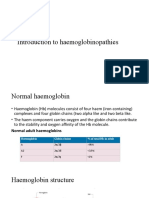
Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
47 viewsHemoglobin Metabolism
Hemoglobin Metabolism
Uploaded by
Melanie TranCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Chapter 14 Pathology RBC and Bleeding Disorders OutlineDocument19 pagesChapter 14 Pathology RBC and Bleeding Disorders OutlineNatan BabekNo ratings yet
- MLT 1027 Learning Outcome 17 MLDY HISTOLOGYDocument136 pagesMLT 1027 Learning Outcome 17 MLDY HISTOLOGYMelanie TranNo ratings yet
- Chapter 14 Red Blood CellsDocument37 pagesChapter 14 Red Blood CellsCatherine LiuNo ratings yet
- Step 2 CK Review - HematologyDocument18 pagesStep 2 CK Review - Hematologyrsmd1986No ratings yet
- Sample Chapter 8.1Document25 pagesSample Chapter 8.1Adel Hassan100% (1)
- Biochemictry: by / Amr Ashraf AwadDocument4 pagesBiochemictry: by / Amr Ashraf AwadHussein MahmoodNo ratings yet
- Hemoglobinopathy - WikipediaDocument1 pageHemoglobinopathy - WikipediaALLAH DITTO KHANNo ratings yet
- HemoglobinDocument56 pagesHemoglobinabdijorgi1No ratings yet
- Hemoglobin & Derivatives: DR. S. Irfan RazaDocument30 pagesHemoglobin & Derivatives: DR. S. Irfan RazaSyed Irfan Raza100% (1)
- Hemoglobin and Myoglobin Structure and FunctionDocument23 pagesHemoglobin and Myoglobin Structure and FunctionHarun MohamedNo ratings yet
- Dr. Niranjan Murthy H.L Assistant Professor Dept of Physiology SSMCDocument22 pagesDr. Niranjan Murthy H.L Assistant Professor Dept of Physiology SSMCnirilibNo ratings yet
- Blood Lectures 2 2017Document41 pagesBlood Lectures 2 2017Philip Abayomi VincentNo ratings yet
- 02 HemoglobinDocument78 pages02 HemoglobinpixiedustNo ratings yet
- Hemoglobin and Its Types: DR Roomi Aijaz Memon Department of Phusiology Isra University HyderabadDocument14 pagesHemoglobin and Its Types: DR Roomi Aijaz Memon Department of Phusiology Isra University HyderabadUSAMA AHMEDNo ratings yet
- 1952uwu270191 H1827272u2bdbdbd017yfndnabab Structure and Fu37373nction Mbbs 2017 BatchDocument88 pages1952uwu270191 H1827272u2bdbdbd017yfndnabab Structure and Fu37373nction Mbbs 2017 BatchRed DiggerNo ratings yet
- Haemopoiesis:: Dr. Anu Elizabeth Joy Asst. Professor Department of Physiology School of Medicine Dire Dawa UniversityDocument48 pagesHaemopoiesis:: Dr. Anu Elizabeth Joy Asst. Professor Department of Physiology School of Medicine Dire Dawa UniversityabdishakurNo ratings yet
- Introduction To HemoglobinopathiesDocument12 pagesIntroduction To HemoglobinopathiesMichael MazvidzaNo ratings yet
- تمريض الاطفال نظري 9Document64 pagesتمريض الاطفال نظري 9jadarcNo ratings yet
- Week 6 - Diagnostic Testing For HemoglobinopathiesDocument53 pagesWeek 6 - Diagnostic Testing For HemoglobinopathiesИван НегарэNo ratings yet
- 2023.LabDx - Trans01.basic Examination of BloodDocument4 pages2023.LabDx - Trans01.basic Examination of BloodstellaNo ratings yet
- Hema Midterm TransDocument19 pagesHema Midterm TransTrisha ManayaNo ratings yet
- Metabolism of HemoglobinDocument46 pagesMetabolism of Hemoglobinlayla hitaNo ratings yet
- Structure and Functions of HemeDocument62 pagesStructure and Functions of HemeBrahmesh GuntamukkalaNo ratings yet
- HGB Metabolism 1Document26 pagesHGB Metabolism 1MARTINEZ JUSTINENo ratings yet
- HemoglobinDocument7 pagesHemoglobinNinik Triayu S100% (2)
- Haemoglobin - Function, Variants, FateDocument27 pagesHaemoglobin - Function, Variants, FateXembergNo ratings yet
- Haemoglobin: Biochemistry and GeneticsDocument34 pagesHaemoglobin: Biochemistry and GeneticsPrincewill SeiyefaNo ratings yet
- 1 - AnemiaDocument25 pages1 - AnemiaDr. Anju K PailyNo ratings yet
- Hemoglobin Opa ThiesDocument34 pagesHemoglobin Opa ThiesFebri fitraNo ratings yet
- HemoglobinDocument33 pagesHemoglobinAkash JaatNo ratings yet
- 4 HGBDocument38 pages4 HGBChona_Delos_Re_1233No ratings yet
- Hema 1 ErythropoiesisDocument20 pagesHema 1 Erythropoiesismarie judimor gomezNo ratings yet
- Haemoglobin: Hiroshani Kulatunga BSC (Hons) MlsDocument36 pagesHaemoglobin: Hiroshani Kulatunga BSC (Hons) MlsNipun ShamikaNo ratings yet
- HaemoglobinDocument55 pagesHaemoglobinPhysiology by Dr RaghuveerNo ratings yet
- Hemoglobinopathy - WikipediaDocument9 pagesHemoglobinopathy - WikipediaEslam NassarNo ratings yet
- Lecture Notes-2-Sickle Cell, ThalassemiaDocument10 pagesLecture Notes-2-Sickle Cell, ThalassemiaManisanthosh KumarNo ratings yet
- 7 HemoglobinopathiesDocument34 pages7 HemoglobinopathiesAhmad SobihNo ratings yet
- Class Review: This Lecture Is Not All-InclusiveDocument127 pagesClass Review: This Lecture Is Not All-InclusiveMelanie TranNo ratings yet
- Hema Lec 1Document3 pagesHema Lec 1ETHELHYN JHANE MACOBNo ratings yet
- Week 3: Hemoglobinopathies: HB Lepore Hbe Hbs HBC HB SC Disease HPFHDocument24 pagesWeek 3: Hemoglobinopathies: HB Lepore Hbe Hbs HBC HB SC Disease HPFHUdyani AgustinaNo ratings yet
- Hemoglobin Function and Variation in Wild PopulationsDocument21 pagesHemoglobin Function and Variation in Wild PopulationsXeyale QuliyevaNo ratings yet
- Bloodsalvage and Blood Product SubstitutesDocument52 pagesBloodsalvage and Blood Product SubstitutesManny GabrielNo ratings yet
- Blood LecturesDocument128 pagesBlood LecturessrhrenaissanceNo ratings yet
- Iron Oxygen Metalloprotein Red Blood Cells Vertebrates InvertebratesDocument28 pagesIron Oxygen Metalloprotein Red Blood Cells Vertebrates InvertebratesJacob MasikaNo ratings yet
- Hemoglobin Formation:: Heme SynthesisDocument2 pagesHemoglobin Formation:: Heme SynthesisJezzah Mae CañeteNo ratings yet
- Alpha Keratin: (A) Both Type I and Type II (B) The RodDocument23 pagesAlpha Keratin: (A) Both Type I and Type II (B) The RodRuth Danielle GasconNo ratings yet
- PDF Test Bank For Rodaks Hematology 5Th Edition by Keohane Online Ebook Full ChapterDocument31 pagesPDF Test Bank For Rodaks Hematology 5Th Edition by Keohane Online Ebook Full Chapterfrancis.holden161100% (4)
- HemoglobinopathiesDocument51 pagesHemoglobinopathiesmontey007No ratings yet
- Structure, Types and Various Methods For Estimation of HaemoglobinDocument49 pagesStructure, Types and Various Methods For Estimation of HaemoglobinChandra ShekharNo ratings yet
- BloodDocument5 pagesBloodAkachukwu ObunikeNo ratings yet
- Haemolytic AnaemiasDocument5 pagesHaemolytic AnaemiasRazib HasanNo ratings yet
- Hemoglobin Metabolism: 1 HeyzgranDocument48 pagesHemoglobin Metabolism: 1 HeyzgranFrancis ValdezNo ratings yet
- Biochemistry of Blood 2Document48 pagesBiochemistry of Blood 2AMEER ALSAABRAWINo ratings yet
- Zoology Full PDF EMDocument108 pagesZoology Full PDF EMSmiruthi RavichandranNo ratings yet
- Red Blood Cells "Best Module Ever"Document4 pagesRed Blood Cells "Best Module Ever"Jose Emmanuel Dolor100% (1)
- Thals and Variants SimpleDocument36 pagesThals and Variants SimpleAli Al-QurweeNo ratings yet
- Structure of HemoglobinDocument8 pagesStructure of HemoglobinAditi RaiNo ratings yet
- Normal Hemoglobin Content: 1-Transport of Respiratory GasesDocument4 pagesNormal Hemoglobin Content: 1-Transport of Respiratory GasesDentistryNo ratings yet
- HB Electrophoresis and HPLC StudyDocument55 pagesHB Electrophoresis and HPLC Studyapi-243480627No ratings yet
- Metabolisme EritrositDocument50 pagesMetabolisme EritrositRamdhana ZaqifahNo ratings yet
- Hemoglobin ElectrophoresisDocument68 pagesHemoglobin Electrophoresisdrafq2000No ratings yet
- RBC Structure and Function (HEMA)Document7 pagesRBC Structure and Function (HEMA)April Lady Faith P. PaundogNo ratings yet
- A Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaFrom EverandA Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaNo ratings yet
- MLT 1027 Learning Outcome 14 Renal UrinaryDocument94 pagesMLT 1027 Learning Outcome 14 Renal UrinaryMelanie TranNo ratings yet
- MLT 1027 Learning Outcome 13 DigestiveDocument226 pagesMLT 1027 Learning Outcome 13 DigestiveMelanie TranNo ratings yet
- 1 - Introduction To HematologyDocument38 pages1 - Introduction To HematologyMelanie Tran100% (1)
- Class Review: This Lecture Is Not All-InclusiveDocument127 pagesClass Review: This Lecture Is Not All-InclusiveMelanie TranNo ratings yet
- Quality Control 1Document59 pagesQuality Control 1Melanie TranNo ratings yet
- RBC DisordersDocument70 pagesRBC DisordersNdor Baribolo100% (1)
- Interpreting Laboratory Results: Key PointsDocument8 pagesInterpreting Laboratory Results: Key PointsMarjorie Joy GreciaNo ratings yet
- Lecture 29-AnemiaDocument35 pagesLecture 29-AnemiaBini JaminNo ratings yet
- Coffeedent June 2021 AfternoonDocument1 pageCoffeedent June 2021 AfternoonHay DayNo ratings yet
- Anemia.: Seminar OnDocument24 pagesAnemia.: Seminar OnAlma Susan100% (1)
- Clinical Features, Diagnosis and Treatment of Heme Pigment-Induced Acute Kidney InjuryDocument7 pagesClinical Features, Diagnosis and Treatment of Heme Pigment-Induced Acute Kidney InjuryemirkurtalicNo ratings yet
- Hemolytic Anemia: NotesDocument9 pagesHemolytic Anemia: NotesRaja SharmaNo ratings yet
- Serological Tests For Cancer DetectionDocument22 pagesSerological Tests For Cancer DetectionShreeyaNo ratings yet
- MacrocytosisDocument6 pagesMacrocytosisAbdul QuyyumNo ratings yet
- MKSAP13-Hematology and OncologyDocument261 pagesMKSAP13-Hematology and OncologyimanNo ratings yet
- Heamatology Dr. Osama PDFDocument94 pagesHeamatology Dr. Osama PDFAnmar ZawahraNo ratings yet
- Vitamin B12 and FolateDocument12 pagesVitamin B12 and FolateAllessandria DimaggioNo ratings yet
- 001assessment Exam ImmunohemaDocument25 pages001assessment Exam ImmunohemaFrankenstein MelancholyNo ratings yet
- Assay Interference A Need For Increased Understanding and TestingDocument9 pagesAssay Interference A Need For Increased Understanding and Testingchali90No ratings yet
- Introduction To HematologyDocument10 pagesIntroduction To HematologyClaire Nicole100% (1)
- Hema311 Lec - Week 5 - Red Cell Structure, Metabolism, Destruction and FunctionDocument6 pagesHema311 Lec - Week 5 - Red Cell Structure, Metabolism, Destruction and FunctionJayvhie Gulane LayanNo ratings yet
- Babesiosis As A Rare Cause of Fever in The Immunocompromised Patient: A Case ReportDocument5 pagesBabesiosis As A Rare Cause of Fever in The Immunocompromised Patient: A Case ReportDaniel Alfredo Galindo ChoqueNo ratings yet
- Clinical Chemistry3Document81 pagesClinical Chemistry3Miguel Alfonso OlfatoNo ratings yet
- Hemolytic AnemiaDocument9 pagesHemolytic AnemiaTheeya QuigaoNo ratings yet
- Chronic Lymphocytic Leukemia: NCCN Guidelines For PatientsDocument82 pagesChronic Lymphocytic Leukemia: NCCN Guidelines For PatientsvnNo ratings yet
- Sickle Cell Anemia: Hba Α Β Hba …….. Α Δ Hb F ……… Α, ΓDocument29 pagesSickle Cell Anemia: Hba Α Β Hba …….. Α Δ Hb F ……… Α, ΓYolanda UriolNo ratings yet
- Hematology PPT 1Document287 pagesHematology PPT 1TarishiMalikNo ratings yet
- LP 10 Anemia 3Document43 pagesLP 10 Anemia 3Anonymous elq7jZiSNo ratings yet
- Plasma ProteinDocument57 pagesPlasma ProteinadulNo ratings yet
- RBC, Structure and FunctionDocument17 pagesRBC, Structure and FunctionAsyha KantifaNo ratings yet
- Biosynthesis of HemoglobinDocument42 pagesBiosynthesis of Hemoglobin95kodok85No ratings yet
Hemoglobin Metabolism
Hemoglobin Metabolism
Uploaded by
Melanie Tran0 ratings0% found this document useful (0 votes)
47 views26 pagesOriginal Title
7. Hemoglobin Metabolism
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
47 views26 pagesHemoglobin Metabolism
Hemoglobin Metabolism
Uploaded by
Melanie TranCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 26
Chapter 4
Hemoglobin Function and
Principles of Hemolysis
Copyright ©2019 F.A. Davis Company
Hemoglobin Synthesis
The function of the R B C’s is to produce,
package, protect, and transport hemoglobin
among various tissues
Hemoglobin
• Responsible for carrying oxygen (oxyhemoglobin)
• Pulls C O2 away from tissues
• Keep balanced p H between the blood
Copyright ©2019 F.A. Davis Company
Red Cell Composition
Heme
• 4 iron atoms iron2+ (linked through histidine a.a)
• Iron surrounded by protoporphyrin ring (multi-
step enzymatic procedure)
• ferroprotoporphyrin
Globin
• 2 pairs of globin chains made up of amino acids
• Alpha and beta chains
Copyright ©2019 F.A. Davis Company
Red Cell Composition
Hemoglobin
• 1o structure = a.a. sequence
• 2o structure = helices and non-helices
• 3o structure = globular arrangements of individual
chains
• 4o structure = tetramer formation of complete hgb
2,3-Diphosphoglycerate (2,3-D P G)
• Produced via Embden-Meyerhof pathway
• Related to oxygen affinity of hemoglobin
Copyright ©2019 F.A. Davis Company
Hemoglobin Molecule
Copyright ©2019 F.A. Davis Company
Genetics and Chain Formation of
Hemoglobin
Chromosome 11
• Genes for epsilon, beta, gamma G and A, delta
chains
Chromosome 16
• Alpha and zeta genes
3 types of hemoglobin in red cell production
• Embryonic hemoglobin
• Fetal hemoglobin
• Adult hemoglobin
Copyright ©2019 F.A. Davis Company
Hemoglobin
Embryonic hemoglobin
• Hemoglobin Gower one (ζ2, ε2)
• Hemoglobin Gower two (α2 ε2)
• Hemoglobin Portland (ζ2 γ2)
Fetal hemoglobin (3 months of fetal
development)
• Hemoglobin F (α2 γ2) – up to 90%
Copyright ©2019 F.A. Davis Company
Hemoglobin (continued)
Adult hemoglobin (3 to 6 months after
delivery)
• Hemoglobin A (α2 β2): 95% to 98%
• Hemoglobin A2 (α2 δ2): 3% to 5%
• Hemoglobin F (α2 γ2): less than 2%
Table 4.1
Copyright ©2019 F.A. Davis Company
Oxygen Dissociation (O D) Curve
The binding and release (reversible) of
oxygen from the hemoglobin molecule
1g hgb = 1.34mL oxygen
bind oxygen = oxygen-rich
release oxygen = oxygen-poor
binding causes allosteric alterations
• tense
• relaxed
Copyright ©2019 F.A. Davis Company
Oxygen Dissociation (O D) Curve
OD curve
• Sigmoid shape (“S” shape)
• Partial pressure of O2 (PO2) = P50 value
• ↑ bound oxygen when ↑ PO2
• Lungs: PO2 is 100 millimeters of mercury = 97%
Hemoglobin saturation with oxygen
• Circulation: PO2 is 40 millimeters of mercury =
75% hemoglobin saturation with oxygen
Copyright ©2019 F.A. Davis Company
Oxygen Dissociation (O D) Curve
(continued)
Copyright ©2019 F.A. Davis Company
O D Curve Changes
Shift to right
• Less attraction to oxygen (release)
• At 40 millimeters of mercury, hemoglobin is 50%
more saturated but willing to give up 50% of
oxygen to tissue if needed
• Lower affinity
‒ Anemia
‒ Acidosis (decreased p H)
‒ Increased 2,3-D P G
‒ Elevated temperature (fever)
Copyright ©2019 F.A. Davis Company
O D Curve Changes (continued)
Shift to left
• More attraction for oxygen
• At 40 millimeters of mercury, hemoglobin is 75%
more saturated but willing to release only 12% to
tissues
• Higher affinity
‒ Presence of abnormal hemoglobins (high affinity)
‒ Alkalosis (increased p H)
‒ ↓ 2,3-D P G, body temp
‒ Multiple transfusions of stored blood where 2,3-D P G
is depleted
Copyright ©2019 F.A. Davis Company
CO2 Transport
secondary function
diffuses into RBC
complex interactions and reactions of
carbonic acid (H2CO3), bicarbonate (HCO3-),
chloride, H+ ions and water
CO2 from tissues transported by
hemoglobin as H+ combines with
bicarbonate to form carbonic acid H2O
and CO2 expelled from lungs
Copyright ©2019 F.A. Davis Company
Abnormal Hemoglobins
Methemoglobin (MetHb)
• Iron in iron3+ state; Not capable of binding oxygen
• If greater than 10%, individuals appear cyanotic
(blue color)
• dyspnea, headache, change in mental status
• Can be induced by aniline drugs or hemoglobin M
(autosomal dominant)
• Avoid offending oxidizing agent
• Treatment: IV Methylene Blue or exchange
transfusions may be required
Copyright ©2019 F.A. Davis Company
Abnormal Hemoglobins
Carboxyhemoglobin (COHb)
• High affinity for carbon monoxide
• Oxygen cannot be delivered to tissues
• Can lead to carbon monoxide poisoning
• Increased in smokers and certain industrial workers
• Headache, dizziness, disorientation
• Blood appears cherry red
• COHb level = greater than 3-10%
• Treatment = oxygen therapy
Copyright ©2019 F.A. Davis Company
Abnormal Hemoglobins (continued)
Sulfhemoglobins
• Affinity for oxygen is lower
• Formed through exposure to sulfonamides or
sulfa-containing drugs
• Persists for life of cell
• Avoid offending agent
Copyright ©2019 F.A. Davis Company
Hemolysis
Cells age Destruction of R B C’s
Interruption of cholesterol and phospholipid
management
Loss of selective permeability
Red cell becomes spheroidal
SA:V decreases
Triggered when ATP generation decreases
Enzymes are destroyed
Copyright ©2019 F.A. Davis Company
Hemolysis
Extravascular 90%
• available energy stores are reduced
• R E S system: spleen, liver, lymph nodes, bone
marrow
• Releases heme and globin contents to be
recycled
• Globin, Heme
• Iron transferrin BM
Copyright ©2019 F.A. Davis Company
Figure 4.4
Copyright ©2019 F.A. Davis Company
Extravascular Hemolysis
↓ Hemoglobin, H C T, R B C count
↑ Reticulocyte count (if bone marrow working)
• Polychromasia in peripheral smear
↑ Serum bilirubin
↓ Haptoglobin
↑LDH
Spherocytes
Urine: ↑ urobilinogen
Copyright ©2019 F.A. Davis Company
Hemolysis
Intravascular
• Lysed directly into blood vessels
• free hemoglobin = haptoglobin
• during complement activation (ABO transfusion
reactions)
Copyright ©2019 F.A. Davis Company
Intravascular Hemolysis
↓ Hemoglobin, H C Hemoglobinuria (red
T, R B C count urine)
↑ Serum bilirubin Possible ↑
↓ Serum reticulocytes
haptoglobin ↑LDH
Hemoglobinemia Schistocytes
(free hemoglobin): Urine: ↑
plasma may appear urobilinogen
red or pink-tinged
Copyright ©2019 F.A. Davis Company
Hemolysis Response
Bone Marrow
• erythroid hyperplasia
• M:E ratio ~1:2
• early release of erythroid precursors
Review Table 4.2
Copyright ©2019 F.A. Davis Company
Classifications Relevant to the Hemolytic
Anemias
Hemolytic Anemias Classified by Intrinsic or Extrinsic Defects (Modified List)
Intrinsic Red Blood Cell Extrinsic Defects Leading to Hemolysis
Defects Leading to Hemolysis
Hemoglobinopathies: structural Autoimmune hemolytic anemia
and synthetic
Red blood cell membrane defects Parasitic infection
Red blood cell enzyme defects Microangiopathic hemolytic anemia
Stem cell defects Environmental agents, including venoms
and chemical agents
Copyright ©2019 F.A. Davis Company
Homework
Read Chapter 4
Test Next Week!
• Cell descriptions and information still relevant
• Safety
Copyright ©2019 F.A. Davis Company
You might also like
- Chapter 14 Pathology RBC and Bleeding Disorders OutlineDocument19 pagesChapter 14 Pathology RBC and Bleeding Disorders OutlineNatan BabekNo ratings yet
- MLT 1027 Learning Outcome 17 MLDY HISTOLOGYDocument136 pagesMLT 1027 Learning Outcome 17 MLDY HISTOLOGYMelanie TranNo ratings yet
- Chapter 14 Red Blood CellsDocument37 pagesChapter 14 Red Blood CellsCatherine LiuNo ratings yet
- Step 2 CK Review - HematologyDocument18 pagesStep 2 CK Review - Hematologyrsmd1986No ratings yet
- Sample Chapter 8.1Document25 pagesSample Chapter 8.1Adel Hassan100% (1)
- Biochemictry: by / Amr Ashraf AwadDocument4 pagesBiochemictry: by / Amr Ashraf AwadHussein MahmoodNo ratings yet
- Hemoglobinopathy - WikipediaDocument1 pageHemoglobinopathy - WikipediaALLAH DITTO KHANNo ratings yet
- HemoglobinDocument56 pagesHemoglobinabdijorgi1No ratings yet
- Hemoglobin & Derivatives: DR. S. Irfan RazaDocument30 pagesHemoglobin & Derivatives: DR. S. Irfan RazaSyed Irfan Raza100% (1)
- Hemoglobin and Myoglobin Structure and FunctionDocument23 pagesHemoglobin and Myoglobin Structure and FunctionHarun MohamedNo ratings yet
- Dr. Niranjan Murthy H.L Assistant Professor Dept of Physiology SSMCDocument22 pagesDr. Niranjan Murthy H.L Assistant Professor Dept of Physiology SSMCnirilibNo ratings yet
- Blood Lectures 2 2017Document41 pagesBlood Lectures 2 2017Philip Abayomi VincentNo ratings yet
- 02 HemoglobinDocument78 pages02 HemoglobinpixiedustNo ratings yet
- Hemoglobin and Its Types: DR Roomi Aijaz Memon Department of Phusiology Isra University HyderabadDocument14 pagesHemoglobin and Its Types: DR Roomi Aijaz Memon Department of Phusiology Isra University HyderabadUSAMA AHMEDNo ratings yet
- 1952uwu270191 H1827272u2bdbdbd017yfndnabab Structure and Fu37373nction Mbbs 2017 BatchDocument88 pages1952uwu270191 H1827272u2bdbdbd017yfndnabab Structure and Fu37373nction Mbbs 2017 BatchRed DiggerNo ratings yet
- Haemopoiesis:: Dr. Anu Elizabeth Joy Asst. Professor Department of Physiology School of Medicine Dire Dawa UniversityDocument48 pagesHaemopoiesis:: Dr. Anu Elizabeth Joy Asst. Professor Department of Physiology School of Medicine Dire Dawa UniversityabdishakurNo ratings yet
- Introduction To HemoglobinopathiesDocument12 pagesIntroduction To HemoglobinopathiesMichael MazvidzaNo ratings yet
- تمريض الاطفال نظري 9Document64 pagesتمريض الاطفال نظري 9jadarcNo ratings yet
- Week 6 - Diagnostic Testing For HemoglobinopathiesDocument53 pagesWeek 6 - Diagnostic Testing For HemoglobinopathiesИван НегарэNo ratings yet
- 2023.LabDx - Trans01.basic Examination of BloodDocument4 pages2023.LabDx - Trans01.basic Examination of BloodstellaNo ratings yet
- Hema Midterm TransDocument19 pagesHema Midterm TransTrisha ManayaNo ratings yet
- Metabolism of HemoglobinDocument46 pagesMetabolism of Hemoglobinlayla hitaNo ratings yet
- Structure and Functions of HemeDocument62 pagesStructure and Functions of HemeBrahmesh GuntamukkalaNo ratings yet
- HGB Metabolism 1Document26 pagesHGB Metabolism 1MARTINEZ JUSTINENo ratings yet
- HemoglobinDocument7 pagesHemoglobinNinik Triayu S100% (2)
- Haemoglobin - Function, Variants, FateDocument27 pagesHaemoglobin - Function, Variants, FateXembergNo ratings yet
- Haemoglobin: Biochemistry and GeneticsDocument34 pagesHaemoglobin: Biochemistry and GeneticsPrincewill SeiyefaNo ratings yet
- 1 - AnemiaDocument25 pages1 - AnemiaDr. Anju K PailyNo ratings yet
- Hemoglobin Opa ThiesDocument34 pagesHemoglobin Opa ThiesFebri fitraNo ratings yet
- HemoglobinDocument33 pagesHemoglobinAkash JaatNo ratings yet
- 4 HGBDocument38 pages4 HGBChona_Delos_Re_1233No ratings yet
- Hema 1 ErythropoiesisDocument20 pagesHema 1 Erythropoiesismarie judimor gomezNo ratings yet
- Haemoglobin: Hiroshani Kulatunga BSC (Hons) MlsDocument36 pagesHaemoglobin: Hiroshani Kulatunga BSC (Hons) MlsNipun ShamikaNo ratings yet
- HaemoglobinDocument55 pagesHaemoglobinPhysiology by Dr RaghuveerNo ratings yet
- Hemoglobinopathy - WikipediaDocument9 pagesHemoglobinopathy - WikipediaEslam NassarNo ratings yet
- Lecture Notes-2-Sickle Cell, ThalassemiaDocument10 pagesLecture Notes-2-Sickle Cell, ThalassemiaManisanthosh KumarNo ratings yet
- 7 HemoglobinopathiesDocument34 pages7 HemoglobinopathiesAhmad SobihNo ratings yet
- Class Review: This Lecture Is Not All-InclusiveDocument127 pagesClass Review: This Lecture Is Not All-InclusiveMelanie TranNo ratings yet
- Hema Lec 1Document3 pagesHema Lec 1ETHELHYN JHANE MACOBNo ratings yet
- Week 3: Hemoglobinopathies: HB Lepore Hbe Hbs HBC HB SC Disease HPFHDocument24 pagesWeek 3: Hemoglobinopathies: HB Lepore Hbe Hbs HBC HB SC Disease HPFHUdyani AgustinaNo ratings yet
- Hemoglobin Function and Variation in Wild PopulationsDocument21 pagesHemoglobin Function and Variation in Wild PopulationsXeyale QuliyevaNo ratings yet
- Bloodsalvage and Blood Product SubstitutesDocument52 pagesBloodsalvage and Blood Product SubstitutesManny GabrielNo ratings yet
- Blood LecturesDocument128 pagesBlood LecturessrhrenaissanceNo ratings yet
- Iron Oxygen Metalloprotein Red Blood Cells Vertebrates InvertebratesDocument28 pagesIron Oxygen Metalloprotein Red Blood Cells Vertebrates InvertebratesJacob MasikaNo ratings yet
- Hemoglobin Formation:: Heme SynthesisDocument2 pagesHemoglobin Formation:: Heme SynthesisJezzah Mae CañeteNo ratings yet
- Alpha Keratin: (A) Both Type I and Type II (B) The RodDocument23 pagesAlpha Keratin: (A) Both Type I and Type II (B) The RodRuth Danielle GasconNo ratings yet
- PDF Test Bank For Rodaks Hematology 5Th Edition by Keohane Online Ebook Full ChapterDocument31 pagesPDF Test Bank For Rodaks Hematology 5Th Edition by Keohane Online Ebook Full Chapterfrancis.holden161100% (4)
- HemoglobinopathiesDocument51 pagesHemoglobinopathiesmontey007No ratings yet
- Structure, Types and Various Methods For Estimation of HaemoglobinDocument49 pagesStructure, Types and Various Methods For Estimation of HaemoglobinChandra ShekharNo ratings yet
- BloodDocument5 pagesBloodAkachukwu ObunikeNo ratings yet
- Haemolytic AnaemiasDocument5 pagesHaemolytic AnaemiasRazib HasanNo ratings yet
- Hemoglobin Metabolism: 1 HeyzgranDocument48 pagesHemoglobin Metabolism: 1 HeyzgranFrancis ValdezNo ratings yet
- Biochemistry of Blood 2Document48 pagesBiochemistry of Blood 2AMEER ALSAABRAWINo ratings yet
- Zoology Full PDF EMDocument108 pagesZoology Full PDF EMSmiruthi RavichandranNo ratings yet
- Red Blood Cells "Best Module Ever"Document4 pagesRed Blood Cells "Best Module Ever"Jose Emmanuel Dolor100% (1)
- Thals and Variants SimpleDocument36 pagesThals and Variants SimpleAli Al-QurweeNo ratings yet
- Structure of HemoglobinDocument8 pagesStructure of HemoglobinAditi RaiNo ratings yet
- Normal Hemoglobin Content: 1-Transport of Respiratory GasesDocument4 pagesNormal Hemoglobin Content: 1-Transport of Respiratory GasesDentistryNo ratings yet
- HB Electrophoresis and HPLC StudyDocument55 pagesHB Electrophoresis and HPLC Studyapi-243480627No ratings yet
- Metabolisme EritrositDocument50 pagesMetabolisme EritrositRamdhana ZaqifahNo ratings yet
- Hemoglobin ElectrophoresisDocument68 pagesHemoglobin Electrophoresisdrafq2000No ratings yet
- RBC Structure and Function (HEMA)Document7 pagesRBC Structure and Function (HEMA)April Lady Faith P. PaundogNo ratings yet
- A Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaFrom EverandA Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaNo ratings yet
- MLT 1027 Learning Outcome 14 Renal UrinaryDocument94 pagesMLT 1027 Learning Outcome 14 Renal UrinaryMelanie TranNo ratings yet
- MLT 1027 Learning Outcome 13 DigestiveDocument226 pagesMLT 1027 Learning Outcome 13 DigestiveMelanie TranNo ratings yet
- 1 - Introduction To HematologyDocument38 pages1 - Introduction To HematologyMelanie Tran100% (1)
- Class Review: This Lecture Is Not All-InclusiveDocument127 pagesClass Review: This Lecture Is Not All-InclusiveMelanie TranNo ratings yet
- Quality Control 1Document59 pagesQuality Control 1Melanie TranNo ratings yet
- RBC DisordersDocument70 pagesRBC DisordersNdor Baribolo100% (1)
- Interpreting Laboratory Results: Key PointsDocument8 pagesInterpreting Laboratory Results: Key PointsMarjorie Joy GreciaNo ratings yet
- Lecture 29-AnemiaDocument35 pagesLecture 29-AnemiaBini JaminNo ratings yet
- Coffeedent June 2021 AfternoonDocument1 pageCoffeedent June 2021 AfternoonHay DayNo ratings yet
- Anemia.: Seminar OnDocument24 pagesAnemia.: Seminar OnAlma Susan100% (1)
- Clinical Features, Diagnosis and Treatment of Heme Pigment-Induced Acute Kidney InjuryDocument7 pagesClinical Features, Diagnosis and Treatment of Heme Pigment-Induced Acute Kidney InjuryemirkurtalicNo ratings yet
- Hemolytic Anemia: NotesDocument9 pagesHemolytic Anemia: NotesRaja SharmaNo ratings yet
- Serological Tests For Cancer DetectionDocument22 pagesSerological Tests For Cancer DetectionShreeyaNo ratings yet
- MacrocytosisDocument6 pagesMacrocytosisAbdul QuyyumNo ratings yet
- MKSAP13-Hematology and OncologyDocument261 pagesMKSAP13-Hematology and OncologyimanNo ratings yet
- Heamatology Dr. Osama PDFDocument94 pagesHeamatology Dr. Osama PDFAnmar ZawahraNo ratings yet
- Vitamin B12 and FolateDocument12 pagesVitamin B12 and FolateAllessandria DimaggioNo ratings yet
- 001assessment Exam ImmunohemaDocument25 pages001assessment Exam ImmunohemaFrankenstein MelancholyNo ratings yet
- Assay Interference A Need For Increased Understanding and TestingDocument9 pagesAssay Interference A Need For Increased Understanding and Testingchali90No ratings yet
- Introduction To HematologyDocument10 pagesIntroduction To HematologyClaire Nicole100% (1)
- Hema311 Lec - Week 5 - Red Cell Structure, Metabolism, Destruction and FunctionDocument6 pagesHema311 Lec - Week 5 - Red Cell Structure, Metabolism, Destruction and FunctionJayvhie Gulane LayanNo ratings yet
- Babesiosis As A Rare Cause of Fever in The Immunocompromised Patient: A Case ReportDocument5 pagesBabesiosis As A Rare Cause of Fever in The Immunocompromised Patient: A Case ReportDaniel Alfredo Galindo ChoqueNo ratings yet
- Clinical Chemistry3Document81 pagesClinical Chemistry3Miguel Alfonso OlfatoNo ratings yet
- Hemolytic AnemiaDocument9 pagesHemolytic AnemiaTheeya QuigaoNo ratings yet
- Chronic Lymphocytic Leukemia: NCCN Guidelines For PatientsDocument82 pagesChronic Lymphocytic Leukemia: NCCN Guidelines For PatientsvnNo ratings yet
- Sickle Cell Anemia: Hba Α Β Hba …….. Α Δ Hb F ……… Α, ΓDocument29 pagesSickle Cell Anemia: Hba Α Β Hba …….. Α Δ Hb F ……… Α, ΓYolanda UriolNo ratings yet
- Hematology PPT 1Document287 pagesHematology PPT 1TarishiMalikNo ratings yet
- LP 10 Anemia 3Document43 pagesLP 10 Anemia 3Anonymous elq7jZiSNo ratings yet
- Plasma ProteinDocument57 pagesPlasma ProteinadulNo ratings yet
- RBC, Structure and FunctionDocument17 pagesRBC, Structure and FunctionAsyha KantifaNo ratings yet
- Biosynthesis of HemoglobinDocument42 pagesBiosynthesis of Hemoglobin95kodok85No ratings yet