Professional Documents
Culture Documents
4 Soft Tissue Nerves
4 Soft Tissue Nerves
Uploaded by
Mahfouz0 ratings0% found this document useful (0 votes)
11 views25 pages1. Nerves can be injured through ischemia, compression, traction, laceration, or burning. The severity of damage ranges from quick recovery to complete interruption.
2. There are 5 classifications of nerve injuries - neurapraxia (reversible conduction block), axonotmesis (axon degeneration but intact nerve sheath), neurotmesis (severed nerve), and degrees 3 and 4 which involve disrupted nerve sheaths and require surgical intervention.
3. Clinical assessment involves testing for signs like Tinel's sign, EMG, and motor/sensory function to determine the severity of injury and prognosis for recovery. Surgical intervention may be required for severe injuries.
Original Description:
Original Title
4-soft-tissue-Nerves
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. Nerves can be injured through ischemia, compression, traction, laceration, or burning. The severity of damage ranges from quick recovery to complete interruption.
2. There are 5 classifications of nerve injuries - neurapraxia (reversible conduction block), axonotmesis (axon degeneration but intact nerve sheath), neurotmesis (severed nerve), and degrees 3 and 4 which involve disrupted nerve sheaths and require surgical intervention.
3. Clinical assessment involves testing for signs like Tinel's sign, EMG, and motor/sensory function to determine the severity of injury and prognosis for recovery. Surgical intervention may be required for severe injuries.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
0 ratings0% found this document useful (0 votes)
11 views25 pages4 Soft Tissue Nerves
4 Soft Tissue Nerves
Uploaded by
Mahfouz1. Nerves can be injured through ischemia, compression, traction, laceration, or burning. The severity of damage ranges from quick recovery to complete interruption.
2. There are 5 classifications of nerve injuries - neurapraxia (reversible conduction block), axonotmesis (axon degeneration but intact nerve sheath), neurotmesis (severed nerve), and degrees 3 and 4 which involve disrupted nerve sheaths and require surgical intervention.
3. Clinical assessment involves testing for signs like Tinel's sign, EMG, and motor/sensory function to determine the severity of injury and prognosis for recovery. Surgical intervention may be required for severe injuries.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
You are on page 1of 25
Peripheral Nerve Injuries
Nerves can be injured by:
1- ischemia
2- compression
3- traction
4- laceration
5- burning
Damage varies in severity from transient
and quick recovery to complete
interruption and degeneration
Transient ischemia
Acute nerve compression causes:
- numbness and tingling within 15 minutes
- Loss of pain and sensibility after 30 min
- Muscle weakness after 45 min
Relief of compression is followed by intense
paresthesia lasting up to 5 min (the familiar pins
and needles after a limb goes asleep)
Feeling is restored within 30 seconds
Full muscle power after about 10 min
Changes are due to transient anoxia and leave no
trace of nerve damage
Tourniquet application during surgery
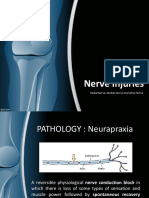
Neurapraxia
Reversible physiological nerve conduction block
Loss of some type of sensation and muscle
power
Followed by spontaneous recovery after a few
days or weeks
Due to mechanical pressure causing segmental
demyelination
Seen typically in crutch palsy, Saturday night
palsy and the milder tourniquet palsy
Axonotmesis
Literally: axonal interruption
More severe nerve injury
Typically after closed fractures and dislocations
There is loss of conduction but the nerve is in continuity
and neural tubes are intact
Distal to the lesion and a few mm retrograde, axons
disintegrate and are resorbed by phagocytes (called
Wallerian degeneration)
Takes only a few days and is accompanied by marked
proliferation of Schwann cells and fibroblasts lining the
endoneurial tube
Degenerative target organs (motor end plates and
sensory receptors) gradually atrophy
If they are not reinnervated within 2 years they will never
recover
Axonotmesis
Axonal regeneration starts within hours of nerve
damage
Encouraged by neurotropic factors produced by
Schwann cells distal to the injury
Numerous fine unmyelinated tendrils grow from
the proximal stump and find their way into the
cell-clogged endoneurial tubes
Axonal processes grow at a speed of about
1mm per day
Larger fibers slowly acquiring a new myelin coat
Eventually they join to end organs which enlarge
and start functioning again
Neurotmesis
Division of the nerve trunk
Or more severe injury without actual cut
Recovery will not occur
Rapid Wallerian degeneration
Endoneurial tubes are destroyed and scarring
occurs that prevents regenerating axons from
entering the distal segment and regain their
target organs
Instead they form a “neuroma” at the site of
injury
Neuroma: regenerating fibers mingling with
proliferating Schwann cells and fibroblasts in a
jumbled knot
Neurotmesis
Even after surgical repair:
- Many new axons fail to reach the distal
segment
- Those that do may not find suitable
Schwann tubes
- Or may not reach the correct end organ in
time
- Or may remain incompletely myelinated
- Function may be adequate but never
normal
Classification of Nv. Inj.
First degree Injury: transient ischemia and
neuropraxia. Reversible
Second degree Injury: axonal degeneration.
Preserved endoneurium. Regeneration can lead
to complete or near complete recovery without
the need for intervention
Third degree Injury: disrupted endoneurium.
Intact perineurial sheaths and limited internal
damage. Fibrosis and crossed connection limit
recovery. Good chances for axons to reach their
targets
Classification
Fourth degree injury: only the epineurium
is intact nerve trunk is still in continuity but
damage is severe. Recovery is unlikely.
The injured segment should be excised
and the nerve repaired or grafted
Fifth degree injury: the nerve is divided
and will have to be repaired.
Clinical Features
Acute nerve injuries are easily missed esp. when
ass. with #s and dislocations
Always test for nerve injuries following any
significant trauma
Look for accompanying vascular injuries
Ask for P&N, weakness. Examine injured limb
systematically for neurology
Accurate mapping
Plastic pen test: dry skin
Repeat examination on intervals
Clinical features
chronic
Smooth and shiny anaesthetic skin in
smooth and shiny
Clues of diminished sensibility such as
cigarette burns.
Wasted muscle groups and fixed postural
defromities
Assessment f nerve recovery
How severe was the lesion
How well is the nerve function now
Examination of power and light touch
Motor recovery is slower than sensory
recovery
Assessment: degree of injury
Low energy injury: neuropraxia, recovery
anticipated
High energy injury: third and fourth
degree, recovery is less predicted
Open injury or very high energy closed
injury: nerve is probably divided and early
exploration is called for.
Tinel’s sign
Peripheral tingling or dysaesthesia provoked by
percussing the nerve
In neuropraxia: TS is negative
In axonotmesis: TS is positive at the site of injury
bec. Of the sensitivity of the sprouts of the
regenerating axons. TS will then advance after a
delay by 1 mm per day
Failure of TS to advance suggests 4th or 5th
degree injury and early exploration is needed
Slow advancement and poor muscle group
response suggest unlikely recovery and the
need for exploration.
EMG: electromyogram
Denervation potentials at the third week if
muscle looses its nerve supply
This excludes neuropraxia
But dose not differentiate between axonotmesis
and neurotmesis: this remains a clinical
distinction
If one waits too long to decide then the target
muscle may have failed irrecoverably and the
answer hardly matters
Assessment: the level of nerve
function
Two point discrimination is a measure of
innervation density
Threshold tests: measure the threshold at
which a sensory receptor is activated.
They are more useful in nerve
compression syndrome where individual
receptors fail to send impulses centrally,
here two point discrimination is preserved
Motor power assessment
Graded on the Medical Research Council scale:
0 no contraction
1 a flicker of activity
2 muscle contraction but unable to overcome
gravity
3 contraction able to overcome gravity
4 contraction against resistance
5 normal power
Prognosis
Type of lesion: neuropraxia always recover fully,
axonotmesis may or may not, neurotmesis will not
unless the nerve is repaired
Level of the lesion: the higher the worse
Type of the nerve: purely motor or purely sensory
recover better than mixed nerves because there is less
likelihood of axonal confusion
Age: children do better
Delay in suture: a most important adverse factor. The
earlier the better. After a few months recovery following
suturing become less likely
Ass. Lesions: even if nerve recovers well, they may
prohibit limb recovery
Surgical techniques: if no experience; transfer
Regional survey
Brachial plexus injuries
Stab or traction
Traction: supraclavicular 65%, infraclavicular
25%, combined 10%
SC: motorcycle injuries
IC: # dislocation of the shoulder, in 25% the
axillary artery is also torn
# of the clavicle rarely damage the plexus
Preganglionic vs. postganglionic
PG: can’t recover and surgically irreparable
Mild lesions (neuropraxia): recover
spontaneously but may need months to recover
fully
Clinical features
level of the lesion
Upper plexus: (C5, C6): shoulder abductors and
external rotators and the forearm supinators are
paralysed. Sensory loss of the outer aspect of
the arm and forearm
Pure lower plexus are rare: paralysed intrinsic
hand muscles and weak wrist and finger flexors.
Loss of sensation in the ulnar forearm and hand
If the entire plexus is damaged, the whole limb is
paralysed and numb
Pre or post ganglionic
Pre (root avulsion): crushing or burning
pain in an anaesthetic hand. Paralysis of
scapular muscles or diaphragm. Horner’s
syndrome. Severe vascular injury. Ass.
Injuries of the cervical spine. Spinal cord
dysfunction.
Histamine test: positive in preganglionic
MRI shows pseudomeningiocele due to
root avulsion
Obstetrical Brachial Plexus Injuries
Excessive traction on brachial plexus
during childbirth
Upper root injury: Erb’s palsy: overweight
babies with shoulder dystocia at delivery
Complete plexus injury: Klumpke’s palsy:
usually after breech delivery of smaller
babies.
clinical
Erb’s: C5, C6 and sometimes C7
abductors and external rotators of the shoulder
and supinators are paralysed
The arm is held to the side internally rotated and
pronated
Klumpke;s: less common, more severe. The arm is
flail and pail. All finger muscle are paralysed.
Vasomotor impairment and unilateral Horner’s
X-rays should be taken to exclude #s of the
shoulder or clavicle
management
Paralysis may recover completely: most
Erb’s. a reliable indicator is the return of
biceps activity by the third month. Absence
of biceps recovery dose not completely
rule out later recovery.
May improve
May persist
Consider operative if no biceps recovey
after 3 months
You might also like
- Macroeconomics 6th Edition Williamson Solutions Manual DownloadDocument13 pagesMacroeconomics 6th Edition Williamson Solutions Manual DownloadDarrell Davis100% (24)
- Mcmaster Nursing Anatomy 1H06 Tutorial Assignment 3Document6 pagesMcmaster Nursing Anatomy 1H06 Tutorial Assignment 3NTRisforthinkersNo ratings yet
- Degeneration & Regeneration of Nerve FibreDocument29 pagesDegeneration & Regeneration of Nerve FibreSana FatimaNo ratings yet
- Nerves Injury: Audi HidayatullahDocument42 pagesNerves Injury: Audi Hidayatullahayu100% (1)
- Basic Science ART & NerveDocument56 pagesBasic Science ART & NerveStar CruiseNo ratings yet
- Peripheral Nerve Injuries - Medical ApplicationsDocument103 pagesPeripheral Nerve Injuries - Medical ApplicationsJune Epe100% (1)
- PT Pediatric Surgery Sec 1Document27 pagesPT Pediatric Surgery Sec 1Amany SaifNo ratings yet
- Epineurium. If The Nerve Contains More Than One Fascicle, The Epineurium May Be Divided IntoDocument18 pagesEpineurium. If The Nerve Contains More Than One Fascicle, The Epineurium May Be Divided Intoayaanshariq99No ratings yet
- Peripheral Nerve Injuries: DR - Prateek Singh Intern Dept. of Orthopaedics BpkihsDocument29 pagesPeripheral Nerve Injuries: DR - Prateek Singh Intern Dept. of Orthopaedics BpkihsjothiNo ratings yet
- Peripheral Nerve InjuryDocument28 pagesPeripheral Nerve InjuryRoydenPTNo ratings yet
- Nerve Injuries: Radial Nerve, Median Nerve and Ulnar NerveDocument26 pagesNerve Injuries: Radial Nerve, Median Nerve and Ulnar NerveaisiyaahNo ratings yet
- 7 - Spinal-InjuriesDocument40 pages7 - Spinal-Injuriesraed faisalNo ratings yet
- Presented by Cathrine Diana PGI Dept of Oral and Maxillofacial SurgeryDocument78 pagesPresented by Cathrine Diana PGI Dept of Oral and Maxillofacial SurgeryDorin PathakNo ratings yet
- NeuropathyDocument54 pagesNeuropathyshreyasNo ratings yet
- Board Review NeuromuscularDocument93 pagesBoard Review NeuromuscularRyan CrooksNo ratings yet
- Peripheral Nerve Injuries: Submitted By:-Manmeet KaurDocument115 pagesPeripheral Nerve Injuries: Submitted By:-Manmeet KaurManmeet KaurNo ratings yet
- PR Ujian Neuro AuliaDocument10 pagesPR Ujian Neuro AuliaAULIA ANGRAININo ratings yet
- Spinal Cord Injury-1Document17 pagesSpinal Cord Injury-1Mariana MillerNo ratings yet
- Peripheral Nerve InjuriesDocument29 pagesPeripheral Nerve InjuriesbrillniksNo ratings yet
- Peripheral Nerve InjuriesDocument207 pagesPeripheral Nerve InjuriesAashka MahetaNo ratings yet
- Peripheral Nerve Injured byDocument4 pagesPeripheral Nerve Injured byAmro OwdahNo ratings yet
- Cervical Spine Injury GregDocument49 pagesCervical Spine Injury GregGregory James100% (1)
- Pathophysiology of Nerve: Dr. Ayisha Qureshi Professor & Hod MBBS, MphilDocument26 pagesPathophysiology of Nerve: Dr. Ayisha Qureshi Professor & Hod MBBS, MphilMuhammad AhmedNo ratings yet
- Peripheral Nerve InjuriesDocument112 pagesPeripheral Nerve InjuriesManmeet Kaur100% (1)
- Peripheral Nerve InjuriesDocument196 pagesPeripheral Nerve InjuriesAhmad A. Fannoon100% (1)
- Nerve Injury Classification, Nerve Degeneration, Regeneration and Repair TechniquesDocument50 pagesNerve Injury Classification, Nerve Degeneration, Regeneration and Repair TechniquesRajveerNo ratings yet
- Peripheral Nerve LesionDocument11 pagesPeripheral Nerve LesionBalaKrishnaNo ratings yet
- Week 6 Portfolio QuestionsDocument6 pagesWeek 6 Portfolio Questionsapi-479716004No ratings yet
- Spine and Spinal Cord Injury - Kuliah Blok 21 Semester 7Document37 pagesSpine and Spinal Cord Injury - Kuliah Blok 21 Semester 79z7txjgkvmNo ratings yet
- Peripheral Nerve ExaminationDocument30 pagesPeripheral Nerve ExaminationMalvinder Singh DhillonNo ratings yet
- Peripheral Nerve InjuriesDocument12 pagesPeripheral Nerve InjuriesJiggs LimNo ratings yet
- Spinal Cord InjuriesDocument35 pagesSpinal Cord InjuriesTitanium TssNo ratings yet
- CNS Path Pharm KelnerDocument9 pagesCNS Path Pharm Kelnerjazzdoc007No ratings yet
- Elective Cases2aDocument156 pagesElective Cases2aMerlin MariandariNo ratings yet
- Nerve TraumaDocument31 pagesNerve TraumaUjjawalShriwastavNo ratings yet
- Cervical Spine InjuryDocument64 pagesCervical Spine Injuryapi-195020000% (1)
- Degeneration and Regeneration of Nerve FibreDocument25 pagesDegeneration and Regeneration of Nerve Fibresunil patelNo ratings yet
- Median, Ulnar and Radial Nerve Injuries: University of Baghdad Al-Kindy College of Medicine Fifth Stage / Group ADocument13 pagesMedian, Ulnar and Radial Nerve Injuries: University of Baghdad Al-Kindy College of Medicine Fifth Stage / Group ANoor Al Zahraa AliNo ratings yet
- Spinal Cord InjuryDocument16 pagesSpinal Cord Injuryjohnlester_jlf100% (2)
- UpikDocument21 pagesUpikaldybebikaNo ratings yet
- Nerve SurgeriesDocument26 pagesNerve SurgeriesAnkita TiwariNo ratings yet
- Nerve Injury & Recovery: The ProblemDocument3 pagesNerve Injury & Recovery: The Problembalab2311No ratings yet
- V. Pathophysiology: Nerve InjuryDocument4 pagesV. Pathophysiology: Nerve Injuryjoanna gurtizaNo ratings yet
- Back PainDocument18 pagesBack PainCabdiladif Ahmed McrfNo ratings yet
- Intro To PT 4Document3 pagesIntro To PT 4Floriza de LeonNo ratings yet
- Ivanne ClinicalDocument10 pagesIvanne Clinicalmohammed.sheeb.yesNo ratings yet
- Spine Emergencies: Presenter: Nur Aizat Supervisor: Dr. FakhriyDocument42 pagesSpine Emergencies: Presenter: Nur Aizat Supervisor: Dr. FakhriyZainal HussainNo ratings yet
- Peripheral Nerve Injury 2Document24 pagesPeripheral Nerve Injury 2Gargi MPNo ratings yet
- Peripheral Nerve Injury and Repair: Adam Osbourne, 5th Year MedicineDocument5 pagesPeripheral Nerve Injury and Repair: Adam Osbourne, 5th Year Medicineayrahma29No ratings yet
- 07 - Peripheral Nerve InjuryDocument48 pages07 - Peripheral Nerve InjurymalikjakNo ratings yet
- Nerve Injury: Departemen Neurologi Fakultas Kedokteran Universitas Islam Sumatera UtaraDocument27 pagesNerve Injury: Departemen Neurologi Fakultas Kedokteran Universitas Islam Sumatera UtaraDea indah damayantiNo ratings yet
- HumanPhysiologyNerve Muscle PhysiologyDocument36 pagesHumanPhysiologyNerve Muscle PhysiologyPriyanka RameshNo ratings yet
- PBL NeuroDocument45 pagesPBL NeuroInsan_aqidNo ratings yet
- Fractures of Spine and Pelvis2007Document70 pagesFractures of Spine and Pelvis2007api-19916399No ratings yet
- Disorder of Neuromuscular Junction: Myasthenia Gravis and Lambert-Eaton Myasthenic SyndromeDocument36 pagesDisorder of Neuromuscular Junction: Myasthenia Gravis and Lambert-Eaton Myasthenic SyndromePraneethaNo ratings yet
- PBLDocument52 pagesPBLInsan_aqidNo ratings yet
- Spinal Cord InjuryDocument9 pagesSpinal Cord Injuryta CNo ratings yet
- Nerve Healing FinalDocument31 pagesNerve Healing FinalKim MateoNo ratings yet
- Degeneration & Regeneration of Nerve FibreDocument29 pagesDegeneration & Regeneration of Nerve FibreSana Fatima100% (2)
- Nerve InjuriesDocument20 pagesNerve InjuriesAnupama NagrajNo ratings yet
- Spinal Stenosis And Pinched Nerve A Simple Guide to These conditionsFrom EverandSpinal Stenosis And Pinched Nerve A Simple Guide to These conditionsRating: 5 out of 5 stars5/5 (1)
- Practical Manual in Biochemistry and Clinical BiochemistryDocument6 pagesPractical Manual in Biochemistry and Clinical BiochemistrycxjvxsogzbNo ratings yet
- Analisis Lemak & Minyak: By. Mulono ApriyantoDocument47 pagesAnalisis Lemak & Minyak: By. Mulono ApriyantoSalsabila NurNo ratings yet
- Strategic Management Case Study: Prepared by Group #1 Emba14BDocument39 pagesStrategic Management Case Study: Prepared by Group #1 Emba14BKalyaniDudhane-PawadeNo ratings yet
- Jurassic Production Facility (JPF) at Sabriya: Supplier Document Cover SheetDocument2 pagesJurassic Production Facility (JPF) at Sabriya: Supplier Document Cover SheetBiswasNo ratings yet
- P Prayer O HallesbyDocument94 pagesP Prayer O HallesbyObed Arriaza100% (4)
- Evangelism 1Document4 pagesEvangelism 1Horace Owiti O.No ratings yet
- Job Interview Questions OkDocument2 pagesJob Interview Questions OkJaqueline FernándezNo ratings yet
- DSM Mixing Tower SkyCiv ReportDocument484 pagesDSM Mixing Tower SkyCiv Reportmincho4104No ratings yet
- 5th-Sunday-of-Lent (2) .2Document1 page5th-Sunday-of-Lent (2) .2Emmanuel ToretaNo ratings yet
- Personality and Its Effect On Group Performance (FINAL)Document56 pagesPersonality and Its Effect On Group Performance (FINAL)gaurav gargNo ratings yet
- 1 Concept Paper On The 6-Year CurriculumDocument9 pages1 Concept Paper On The 6-Year CurriculumJoseph Tabadero Jr.100% (3)
- New Microsoft Word Document Tofik ProposalDocument12 pagesNew Microsoft Word Document Tofik ProposalenbakomNo ratings yet
- M. Wolves 11Document7 pagesM. Wolves 11rakiny05No ratings yet
- Chapter 7 - Cognitive DevelopmentDocument3 pagesChapter 7 - Cognitive DevelopmentmizbigspendaNo ratings yet
- Konsep Pendidikan Religius RasionalDocument14 pagesKonsep Pendidikan Religius RasionalSri ParwatiNo ratings yet
- Clear Choice: TurbomatrixDocument10 pagesClear Choice: TurbomatrixSaleh HamadanyNo ratings yet
- E Commerce Chap 1Document28 pagesE Commerce Chap 1Jannatul FardusNo ratings yet
- Baseband Radio Node Customized Delta Telefonica VCT 2018Document79 pagesBaseband Radio Node Customized Delta Telefonica VCT 2018sammyd2009100% (2)
- Christian History and MissionDocument50 pagesChristian History and MissionJohana Vangchhia100% (1)
- 6 - People vs. VelosoDocument4 pages6 - People vs. Velosogerlie22No ratings yet
- CIOs and The Future of ITDocument8 pagesCIOs and The Future of ITdany odarNo ratings yet
- Unit 7-Chemical Reactions NotesDocument55 pagesUnit 7-Chemical Reactions Notesapi-182809945No ratings yet
- Biography of Jamgön Ju MiphamDocument6 pagesBiography of Jamgön Ju MiphamBLhundrupNo ratings yet
- U Pravom Testu Nema Ponudjenih Reci (BEEN, YOU ) Vec Mozete Upotrebiti Bilo Koje, Ali Recenica Treba Da Ima Smisla I Da Ne Promeni ZnacenjeDocument3 pagesU Pravom Testu Nema Ponudjenih Reci (BEEN, YOU ) Vec Mozete Upotrebiti Bilo Koje, Ali Recenica Treba Da Ima Smisla I Da Ne Promeni ZnacenjeMarko RisticNo ratings yet
- 49 - HD - 2000 New Logo LowDocument12 pages49 - HD - 2000 New Logo LowAgata OwczarekNo ratings yet
- Detergent Flushing of Pre Boiler System-Procedure 250Document11 pagesDetergent Flushing of Pre Boiler System-Procedure 250Sara LopezNo ratings yet
- 85.deep Seabed Mining (12-2013)Document4 pages85.deep Seabed Mining (12-2013)RSTNo ratings yet
- Math InterventionDocument6 pagesMath InterventionPAOLO R. ALARDENo ratings yet
- PMP IttoDocument3 pagesPMP IttoNicoletaNo ratings yet