Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
408 viewsMental Health Admission & Discharge Dip Nursing
Mental Health Admission & Discharge Dip Nursing
Uploaded by
Muranatu CynthiaMental health admissions can be either voluntary or involuntary based on an assessment of the risks posed and treatment needs. Admission involves evaluating the individual's mental state, needs, and risks to determine the appropriate level of observation and care plan. Discharge planning requires coordination between medical professionals, the patient, and family to facilitate community support services and continued treatment post-discharge.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Pediatric Mental Status Exam: General AppearanceDocument3 pagesPediatric Mental Status Exam: General AppearanceZelel GaliNo ratings yet
- Drug Study: Davao Doctors College General Malvar ST., Davao City Nursing ProgramDocument3 pagesDrug Study: Davao Doctors College General Malvar ST., Davao City Nursing ProgramJear RomeroNo ratings yet
- Precipitated Labour 1Document8 pagesPrecipitated Labour 1priyankaNo ratings yet
- Anxiety Disorder and Case PresentationDocument52 pagesAnxiety Disorder and Case Presentationmulanako0% (1)
- Nursing Management of Patients With DementiaDocument9 pagesNursing Management of Patients With DementiaSabita Paudel60% (5)
- Rle AssDocument5 pagesRle AssMikaCasimiroBalunanNo ratings yet
- Case Presentation On CannabisDocument85 pagesCase Presentation On CannabisKisna BhurtelNo ratings yet
- The Burden On The Family of A Psychiatric Patient - Development of An Interview Schedule Pai1981 PDFDocument5 pagesThe Burden On The Family of A Psychiatric Patient - Development of An Interview Schedule Pai1981 PDFHarish Kumar100% (1)
- BpadDocument27 pagesBpadnikitabhattarai20No ratings yet
- HIV CounsellingDocument14 pagesHIV CounsellingEldho SabuNo ratings yet
- Psychiatric Nursing - Mental Status ExaminationDocument4 pagesPsychiatric Nursing - Mental Status ExaminationChien Lai R. BontuyanNo ratings yet
- Application - of - Theory - in - NursingDocument9 pagesApplication - of - Theory - in - Nursingako at ang exo100% (1)
- Mental Status Examination (MSE)Document13 pagesMental Status Examination (MSE)Pia Mae Buaya100% (1)
- Human Rights of Mentally IllDocument5 pagesHuman Rights of Mentally IllShyam100% (2)
- Case 2Document8 pagesCase 2Kreshnik IdrizajNo ratings yet
- Organic Mental Disorder: Presented By: Priyanka Kumari M.Sc. NursingDocument50 pagesOrganic Mental Disorder: Presented By: Priyanka Kumari M.Sc. NursingHardeep KaurNo ratings yet
- The Psychiatric Mental Status Exam (MSE)Document4 pagesThe Psychiatric Mental Status Exam (MSE)dev100% (1)
- Bipolar NCPDocument2 pagesBipolar NCPAngel BunolNo ratings yet
- Mental Retardation Treatment and ManagementDocument12 pagesMental Retardation Treatment and ManagementMelchoniza CalagoNo ratings yet
- Choithram College of NursingDocument16 pagesChoithram College of NursingMonikaNo ratings yet
- A Descriptive Study To Assess The Knowledge Regarding Substance Abuse and Ill Effects Among P.U. Students in The Selected P.U. College of BagalkotDocument3 pagesA Descriptive Study To Assess The Knowledge Regarding Substance Abuse and Ill Effects Among P.U. Students in The Selected P.U. College of BagalkotInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Report of Field Visit To National Centre For Disease ControlDocument12 pagesReport of Field Visit To National Centre For Disease ControlVaishali JainarainNo ratings yet
- Format MSEDocument3 pagesFormat MSESubir Banerjee0% (1)
- Pragyan College of Nursing Bhopal, M.P.: Subject - Mental Health Nursing TopicDocument11 pagesPragyan College of Nursing Bhopal, M.P.: Subject - Mental Health Nursing Topicannu100% (1)
- Seminar 7Document27 pagesSeminar 7Arya Lekshmi100% (1)
- Role of Ophthalmic Nurses With Visually Impaired PatientsDocument6 pagesRole of Ophthalmic Nurses With Visually Impaired PatientsIsaac Aleman0% (1)
- Family Health Nursing: Ms - Neethu Vincent Asst Professor KVM College of NursingDocument9 pagesFamily Health Nursing: Ms - Neethu Vincent Asst Professor KVM College of NursingNeethu VincentNo ratings yet
- Rehabilitation and RecoveryDocument29 pagesRehabilitation and RecoveryImad khanNo ratings yet
- Concept of PsychobiologyDocument21 pagesConcept of Psychobiologydhivyaram100% (1)
- Mental Health Act PDFDocument40 pagesMental Health Act PDFAnilkumar JaraliNo ratings yet
- Admission and Discharge of A Client in Psychiatric UnitDocument18 pagesAdmission and Discharge of A Client in Psychiatric UnitMahipal singh pacharNo ratings yet
- Role and Functions of Psychiatry NurseDocument20 pagesRole and Functions of Psychiatry NurseDhAiRyA ArOrANo ratings yet
- Organic Brain DisorderDocument69 pagesOrganic Brain DisorderHowell Mathew100% (1)
- Unit 6 NJDocument6 pagesUnit 6 NJmaakkanNo ratings yet
- OT7 - Outcome of Occupational Therapy GroupDocument17 pagesOT7 - Outcome of Occupational Therapy GroupAnnbe BarteNo ratings yet
- Importance and Purposes of ResearchDocument3 pagesImportance and Purposes of ResearchKarl Kiw-isNo ratings yet
- Communication and IprDocument12 pagesCommunication and IprDebashrita MisraNo ratings yet
- Mental Health TeamDocument3 pagesMental Health Teammanu sethiNo ratings yet
- Mhn-Issues, Trends, Magnitude, Contemporary Practice HealthDocument15 pagesMhn-Issues, Trends, Magnitude, Contemporary Practice HealthAna MikaNo ratings yet
- Behavior TherapyDocument23 pagesBehavior TherapydhivyaramNo ratings yet
- Process Recording ExampleDocument4 pagesProcess Recording ExampleChristine FernandoNo ratings yet
- Role - Responsibilities of Psychiatry Health NurseDocument3 pagesRole - Responsibilities of Psychiatry Health NurseDhAiRyA ArOrANo ratings yet
- Recreational Therapy Presentee: Sukhdeep Kaur Msc. (N) 1 YearDocument26 pagesRecreational Therapy Presentee: Sukhdeep Kaur Msc. (N) 1 YearSatbir GillNo ratings yet
- Mental Status Examination - Bring To LectureDocument6 pagesMental Status Examination - Bring To LectureJae ChoiNo ratings yet
- Attributes and Skills Required For A CounsellorDocument7 pagesAttributes and Skills Required For A Counsellorgasto mkonoNo ratings yet
- Ect ProcedureDocument11 pagesEct ProcedureDhAiRyA ArOrANo ratings yet
- Mini Mental Status ExamDocument10 pagesMini Mental Status ExamFrench Pastolero-ManaloNo ratings yet
- Electroconvulsive TherapyDocument9 pagesElectroconvulsive TherapyRoanne LaguaNo ratings yet
- Alternative System of MedicineDocument13 pagesAlternative System of MedicineDebipriya Mistry100% (1)
- Legal Issues in Mental Health NursingDocument61 pagesLegal Issues in Mental Health NursingS KANIMOZHINo ratings yet
- Restraining Procedure: General Principles For Use of RestraintsDocument10 pagesRestraining Procedure: General Principles For Use of RestraintsHardeep KaurNo ratings yet
- Recreational TherapyDocument22 pagesRecreational TherapyKishore RathoreNo ratings yet
- MHN, I (U), 6Document51 pagesMHN, I (U), 6akilaNo ratings yet
- Mental Health ContinuumDocument5 pagesMental Health ContinuumrajithapavalurNo ratings yet
- Rehabilitation of The AgedDocument31 pagesRehabilitation of The Agededward osae-oppong100% (1)
- Restraint and Seclusion ppt-2Document22 pagesRestraint and Seclusion ppt-2api-233645719100% (2)
- Sanjivani Psychosocial Rehabilitation Centre, Nedumkunnam, Kottayam DT., KeralaDocument3 pagesSanjivani Psychosocial Rehabilitation Centre, Nedumkunnam, Kottayam DT., KeralaJSM MKZYNo ratings yet
- Hospital Admission To Discharge 13 3 12 OkDocument3 pagesHospital Admission To Discharge 13 3 12 OkHarry Wahyudhy UtamaNo ratings yet
- AHM 540 Acute Care Part 1Document11 pagesAHM 540 Acute Care Part 1abul kalam AzadNo ratings yet
- Presented By-Ms. Yashodhara Ghosh Sen Asistant Professor Ion, BwuDocument63 pagesPresented By-Ms. Yashodhara Ghosh Sen Asistant Professor Ion, BwuyashodharaNo ratings yet
- 3-Physical-Therapist As Patient ManagerDocument38 pages3-Physical-Therapist As Patient ManagerRomana VayaniNo ratings yet
- Hospital Admission and DischargeDocument21 pagesHospital Admission and DischargeYogesh ChandraNo ratings yet
- Beta - Lactam Antibiotics: Prof. R. K. Dixit Pharmacology and Therapeutics K. G. M. U. LucknowDocument29 pagesBeta - Lactam Antibiotics: Prof. R. K. Dixit Pharmacology and Therapeutics K. G. M. U. LucknowHely PatelNo ratings yet
- GuidelinesDocument26 pagesGuidelinesmsc3nNo ratings yet
- Bahan Ajar Kusta & Frambusia PLKNDocument124 pagesBahan Ajar Kusta & Frambusia PLKNpetty arianiNo ratings yet
- Chest Pain Case Write-Up - Doctoring IIIDocument4 pagesChest Pain Case Write-Up - Doctoring IIIchristietwongNo ratings yet
- 12i3uasd Asdhgas D WawanDocument9 pages12i3uasd Asdhgas D Wawanwaluyo ningratNo ratings yet
- 15 Drugs QP Igcse Cie BiologyDocument7 pages15 Drugs QP Igcse Cie BiologyHay Thar TunNo ratings yet
- Abcs of Trauma CareDocument65 pagesAbcs of Trauma CareBeaulah HunidzariraNo ratings yet
- Mitral Valve SurgeryDocument2 pagesMitral Valve SurgeryLena MarieNo ratings yet
- Mental Heath and Ability To WorkDocument4 pagesMental Heath and Ability To Workgladiola janiNo ratings yet
- Zentel 400 MG Tablets GDS23Document6 pagesZentel 400 MG Tablets GDS23Vartika AgarwalNo ratings yet
- EtopexDocument11 pagesEtopexMohammed HaiderNo ratings yet
- Hamal Ko Roknay Ke TareekayDocument1 pageHamal Ko Roknay Ke TareekayAsad ImranNo ratings yet
- Medical Imaging Units SpecsDocument12 pagesMedical Imaging Units Specsar nedungadiNo ratings yet
- The Amazing Cordyceps MushroomDocument63 pagesThe Amazing Cordyceps MushroomSyncOrSwimNo ratings yet
- Herepes PDFDocument8 pagesHerepes PDFsuruthiNo ratings yet
- Fluid Electrolyte ImbalanceDocument15 pagesFluid Electrolyte ImbalancePrasanth Kurien Mathew100% (9)
- 1 s2.0 S1930043321003083 MainDocument5 pages1 s2.0 S1930043321003083 MainSandra ArellanoNo ratings yet
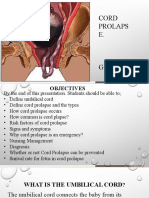
- Cord Prolaps E.: Jens MartenssonDocument19 pagesCord Prolaps E.: Jens MartenssonPeter YanksonNo ratings yet
- Heartcode Complete Bls Provider: Basic Life SupportDocument2 pagesHeartcode Complete Bls Provider: Basic Life SupportNayan ShrivastavaNo ratings yet
- EBN Diarrhea OrasolDocument8 pagesEBN Diarrhea Orasolcharm_peñaNo ratings yet
- Survival GuideDocument4 pagesSurvival Guideeclipse1130No ratings yet
- Laboratory For Medical Tests: Test ReportDocument2 pagesLaboratory For Medical Tests: Test ReportAdnana AndreeaNo ratings yet
- Strategi Kesinambungan Perniagaan Semasa Krisis Pandemik Covid-19: Kajian Rantaian Pengagihan Produk Pertanian Pekebun KecilDocument8 pagesStrategi Kesinambungan Perniagaan Semasa Krisis Pandemik Covid-19: Kajian Rantaian Pengagihan Produk Pertanian Pekebun KecilZuriani YanieNo ratings yet
- An Awareness Session On Blood Donation and Its ImportanceDocument40 pagesAn Awareness Session On Blood Donation and Its Importancekushi krishnaNo ratings yet
- Peritonitis TreatmentDocument3 pagesPeritonitis TreatmentMRFNo ratings yet
- Doctor Information UPDATEDocument40 pagesDoctor Information UPDATERishika BaranwalNo ratings yet
- A Case Study of DIBH To Spare Abdominal Organs at Risk For Renal Cell Carcinoma MR-Guided RadiotherapyDocument14 pagesA Case Study of DIBH To Spare Abdominal Organs at Risk For Renal Cell Carcinoma MR-Guided Radiotherapyapi-525837437No ratings yet
Mental Health Admission & Discharge Dip Nursing
Mental Health Admission & Discharge Dip Nursing
Uploaded by
Muranatu Cynthia0 ratings0% found this document useful (0 votes)
408 views7 pagesMental health admissions can be either voluntary or involuntary based on an assessment of the risks posed and treatment needs. Admission involves evaluating the individual's mental state, needs, and risks to determine the appropriate level of observation and care plan. Discharge planning requires coordination between medical professionals, the patient, and family to facilitate community support services and continued treatment post-discharge.
Original Description:
Original Title
Mental Health Admission & Discharge Dip Nursing.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentMental health admissions can be either voluntary or involuntary based on an assessment of the risks posed and treatment needs. Admission involves evaluating the individual's mental state, needs, and risks to determine the appropriate level of observation and care plan. Discharge planning requires coordination between medical professionals, the patient, and family to facilitate community support services and continued treatment post-discharge.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
408 views7 pagesMental Health Admission & Discharge Dip Nursing
Mental Health Admission & Discharge Dip Nursing
Uploaded by
Muranatu CynthiaMental health admissions can be either voluntary or involuntary based on an assessment of the risks posed and treatment needs. Admission involves evaluating the individual's mental state, needs, and risks to determine the appropriate level of observation and care plan. Discharge planning requires coordination between medical professionals, the patient, and family to facilitate community support services and continued treatment post-discharge.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 7
Mental Health
Admission & Discharge
Diploma Nursing
Lecturer: Donald Conteh
Mental Health Admission
• The decision to admit a person in a Psychiatric Hospital is based on the nature of the
mental distress or psychological difficulties; duration of the psychological difficulties;
disability and deterioration on the level of daily function as a result of the psychological
difficulty and significant risk to self and / or others.
• Admission in a mental health hospital is either an informal (voluntary) or restricted
(involuntary) admission and based on a Mental Health Act.
• Voluntary Admission: the patient voluntarily agrees to hospital admission; and is not
deem by the Psychiatrist to be a danger to self and other; and agrees to the treatment
plan including medication compliance.
• Involuntary admission: the patient with mental illness and who is deem to be a danger
to self and / or others is admitted to an approved mental health hospital against his/ her
will; and not allowed to leave the hospital unless given leave of absence by psychiatrist
or senior mental health nurse. The person may be detained on a Mental Health Act.
• The psychiatrist must be satisfied that the person has a mental illness and needed
treatment that is available in the hospital and without the treatment the person’s health
will deteriorate.
• The Mental Health Act should guide the admission. For a person to be detained he/ she
must have been diagnosed with mental illness or impaired or suffering from a
psychopathic disorder; the treatment required must be available only in the hospital
Admission (cont)
• The admission procedure is initiated with an assessment of the
person’s mental state using validated tools such as TAG, level of risk
and support systems.
• The assessing practitioner also considers the person’s behaviour in
the past 48 hours and deterioration in the level of functioning.
• The assessment should consider what is most relevant to meet the
person’s needs and to utilize the strength of the person, which will
result in reduced risk of causing additional stress during the course of
the assessment.
• Following the of needs and level of risk, the assessing practitioner
mostly psychiatrist or a senior mental health nurse advice on the level
of observation that is to be placed on the person during the initial
days of admission. The observation level should be reviewed on an
on-going basis and should reflect the principle of least restriction.
Admission (cont)
• Admission to hospital is a potentially distressing experience for the patient, carer
and relevant others. Therefore, staff should be aware of the patient and family
potential emotions and must provide information and support to them
throughout the admission procedure.
• The provided information should be given in a manner that reflect all care
options, embraces the principles of recovery and should convey hope. The
information should be clear about the reasons of the patient’s admission, tailored
to the needs of the patient’s, carer and relevant others.
• The patient should be assigned to a named nurse on the ward and his/ her role
identified to the patient so as to enable trust, build a therapeutic relationship and
enhance confidence to devolve information.
• The mental health nurse should be aware of the patient lack of ability to absorb
information at the time of distress and environmental change.
Admission (cont)
• The mental health nurse should inform relevant practitioner and
agencies that were engaged with the patient care about the
admission and request relevant information.
• The social needs of the patient should be considered as early as
possible on admission in order to allow a multi-disciplinary approach
to support the patient following discharge.
• The planning of the patient’s recovery journey must be patient-
centred taking into consideration the assessment of needs and care
planning approach.
• The care plan must address the nursing diagnosis such as
hallucination ( hearing voices); and planning should involve the
patient so as to promote share understanding of the recovery-focused
interventions
Discharge
• The discharge planning requires dedicate time for discussion in a ward
round or clinical meeting involved the patient, nearest family and relevant
professionals and agencies; to agree on interventions and facilitate required
support; making the patient’s transition back home as smoothly as possible.
• There should be updated progress medical and nursing records, current risk
assessment and management plan, contingency plan, and information
about community services for support and follow-up appointment to be
provided to the patient and family in the discharge meeting.
• The discharge of the patient should be well-planned and coordinated
through proper multidisciplinary meetings in the hospital involving all
relevant practitioners and/ or agencies.
• There should be prescribed medication on discharge.
• All communications must be recorded accurately and comprehensively; and
with a thorough care plan with explicit details about follow-up of the
patient and written in a format that the patient and carer understands.
Discharge Follow-up
• The discharge patient should be referred to a Home Treatment Treatment (if
available)
• The patient should be provided 48 Hours follow-up with a Psychiatrist in an Out-
patient clinic to review progress and medication compliance at home.
• If the patient is suffering from a severe and enduring mental illness and/ or a risk
to self and others, he/she should be allocated to a Community Psychiatric Nurse
for case management.
• The patient should be provide initially 3-monthly follow-up and subsequently 6-
monthly follow-up appointments as regular review of mental state and efficacy of
prescribed medication.
Reference
• National Health Service (2009) Admissions to Mental Health Inpatient Services.
Scotland. NHS Quality Improvement
• Ndetei, DM. Szabo, CP. Okasah, T. Mburu, JM (2006) The African textbook of
Clinical Psychiatry and Mental Health. Kenya, AMREF.
You might also like
- Pediatric Mental Status Exam: General AppearanceDocument3 pagesPediatric Mental Status Exam: General AppearanceZelel GaliNo ratings yet
- Drug Study: Davao Doctors College General Malvar ST., Davao City Nursing ProgramDocument3 pagesDrug Study: Davao Doctors College General Malvar ST., Davao City Nursing ProgramJear RomeroNo ratings yet
- Precipitated Labour 1Document8 pagesPrecipitated Labour 1priyankaNo ratings yet
- Anxiety Disorder and Case PresentationDocument52 pagesAnxiety Disorder and Case Presentationmulanako0% (1)
- Nursing Management of Patients With DementiaDocument9 pagesNursing Management of Patients With DementiaSabita Paudel60% (5)
- Rle AssDocument5 pagesRle AssMikaCasimiroBalunanNo ratings yet
- Case Presentation On CannabisDocument85 pagesCase Presentation On CannabisKisna BhurtelNo ratings yet
- The Burden On The Family of A Psychiatric Patient - Development of An Interview Schedule Pai1981 PDFDocument5 pagesThe Burden On The Family of A Psychiatric Patient - Development of An Interview Schedule Pai1981 PDFHarish Kumar100% (1)
- BpadDocument27 pagesBpadnikitabhattarai20No ratings yet
- HIV CounsellingDocument14 pagesHIV CounsellingEldho SabuNo ratings yet
- Psychiatric Nursing - Mental Status ExaminationDocument4 pagesPsychiatric Nursing - Mental Status ExaminationChien Lai R. BontuyanNo ratings yet
- Application - of - Theory - in - NursingDocument9 pagesApplication - of - Theory - in - Nursingako at ang exo100% (1)
- Mental Status Examination (MSE)Document13 pagesMental Status Examination (MSE)Pia Mae Buaya100% (1)
- Human Rights of Mentally IllDocument5 pagesHuman Rights of Mentally IllShyam100% (2)
- Case 2Document8 pagesCase 2Kreshnik IdrizajNo ratings yet
- Organic Mental Disorder: Presented By: Priyanka Kumari M.Sc. NursingDocument50 pagesOrganic Mental Disorder: Presented By: Priyanka Kumari M.Sc. NursingHardeep KaurNo ratings yet
- The Psychiatric Mental Status Exam (MSE)Document4 pagesThe Psychiatric Mental Status Exam (MSE)dev100% (1)
- Bipolar NCPDocument2 pagesBipolar NCPAngel BunolNo ratings yet
- Mental Retardation Treatment and ManagementDocument12 pagesMental Retardation Treatment and ManagementMelchoniza CalagoNo ratings yet
- Choithram College of NursingDocument16 pagesChoithram College of NursingMonikaNo ratings yet
- A Descriptive Study To Assess The Knowledge Regarding Substance Abuse and Ill Effects Among P.U. Students in The Selected P.U. College of BagalkotDocument3 pagesA Descriptive Study To Assess The Knowledge Regarding Substance Abuse and Ill Effects Among P.U. Students in The Selected P.U. College of BagalkotInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Report of Field Visit To National Centre For Disease ControlDocument12 pagesReport of Field Visit To National Centre For Disease ControlVaishali JainarainNo ratings yet
- Format MSEDocument3 pagesFormat MSESubir Banerjee0% (1)
- Pragyan College of Nursing Bhopal, M.P.: Subject - Mental Health Nursing TopicDocument11 pagesPragyan College of Nursing Bhopal, M.P.: Subject - Mental Health Nursing Topicannu100% (1)
- Seminar 7Document27 pagesSeminar 7Arya Lekshmi100% (1)
- Role of Ophthalmic Nurses With Visually Impaired PatientsDocument6 pagesRole of Ophthalmic Nurses With Visually Impaired PatientsIsaac Aleman0% (1)
- Family Health Nursing: Ms - Neethu Vincent Asst Professor KVM College of NursingDocument9 pagesFamily Health Nursing: Ms - Neethu Vincent Asst Professor KVM College of NursingNeethu VincentNo ratings yet
- Rehabilitation and RecoveryDocument29 pagesRehabilitation and RecoveryImad khanNo ratings yet
- Concept of PsychobiologyDocument21 pagesConcept of Psychobiologydhivyaram100% (1)
- Mental Health Act PDFDocument40 pagesMental Health Act PDFAnilkumar JaraliNo ratings yet
- Admission and Discharge of A Client in Psychiatric UnitDocument18 pagesAdmission and Discharge of A Client in Psychiatric UnitMahipal singh pacharNo ratings yet
- Role and Functions of Psychiatry NurseDocument20 pagesRole and Functions of Psychiatry NurseDhAiRyA ArOrANo ratings yet
- Organic Brain DisorderDocument69 pagesOrganic Brain DisorderHowell Mathew100% (1)
- Unit 6 NJDocument6 pagesUnit 6 NJmaakkanNo ratings yet
- OT7 - Outcome of Occupational Therapy GroupDocument17 pagesOT7 - Outcome of Occupational Therapy GroupAnnbe BarteNo ratings yet
- Importance and Purposes of ResearchDocument3 pagesImportance and Purposes of ResearchKarl Kiw-isNo ratings yet
- Communication and IprDocument12 pagesCommunication and IprDebashrita MisraNo ratings yet
- Mental Health TeamDocument3 pagesMental Health Teammanu sethiNo ratings yet
- Mhn-Issues, Trends, Magnitude, Contemporary Practice HealthDocument15 pagesMhn-Issues, Trends, Magnitude, Contemporary Practice HealthAna MikaNo ratings yet
- Behavior TherapyDocument23 pagesBehavior TherapydhivyaramNo ratings yet
- Process Recording ExampleDocument4 pagesProcess Recording ExampleChristine FernandoNo ratings yet
- Role - Responsibilities of Psychiatry Health NurseDocument3 pagesRole - Responsibilities of Psychiatry Health NurseDhAiRyA ArOrANo ratings yet
- Recreational Therapy Presentee: Sukhdeep Kaur Msc. (N) 1 YearDocument26 pagesRecreational Therapy Presentee: Sukhdeep Kaur Msc. (N) 1 YearSatbir GillNo ratings yet
- Mental Status Examination - Bring To LectureDocument6 pagesMental Status Examination - Bring To LectureJae ChoiNo ratings yet
- Attributes and Skills Required For A CounsellorDocument7 pagesAttributes and Skills Required For A Counsellorgasto mkonoNo ratings yet
- Ect ProcedureDocument11 pagesEct ProcedureDhAiRyA ArOrANo ratings yet
- Mini Mental Status ExamDocument10 pagesMini Mental Status ExamFrench Pastolero-ManaloNo ratings yet
- Electroconvulsive TherapyDocument9 pagesElectroconvulsive TherapyRoanne LaguaNo ratings yet
- Alternative System of MedicineDocument13 pagesAlternative System of MedicineDebipriya Mistry100% (1)
- Legal Issues in Mental Health NursingDocument61 pagesLegal Issues in Mental Health NursingS KANIMOZHINo ratings yet
- Restraining Procedure: General Principles For Use of RestraintsDocument10 pagesRestraining Procedure: General Principles For Use of RestraintsHardeep KaurNo ratings yet
- Recreational TherapyDocument22 pagesRecreational TherapyKishore RathoreNo ratings yet
- MHN, I (U), 6Document51 pagesMHN, I (U), 6akilaNo ratings yet
- Mental Health ContinuumDocument5 pagesMental Health ContinuumrajithapavalurNo ratings yet
- Rehabilitation of The AgedDocument31 pagesRehabilitation of The Agededward osae-oppong100% (1)
- Restraint and Seclusion ppt-2Document22 pagesRestraint and Seclusion ppt-2api-233645719100% (2)
- Sanjivani Psychosocial Rehabilitation Centre, Nedumkunnam, Kottayam DT., KeralaDocument3 pagesSanjivani Psychosocial Rehabilitation Centre, Nedumkunnam, Kottayam DT., KeralaJSM MKZYNo ratings yet
- Hospital Admission To Discharge 13 3 12 OkDocument3 pagesHospital Admission To Discharge 13 3 12 OkHarry Wahyudhy UtamaNo ratings yet
- AHM 540 Acute Care Part 1Document11 pagesAHM 540 Acute Care Part 1abul kalam AzadNo ratings yet
- Presented By-Ms. Yashodhara Ghosh Sen Asistant Professor Ion, BwuDocument63 pagesPresented By-Ms. Yashodhara Ghosh Sen Asistant Professor Ion, BwuyashodharaNo ratings yet
- 3-Physical-Therapist As Patient ManagerDocument38 pages3-Physical-Therapist As Patient ManagerRomana VayaniNo ratings yet
- Hospital Admission and DischargeDocument21 pagesHospital Admission and DischargeYogesh ChandraNo ratings yet
- Beta - Lactam Antibiotics: Prof. R. K. Dixit Pharmacology and Therapeutics K. G. M. U. LucknowDocument29 pagesBeta - Lactam Antibiotics: Prof. R. K. Dixit Pharmacology and Therapeutics K. G. M. U. LucknowHely PatelNo ratings yet
- GuidelinesDocument26 pagesGuidelinesmsc3nNo ratings yet
- Bahan Ajar Kusta & Frambusia PLKNDocument124 pagesBahan Ajar Kusta & Frambusia PLKNpetty arianiNo ratings yet
- Chest Pain Case Write-Up - Doctoring IIIDocument4 pagesChest Pain Case Write-Up - Doctoring IIIchristietwongNo ratings yet
- 12i3uasd Asdhgas D WawanDocument9 pages12i3uasd Asdhgas D Wawanwaluyo ningratNo ratings yet
- 15 Drugs QP Igcse Cie BiologyDocument7 pages15 Drugs QP Igcse Cie BiologyHay Thar TunNo ratings yet
- Abcs of Trauma CareDocument65 pagesAbcs of Trauma CareBeaulah HunidzariraNo ratings yet
- Mitral Valve SurgeryDocument2 pagesMitral Valve SurgeryLena MarieNo ratings yet
- Mental Heath and Ability To WorkDocument4 pagesMental Heath and Ability To Workgladiola janiNo ratings yet
- Zentel 400 MG Tablets GDS23Document6 pagesZentel 400 MG Tablets GDS23Vartika AgarwalNo ratings yet
- EtopexDocument11 pagesEtopexMohammed HaiderNo ratings yet
- Hamal Ko Roknay Ke TareekayDocument1 pageHamal Ko Roknay Ke TareekayAsad ImranNo ratings yet
- Medical Imaging Units SpecsDocument12 pagesMedical Imaging Units Specsar nedungadiNo ratings yet
- The Amazing Cordyceps MushroomDocument63 pagesThe Amazing Cordyceps MushroomSyncOrSwimNo ratings yet
- Herepes PDFDocument8 pagesHerepes PDFsuruthiNo ratings yet
- Fluid Electrolyte ImbalanceDocument15 pagesFluid Electrolyte ImbalancePrasanth Kurien Mathew100% (9)
- 1 s2.0 S1930043321003083 MainDocument5 pages1 s2.0 S1930043321003083 MainSandra ArellanoNo ratings yet
- Cord Prolaps E.: Jens MartenssonDocument19 pagesCord Prolaps E.: Jens MartenssonPeter YanksonNo ratings yet
- Heartcode Complete Bls Provider: Basic Life SupportDocument2 pagesHeartcode Complete Bls Provider: Basic Life SupportNayan ShrivastavaNo ratings yet
- EBN Diarrhea OrasolDocument8 pagesEBN Diarrhea Orasolcharm_peñaNo ratings yet
- Survival GuideDocument4 pagesSurvival Guideeclipse1130No ratings yet
- Laboratory For Medical Tests: Test ReportDocument2 pagesLaboratory For Medical Tests: Test ReportAdnana AndreeaNo ratings yet
- Strategi Kesinambungan Perniagaan Semasa Krisis Pandemik Covid-19: Kajian Rantaian Pengagihan Produk Pertanian Pekebun KecilDocument8 pagesStrategi Kesinambungan Perniagaan Semasa Krisis Pandemik Covid-19: Kajian Rantaian Pengagihan Produk Pertanian Pekebun KecilZuriani YanieNo ratings yet
- An Awareness Session On Blood Donation and Its ImportanceDocument40 pagesAn Awareness Session On Blood Donation and Its Importancekushi krishnaNo ratings yet
- Peritonitis TreatmentDocument3 pagesPeritonitis TreatmentMRFNo ratings yet
- Doctor Information UPDATEDocument40 pagesDoctor Information UPDATERishika BaranwalNo ratings yet
- A Case Study of DIBH To Spare Abdominal Organs at Risk For Renal Cell Carcinoma MR-Guided RadiotherapyDocument14 pagesA Case Study of DIBH To Spare Abdominal Organs at Risk For Renal Cell Carcinoma MR-Guided Radiotherapyapi-525837437No ratings yet