Professional Documents
Culture Documents
BS Paratiroid
BS Paratiroid
Uploaded by
No Stradamus0 ratings0% found this document useful (0 votes)
11 views21 pagesThe parathyroid glands are paired endodermal structures located on the thyroid glands. They develop from the third and fourth pharyngeal pouches. The superior parathyroids normally migrate caudally and medially to their final position by the 5th week, while the inferior parathyroids migrate inferiorly along with the developing thymus to reach their normal position by the 7th week. The parathyroid glands consist of chief cells that secrete parathyroid hormone to regulate calcium levels in the blood.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe parathyroid glands are paired endodermal structures located on the thyroid glands. They develop from the third and fourth pharyngeal pouches. The superior parathyroids normally migrate caudally and medially to their final position by the 5th week, while the inferior parathyroids migrate inferiorly along with the developing thymus to reach their normal position by the 7th week. The parathyroid glands consist of chief cells that secrete parathyroid hormone to regulate calcium levels in the blood.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
11 views21 pagesBS Paratiroid
BS Paratiroid
Uploaded by
No StradamusThe parathyroid glands are paired endodermal structures located on the thyroid glands. They develop from the third and fourth pharyngeal pouches. The superior parathyroids normally migrate caudally and medially to their final position by the 5th week, while the inferior parathyroids migrate inferiorly along with the developing thymus to reach their normal position by the 7th week. The parathyroid glands consist of chief cells that secrete parathyroid hormone to regulate calcium levels in the blood.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 21
PARATHYROID GLANDS
Parathyroidsare two paired endocrine
glands located on the thyroid glands
Hence the name
DEVELOPMENT
Endodermal proliferation of 3rd and 4th
pharyngeal pouches
Dorsal aspect of 3rd – inferior
parathyroid
Ventral – thymus
Inferiorparathyroid migrates inferiorly
along with the development of thymus
7th week – normal position
Dorsal aspect of 4th pouch – superior
parathyroid
Ventralaspect and remnant of 5th
pharyngeal poch – ultimobranchial bodies
Sup parathyroid migrates caudally and
medially
5th week – normal position
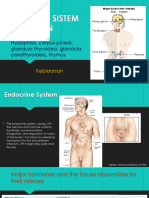
ANATOMY
Two pairs of glands 80 – 97%
>4 – 13%, 3 – 3%
Light yellowish to reddish brown
Oval or lentiform shaped
Bilobed 5%, multilobed 1%
5x3x2 mm
40 – 50 gms
Superior parathyroids – more consistent in
location
Subcapsular
Posterior part of upper half of thyroid lobe
at the cricothyroid juncyion
1cm above the intersection between
inferior thyroid artery and the recurrent
laryngeal nerve
Inferior parathyroids variable in location
inferior, posterior or lateral to the lower
pole 61%
Inferior to lower pole in close relation to
the thyrothymic ligament
26% within cervical part of thymus
2% in the mediastinal portion of thymus
0.2% in the mediastinum
Failureof descent – located above the
superior parathyroid glands surrounded by
remnants of thymic tissue
Superior parathyroids lie posterior and
inferior parathyroid lie anterior to recurrent
laryngeal nerves
ARTERIAL SUPPLY
The inferior parathyroid gland is
supplied by the inferior thyroid artery
approximately 10% of patients, the
inferior thyroid artery is absent, most
commonly on the left side. In these
cases, a branch from the superior
thyroid artery supplies the inferior
parathyroid gland
The superior parathyroid gland is also
usually supplied by the inferior thyroid
artery
By an anastomotic branch between the
inferior thyroid and the superior
thyroid artery
20-45% of cases, the superior parathyroid
glands receive significant vascularity from
the superior thyroid artery
inthe form of a posterior branch of the
superior thyroid artery given off at the level
of the superior pole of the thyroid
Venous drainage occurs into superior
and middle thyroid veins
Nervesupply is by the adrenergic
sympathetic system
Superior and middle cervical sympathetic
ganglia
Perivascular plexus of thyroid gland
Vasomotor but not secretomotor
MICROSCOPY
Thin connective tissue capsule with
intraglandular septa
Chief cells – principle cells,
Light, dark or clear cells
Activechief cells have large golgi
complexes with numerous vesicles
Clearcells are inactive cells with
numerous glycogen granules
Oxyphil cells – eosinophilic cell
Rich in mitochondria
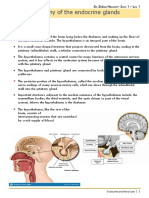
Histology
• Histology---2 cell types
• 1) Principal (Chief) cells secrete
PTH
• ( parathyroid hormone)
• 2) Oxyphil cells –function
unknown, has acidophilic cytoplasm,
many mito. And pyknotic nuclei.
Chief Cells
• Low Ca++ in blood causes PTH secretion from
chief cells
• PTH acts on osteoclasts via osteoblasts to
increase Ca++ in blood from bone
• PTH acts on Kidneys to(a) Ca++ in
blood
• And(b) cause the formation of Vit D (calcitriol)
which intestinal absorption of Ca++
You might also like
- Life Cycle of SecurityDocument40 pagesLife Cycle of SecurityPuneet Sachdeva50% (2)
- HyperthyroidismDocument38 pagesHyperthyroidismKenPedreso100% (2)
- Preventive Maintenance and Inspection ProceduresDocument13 pagesPreventive Maintenance and Inspection ProceduresOsagie AlfredNo ratings yet
- Thyroid and Parathyroid GlandsDocument5 pagesThyroid and Parathyroid GlandsChristopher PhilipsNo ratings yet
- Endocrine Gland....Document62 pagesEndocrine Gland....Sabita TripathiNo ratings yet
- THYROIDDocument100 pagesTHYROIDFrance PalNo ratings yet
- Thyroid Disease: Presentation By: Pimundu Vicent Audo Ritah Tutor: Dr. Fualal JaneDocument41 pagesThyroid Disease: Presentation By: Pimundu Vicent Audo Ritah Tutor: Dr. Fualal JaneEsther AumaNo ratings yet
- It Means Shield It Is Most Vascular GlandDocument9 pagesIt Means Shield It Is Most Vascular GlandDr santoshNo ratings yet
- Endo All MergeDocument586 pagesEndo All MergeShivani DurgeNo ratings yet
- Endicronology Anatomy 3Document4 pagesEndicronology Anatomy 3shahab shamsiNo ratings yet
- Parathyroid Glands: DR Priyanka ShastriDocument70 pagesParathyroid Glands: DR Priyanka ShastriNo StradamusNo ratings yet
- C10 Endocrine SystemDocument24 pagesC10 Endocrine Systemwajomi100% (1)
- Anatomy, Physiology and Pathology of The Thyroid Gland: DR Suchitra Iyrpg Department of Prosthodontics SRMCDocument46 pagesAnatomy, Physiology and Pathology of The Thyroid Gland: DR Suchitra Iyrpg Department of Prosthodontics SRMCdrsuchitramohanNo ratings yet
- Anatomi Sistem Endokrin KebidananDocument35 pagesAnatomi Sistem Endokrin Kebidananatmalinda2016No ratings yet
- Endocrine GlandsDocument24 pagesEndocrine GlandsZoyaNo ratings yet
- Neck Diseases: Affiliated Hospital Of Jining Medical Colledge Dep.Mammary And Thyroid Surgery Zhu Kunbing 朱坤兵Document61 pagesNeck Diseases: Affiliated Hospital Of Jining Medical Colledge Dep.Mammary And Thyroid Surgery Zhu Kunbing 朱坤兵sanjivdasNo ratings yet
- ERD BlockDocument399 pagesERD BlockAhmed IbrahimNo ratings yet
- Anatomi Endokrin Mei 2019Document64 pagesAnatomi Endokrin Mei 2019insiya insiyaNo ratings yet
- Anatomy of ParathyroidDocument2 pagesAnatomy of ParathyroidNnanyelugo AdaobiNo ratings yet
- Pituitary GlandDocument66 pagesPituitary GlandAsmita BhattNo ratings yet
- Thyroid PreDocument370 pagesThyroid PreQuennie Gumapac-PabloNo ratings yet
- Lapsus InvaginasiDocument41 pagesLapsus InvaginasiHanda YaniNo ratings yet
- ANA Trans - Endo ReproDocument14 pagesANA Trans - Endo ReproSan LapuhapuNo ratings yet
- Thyroid & Parathyroid GlandsDocument21 pagesThyroid & Parathyroid GlandsAzizan HannyNo ratings yet
- Lecture-11 The Endocrine SystemDocument36 pagesLecture-11 The Endocrine SystemzahraaNo ratings yet
- Thyroid GlandDocument19 pagesThyroid Glandplay listNo ratings yet
- Histology of The Endocrine System: Ma. Minda Luz M. Manuguid, M.DDocument27 pagesHistology of The Endocrine System: Ma. Minda Luz M. Manuguid, M.Dchocoholic potchiNo ratings yet
- Anatomy Endocrine System PPT 2023Document70 pagesAnatomy Endocrine System PPT 2023bereket bekeleNo ratings yet
- W4-15 Endocrine and Alimentary Layers of The Neck Lecture PDFDocument75 pagesW4-15 Endocrine and Alimentary Layers of The Neck Lecture PDFSAHIL AGARWALNo ratings yet
- ParathyroidDocument6 pagesParathyroidoluwasujimNo ratings yet
- Thyroid Pre PDFDocument370 pagesThyroid Pre PDFLidijaNo ratings yet
- 3) Thyroid Gland MDSC 2101 2014Document32 pages3) Thyroid Gland MDSC 2101 2014Kay Bristol100% (1)
- Endocrinology 2Document13 pagesEndocrinology 2Dr.Mahesh kumar GuptaNo ratings yet
- Thyroid Malignancies: Anatomy Rukman MeccaDocument26 pagesThyroid Malignancies: Anatomy Rukman MeccaRukman MeccaNo ratings yet
- Anatomy, Embryology and Histology of Thyroid Gland: Intern DR - Bibhuti Lacoul Shree Birendra HospitalDocument26 pagesAnatomy, Embryology and Histology of Thyroid Gland: Intern DR - Bibhuti Lacoul Shree Birendra HospitalprostaglandinNo ratings yet
- Endocrine System: Dr. Fitriani Lumongga Dr. Lita FeriyawatiDocument36 pagesEndocrine System: Dr. Fitriani Lumongga Dr. Lita FeriyawatiWilan Dita NesyiaNo ratings yet
- Lecture Endokrin 2014Document22 pagesLecture Endokrin 2014via73No ratings yet
- Anatomy of The Thyroid GlandDocument21 pagesAnatomy of The Thyroid GlandIsaac OnigbindeNo ratings yet
- Endocrine System - de Jesus MDDocument3 pagesEndocrine System - de Jesus MDKerenTabuenaNo ratings yet
- Department of ZoologyDocument27 pagesDepartment of ZoologyAleenaNo ratings yet
- Anatomy of The Endocrine Glands: HypothalamusDocument10 pagesAnatomy of The Endocrine Glands: Hypothalamusgashbin latifNo ratings yet
- Thyroid Gland BasicsDocument25 pagesThyroid Gland BasicsSreekar DevarakondaNo ratings yet
- 2-Thyroid & Parathyroid GlandsDocument41 pages2-Thyroid & Parathyroid Glandsali msheikNo ratings yet
- Hormones of The Anterior PituitaryDocument21 pagesHormones of The Anterior PituitaryRed MistNo ratings yet
- ThyroidectomyDocument45 pagesThyroidectomyNur Lisa HamzahNo ratings yet
- Thyroid DiseasesDocument76 pagesThyroid DiseasesSolomon Fallah Foa SandyNo ratings yet
- Pankreas & LienDocument38 pagesPankreas & LienopimadridistaNo ratings yet
- ENDOCRINE and FEMALE Genital SystemsDocument9 pagesENDOCRINE and FEMALE Genital SystemsIshraq AfifiNo ratings yet
- THYROID LECTURE DR OCAMPO (1) (Autosaved)Document106 pagesTHYROID LECTURE DR OCAMPO (1) (Autosaved)SamNo ratings yet
- Thyroid GlandDocument48 pagesThyroid GlandAleksNo ratings yet
- Embryology of The Neck & Neck MassesDocument52 pagesEmbryology of The Neck & Neck MassesArfian Deny PNo ratings yet
- Endocrinesystem NotesDocument53 pagesEndocrinesystem NotesMisab MKNo ratings yet
- Surgical Anatomy of The Parathyroid Glands - Uptodate 2022Document8 pagesSurgical Anatomy of The Parathyroid Glands - Uptodate 2022juanrangoneNo ratings yet
- Histology and Gross Pancreas 2019Document59 pagesHistology and Gross Pancreas 2019Azwaah Hassan100% (1)
- Parotid Gland: Rajkumar EuniceDocument20 pagesParotid Gland: Rajkumar EuniceEcah BrendanNo ratings yet
- Thyroid GlandDocument81 pagesThyroid Glanddr_shamimrNo ratings yet
- Da Souza Endocrine-GlandsDocument16 pagesDa Souza Endocrine-Glandsgaza slimNo ratings yet
- Presented By: Mohammad Arif Mohini Singh Mudit Aggarwal Muskan JaiswalDocument25 pagesPresented By: Mohammad Arif Mohini Singh Mudit Aggarwal Muskan Jaiswalar921712No ratings yet
- Anatomy and Physiology of ThyroidDocument74 pagesAnatomy and Physiology of ThyroidSajid NadafNo ratings yet
- Development of Thyroid GlandDocument37 pagesDevelopment of Thyroid GlandnrahmaNo ratings yet
- Anatomia Sistemului EndocrinDocument15 pagesAnatomia Sistemului EndocrinRaul MuresanNo ratings yet
- Pneumonia 190706120001Document26 pagesPneumonia 190706120001No StradamusNo ratings yet
- Steroids: Abuse & Misuse ofDocument12 pagesSteroids: Abuse & Misuse ofNo StradamusNo ratings yet
- Steroids: Madiha AhmedDocument12 pagesSteroids: Madiha AhmedNo StradamusNo ratings yet
- Steroids: By: Sean KilcoyneDocument10 pagesSteroids: By: Sean KilcoyneNo StradamusNo ratings yet
- Parathyroid Gland: Dr. R. KalliecharanDocument6 pagesParathyroid Gland: Dr. R. KalliecharanNo StradamusNo ratings yet
- Parathyroid Glands: DR Priyanka ShastriDocument70 pagesParathyroid Glands: DR Priyanka ShastriNo StradamusNo ratings yet
- The Histology of Female Genital System: I Wayan SugiritamaDocument36 pagesThe Histology of Female Genital System: I Wayan SugiritamaNo StradamusNo ratings yet
- Dr. W A P S R Weerarathna Registrar in Medicine-WD 10/02Document45 pagesDr. W A P S R Weerarathna Registrar in Medicine-WD 10/02No StradamusNo ratings yet
- 09 at 015 1Document4 pages09 at 015 1David ParariNo ratings yet
- Pre-Membership Requirements: Quezon Public School Teachers and Employees Multipurpose CooperativeDocument2 pagesPre-Membership Requirements: Quezon Public School Teachers and Employees Multipurpose CooperativeRoselyn San Diego PacaigueNo ratings yet
- Selected Student List For Reporting (A Unit) Reporting Date: 15/01/2023 and 16/01/2023 Published Date: 14/01/2023Document19 pagesSelected Student List For Reporting (A Unit) Reporting Date: 15/01/2023 and 16/01/2023 Published Date: 14/01/2023いずちあさみNo ratings yet
- Gess302 PDFDocument12 pagesGess302 PDFKrishNo ratings yet
- Burmese DanceDocument2 pagesBurmese DanceKo Ye50% (2)
- SS 11Document31 pagesSS 11Christopher MendozaNo ratings yet
- Module 6 - Letter To The Young Women of MalolosDocument7 pagesModule 6 - Letter To The Young Women of MalolosJr CialanaNo ratings yet
- Half Nelson - Mandela de Beers DiamondDocument3 pagesHalf Nelson - Mandela de Beers Diamonddouglas rodriguesNo ratings yet
- 03 Debt Markets SOLUTIONSDocument22 pages03 Debt Markets SOLUTIONSSusanNo ratings yet
- Brown Act Petition - San Diego BOS 1/20/2012Document63 pagesBrown Act Petition - San Diego BOS 1/20/2012Terry FranckeNo ratings yet
- Duc Quan Nguyen Résumé: ProfileDocument3 pagesDuc Quan Nguyen Résumé: Profileapi-670240415No ratings yet
- Questions of MTP and RTPDocument144 pagesQuestions of MTP and RTPGaurang ChhanganiNo ratings yet
- Merlin 6000 ManualDocument112 pagesMerlin 6000 Manualbillb60No ratings yet
- Shantanu Agnihotri - HistoryDocument31 pagesShantanu Agnihotri - HistoryShantanu AgnihotriNo ratings yet
- SAI Global - Food Fraud The Basic, 2019 (7p)Document7 pagesSAI Global - Food Fraud The Basic, 2019 (7p)Mark KwanNo ratings yet
- Acdasoa On The Spot Logo Making Contest GuidelinesDocument2 pagesAcdasoa On The Spot Logo Making Contest GuidelinesAlma Reynaldo TucayNo ratings yet
- Transport Corporation of India LimitedDocument3 pagesTransport Corporation of India LimitedAshutosh BaishNo ratings yet
- Ctp2017!03!391 - Kor Kadet Polis-Ebss - Yn4wnDocument2 pagesCtp2017!03!391 - Kor Kadet Polis-Ebss - Yn4wnsimah imaNo ratings yet
- Emergency Motion Darrell VolentineDocument12 pagesEmergency Motion Darrell VolentinesmallcapsmarketNo ratings yet
- List of Case Studies On Strategy (Catalogue IV)Document53 pagesList of Case Studies On Strategy (Catalogue IV)Sushil Agrawal0% (1)
- Rpt-Sow Form 3 2024Document6 pagesRpt-Sow Form 3 2024g-16025707No ratings yet
- August 2021 Update - Offerpad Investor Presentation - VFFFDocument44 pagesAugust 2021 Update - Offerpad Investor Presentation - VFFFtempvjNo ratings yet
- Sweden ArchitechtureDocument7 pagesSweden ArchitechturekonstacNo ratings yet
- Plea Bargaining Framework in Drugs CasesDocument6 pagesPlea Bargaining Framework in Drugs CasesMack Hale BunaganNo ratings yet
- Review Trip Details and BookDocument1 pageReview Trip Details and BookHamza HamdanNo ratings yet
- A Fresh Perspective of Paul's Missionary Strategies-The Mentoring For Multiplication ModelDocument18 pagesA Fresh Perspective of Paul's Missionary Strategies-The Mentoring For Multiplication ModelWilliam YeongNo ratings yet
- Diplomatic Protection of Natural Persons (Final)Document12 pagesDiplomatic Protection of Natural Persons (Final)Bárbara Ribeiro EstevesNo ratings yet
- 4PS FinalDocument44 pages4PS Finalcorazon lopez100% (2)