Professional Documents
Culture Documents
lec 8 PDL النظري
lec 8 PDL النظري
Uploaded by
حسين العراقي0 ratings0% found this document useful (0 votes)
15 views11 pagesThe periodontal ligament (PDL) is a fibrous connective tissue located between the alveolar bone and cementum. It contains collagen fibers, ground substances, fibroblasts, osteoblasts, cementoblasts, osteoclasts and blood vessels. The PDL fibers are arranged in groups including principal, gingival, alveolar crest and horizontal fibers that provide attachment of the tooth to the jaw bone and sensory functions. The PDL supports the tooth, senses pressure and touch, provides nutrition to cementum and bone, and facilitates formation of new fibers, cementum and bone through its cells.
Original Description:
Original Title
lec 8 PDL النظري
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe periodontal ligament (PDL) is a fibrous connective tissue located between the alveolar bone and cementum. It contains collagen fibers, ground substances, fibroblasts, osteoblasts, cementoblasts, osteoclasts and blood vessels. The PDL fibers are arranged in groups including principal, gingival, alveolar crest and horizontal fibers that provide attachment of the tooth to the jaw bone and sensory functions. The PDL supports the tooth, senses pressure and touch, provides nutrition to cementum and bone, and facilitates formation of new fibers, cementum and bone through its cells.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
15 views11 pageslec 8 PDL النظري
lec 8 PDL النظري
Uploaded by
حسين العراقيThe periodontal ligament (PDL) is a fibrous connective tissue located between the alveolar bone and cementum. It contains collagen fibers, ground substances, fibroblasts, osteoblasts, cementoblasts, osteoclasts and blood vessels. The PDL fibers are arranged in groups including principal, gingival, alveolar crest and horizontal fibers that provide attachment of the tooth to the jaw bone and sensory functions. The PDL supports the tooth, senses pressure and touch, provides nutrition to cementum and bone, and facilitates formation of new fibers, cementum and bone through its cells.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 11
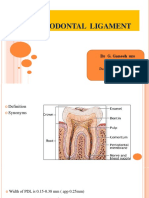
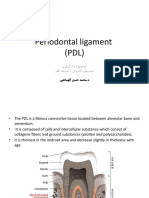
Periodontal ligament
)(PDL
المحاظرة /8النظري
قسم طب االسنان /أنسجة الفم
د.محمد حسن الهماشي
• The PDL is a fibrous connective tissue located between aleveolar bone and
cementum.
• It is composed of cells and intercellular substance which consist of
collagene fibers and ground substances (protien and polysaccharides).
• It is thinnest in the midroot area and decrease slightly in thickness with
age.
Cellular composition of PDL
Cells of PDL may be divided into three categories:
1- synthetic cells:
they have the ability to produce and secret proteins, they include:
a. Fibroblasts:
• Are the most common cells in PDL (65%) of total PDL cells.
• They are responsible for the formation of ground substance and
collagen fibers of PDL.
b. Osteoblasts:
• They are bone forming cells.
• They are covering the periodontal surface of the aleveolar bone.
c. Cementoblasts:
• Cementum forming cells.
• They are found covering the periodontal surface of the cementum
2- Resorptive cells:
a. Fibroblasts:
• They are capable of both synthesis and ingestion of PDL collagen fibers.
b. Osteoclasts:
• These cells resorb bone surface.
• Their presence on bone surface indicates that resorption was active or had recently
occurred.
c. Cementoclasts:
• They are resemble osteoclasts.
3- Other cells:
a. Progenitor cells:
• They are undifferentiated mesenchymal cells that have the capacity to undergo
mitotic division and differentiate into another type of PDL cells.
b. Epithelial cell rest of Malassez:
• These are the remnants of HERS found close to C.
• Under certain pathological conditions they can under rapid proliferation and produce
a variety of cysts or tumors.
c. Defense cells:
• These include mast cells, macrophage cells and neutrophils cells, they increase in no.
during PDL inflammation.
Blood vessels of PDL:
1. Branches from the apical vessels that supply the dental pulp.
2. Branches from the intra-alveolar vessels, these are the main branches run horizontally
penetrate the alveolar bone to enter the PDL, they are called perforated arteries.
3. Branches from the gingival vessels that enter the PDL from the gingiva.
Nerves :
The nerve supply from the maxillary and mandibular branches of the 5 th cranial nerve
(trigeminal).
Fibers of PDL:
These are made up of collagen fibers and
oxytalan fibers.
1- collagen fibers:
They form the major element with in PDL &
they include:
A. Principle fibers of PDL.
B. Gingival fibers groups.
A. Principle fibers of PDL:
• One end embedded in C. and the other end embedded in alveolar
bone.
• The embedded portion of the principle fibers are called sharpeyʼs fibers.
• These fibers can be divided into 5 groups according to the direction in
which they run in the PDL as follow:
1. Alevolar crest fibers group: they are attached to cervical part of the C.
just below C.E.J. and insert into the crest of alveolar bone.
2. Horizontal fibers group: they extend in horizontal direction from the
midroot C. to the adjacent alveolar bone.
3. Oblique fibers group: they represent the most numerous type in PDL
and run from the C. in an oblique direction to insert in alveolar bone.
4. Apical fibers group: they extend from apical C. to the adjacent alveolar
bone.
5. Interradicular fibers group: they are located between the roots of
multirooted teeth and extend perpendicular from the C. into the crest
of interradicular septa.
B.gingival fiber groups:
• These are collagen fibers which are not really from PDL.
• Their function is to attach the gingiva to the tooth.
• These bundles are arranged in groups as follows:
1. Dentogingival group: they are the most numerous, extending
from the cervical C. to the gingiva.
2. Alevologingival group: they radiate from the alveolar crest
bone to the gingiva.
3. Circular group: this small group of fibers form aband around
the neck of teeth.
4. Dentoperiosteal group: they run from the cervical C. to the
periosteum of the alveolar bone.
5. Transseptal group: these fibers are connect two adjacent
teeth, they run from the C. of one tooth over the alveolar
bone to the C. of the adjacent tooth.
2- Oxytalan fibers:
• they run vertically from apical C. and terminate in the arteries, veins
and lymphatic.
• Their function is to regulate vascular flow in relation to tooth
function.
Functions of PDL:
1. Supportive: they provide attachment for the tooth to the jaw bone.
2. Sensory: they have mechanoreceptors contribute to the pressure
and touch on the tooth.
3. Nutritive: the blood vessels in PDL provides nutritional supply to
the cementocytes in C. and to the most superficial alveolar bone
osteocytes.
4. Formative: the fibroblasts are responsible for new collagen fiber
formation, another formative function is achieved by cementoblast
and osteoblast which are essential in building up C. and alveolar
bone.
You might also like
- Eating Habits ProjectDocument31 pagesEating Habits Projectcharanleen89% (9)
- Preconception Care & Planned ParenthoodDocument7 pagesPreconception Care & Planned ParenthoodDelphy Varghese100% (8)
- Motorized Treadmill: Owner'S ManualDocument46 pagesMotorized Treadmill: Owner'S ManualMohammed ShabanNo ratings yet
- Dental PulpDocument53 pagesDental Pulpdr parveen bathla67% (3)
- The Social Construction of Contested Illness Legitimacy: A Grounded Theory AnalysisDocument21 pagesThe Social Construction of Contested Illness Legitimacy: A Grounded Theory AnalysisPelículasVeladasNo ratings yet
- Casestudy Gastric CarcinomaDocument56 pagesCasestudy Gastric CarcinomaMJ Amarillo92% (12)
- Al Mashreq College of Dentistry Oral Histology Dr. Omar Faridh Fawzi Periodontal Ligament (PDL)Document5 pagesAl Mashreq College of Dentistry Oral Histology Dr. Omar Faridh Fawzi Periodontal Ligament (PDL)Abdulrahman UdayNo ratings yet
- Periodontal Ligament: Teeth Maxillary MandibularDocument7 pagesPeriodontal Ligament: Teeth Maxillary MandibularAsfoor gake1No ratings yet
- Presentation by TarigDocument39 pagesPresentation by Tarigsamar yousif mohamedNo ratings yet
- Peridontal LigamentDocument33 pagesPeridontal Ligamentasma.aseeri123No ratings yet
- Periodontal Ligament: RIC. Dental Students Batch 1Document42 pagesPeriodontal Ligament: RIC. Dental Students Batch 1Tariq WalidNo ratings yet
- Periodontal LigamentDocument27 pagesPeriodontal Ligamentsamar yousif mohamedNo ratings yet
- PerioDontal LigamentDocument18 pagesPerioDontal LigamentDENTALORG.COMNo ratings yet
- Periodontium (4) : Periodontal LigamentsDocument6 pagesPeriodontium (4) : Periodontal Ligamentsمحمد محمود القحيفNo ratings yet
- Periodontal LigamentDocument56 pagesPeriodontal LigamentPurwana Nasir100% (2)
- Sulcular Epithelium:: Periodontics Lec. 2Document7 pagesSulcular Epithelium:: Periodontics Lec. 2زهرة الحبNo ratings yet
- Periodontal Ligament: Ganesh Ganji 2 Year PGDocument34 pagesPeriodontal Ligament: Ganesh Ganji 2 Year PGNareshNo ratings yet
- Periodontal LigamentDocument65 pagesPeriodontal LigamentReshmaa Rajendran100% (1)
- Null 2Document45 pagesNull 2moh.ahm3040No ratings yet
- Periodontal LigamentDocument43 pagesPeriodontal LigamentShashi kiran0% (1)
- Periodontal LigamentDocument56 pagesPeriodontal LigamentDent DealsNo ratings yet
- 1.attachment Apparatus (Part I) Periodontal LigamentDocument43 pages1.attachment Apparatus (Part I) Periodontal Ligamentsaged loaiNo ratings yet
- 4 - The Periodontium (Mahmoud Bakr)Document128 pages4 - The Periodontium (Mahmoud Bakr)MobarobberNo ratings yet
- Presentation Orthodontic - Removed 2Document16 pagesPresentation Orthodontic - Removed 2nabafuad98No ratings yet
- Orthodontic M.MDocument17 pagesOrthodontic M.Mnabafuad98No ratings yet
- - periodontal Ligament Ppt - نسخةDocument43 pages- periodontal Ligament Ppt - نسخةkoka51339No ratings yet
- Pulp and PDLDocument37 pagesPulp and PDLamna faridNo ratings yet
- Semina 2periodontal Ligament NUSDocument102 pagesSemina 2periodontal Ligament NUSnusreenNo ratings yet
- Dental Pulp Lecture 3Document10 pagesDental Pulp Lecture 3Mohamed Harun B. SanohNo ratings yet
- Oral. H Lec.12Document4 pagesOral. H Lec.12Abdulrahman UdayNo ratings yet
- 5pdl 190625130010 2Document88 pages5pdl 190625130010 2khaled alahmadNo ratings yet
- Gingiva 2Document32 pagesGingiva 2samar yousif mohamedNo ratings yet
- Screenshot 2024-06-24 at 2.48.14 PMDocument17 pagesScreenshot 2024-06-24 at 2.48.14 PMايمن صباح عبد حماديNo ratings yet
- Lec 9 Alveolar BoneDocument10 pagesLec 9 Alveolar Boneحسين العراقي0% (1)
- PeriodontiumDocument86 pagesPeriodontiumShahzeb MemonNo ratings yet
- Presentation Orthodontic - RemovedDocument12 pagesPresentation Orthodontic - Removednabafuad98No ratings yet
- Cartilage: Histology Part 1: Module2, Unit 2Document30 pagesCartilage: Histology Part 1: Module2, Unit 2Obansa JohnNo ratings yet
- Functions of BoneDocument7 pagesFunctions of BoneDTM FHKNo ratings yet
- Periodontal LigamentDocument38 pagesPeriodontal LigamentyogeshNo ratings yet
- Anatomy Lec-2Document25 pagesAnatomy Lec-2aminqasm111No ratings yet
- Human Cell TypesDocument75 pagesHuman Cell Typesmegamemory14No ratings yet
- Oral Lec 8Document9 pagesOral Lec 8Adam AliraqiNo ratings yet
- Periodontal LigamentDocument47 pagesPeriodontal LigamentPrerna KrishanNo ratings yet
- 3 Periodontal LigamentDocument34 pages3 Periodontal LigamentAisha AldossaryNo ratings yet
- Animal OrganizationDocument6 pagesAnimal OrganizationAldi RegarNo ratings yet
- Pulp Lec.8 2018Document5 pagesPulp Lec.8 2018Safura IjazNo ratings yet
- Root DevelopmentDocument16 pagesRoot DevelopmentElena CristinaNo ratings yet
- Tissue Types and Cell ModificationDocument47 pagesTissue Types and Cell ModificationBheya Samantha MontieroNo ratings yet
- Periodontal LigamentDocument103 pagesPeriodontal Ligamentanukbhatgmail.com anukbhatgmail.comNo ratings yet
- Periodontal Ligament: by Helen R. Hallare, DDMDocument34 pagesPeriodontal Ligament: by Helen R. Hallare, DDMceudmd3dNo ratings yet
- Organization of Living BeingsDocument6 pagesOrganization of Living BeingsSanhitha RameshNo ratings yet
- The Periodontal Ligament A Link Between The Cementum and Alveolar BoneDocument18 pagesThe Periodontal Ligament A Link Between The Cementum and Alveolar BoneAthenaeum Scientific PublishersNo ratings yet
- Genbio2 Week 2Document39 pagesGenbio2 Week 2Noel Vincent AgonoyNo ratings yet
- 15 Pulpa Gigi (DRG Tetiana)Document40 pages15 Pulpa Gigi (DRG Tetiana)abiyuNo ratings yet
- Periodontal Ligament 1Document60 pagesPeriodontal Ligament 1ashishubaNo ratings yet
- Ingles Medico I: Epithelial TissuesDocument3 pagesIngles Medico I: Epithelial TissuesSamuel RomeroNo ratings yet
- CartilageDocument33 pagesCartilageRahaf MajadlyNo ratings yet
- Pulpal and Periradicular Histology and PathologyDocument15 pagesPulpal and Periradicular Histology and PathologyAmin HedayatpourNo ratings yet
- Dental Pulp: University of Djilali Liables Faculty of Medecine Taleb Mourad Departement of DentistryDocument42 pagesDental Pulp: University of Djilali Liables Faculty of Medecine Taleb Mourad Departement of DentistryjoumanaNo ratings yet
- Histology and Physiology of The Dental Pulp: Dr. Shibu Thomas MathewDocument27 pagesHistology and Physiology of The Dental Pulp: Dr. Shibu Thomas MathewLammo BlwNo ratings yet
- 6 PulpDocument12 pages6 Pulpahmedfawakh0No ratings yet
- Periodontium 4Document45 pagesPeriodontium 4shahzeb memonNo ratings yet
- Advanced farriery knowledge: A study guide and AWCF theory course companionFrom EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNo ratings yet
- lec 8 PDL النظريDocument11 pageslec 8 PDL النظريحسين العراقيNo ratings yet
- Lec 11 Arrangment of TeethDocument24 pagesLec 11 Arrangment of Teethحسين العراقيNo ratings yet
- Lec 9 Alveolar BoneDocument10 pagesLec 9 Alveolar Boneحسين العراقي0% (1)
- Lec 10 Selection of Artificial TeethDocument19 pagesLec 10 Selection of Artificial Teethحسين العراقيNo ratings yet
- Lec 6+7 Oral H.Document35 pagesLec 6+7 Oral H.حسين العراقيNo ratings yet
- Information Systems For Healthcare Management Eighth Edition 8Th Edition Full ChapterDocument41 pagesInformation Systems For Healthcare Management Eighth Edition 8Th Edition Full Chapterarnold.kluge705100% (24)
- WHH Vacancy Announcement - WASH Field OfficerDocument2 pagesWHH Vacancy Announcement - WASH Field OfficerAwes SewsaNo ratings yet
- Osorio Ii Elementary School Referral System For Students in Crisis Physically, Verbally or Sexual AbuseDocument8 pagesOsorio Ii Elementary School Referral System For Students in Crisis Physically, Verbally or Sexual AbuseBenj AlejoNo ratings yet
- Alabama K-12 School Facilities 2022 - List of ProjectsDocument13 pagesAlabama K-12 School Facilities 2022 - List of ProjectsTrisha Powell CrainNo ratings yet
- Physiology of TasteDocument45 pagesPhysiology of TasteDaffa YudhistiraNo ratings yet
- Skin Disease in DogsDocument18 pagesSkin Disease in DogsBibek SutradharNo ratings yet
- Iris Peabody Vanderbilt Edu-ResourcesDocument3 pagesIris Peabody Vanderbilt Edu-ResourcesEdward Fabian SanchezNo ratings yet
- Health Talk DehydrationDocument19 pagesHealth Talk DehydrationrizwanNo ratings yet
- Reasons Why A Child Becomes A Bully: BullyingDocument2 pagesReasons Why A Child Becomes A Bully: BullyingKeran VarmaNo ratings yet
- An Unusual Case of Corpse Dismemberment: Tomasz Konopka, MD, PHD, Filip Bolechała, MD, and Marcin Strona, MDDocument3 pagesAn Unusual Case of Corpse Dismemberment: Tomasz Konopka, MD, PHD, Filip Bolechała, MD, and Marcin Strona, MDGabriel GabrielNo ratings yet
- Journal of Cranio-Maxillo-Facial Surgery: Matthias Zimmermann, Emeka NkenkeDocument6 pagesJournal of Cranio-Maxillo-Facial Surgery: Matthias Zimmermann, Emeka Nkenkekarla gonzalezNo ratings yet
- Periodontal Disease As A Specific, Albeit Chronic, Infection: Diagnosis and TreatmentDocument26 pagesPeriodontal Disease As A Specific, Albeit Chronic, Infection: Diagnosis and TreatmentGali Alfaro ZagalNo ratings yet
- MS PRO Portable by MEDICALSOFTDocument19 pagesMS PRO Portable by MEDICALSOFTNagoya Grampus EightNo ratings yet
- Community Health Centre Organization and FunctionsDocument10 pagesCommunity Health Centre Organization and FunctionsKailash NagarNo ratings yet
- Creatine Supplementation Elicits Greater Muscle Hypertrophy in Upper Than Lower Limbs and Trunk in Resistance Trained MenDocument8 pagesCreatine Supplementation Elicits Greater Muscle Hypertrophy in Upper Than Lower Limbs and Trunk in Resistance Trained MenRodrigo CamposNo ratings yet
- Shadow Work Journal Prompts Illustrated PDFDocument51 pagesShadow Work Journal Prompts Illustrated PDFkkccNo ratings yet
- Assessment of New BornDocument58 pagesAssessment of New BornEllen Angel100% (2)
- UNK Summer Graduate ListDocument4 pagesUNK Summer Graduate ListNTV NewsNo ratings yet
- Clean and Hygienic Comfort Room Action PlanDocument2 pagesClean and Hygienic Comfort Room Action Plankariza pugalNo ratings yet
- Nutrient Content of Rabbit Meat As Compared To Chicken, Beef and Pork MeatDocument7 pagesNutrient Content of Rabbit Meat As Compared To Chicken, Beef and Pork Meatjohar MohammadNo ratings yet
- 2023 AHA CPR Training 3opportunities 1Document1 page2023 AHA CPR Training 3opportunities 1ramonenfermagemnotraumaNo ratings yet
- Hiphop Dance Performance RubricDocument2 pagesHiphop Dance Performance RubricIrvin Aaron Amigable100% (1)
- Chapter 1Document7 pagesChapter 1WATI KAKINo ratings yet
- SOWK6274 Course Outline 2022-23 (Website)Document9 pagesSOWK6274 Course Outline 2022-23 (Website)Ccc MrNo ratings yet
- Breastfeeding (Pagpaduruh)Document17 pagesBreastfeeding (Pagpaduruh)Meryana SalaNo ratings yet