Professional Documents
Culture Documents
Antianginal Drugs: Roger Joseph Ii R. Jecino, M.D
Antianginal Drugs: Roger Joseph Ii R. Jecino, M.D
Uploaded by
Franz Earl Niño Albesa0 ratings0% found this document useful (0 votes)
20 views31 pagesThis document discusses drugs used to treat angina pectoris. It begins by defining terms related to coronary artery disease and angina. It then describes various classes of antianginal drugs including nitrates, beta-blockers, calcium channel blockers, and piperazineacetamide. For each drug class, it discusses mechanisms of action, indications, pharmacokinetics, contraindications, adverse effects, drug interactions, and nursing considerations. The document also covers lipid-lowering agents including bile acid sequestrants, HMG-CoA reductase inhibitors, cholesterol absorption inhibitors, fibrates, and niacin. It provides details on the mechanisms, indications, and side effects of each lipid-lower
Original Description:
Original Title
Antianginal-Drugs-1.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses drugs used to treat angina pectoris. It begins by defining terms related to coronary artery disease and angina. It then describes various classes of antianginal drugs including nitrates, beta-blockers, calcium channel blockers, and piperazineacetamide. For each drug class, it discusses mechanisms of action, indications, pharmacokinetics, contraindications, adverse effects, drug interactions, and nursing considerations. The document also covers lipid-lowering agents including bile acid sequestrants, HMG-CoA reductase inhibitors, cholesterol absorption inhibitors, fibrates, and niacin. It provides details on the mechanisms, indications, and side effects of each lipid-lower
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
20 views31 pagesAntianginal Drugs: Roger Joseph Ii R. Jecino, M.D
Antianginal Drugs: Roger Joseph Ii R. Jecino, M.D
Uploaded by
Franz Earl Niño AlbesaThis document discusses drugs used to treat angina pectoris. It begins by defining terms related to coronary artery disease and angina. It then describes various classes of antianginal drugs including nitrates, beta-blockers, calcium channel blockers, and piperazineacetamide. For each drug class, it discusses mechanisms of action, indications, pharmacokinetics, contraindications, adverse effects, drug interactions, and nursing considerations. The document also covers lipid-lowering agents including bile acid sequestrants, HMG-CoA reductase inhibitors, cholesterol absorption inhibitors, fibrates, and niacin. It provides details on the mechanisms, indications, and side effects of each lipid-lower
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 31
Antianginal Drugs
ROGER JOSEPH II R. JECINO, M.D.
Terminology
Angina pectoris – chest pain, caused by the imbalance between oxygen being supplied to the heart
muscle and demand for oxygen by the heart muscle
Atheroma – plaque in the endothelial lining of arteries
Atherosclerosis – narrowing of the arteries caused by buildup of atheromas.
Coronay Artery Disease – characterized by progressive narrowing of coronary arteries
Myocardial Infarction – end result of vessel blockage in the heart, leads to ischemia and then
necrosis of the area cut off from the blood supply.
Stable Angina – pain due to imbalance of myocardial oxygen supply and demand that is relieved
by rest.
Unstable Angina - pain due to imbalance of myocardial oxygen supply and demand that persists
even at rest.
Coronary Artery Disease
Coronary Artery Disease
Antianginal Agents
Helps restore the appropriate supply and demand ratio in oxygen
delivery to the myocardium when rest is not enough.
Improve blood flow through the following mechanisms:
Dilate blood vessels – increase the supply of oxygen
Decrease the work of the heart - decrease the demand of oxygen
Antianginal Agents
Nitrates
Beta-Blockers
Calcium Channel Blockers
Piperazineacetamide
Nitrates
Short Acting – Nitroglycerine
Long Acting – Isosorbide Dinitrate (Isordil) and Isosorbide Mononitrate
(Imdur)
Mechanism of Action
Relax and Dilate veins, arteries and capillaries allowing increase blood flow through the
coronary vessels. Dilates the Veins more than the Arteries
Dilation of arteries leads to a decrease in SVR thus leading to a drop in blood pressure thus
decreasing the afterload
Dilation of veins also leads to pooling of blood in veins and capillaries decreasing preload
Indication
Prevention and Treatment of attacks of Angina Pectoris
Pharmacokinetics:
Nitroglycerine
Sublingual
Check under the tongue
Have the patient take a sip of water before taking the medication
Caution patient not to swallow the drug
Encourage the patient to alternate sides of the tongue
Transbuccal
Check the inside of the cheeks
Caution the patient not to swallow the drug
Transdermal
When applying a new patch, always clean the are every after removing the old transdermal patch.
Intravenous
Amyl Nitrate – inhalational
ISDN/ISMN – oral forms
Contraindications and Cautions
Allergy to nitrates
Severe anemia – decrease in cardiac output could be detrimental in patients
who already has a decrease ability to deliver oxygen
Head trauma/cerebral hemorrhage – relaxation of blood vessels could
further aggravate the bleeding
Pregnancy and lactation
Caution
Hepatic and renal failure
Hypotension/hypovolemia
Conditions that limit cardiac output (e.g. cardiac tamponade)
Adverse Events
Adverse events are related to vasodilation
CNS
Headache, dizziness, and weakness
GI
Nausea, vomiting and incontinence
Cardiovascular
Hypotension, reflex tachycardia, syncope and antianginal
Transdermal patch
Contact dermatitis
Local hypersensitivity reaction
Clinically Important Drug-Drug Interaction
Ergot derivatives – increases the risk of hypertension and decreased
antianginal effect
Heparin – decreases therapeutic effect of heparin
Sildenafil – causes serious hypotension and cardiovascular events
Nursing Consideration
Assessment
Assess for contraindications or cautions
Perform physical assessment to establish baseline status before and after
beginning therapy
Skin inspection
Assess the complaint of chest pain
Assess the neurologic status
Obtain ECG as ordered to evaluate the heart rate and rhythm
Monitor laboratory results
Nursing Consideration
Nursing Diagnoses
Decreased cardiac output related to vasodilation and hypotensive effects
Risk for injury related to CNS or cardiovascular effects
Ineffective tissue perfusion related to hypotension
Deficient knowledge regarding the drug therapy
Nursing Consideration
Implementation
Give sublingual preparations under the tongue or in the buccal pouch end encourage
the patient not to swallow.
Ask the patient if the tablets fizzles or burns
Instruct the patient that a sublingual dose may be repeated in 5 minutes if relief is not
felt for a maximum of 3 doses
Give sustained release form with water, caution not to chew or crush the drug
Rotate the sites of topical forms to decrease the risk of skin abrasions and breakdown
Make sure that the translingual spray is used under the tongue and not inhaled
Beta-Blockers
MOA: blocks the stimulatory effects of the sympathetic
nervous system this results in the following:
Decrease in the excitability of heart
Decrease in the cardiac output
Decrease in the cardiac oxygen consumption
Lowering of blood pressure
Indications:
Long term treatment of angina pectoris caused by atherosclerosis
Used in combination with nitrates to increase exercise tolerance
Calcium Channel Blockers
MOA:
inhibit the movement of calcium ion across the membranes of myocardial and
arterial muscle cells, altering the action potential and blocking muscle cell
contraction.
Decreases the preload and afterload which decreases cardiac workload and
decrease oxygen consumption
Indication:
Treatment of prinzmetal angina
Treatment for chronic angina, effort associated angina and hypertension
Lipid-Lowering Agents
ROGER JOSEPH II R. JECINO, R.N., M.D.
Bile Acid Sequestrants
Drugs: Cholestyramine, colestipol, colesevelam
Mechanism of action
Bind with bile acids in the intestine to form an insoluble complex that is then excreted
in the feces.
Indications
Used to reduce serum cholesterol in patients with primary hypercholesterolemia
(manifested by high cholesterol and high LDL)
Pharmacokinetics
Not absorbed systematically
Act while in the intestine and excreted directly in the feces
Bile Acid Sequestrants
Contraindications and cautions:
Hypersensitivity reaction
Complete biliary obstruction
Abnormal intestinal function
Pregnancy and lactation
Adverse effect
Vitamin A and D deficiency
Increased bleeding tendency due to decrease absorption of vitamin K
Drug to drug interaction
Bile acid sequestrants decreases or delays the absorption of thiazide, digoxin, warfarin, thyroid
hormones, and corticosteroids. If to be taken should be 1 hour before or 4-6 after the BAS.
HMG-CoA Reductase Inhibitors
Drugs: Simvastatin, Atorbastatin, Rosuvastatin
MOA:
Blocks the early rate limiting enzyme (HMG CoA Reductase) in the synthesis of cellular cholesterol
Indications:
For patients with high cholesterol and LDL
Prevention of Myocardial Infarction in patient with multiple risk factors
Pharmacokinetics:
Absorbed in the GI tract and undergo first pass metabolism
Excreted through the feces and urine
Effective at night
Crosses the placenta and is present in milk
HMG-CoA Reductase Inhibitors
Contraindication and Cautions:
Hypersensitivity
Active liver disease and alcohol liver disease
Pregnancy and lactation
Adverse Events:
Most common: Flatulence, abdominal pain, cramps, nausea, vomiting and
constipation
Increased concentrations of liver enzymes
Acute Liver Failure
Rhabdomyolysis
Cholesterol Absorption Inhibitors
Drugs: ezetimibe
MOA: decrease the absorption of dietary cholesterol from the brush border of the
small intestine
Indication: adjunct to diet and exercise to lower cholesterol
Pharmacokinetics: absorbed well after oral administration, metabolized in the liver
and small intestine and excreted in the urine and feces
Contraindications: hypersensitivity reaction, when used with statin it should not be
used during pregnancy and lactation or with severe liver disease
Adverse effect: Mild abdominal pain and diarrhea – most common
Fibrates
Drugs: Fenofibrate and Gemfibrozil
MOA: stimulate the breakdown of lipoproteins from the tissue and
their removal in the plasma.
Fenofibrate – inhibits the triglyceride synthesis in the liver, resulting in
reduction of LDL
Indication: used for patient with high Triglyceride
Gemfibrozil – inhibits peripheral breakdown of lipids,
Indication: used for patient with high triglyceride and LDL and also in patient with low
HDL.
Vitamin B3 (Niacin)
Inhibits the release of free fatty acids from adipose tissue, increases the rate of
triglyceride removal from the plasma.
Reduces LDL and Triglyceride levels
Increases HDL levels
Decreases the levels of apoprotein
Side effect: cutaneous flushing, nausea and abdominal pain
Increases uric acid and may predispose patient to GOUT
Thank You
You might also like
- Family Medicine Remembered QuestionsDocument4 pagesFamily Medicine Remembered QuestionsPrince Du100% (1)
- Pathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFDocument62 pagesPathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFrobert.short87298% (53)
- Cardiac Med ChartsDocument6 pagesCardiac Med ChartsNursingSchoolNotes100% (15)
- Discharge PlanDocument2 pagesDischarge PlanRenee Palay50% (2)
- Updated Pediatric TB Guidelines 2019 - Guidance DocumentDocument87 pagesUpdated Pediatric TB Guidelines 2019 - Guidance Documentjaj75% (4)
- Antihypertensive Pharmacologic Agents: Nr33 K Burger, Msed, MSN, RN, CneDocument28 pagesAntihypertensive Pharmacologic Agents: Nr33 K Burger, Msed, MSN, RN, CneLopez JoeNo ratings yet
- Cardiovascular Agents: Florianne E. Adlawan, R.NDocument31 pagesCardiovascular Agents: Florianne E. Adlawan, R.NadlawanflorianneNo ratings yet
- Cardiotonic DrugsDocument67 pagesCardiotonic DrugsLady Mae Ramos100% (1)
- Drug StudyDocument6 pagesDrug StudyIrveen Joy RamirezNo ratings yet
- FINAL Drug StudyDocument9 pagesFINAL Drug StudyKristen Leigh MarianoNo ratings yet
- Drug StudyDocument6 pagesDrug StudyMaurence John Feliciano LuluquisenNo ratings yet
- DrugsDocument7 pagesDrugsEloisa Abarintos RacalNo ratings yet
- Cardiotronic MedicationsDocument13 pagesCardiotronic MedicationsTee WoodNo ratings yet
- Spironolactone: Generic Name Brand Name ClassificationDocument5 pagesSpironolactone: Generic Name Brand Name ClassificationShermalyn SalahuddinNo ratings yet
- Congestive Heart Failure: CardiacDocument36 pagesCongestive Heart Failure: CardiacHUZAIFA YAMAANNo ratings yet
- Drug Study For TetanusDocument10 pagesDrug Study For TetanusMei PayumoNo ratings yet
- Pharm ReveiwerDocument19 pagesPharm Reveiwerpinedaalexa758No ratings yet
- Drug Study ICUDocument15 pagesDrug Study ICUJulie Nambatac100% (1)
- MM MM MM MM MMM MMMMM M MM M MMMM MMMMM MMM MM MMM MM!M M!"M#MM MM M $M M %MMM MM "M "MM M MMM MDocument9 pagesMM MM MM MM MMM MMMMM M MM M MMMM MMMMM MMM MM MMM MM!M M!"M#MM MM M $M M %MMM MM "M "MM M MMM M배기숭No ratings yet
- Drugs Affecting Cardiac and Renal Systems LecDocument10 pagesDrugs Affecting Cardiac and Renal Systems LecMichelle ErikaNo ratings yet
- Emergency DrugsDocument5 pagesEmergency DrugsArra PlacidesNo ratings yet
- Drugs Action Indication Contraindication Adverse Effects Nursing ConsiderationDocument7 pagesDrugs Action Indication Contraindication Adverse Effects Nursing ConsiderationPrincess Jenelly CampomanesNo ratings yet
- UWORLDNCLEXreview2021 PDFDocument100 pagesUWORLDNCLEXreview2021 PDFmahshid kianiNo ratings yet
- Indication Specific Action Side Effects/ Adverse Effects Nursing Consideration/ Patient TeachingDocument6 pagesIndication Specific Action Side Effects/ Adverse Effects Nursing Consideration/ Patient TeachingKrista Madranca CastroNo ratings yet
- Exam 3 Study Guide PharmacologyDocument23 pagesExam 3 Study Guide PharmacologymmonsonfNo ratings yet
- Drug StudyDocument10 pagesDrug StudyHelen ReonalNo ratings yet
- A Drug Study On EpinephrineDocument7 pagesA Drug Study On EpinephrineMaesy Garcia LorenaNo ratings yet
- Medication Classificatio N Action Indication Contraindication Adverse Effect Nursing Intervention Generic Name: CNS: GIDocument4 pagesMedication Classificatio N Action Indication Contraindication Adverse Effect Nursing Intervention Generic Name: CNS: GIKathleenDawalNo ratings yet
- Drug Dosage Mechanism of Action Specific Indication Contraindicati ON Adverse Effect Nursing PrecautionDocument11 pagesDrug Dosage Mechanism of Action Specific Indication Contraindicati ON Adverse Effect Nursing PrecautionIzabela UyNo ratings yet
- ECLAMPSIA Drug StudyDocument10 pagesECLAMPSIA Drug Studyjessica_omegaNo ratings yet
- Drug Study - LeptospirosisDocument19 pagesDrug Study - LeptospirosisCamille PinedaNo ratings yet
- Drug StudyDocument7 pagesDrug StudyRenee Dwi Permata MessakaraengNo ratings yet
- Aspirin: Anticoagulants Antiplatelets & Fibronolytic (Thrombolytics) Nonsteroid Anti-Inflamatory Drugs (Nsaids)Document3 pagesAspirin: Anticoagulants Antiplatelets & Fibronolytic (Thrombolytics) Nonsteroid Anti-Inflamatory Drugs (Nsaids)Acuña MonalyNo ratings yet
- Drug StudyDocument8 pagesDrug StudyJheryck SabadaoNo ratings yet
- Drug StudyDocument14 pagesDrug StudyHannah Philene D. CalubNo ratings yet
- Medication ListDocument16 pagesMedication ListxNo ratings yet
- Ca ChannelDocument30 pagesCa ChannelKency DoneyNo ratings yet
- Drug StudyDocument23 pagesDrug StudyJoyce Anne SupnetNo ratings yet
- Drug Presentation On Anti-Hypertensive: All India Institute of Medical and Science New Delhi 2021-2022Document12 pagesDrug Presentation On Anti-Hypertensive: All India Institute of Medical and Science New Delhi 2021-2022Priya SinghNo ratings yet
- Drug StudyDocument14 pagesDrug StudyKatrina EstoconingNo ratings yet
- 10-11 Treatment of HypertensionDocument11 pages10-11 Treatment of HypertensionHanif GandohNo ratings yet
- Diazepam, Lanoxin, Hemostan, NaprexDocument6 pagesDiazepam, Lanoxin, Hemostan, NaprexRene John Francisco100% (1)
- PharmaDocument6 pagesPharmaHeid YUKINo ratings yet
- Drugs Used in HF IIDocument40 pagesDrugs Used in HF IIJamal LudinNo ratings yet
- Pharmacology: Unit VIIIDocument92 pagesPharmacology: Unit VIIIChristian Laraya AlayonNo ratings yet
- Emergency Drugs Crash CartDocument14 pagesEmergency Drugs Crash CartEricson SomeraNo ratings yet
- Drug StudyDocument3 pagesDrug Studyanon_11638632No ratings yet
- Final Drug StudyDocument22 pagesFinal Drug StudyPaula Xavier AlfalahiNo ratings yet
- Activated Charcoal: Adverse EffectsDocument14 pagesActivated Charcoal: Adverse EffectsAntonetteNo ratings yet
- BNSC CVSDocument37 pagesBNSC CVSosewapeace14No ratings yet
- NorvascDocument1 pageNorvascIsabel Barredo Del MundoNo ratings yet
- Antianginal & Vasodilating Drugs: Mrs. Davis, MSN/RN 2020Document32 pagesAntianginal & Vasodilating Drugs: Mrs. Davis, MSN/RN 2020HannaNo ratings yet
- Drugs Affecting Cardiac and Renal Systems: Jan Bazner-Chandler MSN, CNS, C-PNP, RNDocument70 pagesDrugs Affecting Cardiac and Renal Systems: Jan Bazner-Chandler MSN, CNS, C-PNP, RNromeorobin07No ratings yet
- Ix. Pharmacologic Management Brand Name Classification Indication Mechanism of Action Dosage and Frequency Adverse Reactions Nursing ConsiderationDocument21 pagesIx. Pharmacologic Management Brand Name Classification Indication Mechanism of Action Dosage and Frequency Adverse Reactions Nursing ConsiderationDizerine Mirafuentes RolidaNo ratings yet
- NCP and DSDocument6 pagesNCP and DSfranzcatchie100% (1)
- AMLODIPINEDocument3 pagesAMLODIPINEDianpratiwi22No ratings yet
- Drug StudyDocument8 pagesDrug StudySarie LevitaNo ratings yet
- Drug OrderDocument4 pagesDrug OrderVic MagtotoNo ratings yet
- Diuretics: Mrs. Davis, MSN/RN 2020Document36 pagesDiuretics: Mrs. Davis, MSN/RN 2020HannaNo ratings yet
- CVA Drug StudyDocument51 pagesCVA Drug StudyKarel LuNo ratings yet
- Drug Study (Capitol)Document8 pagesDrug Study (Capitol)Joy CalmerinNo ratings yet
- Cardiovascular PharmacologyDocument61 pagesCardiovascular PharmacologyTeeOne920% (1)
- Critical Care Medications: Anti-Arrhythmics Study Guide: Critical Care EssentialsFrom EverandCritical Care Medications: Anti-Arrhythmics Study Guide: Critical Care EssentialsNo ratings yet
- 6 - Pediatric Disorders - Rosales (P2) - AfssstDocument11 pages6 - Pediatric Disorders - Rosales (P2) - AfssstFranz Earl Niño AlbesaNo ratings yet
- Finals Schedule RubyDocument2 pagesFinals Schedule RubyFranz Earl Niño AlbesaNo ratings yet
- 4 - Imci - Orpeza - AfssstDocument19 pages4 - Imci - Orpeza - AfssstFranz Earl Niño AlbesaNo ratings yet
- NCA - 2.5 - Postpartum Complications-Labordo-saldana-serrano-sabejon-sarsozaDocument7 pagesNCA - 2.5 - Postpartum Complications-Labordo-saldana-serrano-sabejon-sarsozaFranz Earl Niño AlbesaNo ratings yet
- 17 - Fluid-Electrolyte-And-Acid-Base-Balance-Lledo-MontibonDocument14 pages17 - Fluid-Electrolyte-And-Acid-Base-Balance-Lledo-MontibonFranz Earl Niño Albesa100% (1)
- 12.2 - Community Health Nursing - Cezar - AfssstDocument14 pages12.2 - Community Health Nursing - Cezar - AfssstFranz Earl Niño AlbesaNo ratings yet
- 19 Musculoskeletal System DR - FallerDocument27 pages19 Musculoskeletal System DR - FallerFranz Earl Niño AlbesaNo ratings yet
- Nca-4.1 - Community-Health-Nursing-Orpeza-Badar-Barcelon-Berino-BerisoDocument11 pagesNca-4.1 - Community-Health-Nursing-Orpeza-Badar-Barcelon-Berino-BerisoFranz Earl Niño AlbesaNo ratings yet
- Finals Schedule SAPPHIREDocument2 pagesFinals Schedule SAPPHIREFranz Earl Niño AlbesaNo ratings yet
- Drug Classificati ON Mechanism of Action Indications Contraindications Side Effects/ Adverse Effects Nursing ConsiderationsDocument3 pagesDrug Classificati ON Mechanism of Action Indications Contraindications Side Effects/ Adverse Effects Nursing ConsiderationsFranz Earl Niño AlbesaNo ratings yet
- Drug Classification Mechanism of Action Indications Contraindications Side Effects/ Adverse Effects Nursing ConsiderationsDocument2 pagesDrug Classification Mechanism of Action Indications Contraindications Side Effects/ Adverse Effects Nursing ConsiderationsFranz Earl Niño AlbesaNo ratings yet
- Drug Classification Mechanism of Action Indications Contraindication S Side Effects/ Adverse Effects Nursing Considerations - AssessmentDocument2 pagesDrug Classification Mechanism of Action Indications Contraindication S Side Effects/ Adverse Effects Nursing Considerations - AssessmentFranz Earl Niño AlbesaNo ratings yet
- Cues Nursing Diagnosis Scientific Rationale Objectives Intervention Rationale Evaluation IndependentDocument2 pagesCues Nursing Diagnosis Scientific Rationale Objectives Intervention Rationale Evaluation IndependentFranz Earl Niño AlbesaNo ratings yet
- COMMUNICATIONDocument26 pagesCOMMUNICATIONFranz Earl Niño AlbesaNo ratings yet
- Hormones, Mitotic, Cancer Cell AntineoplasticDocument11 pagesHormones, Mitotic, Cancer Cell AntineoplasticFranz Earl Niño AlbesaNo ratings yet
- Nursing Informatics: Doña Remedios Trinidad Romualdez Medical Foundation, Inc. 2 Semester, S.Y. 2019-2020Document10 pagesNursing Informatics: Doña Remedios Trinidad Romualdez Medical Foundation, Inc. 2 Semester, S.Y. 2019-2020Franz Earl Niño AlbesaNo ratings yet
- Barcelon Antihypertensive-AgentsDocument12 pagesBarcelon Antihypertensive-AgentsFranz Earl Niño AlbesaNo ratings yet
- Dona Remedios Trinidad Romualdez Medical Foundation College of Nursing Worksheet On NCM 109 - RLE Concept: Nursing Procedures Related To Oxygenation (Respiratory System)Document18 pagesDona Remedios Trinidad Romualdez Medical Foundation College of Nursing Worksheet On NCM 109 - RLE Concept: Nursing Procedures Related To Oxygenation (Respiratory System)Franz Earl Niño AlbesaNo ratings yet
- Drugs Affecting BPDocument13 pagesDrugs Affecting BPFranz Earl Niño AlbesaNo ratings yet
- Generic Name: BeforeDocument2 pagesGeneric Name: BeforeFranz Earl Niño AlbesaNo ratings yet
- Obtaining A Capillary Blood Specimen To Measure Blood GlucoseDocument3 pagesObtaining A Capillary Blood Specimen To Measure Blood GlucoseFranz Earl Niño AlbesaNo ratings yet
- Goal Met As Evidenced byDocument2 pagesGoal Met As Evidenced byFranz Earl Niño AlbesaNo ratings yet
- M. Tuberculosis M. LepraeDocument47 pagesM. Tuberculosis M. LepraeFranz Earl Niño AlbesaNo ratings yet
- Pharmacological SheetDocument4 pagesPharmacological SheetFranz Earl Niño AlbesaNo ratings yet
- Swimming ReportDocument8 pagesSwimming ReportFranz Earl Niño AlbesaNo ratings yet
- Augmented Theory of Successful Intelligence: Launc HDocument11 pagesAugmented Theory of Successful Intelligence: Launc HFranz Earl Niño AlbesaNo ratings yet
- Code of Ethics FOR Registered NursesDocument24 pagesCode of Ethics FOR Registered NursesFranz Earl Niño AlbesaNo ratings yet
- Cardiovascular Physiology: Dr. Roger Joseph Ii R. JecinoDocument17 pagesCardiovascular Physiology: Dr. Roger Joseph Ii R. JecinoFranz Earl Niño AlbesaNo ratings yet
- Assessment of The NewbornDocument46 pagesAssessment of The NewbornFranz Earl Niño AlbesaNo ratings yet
- Technology: Andrei Philippe L. Gastones Grade 11 STEM - Avocado S.Y. 2016-2017 Mrs. Mary Jane GalanDocument1 pageTechnology: Andrei Philippe L. Gastones Grade 11 STEM - Avocado S.Y. 2016-2017 Mrs. Mary Jane GalanFranz Earl Niño AlbesaNo ratings yet
- Healthcare Quality Account 2021-22Document98 pagesHealthcare Quality Account 2021-22Adeuga ADEKUOYENo ratings yet
- CEU Ficha MED Odontologia 0721 ENDocument5 pagesCEU Ficha MED Odontologia 0721 ENEvgeni StanevNo ratings yet
- Coronary Artery Bypass Graft Surgery in Patients With Ischemic Heart FailureDocument31 pagesCoronary Artery Bypass Graft Surgery in Patients With Ischemic Heart Failuresree vidhyaNo ratings yet
- The Proportions of Term or Late Preterm Births After Exposure To Early Antenatal Corticosteroids, and Outcomes - Systematic Review and Meta-Analysis of 1.6 Million InfantsDocument13 pagesThe Proportions of Term or Late Preterm Births After Exposure To Early Antenatal Corticosteroids, and Outcomes - Systematic Review and Meta-Analysis of 1.6 Million InfantsAnnette GaspardNo ratings yet
- Practical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All ChapterDocument67 pagesPractical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All Chapterpaul.wells767100% (6)
- Robert F Kennedy Jr. Exposes Bill Gates' Vaccine Dictatorship Plan - Cites Gates' Twisted 'Messiah Complex' - Fort RussDocument1 pageRobert F Kennedy Jr. Exposes Bill Gates' Vaccine Dictatorship Plan - Cites Gates' Twisted 'Messiah Complex' - Fort RussZsi GaNo ratings yet
- Illustrated Medical Dictionary: Melloni'sDocument4 pagesIllustrated Medical Dictionary: Melloni'sAryan SinghNo ratings yet
- 1647496816893-ACT Medical Certificate FormatDocument2 pages1647496816893-ACT Medical Certificate FormatTopaNo ratings yet
- Pancreaticcancer 150917114601 Lva1 App6891Document25 pagesPancreaticcancer 150917114601 Lva1 App6891enam professorNo ratings yet
- Analisa Ergonomi Pada Penjual Jamu GEndongDocument5 pagesAnalisa Ergonomi Pada Penjual Jamu GEndongNath andNo ratings yet
- Osteoarthritis AlgorithmDocument2 pagesOsteoarthritis AlgorithmValarmaty VeerasenanNo ratings yet
- 177-Years-Medical-Experimentation Ebook Ty Charlene BollingerDocument59 pages177-Years-Medical-Experimentation Ebook Ty Charlene BollingerDan Mihaela100% (1)
- 02 CommonNBproblems 2 HandoutDocument16 pages02 CommonNBproblems 2 HandoutMisoo KimNo ratings yet
- Astasthana Pariksha - A Diagnostic Method of Yogaratnakara and Its Clinical ImportanceDocument17 pagesAstasthana Pariksha - A Diagnostic Method of Yogaratnakara and Its Clinical Importancenarayana asso100% (1)
- Financial Analysis of Ad Din FoundationDocument53 pagesFinancial Analysis of Ad Din FoundationMd. SaifullahNo ratings yet
- Lower Extremity Prosthesis Part IIDocument98 pagesLower Extremity Prosthesis Part IIsjs6r8wwv9No ratings yet
- Sexually Transmitted Diseases: Krizzia Jana P. MolinaDocument20 pagesSexually Transmitted Diseases: Krizzia Jana P. MolinaKrizzia Jana MolinaNo ratings yet
- PrimeTimes - July 2017 WKTDocument10 pagesPrimeTimes - July 2017 WKTtimesnewspapersNo ratings yet
- Kirk2007 ImportanteDocument9 pagesKirk2007 ImportanteeswaynedNo ratings yet
- Karakteristik Klinis Pasien Blefaroptosis Yang Telah Dilakukan Operasi Di Rumah Sakit Mata Cicendo - Mareta Gustia NingsihDocument8 pagesKarakteristik Klinis Pasien Blefaroptosis Yang Telah Dilakukan Operasi Di Rumah Sakit Mata Cicendo - Mareta Gustia NingsihkarinarakhmaNo ratings yet
- 4th Quarter MAPEH (HEALTHDocument6 pages4th Quarter MAPEH (HEALTHaldrinepangilinan0111No ratings yet
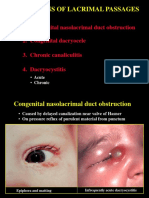
- Infections of Lacrimal PassagesDocument8 pagesInfections of Lacrimal PassagesgeorginaNo ratings yet
- Quality OrientationDocument89 pagesQuality OrientationahamedsahibNo ratings yet
- 2021 Budget Mooe GuidelinesDocument11 pages2021 Budget Mooe GuidelinesWilbert Reuyan100% (2)
- Neurotic, Stress Related and Somatoform Disorders 2Document73 pagesNeurotic, Stress Related and Somatoform Disorders 2Sonny JhaNo ratings yet
- 4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackDocument128 pages4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackVina EmpialesNo ratings yet