Professional Documents
Culture Documents
Bones and Joints: Bone Is A Specialised Connective Tissue Which Has
Bones and Joints: Bone Is A Specialised Connective Tissue Which Has
Uploaded by
vaishnavi0 ratings0% found this document useful (0 votes)
25 views34 pagesBone provides structural support, protects organs, enables movement, and produces blood cells. It consists of compact and spongy bone, and undergoes modeling and remodeling throughout life by osteoblasts, osteocytes, and osteoclasts. Bone fractures heal through inflammatory, reparative, and remodeling phases over 6-8 weeks. Osteoporosis and osteomyelitis are bone diseases characterized by low bone mass and bone inflammation, respectively. Joints include fibrous, cartilaginous, and synovial joints, and diseases like osteoarthritis, rheumatoid arthritis, and gouty arthritis cause joint inflammation and damage.
Original Description:
Original Title
Bones and Joints
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentBone provides structural support, protects organs, enables movement, and produces blood cells. It consists of compact and spongy bone, and undergoes modeling and remodeling throughout life by osteoblasts, osteocytes, and osteoclasts. Bone fractures heal through inflammatory, reparative, and remodeling phases over 6-8 weeks. Osteoporosis and osteomyelitis are bone diseases characterized by low bone mass and bone inflammation, respectively. Joints include fibrous, cartilaginous, and synovial joints, and diseases like osteoarthritis, rheumatoid arthritis, and gouty arthritis cause joint inflammation and damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
25 views34 pagesBones and Joints: Bone Is A Specialised Connective Tissue Which Has
Bones and Joints: Bone Is A Specialised Connective Tissue Which Has
Uploaded by
vaishnaviBone provides structural support, protects organs, enables movement, and produces blood cells. It consists of compact and spongy bone, and undergoes modeling and remodeling throughout life by osteoblasts, osteocytes, and osteoclasts. Bone fractures heal through inflammatory, reparative, and remodeling phases over 6-8 weeks. Osteoporosis and osteomyelitis are bone diseases characterized by low bone mass and bone inflammation, respectively. Joints include fibrous, cartilaginous, and synovial joints, and diseases like osteoarthritis, rheumatoid arthritis, and gouty arthritis cause joint inflammation and damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 34
BONES AND JOINTS
Bone is a specialised connective tissue which has
structural ,protective,metabolic and
haemopoietic function.attachment of muscles &
tendons,movement.
Regions :Epiphysis, metaphysis ,Diaphysis.
Types of bone: 1.Compact Or Cortical
2.Cancellous Or spongy –red marrow
Cells of bone tissue: Osteoblasts,Osteocytes &
Osteoclasts
Osteoid –unmineralised matrix
Ossification: 1.membranous 2.Endochondral
Bone fracture & healing
Fracture—Discontinuity of the bone,
Types;simple,compound, pathological
Phases: 1.inflammatory phase -haemorrahge-
inflammatory cells-granulation tissue-non-
lamellar or woven bone--soft tissue callus
2.Reparative Phase- soft tissue callus replaced
by Lamellar bone and is mineralised.3weeks
weight bearing can be tolerated.
3. Remodelling Phase.-Osteoclasts
Process of healing takes 6-8 weeks
Complications:non
union,Pseudoarthrosis,deformity
Osteoporosis
Reduced bone mass leading to porosity of
bones –more resorption of bone than
formation.
-Primary: Postmenopausal, old age ( oestrogen
, anabolic steroid effect reducing )
Secondary:1.Hyperthyroidism
2.Hyperparathyroidism.3. Drugs-steroids
4.malabsorption ,malnutrition.
Complications : patholgical fracture.
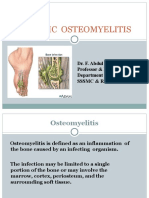
Osteomyelits
Inflammation of the bone and marrow
Types: 1.Pyogenic 2.tuberculous
Pyogenic Osteomyelitis :80-90%
Staphylococcus aureus-10-20%
Esch.coli,pseudomonas,klebsiella,haemophilus
Portal of entry; 1.skin –compound fracture
2. tooth abscess –maxilla,mandible
3.Blood borne : boil & paranychia
4. surgical procedure:
Osteomyelits-pathogenesis
Metaphysis -capillary loops-slowing of blood
Organism reaches marrow
Acute inflammatory reaction( exudate formed )
Necrosis of bone due to pressure & pus
formation ( Sequestrum).
Pus penetrates periosteum & skin to form
draining sinus
Reactive New Bone
( Involcrum)formationaround the periphery of
inflammatory reaction
Osteomyelitis - Pyogenic
Complications ;1.Septecemia 2.acute
suppurative arthritis 3.Pathological fracture
4.squamous cell carcinoma 5.Amyloidosis
Clinical features.-fever,chills,malaise, pain at
site
Diagnosis : .1.Radiological
2.blood culture 3. biopsy
Tuberculous Osteomyelitis
Mycobacterium tuberculosis
Source : Blood borne from a focus of pulmonary
or extrapulmonary disease
Site : spine ( thoracic & Lumbar vertebra ) Pott’s
abscess.caseous necrosis with giant cells
Clinical features :low grade evening rise of
temp.pain on movement,weight loss
Complications:1.destruction of vertebra2.Psoas
abscess 3. TB arthritis
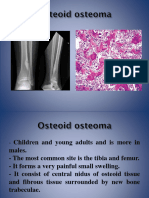
Bone tumours-Osteogenic sarcoma
Most common, highly malignant of bone tumours.
Characterised by formation of bone matrix or
osteoid ( unmineralised bone ) by malignant cells.
Age /sex :10-20 years, Boys more affected.
Site: arises from Metaphysis of long bones of
extremities- Lower end of femur,upper tibia,upper
fibula,proximal humerus.
Osteogenic sarcoma-Morphology
Gross: big ,bulky,grey-white in colour,gritty.
Shows areas of haemorrhage & cystic
degeneration .tumour extends into the adjacent
soft tissue ( Mutton leg appearance )
Microscopy : pleomorphic tumour cells with
large hyperchromatic nuclei & show mitotic
figures.Bizarre tumour giant cells are common.
Production of Osteoid by malignant tumour
cells is the diagnostic feature.
Osteogenic sarcoma ( contd )
Clinical features :painful,progressively
enlarging mass around the knee or other
involved site. The area is swollen and
tender.the adjacent joint function is affected.
Radiographic : Codman Triangle-space
between cortex and elevated periosteum
appears as a triangular shadow. Sun-Ray –
parallel lines of mineral deposition in the
periosteum.
Spread: Local ; Blood spread –lungs,brain
Joints
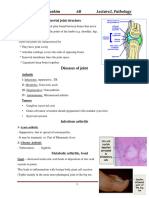
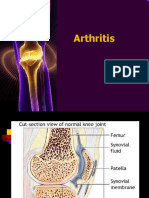
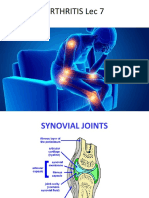
Joints formed by two or more bones provide
movements and mechanical stability to the
body. The joints consist of articular cartilage
with a joint space ( synovial cavity ) lined by
synovial membrane. The articular cartilage
provides friction free movement within the
joints and acts as a shock absorber. The
synovial cavity contains clear & viscous
synovial fluid containing hyaluronic acid.The
fluid acts as a lubricant & supplies nutrient to
the articular hyaline cartilage.
Joints
1.Fibrous Joints: no movement-skull,maxilla
2.Cartilaginous Joints : slight movement
Symphysis Pubis & bodies of vertebra
3. Synovial joints : Free movement
Osteoarthritis
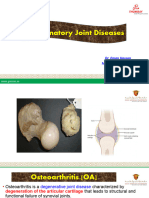
Osteoarthritis is a degenerative ,slowly
progressive, non-inflammatory joint disease.
Osteoarthritis is a misnomer as there is no
inflammatory reaction: Osteoarthosis will be a
better term.
Involves articular cartilage & subchondral bone.
Joints affected; weight bearing –knee,hips,spine
Non-weight bearing-inter-phalangeal joints of
fingers,first carpometacarpal&tarsometatarsal
Osteoarthritis
1. Primary :aging process
2. Secondary:younger individuals-
a) previous injury to a joint b) diabetes
c)haemochromatosis
Pathogenesis & morphology :
Changes in the articular cartilage; cracks develop
on the surface of articular cartilage-synovial
fluid flows along these cracks & penetrates
deeper into the cartilage.Dead pieces of
cartilage fragment are shed as loose
bodies(Joint mices)into the synovial cavity.
Osteoarthritis
Changes in the subchondral bone: After the
articular cartilage is sloughed off, the bone
beneath it ( subchondral bone) is exposed &
becomes the new articular surface. The bone
appears thick,smooth,shiny giving it polished
ivory appearance ( bone eburnation). Synovial
fluid enters bone marrow forming subchondral
bone cyst. The loculated fluid collection
increases in size surrounded by reactive bone
wall.Mushroom-shaped pearly-grayish bony
outgrowths(spurs) called Osteophytes develop
in the periphery of the joint surface.
Osteoarthritis
Clinical features:
Slowly progressive disease & causes long-
term disability
Deep aching pain which worsens with joint
movement & is relieved by rest.
Joint swollen, tender & may demonstrate
crepitus
Osteophytes in spine can cause nerve root
compression.
Heberden nodes-osteophytes in distal
interphalangeal joints
Rheumatoid Arthritis
Rheumatoid arthritis is a chronic ,progressive,
Inflammatory,Autoimmune disease.It is a
systemic disorder where inflammatory changes
not only affect the joints but also blood vessels,
heart,skin.Antigen-antibody complexes are
found in the blood& synovial fluid. Genetic
factors may be involved.
RA is an acute febrile condition usually with
periods of remission & exacerbation of varying
lengths of time.
Rheumatoid arthritis
Most commonly affects proximal
interphalangeal & metacarpophalangeal
joints.other jts: feet,elbow,knee,ankle,spine.
With each febrile exacerbation,there is
additional & cumulative damage to the joints
leading to increasing deformity,pain and loss of
function.
Age/Sex; 40-70 years– Women more affected
Rheumatoid Arthritis- Morphology
Synovium: Gross : Involved synovium is oedematous and thickened.
Microscopy:1.Synovial hyperplasia which may form finger-like
structures(villi).
2.dense inflammatory infiltrate of lympocytes
Plasma cells & Macrophages.
3.Pannus formation-pannus consists of inflammatory cells,granulation
tissue and synovial stroma.Pannus grows over articular cartilage&
destroys it.It bridges the apposing bones forming a Fibrous Ankylosis
which may ossify to form a Bony Ankylosis.
Rheumatoid Arthritis
Clinical Features: slow and insidious in onset.
Presents with malaise,fatigue,fever. The
affected joints are swollen,warm,painful and
stiff on arising or following inactivity.
Deformities:radial deviation of the wrist,ulnar
deviation of the fingers,flexion-hyperextension
abnormalities of the fingers(swan neck )
Laboratory findings: 1.Rheumatoid
factor2.Anti-CCP( cyclic citrullinated peptide )
3.antinuclear antibody 4. ESR . 5. CRP
Gouty Arthritis
Gout is characterised by hyperuricemia and deposition
of urate crystals in joints & kidneys.
Disorder of Purine metabolism.
Classification :1. Primary ( idiopathic) hyperuricemia
occurs without any disease.
2.secondary :a) Increased catabolism of nucleic acid due
to increased cell turnover-leukemia, cancer b)
decreased excretion of uric acid with normal production.
( eg. Chronic renal failure)
Gouty Arthritis
Uric acid is the end-product of purine metabolism.
Gouty arthritis is usually an extremely painful
attack with a rapid onset of inflammation.The
iflammation is precipitated by the deposition of uric
acid crystals in the synovium & fluid within the
joint.The white cells engulf the crystals& release
chemicals which promote inflammation which
causes pain,heat & redness of the joint.
Diet rich in purine : meat, fish
Gouty Arthritis-Morphology
Acute arthritis : characterised by oedema, congestion and
dense infiltration of synovium by neutrophils.MSU
( monosodium urate)crystals are long,needle shaped and
arranged in small clusters in the synovium.
Chronic tophaceous arthritis:It follows repeated attacks of
acuteattacks.The synovium shows fibrosis,thickening and
infiltration by inflammatory cells.It forms a pannus which
destroys the articular cartilage and triggers juxta-articular
bone erosion.
Gouty Arthritis
Tophi ; lesions consisting of large aggregates of
monosodium urate (MSU) crystals,surrounded by
inflammatory cells .They are pathognomic of gout
and are commonly found in the articular
cartilage,periarticular ligaments, tendons & soft
tissues.Microscopically they consist of aggregates
of MSU surrounded by macrophages,lympocytes
and foreign body giant cells.
Gouty Arthritis
Clinical features:1. common in men than
women
2. age : after 30 years 3. commonest site--- Big
Toe—other sites:ankle,heel& wrist
4. Four stages-a) asymptomatic hperuricemia
b)acute gouty arthritis c)intercritical gout
d)chronic tophoceous gout. Initial acute attack
resolves completely followed by asymptomatic
interval( intercritical).Recurrent attacks lead to
deformity.5.high serum uric acid & presence of
uric acid crystals in the synovial fluid .
You might also like
- 2018 CSB520 ANSWERS Skeletal System PathologyDocument4 pages2018 CSB520 ANSWERS Skeletal System PathologyNathanNo ratings yet
- Eric OsteomyelitisDocument22 pagesEric OsteomyelitisJonathan Delos ReyesNo ratings yet
- Referat OsteoarthritisDocument4 pagesReferat OsteoarthritismarindadaNo ratings yet
- L 2 Pathology, Joints Diseases Lecture NotesDocument4 pagesL 2 Pathology, Joints Diseases Lecture Notesamrwheed9No ratings yet
- Due To The Sharp Bending of The Vessels in The Metaphysic and Also by The Hematoma Formed After InjuryDocument6 pagesDue To The Sharp Bending of The Vessels in The Metaphysic and Also by The Hematoma Formed After InjuryBashar EbrahimNo ratings yet
- Pathology of Bone and Soft Tissue-LectureDocument52 pagesPathology of Bone and Soft Tissue-Lecturejohnwickshopping79No ratings yet
- JointsDocument68 pagesJointsLaine ZeeNo ratings yet
- Osteoarthritis (Oa) : Prakash Thakulla InternDocument48 pagesOsteoarthritis (Oa) : Prakash Thakulla InternPrakash ThakullaNo ratings yet
- Disorders of Bone II-2Document59 pagesDisorders of Bone II-2Guhan DergNo ratings yet
- OsteomyelitisDocument147 pagesOsteomyelitisAnkit Agur100% (1)
- OSTEOARTHRITISDocument36 pagesOSTEOARTHRITISHzm Mus83% (12)
- Osteomyelitis LaikaDocument4 pagesOsteomyelitis LaikaAl Lai KaNo ratings yet
- 4 Curs Osteomielita Engl BunDocument41 pages4 Curs Osteomielita Engl BunCatalin PaulNo ratings yet
- Arthritis 180325095830 PDFDocument77 pagesArthritis 180325095830 PDFHesoca HuxNo ratings yet
- Bone TheoryDocument19 pagesBone Theoryسہاجہدةه لہلہهNo ratings yet
- Osteoarthritis & Rheumatoid ArthritisDocument60 pagesOsteoarthritis & Rheumatoid ArthritisSaya MenangNo ratings yet
- Pathology Muskulo SkletalDocument68 pagesPathology Muskulo SkletalwilliamNo ratings yet
- 3-Students - Arthritis Copy - 231017 - 184459 - 231018 - 14 - 231018 - 165509Document36 pages3-Students - Arthritis Copy - 231017 - 184459 - 231018 - 14 - 231018 - 165509Moayad IsmailNo ratings yet
- Osteomyelitis 130708212636 Phpapp01Document107 pagesOsteomyelitis 130708212636 Phpapp01merikasorNo ratings yet
- Orthopaedic SlidesDocument163 pagesOrthopaedic SlidesVivian ChepkemeiNo ratings yet
- Bone Infections For PMDocument31 pagesBone Infections For PM202201666No ratings yet
- Osteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRDocument28 pagesOsteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRgita cahayaNo ratings yet
- Morpho of Bone JointDocument2 pagesMorpho of Bone JointHassan AhmadNo ratings yet
- OsteomyelitisDocument29 pagesOsteomyelitistaha saadNo ratings yet
- L25 Inflammatory Joint DiseasesDocument27 pagesL25 Inflammatory Joint Diseases8ht2twrg5fNo ratings yet
- Review Sistem GerakDocument63 pagesReview Sistem GerakDanur AdiNo ratings yet
- MSK Lecture DR - Ba 2014 15Document55 pagesMSK Lecture DR - Ba 2014 15marina_shawkyNo ratings yet
- Non Neoplastic Diseases of BoneDocument45 pagesNon Neoplastic Diseases of BoneKNo ratings yet
- Arthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR JaneDocument73 pagesArthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR Janeumanantini06No ratings yet
- General OrthopaedicsDocument50 pagesGeneral Orthopaedicsضبيان فرحانNo ratings yet
- Presentation 1Document120 pagesPresentation 1Khurram ChauhanNo ratings yet
- WK 2 NFK 202Document88 pagesWK 2 NFK 202JSeasharkNo ratings yet
- Inflammatory Lesions of The JAW: Bhavika Pol Vhatkar 1 Yr PGDocument132 pagesInflammatory Lesions of The JAW: Bhavika Pol Vhatkar 1 Yr PGArpita SankhwarNo ratings yet
- Knee Anatomy & Disorders: By: Nour Abu Al-Sha'arDocument28 pagesKnee Anatomy & Disorders: By: Nour Abu Al-Sha'arAlisha FatimaNo ratings yet
- Osteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Document64 pagesOsteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Linda SugiartoNo ratings yet
- Orthopedic Tumors and OsteoarthritisDocument6 pagesOrthopedic Tumors and OsteoarthritisSai Snigdha MohantyNo ratings yet
- 7 - Knee Joint - D3Document28 pages7 - Knee Joint - D3aslooclt100% (1)
- Year 2 Semester 2Document88 pagesYear 2 Semester 2JSeasharkNo ratings yet
- Disease of Skeletal Muscle and JointsDocument7 pagesDisease of Skeletal Muscle and JointsNur Amirah FarhanahNo ratings yet
- Xray of Bones in OsteomyelitisDocument35 pagesXray of Bones in OsteomyelitisBukola AjokeNo ratings yet
- Chronic OsteomylitisqDocument5 pagesChronic Osteomylitisqdrahmed1028No ratings yet
- Osteomyelitis: Mariamawit B Dbu, College of MedicineDocument34 pagesOsteomyelitis: Mariamawit B Dbu, College of MedicinedenekeNo ratings yet
- Bone andDocument33 pagesBone andSuci MayveraNo ratings yet
- OsteomyelitisDocument41 pagesOsteomyelitisArumpaavai PugazhiniNo ratings yet
- OsteoarthritisDocument25 pagesOsteoarthritisRaymund Christopher Dela PeñaNo ratings yet
- Bone 2Document43 pagesBone 2kazelio2017No ratings yet
- Chronic Osteomyelitis: Dr. F. Abdul Khader Professor & HOD Department of Orthopaedics SSSMC & RiDocument31 pagesChronic Osteomyelitis: Dr. F. Abdul Khader Professor & HOD Department of Orthopaedics SSSMC & RiDr. F. Abdul KhaderNo ratings yet
- Inflammatory Disease of BonesDocument93 pagesInflammatory Disease of BonesNelson LagatNo ratings yet
- Osteoarthritis and OsteoporosispptDocument92 pagesOsteoarthritis and OsteoporosispptDian Puspa0% (1)
- Curs 9 Imagistica MSKDocument62 pagesCurs 9 Imagistica MSKn bNo ratings yet
- Skeletal DiseasesDocument3 pagesSkeletal Diseasessweetheart10No ratings yet
- Osteomyelitis: ClassificationDocument5 pagesOsteomyelitis: Classificationthanuja mathewNo ratings yet
- JointsDocument43 pagesJointskamaluNo ratings yet
- Joint DiseaseDocument5 pagesJoint DiseaseKimrose TampusNo ratings yet
- Bone and Joint TBDocument15 pagesBone and Joint TBSunil Kumar PdNo ratings yet
- 5 Inflammation of Bone NewDocument15 pages5 Inflammation of Bone Newnightfury200313No ratings yet
- Arthritis MBBS FDocument49 pagesArthritis MBBS FThoufic AhmedNo ratings yet
- Osteonecrosis: Avascular NecrosisDocument8 pagesOsteonecrosis: Avascular NecrosisJezreel BonaNo ratings yet
- 12 Rheumatoid ArthritisDocument9 pages12 Rheumatoid ArthritisAhmed aljumailiNo ratings yet
- AnnapooraniDocument232 pagesAnnapooranivaishnaviNo ratings yet
- Motor LearningDocument62 pagesMotor LearningvaishnaviNo ratings yet
- Splints BracesDocument18 pagesSplints BracesvaishnaviNo ratings yet
- TSNJ - Volume 24 - Issue 1 - Pages 252-273Document22 pagesTSNJ - Volume 24 - Issue 1 - Pages 252-273vaishnaviNo ratings yet
- MG 2Document5 pagesMG 2vaishnaviNo ratings yet
- Kues 2015 HowtoMeasuretheImpactofPremensDocument47 pagesKues 2015 HowtoMeasuretheImpactofPremensvaishnaviNo ratings yet
- Masters of Physiotherapy (MPT) Degree Course First Year MPTDocument14 pagesMasters of Physiotherapy (MPT) Degree Course First Year MPTvaishnaviNo ratings yet
- MG 1Document32 pagesMG 1vaishnaviNo ratings yet
- Bmjopen 2020 July 10 7 Inline Supplementary Material 1Document7 pagesBmjopen 2020 July 10 7 Inline Supplementary Material 1vaishnaviNo ratings yet
- 12 Biomechanical NewDocument9 pages12 Biomechanical NewvaishnaviNo ratings yet
- Ways of Coping With Premenstrual Change - Development and Validation of A Premenstrual Coping Measure - BMC Women's Health - Full TextDocument4 pagesWays of Coping With Premenstrual Change - Development and Validation of A Premenstrual Coping Measure - BMC Women's Health - Full TextvaishnaviNo ratings yet
- Mac Pmss BF May2014 CopyrightDocument1 pageMac Pmss BF May2014 CopyrightvaishnaviNo ratings yet
- AneeshaDocument100 pagesAneeshavaishnaviNo ratings yet
- Chest Xray Viii SemDocument76 pagesChest Xray Viii SemvaishnaviNo ratings yet
- Biomech of Elbow JTDocument19 pagesBiomech of Elbow JTvaishnaviNo ratings yet
- Elbow JointDocument5 pagesElbow JointvaishnaviNo ratings yet
- 15759-Texto Do Artigo-105795-1-10-20140911Document9 pages15759-Texto Do Artigo-105795-1-10-20140911vaishnaviNo ratings yet
- Cardiac Arrest and RescuecitationDocument50 pagesCardiac Arrest and RescuecitationvaishnaviNo ratings yet
- Cervical ExaminationDocument7 pagesCervical ExaminationvaishnaviNo ratings yet
- Atelectasis 181227153553Document59 pagesAtelectasis 181227153553vaishnaviNo ratings yet
- Abg 24.6.2020 Viii SemDocument37 pagesAbg 24.6.2020 Viii SemvaishnaviNo ratings yet
- Ankle and FootDocument4 pagesAnkle and FootvaishnaviNo ratings yet
- Aerobic ExerciseDocument6 pagesAerobic ExercisevaishnaviNo ratings yet
- Phy 2Document20 pagesPhy 2vaishnaviNo ratings yet
- Q.P. Code: 278154Document7 pagesQ.P. Code: 278154vaishnaviNo ratings yet
- Abg Analysis and InterpretationDocument27 pagesAbg Analysis and InterpretationvaishnaviNo ratings yet
- Abs 1Document23 pagesAbs 1vaishnaviNo ratings yet
- Phy 1Document22 pagesPhy 1vaishnaviNo ratings yet
- Q.P. Code: 278153Document7 pagesQ.P. Code: 278153vaishnaviNo ratings yet
- Abs 2Document20 pagesAbs 2vaishnaviNo ratings yet
- Drug Induced Kidney DeseaseDocument12 pagesDrug Induced Kidney DeseaseNurul MasyithahNo ratings yet
- Interpretation of The Reptile Blood ProfileDocument8 pagesInterpretation of The Reptile Blood ProfileAndre NgoNo ratings yet
- Natural Ways To Reduce Uric Acid in The BodyDocument17 pagesNatural Ways To Reduce Uric Acid in The Bodyaj dancel marcosNo ratings yet
- JCM 12 06173Document20 pagesJCM 12 06173Taulant MukaNo ratings yet
- Gout and Chinese MedicineDocument7 pagesGout and Chinese MedicineVictoria Balmus100% (1)
- BSN 3-B (GROUP 2) - CLINICAL CASE ANALYSIS - Arthritis (REVISED)Document7 pagesBSN 3-B (GROUP 2) - CLINICAL CASE ANALYSIS - Arthritis (REVISED)Florence Dumawal FariñasNo ratings yet
- Degradation of Purine PDFDocument36 pagesDegradation of Purine PDFShrey SundriyalNo ratings yet
- Metabolism of NucleoproteinsDocument71 pagesMetabolism of NucleoproteinsMi PatelNo ratings yet
- Staghorn Calculi: Department of SurgeryDocument22 pagesStaghorn Calculi: Department of SurgeryHana FauziNo ratings yet
- Daun BinahongDocument9 pagesDaun Binahongkampus merdeka21No ratings yet
- Biochemical Analysis of BloodDocument67 pagesBiochemical Analysis of BloodbhavanaNo ratings yet
- Pathogenesis of GoutDocument3 pagesPathogenesis of GoutDebby ElviraNo ratings yet
- DS 262 265ab 267Document4 pagesDS 262 265ab 267ROLAND LAURENCE BARGO JARDIOLINNo ratings yet
- Gouty ArthritisDocument12 pagesGouty ArthritisManoj KandoiNo ratings yet
- Flavonoid Compounds of Tapak Liman Plant (Elephantopus Scaber) As AntihyperuricemiaDocument7 pagesFlavonoid Compounds of Tapak Liman Plant (Elephantopus Scaber) As AntihyperuricemiaNeni Sri GunartiNo ratings yet
- Estimation of Uric Acid Levels in SerumDocument6 pagesEstimation of Uric Acid Levels in Serumvicky_law_280% (5)
- Arthritis Case Presentation - Dr. KlaesDocument27 pagesArthritis Case Presentation - Dr. KlaesShanti VennamNo ratings yet
- Rheumatology MRCP1Document186 pagesRheumatology MRCP1Raouf Ra'fat Soliman100% (3)
- 0 - Management of HyperuricemiaDocument44 pages0 - Management of HyperuricemiaYayuk Abay TambunanNo ratings yet
- Hematological Complications of CHDDocument3 pagesHematological Complications of CHDHamzaNo ratings yet
- Nutritional Interventions in Heart Failure PatientsDocument32 pagesNutritional Interventions in Heart Failure PatientsandrianhoerulanwarNo ratings yet
- FINAL CASE-GOUT... PrintDocument69 pagesFINAL CASE-GOUT... PrintVelz Noli100% (3)
- Uric AcidDocument30 pagesUric AcidKesavanVeeraNo ratings yet
- APNC 520 Exam 10 Study Guide Musculoskeletal DisordersDocument15 pagesAPNC 520 Exam 10 Study Guide Musculoskeletal DisordersMariaNo ratings yet
- Group No. 6: Case 6Document12 pagesGroup No. 6: Case 6JOSLIN ROZ GALILEANo ratings yet
- Vijay ShreeDocument98 pagesVijay ShreeRafi SungkarNo ratings yet
- Analisis Kromatografi Lapis Tipis (KLT) Dan Aktivitas Antihiperurisemia Ekstrak Rebung SchizostachyumDocument13 pagesAnalisis Kromatografi Lapis Tipis (KLT) Dan Aktivitas Antihiperurisemia Ekstrak Rebung SchizostachyumEdwin SaputraNo ratings yet
- Preliminary Report of Gout Arthritis Stage Gerontic NursingDocument16 pagesPreliminary Report of Gout Arthritis Stage Gerontic NursingAulia SandraNo ratings yet
- FOCUS STUDY For FebuxostatDocument7 pagesFOCUS STUDY For FebuxostatshaheenNo ratings yet
- NPNS QuizDocument2 pagesNPNS QuizAshley TañamorNo ratings yet