Professional Documents
Culture Documents
Skin Diseases Presentation2
Skin Diseases Presentation2
Uploaded by
DaniTade0 ratings0% found this document useful (0 votes)
61 views40 pagesThis document summarizes several common skin diseases including impetigo, scabies, tinea capitis, and atopic dermatitis. It describes the etiology, clinical presentation, diagnosis, and treatment of each condition. Impetigo is a bacterial infection that presents as honey-colored crusts or bullae. Scabies is caused by mite infestation and causes intense pruritus. Tinea capitis is a fungal infection of the scalp that may appear as patches of alopecia or kerion nodules. Atopic dermatitis is a chronic pruritic condition often beginning in infancy that involves dry, eczematous skin and is treated with moisturizers
Original Description:
Original Title
Skin diseases presentation2.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes several common skin diseases including impetigo, scabies, tinea capitis, and atopic dermatitis. It describes the etiology, clinical presentation, diagnosis, and treatment of each condition. Impetigo is a bacterial infection that presents as honey-colored crusts or bullae. Scabies is caused by mite infestation and causes intense pruritus. Tinea capitis is a fungal infection of the scalp that may appear as patches of alopecia or kerion nodules. Atopic dermatitis is a chronic pruritic condition often beginning in infancy that involves dry, eczematous skin and is treated with moisturizers
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
61 views40 pagesSkin Diseases Presentation2
Skin Diseases Presentation2
Uploaded by
DaniTadeThis document summarizes several common skin diseases including impetigo, scabies, tinea capitis, and atopic dermatitis. It describes the etiology, clinical presentation, diagnosis, and treatment of each condition. Impetigo is a bacterial infection that presents as honey-colored crusts or bullae. Scabies is caused by mite infestation and causes intense pruritus. Tinea capitis is a fungal infection of the scalp that may appear as patches of alopecia or kerion nodules. Atopic dermatitis is a chronic pruritic condition often beginning in infancy that involves dry, eczematous skin and is treated with moisturizers
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 40
Skin diseases
Moderator –Dr. Teshome
Impetigo
Impetigo is a contagious superficial bacterial infection observed most
frequently in children.
It may be classified as primary impetigo (direct bacterial invasion of
previously normal skin) or secondary impetigo (infection at sites of
minor skin trauma such as abrasions, minor trauma, and insect bites, or
underlying conditions such as eczema)
-there are 2 classic forms of impetigo.
A. Non bullous impetigo
B. Bullous impetigo
Clinically manifestation
Non bullous impetigo
- Lesions typically begin on the skin of the face or on extremities that
have been traumatized like insect bites,abbrasions and lacerations.
- A tiny vesicle or pustule forms initially and rapidly develops into a
honey-colored crusted plaque that is generally <2 cm in diameter.
- Lesions are associated with little to no pain or surrounding erythema,
and constitutional symptoms are generally absent.
Bullous impetigo
• mainly an infection of infants and young children.
• Flaccid, transparent bullae develop most commonly on skin of the
face, buttocks, trunk, perineum, and extremities.
• Neonatal bullous impetigo can begin in the diaper area.
Treatment of impetigo
• Topical therapy with mupirocin 2%, and retapamulin 1% 2-3
times a day for 10-14 days for localized disease by staph.aureus.
• Systemic therapy with oral antibiotics should be prescribed for
patients with streptococcal or widespread involvement of
staphylococcal infection cellulitis, furunculosis, abscess formation,
or suppurative lymphadenitis. Cephalexin, 25-50 mg/kg/day in 3-
4 divided doses for 7-10 days.
complications
• osteomyelitis, septic arthritis, pneumonia, and septicemia
• PSGN
Scabies
• caused by burrowing and release of toxic or antigenic substances
by the female mite Sarcoptes scabiei
• The most important factor that determines the spread of scabies is
the extent and duration of physical contact with an affected
individual and so children and sexual partners are the most
affected.
Ethiology and pathogenesis
• After impregnation on the skin surface, a gravid female exudes a
keratolytic substance and burrows into the stratum corneum, often
forming a shallow well within 30 min.
• She deposits 10-25 oval eggs and numerous brown fecal pellets
(scybala) daily for 4-5 weeks and dies within the burrow.
• The eggs hatch in 3-5 days, releasing larvae that move to the skin
surface to molt into nymphs. Maturity is achieved in approximately 2-
3 wk. Mating occurs, and the gravid female invades the skin to
complete the life cycle.
Clinical manifestation
• Scabies is heralded by intense pruritis, particularly at night.
• The first sign of the infestation often consists of 1-2 mm red papules,
some of which are excoriated, crusted,or scaling
• Thread like burrows are the classic lesion in scabies.
• In infants, bullae and pustules are relatively common. The eruption
may also include wheals, papules,vesicles, and a superimposed
eczematous dermatitis .
• The palms, soles, and scalp are often affected.
older children and adolescents -the clinical pattern is similar to that in
adults
interdigital spaces, wrist flexors, anterior axillary folds,
ankles, buttocks, umbilicus and belt line, groin, genitals
in men, and areolas in women
Crusted scabies- seen in immunocompromised, mental retardation and
sensory loss
Differential diagnosis
• Depends on the type of lesion present.
• Papulovesicular lessions may confuse with papular urticaria,
chickenpox, viral exanthems, drug eruptions, dermatitis herpetiformis,
and folliculitis.
• Eczematous lesions may mimic atopic dermatitis and seborrheic
dermatitis, and the less common bullous disorders of childhood
Diagnosis
• Diagnosis of scabies can often be made clinically but is confirmed by
microscopic identification of mites, ova and scybala in epithelial
debris.
• Scrapings most often test positive when obtained from burrows or
fresh papules.
Treatment -The entire family should be treated
-Clothing, bed linens, and towels should be washed in hot water and
dried using high heat
Tinea capitis
-Dermatophyte infection of the scalp most often caused by
Trichophyton tonsurans, occasionally by Microsporum canis.
-In microsporum and some trychophyton infections, the spores are
distributed in a sheath like fashion around the hair shaft (Ectotrix)
-Trichophyton tonsurans produce infection within the hair shaft
(Endothrix)
1.Scaly patches with alopecia (gray patches) – Single or multiple scaly
patches with hair loss are a common presentation of ectothrix infections
2.Patches of alopecia with black dots- Broken-off hairs near surface give
appearance of “dots”. Tends to be diffuse and poorly circumscribed. Resembles
seborrheic dermatitis
3.Kerion-Characterized by boggy, purulent, inflamed nodules and plaques
extremely painful; drains pus from multiple openings, like honeycomb
4.Favus- Thick yellow adherent crusts (scutula) composed of skin debris and
hyphae that are pierced by remaining hair shafts. Caused by T. schoenleinii
uniquely.
Differential diagnosis
• Tinea capitis can be confused with seborrheic dermatitis,
psoriasis,alopecia areata.
• In adolescents, the patchy, moth-eaten type of alopecia associated
with secondary syphilis may resemble tinea capitis.
• If scarring occurs, discoid lupus erythematosus and lichen planopilaris
must also be considered in the differential diagnosis.
Investigation
• Wood lamp examination of infected hair
• Microscopic examination of a KOH preparation of infected hair from
active border of lesion.
• Culture obtained by planting broken off infected hairs on Sabouraud
medium with reagents to inhibit growth of other organisms. Such
identification.
• may require 2 wk or more
Treatment
• Treatment is with griseofulvin 20 to 25mg/kg/d at least for 8-12
weeks
• Better absorption with fatty food, and given at night.
• Adverse reaction is rare but includes nausea, vomiting, blood
dyscariasis, phototoxicity and hepatotoxicity.
• Terbinafine is also effective at a dosage of 3-6 mg/kg/24 hr for 4-6 wk
or possibly in pulse therapy, although it has limited activity against M.
canis
• All contacts and family members should be examined and treated
• Chronic untreated kerion and favus, can result in permanent scarring
alopecia
• Topical antifungals are not effective alone, but it may be an important
adjunct because it may decrease the shedding of spores, and should
be recommended in all patients.
• Topical antifungals like -2.5% selenium sulfide
. - ketoconazole shampoo
-zinc pyrithione
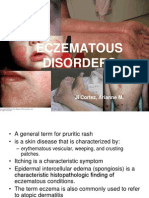
Atopic dermatitis
• Atopic dermatitis (ie, eczema) is a chronic pruritic skin condition due to
hereditary predisposition to react for sensitizers usually beginning in
infancy.
• is the most common chronic relapsing skin disease seen in infancy and
childhood.
• Occurs in 10-30% children worldwide.
• Occurs with other atopic diseases like asthma, allergic rhinitis and food
allergy
• Atopic march- Infants with AD are predisposed to development of
allergic rhinitis and/or asthma later in childhood.
Clinical manifestation
• Intense pruritus, especially at night, and cutaneous reactivity are the
cardinal features of AD.
• Skin reaction pattern and distribution vary with the patient’s age and
disease activity.
• In Infancy involves the face, scalp, and extensor surfaces of the
extremities. The diaper area is usually spared.
• Older children and children with chronic AD have lichenification and
localization of the rash to the flexural folds of the extremities.
Diagnosis
• AD is diagnosed on the basis of 3 major features:
• pruritus
• An eczematous dermatitis that fits into a typical presentation,
• and a chronic or chronically relapsing course.
• Associated features, such as a family history of asthma, hay fever,
elevated IgE, and immediate skin test reactivity, are variably present.
Treatment
• The treatment of AD requires a systematic, multifaceted approach
that incorporates -skin hydration
• -topical anti-inflammatory therapy
• -identification and elimination of flare factors
• -systemic therapy
Cutaneous hydration
• Moisturizers are first-line therapy. Lukewarm soaking baths for 15-20
min followed by the application of an occlusive emollient to retain
moisture provide symptomatic relief.
• This is because patients with AD have impaired skin barrier function
from reduced lipid levels, they present with diffuse, abnormally dry
skin, or xerosis
Topical corticosteroids
• The cornerstone of antiinflammatory treatment for acute
exacerbations of AD
• There are 7 classes of topical glucocorticoids, ranked according to
their potency as determined by vasoconstrictor assay. Class 4-7 are
considered lower potency.
• ultrahigh-potency glucocorticoids should not be used on the face or
intertriginous areas and should be used only for very short periods on
the trunk and extremities
• Mid-potency glucocorticoids can be used for longer periods to treat
chronic AD involving the trunk and extremities.
• Table 145-5 Selected Topical Corticosteroid
• Preparations*
•GROUP 1
•Clobetasol propionate (Temovate) 0.05% ointment/cream
•Betamethasone dipropionate (Diprolene) 0.05% ointment/lotion/gel
•Fluocinonide (Vanos) 0.1% cream
•GROUP 2
•Mometasone furoate (Elocon) 0.1% ointment
•Halcinonide (Halog) 0.1% cream
•Fluocinonide (Lidex) 0.05% ointment/cream
•Desoximetasone (Topicort) 0.25% ointment/cream
•Betamethasone dipropionate (Diprolene) 0.05% cream
•GROUP 3
•Fluticasone propionate (Cutivate) 0.005% ointment
•Halcinonide (Halog) 0.1% ointment
•Betamethasone valerate (Valisone) 0.1% ointment
• GROUP 4
• Mometasone furoate (Elocon) 0.1% cream
• Triamcinolone acetonide (Kenalog) 0.1% ointment/cream
• Fluocinolone acetonide (Synalar) 0.025% ointment
• GROUP 5
• Fluocinolone acetonide (Synalar) 0.025% cream
• Hydrocortisone valerate (Westcort) 0.2% ointment
• GROUP 6
• Desonide (DesOwen) 05% ointment/cream/lotion
• Alclometasone dipropionate (Aclovate) 0.05% ointment/cream
• GROUP 7
• Hydrocortisone (Hytone) 2.5% , 1%, 0.5% ointment/cream/lotion
Systemic glucocorticoids
• Systemic corticosteroids are rarely indicated in the treatment of
chronicAD.
• The dramatic clinical improvement that may occur with systemic
corticosteroids is frequently associated with a severe rebound flare of
AD after therapy discontinuation.
Seborrheic dermatitis
• Seborrheic dermatitis is a self-limiting eruption consisting of
erythematous plaques with greasy-looking, yellowish scales
distributed on areas rich in sebaceous glands such as the scalp, the
external ear, the center of the face, and the intertriginous areas.
• Pathogenesis is not known, but the associated factors are
• Individual susceptibility
• Sebume and
• Malassezia spp
Clinical manifestation
• The most common manifestation of seborrheic dermatitis in
newborns and infants is "cradle cap," an asymptomatic and non-
inflammatory accumulation of yellowish, greasy scales on the scalp
• The infant is generally well; feeding and sleep are not disturbed. The
pruritus is mild in most cases. The clinical manifestations fluctuate,
but most cases eventually resolve spontaneously within weeks to a
few months.
• The mildest and most common form of scalp seborrheic dermatitis is
dandruff
Differential diagnosis
• Atopic dermatitis-The erythematous, scaly, and crusted lesions of
atopic dermatitis are generally poorly demarcated, and commonly
involve the cheeks, scalp, and extensor surfaces of the limb
• Psoriasis- is uncommon in infancy, psoriatic plaques are sharply
defined, shiny and bright red in color, with the typical large, silvery
scales of psoriasis usually seen in nonintertriginous areas
• Tinea capitis- may present as a scaly scalp dermatitis with moderate
or minimal inflammation . Hair loss generally is present but is not
always easy to detect. KOH examination of the hair shaft and fungal
cultures will confirm the diagnosis.
References
• Nelson 20th edition
• Uptodate 2018
Thank you
prepared by – Dawit Yohannes
You might also like
- All Sons & Daughters - SongbookDocument26 pagesAll Sons & Daughters - SongbookJesseJ.CannonII100% (2)
- Skin Diseases PresentationDocument23 pagesSkin Diseases PresentationDaniTadeNo ratings yet
- Scabies and ImpetigoDocument13 pagesScabies and ImpetigoValabhoju Bindu MadhaviNo ratings yet
- IZZ - PiodermaDocument51 pagesIZZ - PiodermavivilmNo ratings yet
- DERMATOLOGY QuinterDocument177 pagesDERMATOLOGY QuinterstaceyatienoomaNo ratings yet
- Eczema and DermatitisDocument47 pagesEczema and DermatitisDeborah ChemutaiNo ratings yet
- Superficial Mycoses Group 4Document38 pagesSuperficial Mycoses Group 4prudence azenaborNo ratings yet
- Derma ADDocument49 pagesDerma ADFatima Marwa Teo MaghinayNo ratings yet
- Skin Conditions Part II-1Document54 pagesSkin Conditions Part II-1mohamedkallon1996No ratings yet
- Skin Bacterial Diseases - Part - IDocument9 pagesSkin Bacterial Diseases - Part - IElijah WoodNo ratings yet
- 2F and 2H Lecture 10Document50 pages2F and 2H Lecture 10Mark PalomarNo ratings yet
- Superficial Fungal Infections of The Skin VoiceoverDocument67 pagesSuperficial Fungal Infections of The Skin VoiceoverMedo JT100% (1)
- Derma 2Document40 pagesDerma 2tyleree3No ratings yet
- Derma RXDocument46 pagesDerma RXBayisa GirmaNo ratings yet
- Case Report InfeksiDocument82 pagesCase Report InfeksithiwiekyuNo ratings yet
- Bullous Disorders, Bacterial and Fungal Skin InfectionsDocument95 pagesBullous Disorders, Bacterial and Fungal Skin InfectionsDeborah ChemutaiNo ratings yet
- PyodermaDocument81 pagesPyodermaAtikaNo ratings yet
- Skin DisordersDocument202 pagesSkin DisordersMj Briones100% (1)
- Penyakit Kulit Tropis: Heryanto SyamsuddinDocument248 pagesPenyakit Kulit Tropis: Heryanto SyamsuddinBunga Tri AmandaNo ratings yet
- Eczematous Disorders CFM REPORT 2Document32 pagesEczematous Disorders CFM REPORT 2Arianne CortezNo ratings yet
- Impetigo: Idowu O. A RN, M.SCDocument15 pagesImpetigo: Idowu O. A RN, M.SCDebby Love GoodluckNo ratings yet
- DermatitisDocument61 pagesDermatitisAlex XanderNo ratings yet
- Adebola Ogunbiyi, FMCP, FWACP, FRCP, FNAMED UCH, IbadanDocument63 pagesAdebola Ogunbiyi, FMCP, FWACP, FRCP, FNAMED UCH, Ibadanadamu mohammadNo ratings yet
- 2 EczemaDocument5 pages2 Eczemaحسين طاهر حاتم طاهرNo ratings yet
- Overview of Skin InfectionsDocument53 pagesOverview of Skin Infectionsadamu mohammadNo ratings yet
- Dermatology Cutaneous Bacterial InfectionsDocument139 pagesDermatology Cutaneous Bacterial InfectionsArianne Joy C. TamarayNo ratings yet
- Zoe Yichang Central People's HospitalDocument32 pagesZoe Yichang Central People's HospitalMohsin Tanmoy100% (1)
- Dr. R. Sekhon - Dermatology Telehealth Jan 27 MRDocument45 pagesDr. R. Sekhon - Dermatology Telehealth Jan 27 MRAnissa ADNo ratings yet
- Tinea Cruris Imp Points With ReferencesDocument35 pagesTinea Cruris Imp Points With ReferencesSyed Saqib AliNo ratings yet
- Bacterial - Viral InfectionsDocument61 pagesBacterial - Viral InfectionsMoayad NawaflehNo ratings yet
- Sarcoptes Scabiei: ScabiesDocument39 pagesSarcoptes Scabiei: ScabiesEx CalioseNo ratings yet
- Cutaneous InfectionsDocument148 pagesCutaneous InfectionsPratzNo ratings yet
- Dermatology 3Document24 pagesDermatology 3حسين طاهر حاتم طاهرNo ratings yet
- ImpetigoDocument24 pagesImpetigoIvan Sitohang100% (2)
- Ringworm (Dermatophytosis)Document20 pagesRingworm (Dermatophytosis)Santosh BhandariNo ratings yet
- Dermatology ReVIsION.Document8 pagesDermatology ReVIsION.Aadan BilowNo ratings yet
- Important Diseases1 - Skin and EyeDocument40 pagesImportant Diseases1 - Skin and EyePeiyong TanNo ratings yet
- Lichen PlanusDocument6 pagesLichen Planusأحمد عبد الوهابNo ratings yet
- Skin Infestation PDFDocument30 pagesSkin Infestation PDFHampson MalekanoNo ratings yet
- Skin Disease: Roshana MallawaarachchiDocument51 pagesSkin Disease: Roshana MallawaarachchiRoshana Mallawaarachchi100% (1)
- 2.dermatologic Pharmacotherapy (Autosaved)Document214 pages2.dermatologic Pharmacotherapy (Autosaved)Waaqoo Guutuu Waaqoo GuutuuNo ratings yet
- 11 DermatitisDocument39 pages11 DermatitisLQYNo ratings yet
- Maryville NURS 623 ExamDocument14 pagesMaryville NURS 623 ExamWizzardNo ratings yet
- Bacterial Infections of SkinDocument41 pagesBacterial Infections of SkinYovan Prakosa100% (1)
- finalPEDIATRIC DERMATOLOGYDocument58 pagesfinalPEDIATRIC DERMATOLOGYShiva RamNo ratings yet
- MF3 - LeprosyDocument25 pagesMF3 - LeprosyAnnbe BarteNo ratings yet
- Dermatology Primer: Selected Skin Diseases and Treatment Tailored For The Athletic TrainerDocument64 pagesDermatology Primer: Selected Skin Diseases and Treatment Tailored For The Athletic TrainerSilviu100% (1)
- Integumentary Disorders (New)Document41 pagesIntegumentary Disorders (New)coosa liquorsNo ratings yet
- Atopic DermatitisDocument43 pagesAtopic DermatitisSaurav Arora100% (2)
- Blistering DisordersDocument7 pagesBlistering DisordersSaman SarKoNo ratings yet
- ScabiesDocument39 pagesScabiesShahzeb KhanNo ratings yet
- Atopic® 0.1% Ointment Back To The Typical Life: Saleem AlawnehDocument46 pagesAtopic® 0.1% Ointment Back To The Typical Life: Saleem AlawnehMuhammed AskarNo ratings yet
- ArthropodsDocument42 pagesArthropodsKateNo ratings yet
- Contagious Ecthyma (Contagious Pustular Dermatitis, Orf, Scabby Mouth, Soremouth)Document9 pagesContagious Ecthyma (Contagious Pustular Dermatitis, Orf, Scabby Mouth, Soremouth)Tamiru LegesseNo ratings yet
- Communicable Diseases2Document46 pagesCommunicable Diseases2wanjalakijanahNo ratings yet
- l7 Common Bacterial Infection in DermatologyDocument35 pagesl7 Common Bacterial Infection in DermatologyOmar HamwiNo ratings yet
- Vernal Keratoconjunctivitis: - Dr. Zulfiqar AliDocument30 pagesVernal Keratoconjunctivitis: - Dr. Zulfiqar AliAsad FrazNo ratings yet
- Derma NotesDocument52 pagesDerma NotesUsmanNo ratings yet
- Psoriasis: Presented By: Rana AhmedDocument81 pagesPsoriasis: Presented By: Rana AhmedIbrahim Sidahmed AliNo ratings yet
- Folliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesFrom EverandFolliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesNo ratings yet
- Complete Medical Guide for Disease Volume VII; Atopic DermatitisFrom EverandComplete Medical Guide for Disease Volume VII; Atopic DermatitisNo ratings yet
- Introduction To AlgebraDocument477 pagesIntroduction To AlgebraFranknire IgNo ratings yet
- The Effects of TikTok Usage On Grade 11 Students of San Fabian National High SchoolDocument16 pagesThe Effects of TikTok Usage On Grade 11 Students of San Fabian National High SchoolKzz PerezNo ratings yet
- Qualitative ResearchDocument48 pagesQualitative ResearchJam BarredoNo ratings yet
- 1st and Scond Kalma SharifDocument20 pages1st and Scond Kalma SharifQamarManzoorNo ratings yet
- Kunci Jawaban Pat X Bahasa InggrisDocument5 pagesKunci Jawaban Pat X Bahasa InggrisjuraganshuleeNo ratings yet
- Relationship Between Market Orientation, Entrepreneurial Orientation, and Firm Performance in Thai Smes: The Mediating Role of Marketing CapabilitiesDocument25 pagesRelationship Between Market Orientation, Entrepreneurial Orientation, and Firm Performance in Thai Smes: The Mediating Role of Marketing CapabilitiesMahipal18No ratings yet
- Plaintiffs-Appellants Opening Brief: Ronald Pierce et al vs. Chief Justice Tani Cantil-Sakauye Judicial Council Chair and Steven Jahr Judicial Council Administrative Director - Federal Class Action Lawsuit for Alleged Illegal Use of California Vexatious Litigant Law by Family Court Judges in Child Custody Disputes - Ventura County - Tulare County - Sacramento County - San Mateo County - Santa Clara County - Riverside County - San Francisco County - US District Court for the Northern District of California Judge Jeffrey S. White - US Courts for the Ninth Circuit - 9th Circuit Court of Appeal Class Action for Injunctive and Declaratory ReliefDocument285 pagesPlaintiffs-Appellants Opening Brief: Ronald Pierce et al vs. Chief Justice Tani Cantil-Sakauye Judicial Council Chair and Steven Jahr Judicial Council Administrative Director - Federal Class Action Lawsuit for Alleged Illegal Use of California Vexatious Litigant Law by Family Court Judges in Child Custody Disputes - Ventura County - Tulare County - Sacramento County - San Mateo County - Santa Clara County - Riverside County - San Francisco County - US District Court for the Northern District of California Judge Jeffrey S. White - US Courts for the Ninth Circuit - 9th Circuit Court of Appeal Class Action for Injunctive and Declaratory ReliefCalifornia Judicial Branch News Service - Investigative Reporting Source Material & Story IdeasNo ratings yet
- Deshmukh Gruh UdyogDocument10 pagesDeshmukh Gruh UdyogJITNo ratings yet
- Proffer Nick EjakDocument4 pagesProffer Nick EjakWXYZ-TV Channel 7 DetroitNo ratings yet
- Ras Self Reflection FormDocument2 pagesRas Self Reflection Formapi-321025320No ratings yet
- Squash MojosDocument5 pagesSquash Mojosamelia pajarilloNo ratings yet
- PracticumDocument3 pagesPracticummataraiNo ratings yet
- Individual Inventory Form Personalbackground: Binmaley Catholic School, Inc. Binmaley, PangasinanDocument3 pagesIndividual Inventory Form Personalbackground: Binmaley Catholic School, Inc. Binmaley, PangasinanroseNo ratings yet
- Phil. Canonical AuthorsDocument29 pagesPhil. Canonical AuthorsCharlotte OlsenNo ratings yet
- Lesson Plan For TP2Document15 pagesLesson Plan For TP2Thiên LýNo ratings yet
- JNTU Old Question Papers 2007Document7 pagesJNTU Old Question Papers 2007Srinivasa Rao G100% (1)
- Chapter Four Non-Isothermal Reactors DesignDocument16 pagesChapter Four Non-Isothermal Reactors Designمصطفى العباديNo ratings yet
- Reviewer S008 - Its Databases - National - 2022Document8 pagesReviewer S008 - Its Databases - National - 2022Yasir RyaldiNo ratings yet
- Reservoir Engineers Competency Matrix - Society of Petroleum EngineersDocument5 pagesReservoir Engineers Competency Matrix - Society of Petroleum Engineersbillal_m_aslamNo ratings yet
- Sue MillerDocument27 pagesSue MillerCAILNo ratings yet
- Continental - airlinesMIT Case StudyDocument14 pagesContinental - airlinesMIT Case StudyZoeyHakimNo ratings yet
- Cefepime: Ellie Marie F. Royales - PH-3ADocument10 pagesCefepime: Ellie Marie F. Royales - PH-3AEllie Marie RoyalesNo ratings yet
- Linear Programming: Basic Concepts: Irwin/Mcgraw-HillDocument30 pagesLinear Programming: Basic Concepts: Irwin/Mcgraw-Hillgttrans111No ratings yet
- Philippine - Airlines - Inc. - v. - Santos - JR - DigestDocument2 pagesPhilippine - Airlines - Inc. - v. - Santos - JR - DigestAllen Windel BernabeNo ratings yet
- Determining Relationship Between Strategic Human RDocument9 pagesDetermining Relationship Between Strategic Human RHarrison LopesNo ratings yet
- Praying Against The Spirit of The Valley (Dr. D.K. Olukoya (Olukoya, Dr. D.K.) )Document45 pagesPraying Against The Spirit of The Valley (Dr. D.K. Olukoya (Olukoya, Dr. D.K.) )ovie stephen100% (3)
- A Handbook: Epicyclic GearingDocument8 pagesA Handbook: Epicyclic GearingrafeipNo ratings yet
- Triterion GH JournalDocument7 pagesTriterion GH JournalEtienne LNo ratings yet
- Scripts RhcsaDocument3 pagesScripts RhcsaDeshfoss Deepak100% (1)