 - NephrologyDocument92 pages17 - Toronto Notes 2011 - NephrologyKhairulsani Yusof100% (2)
- Pharmacy Technician January 2023 - FINALDocument7 pagesPharmacy Technician January 2023 - FINALMasoomaIjazNo ratings yet
- Genetic Dis & AnaesthDocument19 pagesGenetic Dis & AnaesthaksinuNo ratings yet
- Ingrown Toenail: A Small Nail Causing A Big Pain: Healthy ToenailsDocument4 pagesIngrown Toenail: A Small Nail Causing A Big Pain: Healthy ToenailsZoganiteNo ratings yet
- Marketing ManagementDocument10 pagesMarketing ManagementRishi RohanNo ratings yet
- Health Caring Architecture LOW PDFDocument152 pagesHealth Caring Architecture LOW PDFAminaNo ratings yet
- APA DSM 5 Substance Use DisorderDocument2 pagesAPA DSM 5 Substance Use DisorderRicardo Antonio Rivas SánchezNo ratings yet
- FDA Executive Summary Dermal FillersDocument41 pagesFDA Executive Summary Dermal FillersAhmed Sad100% (1)
- Kring Abnormal Psychology Chapter 5 Mood Disorders NotesDocument14 pagesKring Abnormal Psychology Chapter 5 Mood Disorders NotesAnn Ross FernandezNo ratings yet
- Introduction To Preventive DentistryDocument27 pagesIntroduction To Preventive DentistryTin MawNo ratings yet