Professional Documents
Culture Documents
Central Nervous System 10
Central Nervous System 10
Uploaded by
Kori Yerivan McDaniel0 ratings0% found this document useful (0 votes)
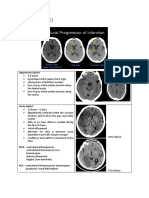
235 views165 pagesCentral nervous system cellular injury and pathology can affect neurons, astrocytes, oligodendrocytes, ependymal cells, choroid plexus, microglia and blood vessels. Neurons are vulnerable to acute injury, neurodegenerative diseases, viral infections and aging. Astrocytes repair injury through gliosis. Oligodendrocytes produce myelin. Ependymal cells line ventricles and astrocyte proliferation can be triggered by disruption. Microglia are phagocytes that aggregate at injury sites. Cerebral edema, hydrocephalus, herniation, cerebrovascular diseases, intracranial hemorrhage and vascular malformations can all impact the central nervous system.
Original Description:
Original Title
Central_Nervous_System_10
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCentral nervous system cellular injury and pathology can affect neurons, astrocytes, oligodendrocytes, ependymal cells, choroid plexus, microglia and blood vessels. Neurons are vulnerable to acute injury, neurodegenerative diseases, viral infections and aging. Astrocytes repair injury through gliosis. Oligodendrocytes produce myelin. Ependymal cells line ventricles and astrocyte proliferation can be triggered by disruption. Microglia are phagocytes that aggregate at injury sites. Cerebral edema, hydrocephalus, herniation, cerebrovascular diseases, intracranial hemorrhage and vascular malformations can all impact the central nervous system.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
235 views165 pagesCentral Nervous System 10
Central Nervous System 10
Uploaded by
Kori Yerivan McDanielCentral nervous system cellular injury and pathology can affect neurons, astrocytes, oligodendrocytes, ependymal cells, choroid plexus, microglia and blood vessels. Neurons are vulnerable to acute injury, neurodegenerative diseases, viral infections and aging. Astrocytes repair injury through gliosis. Oligodendrocytes produce myelin. Ependymal cells line ventricles and astrocyte proliferation can be triggered by disruption. Microglia are phagocytes that aggregate at injury sites. Cerebral edema, hydrocephalus, herniation, cerebrovascular diseases, intracranial hemorrhage and vascular malformations can all impact the central nervous system.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 165
Central Nervous System
Patterns of Cellular Injury
• Neurons
– Acute neuronal injury
• “Red neurons”, eosinophilic cytoplasm
• Spheroids, disruption of axonal transport
• Central chromatolysis, axonal injury
– Neurodegenerative diseases
• Intracellular inclusions
• Dystrophic neurites
– Viral infections—inclusions
– Aging--lipofuscin
Patterns of Cellular Injury
• Astrocytes
– Repair and scar formation (gliosis)
• Hypertrophy and hyperplasia
• Gemistocytic astrocyte, bright pink cytoplasm
• Minimal extracellular matrix deposition
• Limited fibroblast involvement
• Long standing gliosis
– Fibrillary astrocytes and Rosenthal fibers
– Degenerative change
• Corpora amylacea in astrocytic processes
Patterns of Cellular Injury
• Oligodendrocytes
– Produce myelin
– Multiple neurons per cell
• Ependymal cells
– Line ventricles
– Disruption triggers subependymal astrocyte
proliferation (ependymal granulations)
• Choroid plexus
– Secretes CSF
Patterns of Cellular Injury
• Microglia
– Phagocytes
• Bone marrow derived
– Activated by tissue injury
– Microglial nodules
• Aggregates at site of tissue injury
• Congregate around portions of dying neurons
– Neuronophagia
Cerebral Edema
• Accumulation of excess fluid within the brain
parenchyma
– Vasogenic edema
• Integrity of blood-brain barrier is disrupted
• Fluid shifts from vascular compartment to intercellular
spaces
• Inflammation or tumors
– Cytotoxic edema
• Membrane injury
• Increased intracellular fluid
• Hypoxic/ischemic insult or toxins
– Often occur together
Hydrocephalus
• Accumulation of excessive CSF within the
ventricular system
– Impaired flow
– Impaired resorption
– Excess production (rarely)
• Before suture closure
– Enlargement of head
• After suture closure
– Expansion of ventricles
– Increased intracranial pressure
Hydrocephalus
• Noncommunicating hydrocephalus
– Obstruction within ventricular system
– Enlargement of ventricles proximal to block
• Communicating hydrocephalus
– Reduced resorption
– All ventricles enlarged
• Hydrocephalus ex vacuo
– Secondary to loss of brain parenchyma
Herniation
• Focal expansion of brain causes it to be
displaced in relation to dural folds or bony
structures
– Occurs when volume of brain exceeds limits
permitted by compression of veins and
displacement of CSF
– Intracranial pressure rises
– Usual result is compromise of blood supply to
“pushed” tissue
Herniation
• Subfalcine (cingulate) herniation
– Unilateral or asymmetric expansion of a
cerebral hemisphere
– Cingulate gyrus displaced under edge of falx
cerebri
– Associated with compression of anterior
cerebral artery branches
Herniation
• Transtentorial (uncinate) herniation
– Medial aspect of temporal lobe compressed against
free edge of tentorium cerebelli
– Oculomotor nerve is compromised on side of lesion
(CN III palsy and “blown” pupil)
– Posterior cerebral artery may be compressed
• Primary visual cortex
– May compress contralateral cerebral peduncle
(hemiparesis ipsilateral to herniation)
– Duret hemorrhages in midbrain and pons
• Midline or paramedian hemorrhages from tearing of
penetrating veins and arteries
Herniation
• Tonsilar herniation
– Displacement of cerebellar tonsils through the
foramen magnum
– Brainstem compression
– Compromises respiratory and cardiac centers
in medulla
Cerebrovascular Diseases
• Any abnormality of the brain caused by a
pathologic process involving blood vessels
– Thrombotic occlusion of vessels
– Embolic occlusion of vessels
– Vascular rupture
• Occlusion of vessels
– Loss of oxygen and metabolic substrates resulting in
infarction
• Hemorrhage
– Direct tissue damage and secondary ischemia
Cerebrovascular Diseases
• Brain requires a continuous supply of glucose
and oxygen
• Oxygen is the limiting substance
– Functional hypoxia
• Low partial pressure of oxygen
• Impaired oxygen carrying capacity
• Inhibition of oxygen use by tissues
– Ischemia, transient or permanent
• Interruption of normal circulatory flow
– Reduced perfusion pressure
– Vascular obstruction
Global Cerebral Ischemia
• Widespread ischemic/hypoxic injury resulting from a
generalized reduction in cerebral perfusion
• Outcome varies with severity of insult
• Neurons are much more sensitive to hypoxia than glial
cells
• Most sensitive
– Pyramidal cells of CA1 of hippocampus
– Purkinje cells of the cerebellum
– Pyramidal cells of neocortex
• Border zone (“watershed”) infarcts
– Wedge shaped infarcts at edge of arterial perfusion fields
– ACA-MCA border
Global Cerebral Ischemia
• Morphology
– Brain swollen, poor demarcation between
gray and white matter
– Microscopic of irreversible ischemic injury
(infarction)
• Early (12-24 hours): red neurons, infiltration of
neutrophils
• Subacute (24 hr-2wks): necrosis, macrophages,
vascular proliferation, reactive gliosis
• Repair (>2wks): removal of necrotic tissue,
disorganization, gliosis
Focal Cerebral Ischemia
• Arterial occlusion leading to focal ischemia
or infarction
– Embolization
• More common
• Sources: cardiac mural thrombi, atheromatous
plaques, paradoxical emboli, cardiac surgery, other
material (tumor, fat, air)
• Middle cerebral artery most frequently involved
– Branch points, preexisting luminal stenoses
Focal Cerebral Ischemia
– In situ thrombosis
• Atherosclerosis
– Carotid bifurcation, origin of MCA, basilar artery
• Infarcts are divided into two large groups
– Nonhemorrhagic
– Hemorrhagic
• Hemorrhage is due to reperfusion of ischemic
tissue
Focal Cerebral Ischemia
• Morphology
– Macroscopic
• 0-6 hrs: nothing
• 6-48 hrs: pale, soft swollen, indistinct gray-white
matter junction
• 2-10 days: gelatinous, friable, affected area is
defined as edema resolves
• 10 days-3 wks: tissue liquefies leaving cavity
– Microscopic (see previous)
Intracranial Hemorrhage
• Hemorrhage can occur at a variety of sites
• Each site has associated causes
Primary Brain Parenchymal
Hemorrhage
• Peak incidence at age 60
• Rupture of small intraparenchymal vessel
• Hypertension is most common underlying
cause (15% of deaths with chronic HTN)
• Basal ganglia, thalamus, pons, cerebellum
• Location and size determine clinical
manifestations
Cerebral Amyloid Angiopathy
• Amyloidogenic peptides deposit in the
walls of small and medium caliber
meningeal and cortical vessels
• Weakens vessel walls
• Spares vasculature of white and deep gray
matter
• Often referred to as lobar hemorrhages
due to involvement of cerebral cortex
Saccular Aneurysms
• Most frequent cause of clinically significant
subarachnoid hemorrhage is rupture of a
saccular aneurysm
• 90% occur in the anterior circulation
• Multiple aneurysms occur in 20-30% of cases
• Associated with disorders of extracellular matrix
proteins
• Increased risk in individuals with autosomal
dominant polycystic kidney disease
Saccular Aneurysms
• Overall, 1.3% per year rate of bleeding
– Risk increases with size
– 10mm has 50% per year rate of bleeding
• Subarachnoid hemorrhage has additional acute
risk of ischemia due to vasospasm of other
vessels
• Healing phase involves risk of obstruction of
CSF flow and resorption
• 25-50% of individuals die with first rupture
• Sudden, excruciating headache
Saccular Aneurysms
• Morphology
– Thin walled out-pouching of an artery
– Muscular wall and internal elastic lamina are
absent from the sac
– Sac is thickened hyalinized intima
Vascular Malformations
• Arteriovenous malformations (AVM)
– Enlarged blood vessels separated by gliotic tissue
– M:F is 2:1
– Presents most often between 10 and 30 yrs of age
• Seizure disorder, intracerebral hemorrhage, subarachnoid
hemorrhage
– Large AVM can cause high output heart failure in
infants
– Most dangerous vascular malformation
– Can be in subarachnoid space, extend into brain, or
entirely within brain
Vascular Malformations
• Cavernous hemangiomas
– Distended loosely organized vascular channels
without intervening nervous tissue
– Occur in cerebellum, pons, subcortical regions
– Low flow, no AV shunting
• Capillary telangiectasias
– Thin walled vascular channels separated by normal
brain parenchyma
– Pons
• Venous angiomas
– Ectatic venous channels
Hypertensive Cerebrovascular
Disease
• Effects of hypertension on the brain
– Massive hypertensive intracerebral
hemorrhage
– Lacunar infarcts
– Slit hemorrhages
– Hypertensive encephalopathy
Hypertensive Cerebrovascular
Disease
• Arterio- and Arteriolo- sclerosis
– Deep penetrating vessels of basal ganglia,
white matter, and brain stem
– Hyaline change makes vessel walls weaker
– Charcot-Bouchard microaneurysms
• Less than 300 microns in diameter
• May rupture and bleed
Hypertensive Cerebrovascular
Disease
• Lacunar infarcts
– Small cavitary infarcts just a few millimeters
wide
– Deep gray matter, internal capsule, deep
white matter, pons
– Can be silent or cause significant neurological
impairment
• Slit hemorrhage
– Small hemorrhage that heals leaving a slit-like
cavity
Hypertensive Cerebrovascular
Disease
• Acute hypertensive encephalopathy
– Acute cerebral dysfunction
– Increased intracranial pressure
– Petechiae and fibrinoid necrosis of arterioles
in gray and white matter
Vasculitis
• Infectious arteritis
• Systemic vasculitis
• Primary angiitis of the CNS
– Involves multiple small to medium
parenchymal and subarachnoid vessels
– Diffuse encephalopathic picture
– Steroids and immunosuppressive treatment
Trauma
• Significant cause of death and disability
• Severity and site of injury affect outcome
• Variables: shape of object, force of
impact, head in motion
• Penetrating or blunt, open or closed
• External appearance doesn’t necessarily
correlate with extent of brain injury
• Parenchymal and/or vascular injury
Traumatic Parenchymal Injury
• Contusions
– Brain impacts the skull
• Coup and contrecoup
• Rapid tissue displacement and vascular rupture
– Hemorrhage, tissue injury, edema
– Crests of gyri
• Orbital gyri of frontal lobe, temporal lobe (esp. tips)
• Laceration
– Penetration of brain
• Tissue tearing, vascular disruption, hemorrhage
• Linear path
Traumatic Parenchymal Injury
• Diffuse axonal injury
– Widespread damage to axons within the brain
• Angles of lateral ventricles or brainstem most
commonly affected
– Movement of one region relative to another
• Angular acceleration alone can cause this without
impact
• Axonal disruption (integrity or function) and
hemorrhage
– 50% of patients who develop coma shortly
after trauma
Traumatic Parenchymal Injury
• Concussion
– Reversible altered consciousness from head
injury in the absence of contusion
– Transient neurological dysfunction
• Loss of consciousness
• Temporary respiratory arrest
• Loss of reflexes
– Complete neurological recovery
• Amnesia for the event
– Pathogenesis unknown
Traumatic Vascular Injury
• Direct trauma and disruption of the vessel
wall
• May occur in one or more compartments
– Epidural
– Subdural
– Subarachnoid
– Intraparenchymal
Traumatic Vascular Injury
• Epidural hematoma
– Torn vessel in the dura
• Middle meningeal artery
– Often with skull fracture
– Blood under arterial pressure separates dura from the
inner surface of the skull
• Smooth inner contour that compresses brain
– Patients can be lucid for several hours between
trauma and development of neurological signs
• Neurosurgical emergency
Traumatic Vascular Injury
• Subdural hematoma
– Tearing of bridging veins caused by rapid movement
of the brain
• Bleed into the subdural space
• Most common over lateral aspect of cerebral hemispheres
• 10% bilateral
– Increased risk
• Brain atrophy—stretched veins
• Infants—thin walled veins
– Become manifest within 48 hours of injury
• Signs attributable to pressure on the brain
• Headache, confusion, sometimes localizing
• Progressive neurological deterioration, rarely with acute
decompensation
Traumatic Vascular Injury
• Subdural hematoma
– Bleeding is usually self-limited
– If not evacuated, hematoma will organize over time
• Fibroblasts grow in from dura
• Granulation tissue matures and forms “subdural membranes”
– Subdural hematomas frequently rebleed becoming
chronic subdural hematomas
– Symptomatic subdural hematomas are treated by
removing the organizing blood and tissue
Malformations
• Neural tube defects
– Failure of a portion of the neural tube to close or
reopening after successful closure
– Involve some combination of neural tissue, meninges,
and overlying bone or soft tissues
– Most frequent CNS malformations
– Folate deficiency during initial weeks of gestation is
risk factor
– Early detection by ultrasound and α-fetoprotein
– 4-5% recurrence risk in subsequent pregnancies
Neural Tube Defects
• Spinal cord involvement most common
– Spina bifida occulta
• Asymptomatic bony defect
– Myelomeningocele
• Extension of CNS tissue through a defect in the
vertebral column
– Problems with motor and sensory in lower limbs,
bowel/bladder control
– Infection risk from thin or ulcerated overlying skin
Neural Tube Defects
• Brain end of neural tube
– Anencephaly
• Absence of brain and top of skull
– Encephalocele
• Diverticulum of malformed CNS tissue extending
through a defect in the cranium
– Posterior more common than anterior
Forebrain Malformations
• Microencephaly
– Abnormally small brain
– Associated with chromosome abnormalities, fetal
alcohol syndrome, in utero HIV infection
• Lissencephaly (agyria)
– Absence of normal gyration and smooth surfaced
brain
– Disruption of normal neuronal migration and
differentiation
• Abnormally thickened cortex and only four layered
– Pachygyria is a less widespread form
Forebrain Malformations
• Polymicrogyria
– Increased number of irregularly formed gyri
– Altered cortical architecture
• Holoprosencephaly
– Disruption of normal midline patterning
• Mild forms may just have absence of olfactory bulbs and
related structures
• In severe forms the brain may not be divided into lobes or
hemispheres
– Midline facial defects
• Mutations in sonic hedgehog linked to some cases
Posterior Fossa Anomalies
• Most commonly result in misplaced or absent
cerebellum and hydrocephalus
• Arnold-Chiari malformation
– Chiari type II malformation
• Small posterior fossa, misshapen midline cerebellum with
downward extension of vermis through foramen magnum
• Hydrocephalus and lumbar myelomeningocele are typically
also present
– Chiari I malformation
• Low-lying cerebellar tonsils extend through the foramen
magnum
• Obstruction of CSF flow and compression of medulla
• Headache and cranial nerve deficits
Posterior Fossa Anomalies
• Dandy-Walker malformation
– Enlarged posterior fossa
– Cerebellar vermis is absent (or rudimentary
anterior portion)
– Large midline cyst
• Lined with ependyma and is contiguous with
leptomeninges on its outer surface
– Dysplasia of brainstem nuclei are commonly
found
Spinal Cord Abnormalities
• Hydromyelia
– Expansion of the central canal
• Syringomyelia (syrinx)
– Fluid filled cleft-like cavity in the inner portion of the
spinal cord
– May also be acquired
• Associated with destruction of adjacent gray and
white matter, surrounded by reactive gliosis
• Cervical cord most often affected
Perinatal Brain Injury
• Cerebral palsy
– Nonprogressive neurological motor disorder
characterized by spasticity, dystonia,
ataxia/athetosis, and paresis attributable to
injury occurring during the prenatal and
perinatal periods
Perinatal Brain Injury
• Intraparenchymal hemorrhage
– Within germinal matrix of premature infants
– May extend to ventricles and subarachnoid space
– Sometimes leading to hydrocephalus
• Periventricular leukomalacia
– Infarcts in the supratentorial periventricular white
matter, esp. in premature infants
– Leaves chalky yellow plaques in white matter with
calcifications
– If involves gray matter too, large cystic lesions can
develop throughout the hemispheres (multicystic
encephalopathy)
Infections
• Nervous tissue damaged by
– Direct injury of neurons or glia
– Microbial toxins
– Effects of inflammatory response
– Immune-mediated mechanisms
• Routes of entry
– Hematogenous (most common)
• Arterial or venous less commonly
– Direct implantation
• Post-traumatic
– Local extension from skull, spine, or malformation
– Peripheral nerves
Epidural and Subdural Infections
• Bacterial or fungal
• Usually by direct local spread
• Epidural abscess
– Commonly associated with osteomyelitis
– Spinal epidural abscess can cause cord compression
• Subdural empyema
– May produce a mass effect
– Thrombophlebitis of bridging veins→infarction of brain
Meningitis
• Inflammatory process of leptomeninges
and CSF in the subarachnoid space
– Meningoencephalitis is spread of infection
from the meninges to the underlying brain
– Usually an infection, can be chemical
– Infectious meningitis
• Acute pyogenic
• Aseptic
• Chronic
Acute Pyogenic Meningitis
• Wide range of bacteria
• Most likely depends on age
– Neonates: E. coli, group B streptococci
– Elderly: S. pneumoniae, Listeria monocytogenes
– Adolescents/young adults: Neisseria meningitides
• Systemic signs of infection superimposed on
meningeal irritation and neurological impairment
• CSF: neutrophils, ↑ protein, ↓glucose, bacteria
• Exudate in leptomeninges over surface of brain
Acute Pyogenic Meningitis
• When fulminant, inflammatory cells may
infiltrate leptomeningeal veins, spread to
the brain, or extend to the ventricles
• Phlebitis may lead to thrombosis and
hemorrhagic infarction of the brain
• Untreated, it may be fatal
• Effective antimicrobial treatment greatly
reduces mortality
Aseptic Meningitis
• Aseptic is a misnomer
– Clinical term for an illness comprising meningeal
irritation, fever, and alterations of consciousness of
relatively acute onset without recognizable organisms
• Less fulminant, usually self-limiting, and usually
treated symptomatically
• CSF: lymphocytosis, moderately elevated
protein, normal glucose
• Pathogen can be identified in about 70% of
cases, usually an enterovirus
Chronic Meningitis
• Tuberculous meningitis
– CSF: pleiocytosis (↑ leukocytes) of mononuclear cells
or neutrophils and mononuclear cells, ↑ protein, ↓
glucose
– May have an intraparenchymal mass (tuberculoma)
– Usually affects basal meninges
• Meninges contain infiltrate of lymphocytes, plasma cells, and
macrophages
• Possibly even well-formed granulomas
– Cause of arachnoid fibrosis that may lead to
hydrocephalus
Chronic Meningitis
• Neurosyphilis
– Tertiary stage of syphilis, occurs in about 10% of
untreated infections
– Meningovascular neurosyphilis is a major
manifestation
• Chronic meningitis usually involving the base of the brain
• Cerebral gummas may occur in relation to the meninges and
extend into the brain
– Paretic neurosyphilis is the parenchymal disease
• Insidious progressive loss of mental and physical functions
with mood alterations, terminating in dementia
Chronic Meningitis
– Tabes dorsalis
• Damage to sensory nerves in dorsal roots
– Impaired proprioception
» Locomotor ataxia
– Impaired pain sensation
» Joint damage, skin damage
– Lightning pains
– Absence of deep tendon reflexes
– HIV infection increases risk of neurosyphilis
• Increased rate of progression and severity of
disease
Parenchymal Infections
• Any type of microbial organism can potentially
infect the brain
• Different types of organisms generally have
different patterns of involvement
– Viruses are most diffuse
– Bacteria (when not meningitis) are most localized
– Other are more mixed
– Immunosuppression leads to more widespread
involvement of any particular agent
Brain Abscess
• Nearly always caused by bacteria
• Destructive lesions
– Progressive focal signs
– Signs of increased intracranial pressure
– CSF: ↑ WBC and protein, glucose normal
• Complications
– ICP, herniation can be fatal
– Rupture, ventriculitis, meningitis, venous
sinus thrombosis
Viral Encephalitis
• Parenchymal infection of brain that also always
is associated with meningeal inflammation
(meningoencephalitis)
• Most show perivascular and parenchymal
mononuclear infiltrates, microglial nodules, and
neuronophagia
• Various viruses may have
– Inclusion bodies
– Specific cell types or particular areas involved
– Immune-mediated injury
– Congenital malformation
Arboviruses
• Arthropod-borne viruses (mostly
mosquitoes)
– Eastern and Western equine encephalitis
– West Nile virus
• Patients develop generalized as well as
focal signs
Herpes Simplex Type 1
• Most common in children and young
adults
• Affects inferior and medial temporal lobes
and orbital gyri of frontal lobe
– Alterations in mood, memory, and behavior
• Necrotizing and often hemorrhagic
• Inclusions in neurons and glia
Herpes Simplex Type 2
• Usually manifests in adults as meningitis
• Disseminated severe encephalitis in
neonates born by vaginal delivery to
women with primary active genital
infections
Cytomegalovirus
• Fetuses and immunocompromised individuals
• Tends to localize in the paraventricular
subependymal regions
– Severe hemorrhagic necrotizing ventriculoencephalitis
and choroid plexitis
• In utero infection
– Periventricular necrosis produces severe brain
destruction
– Microcephaly and periventricular calcification
Rabies
• Enters CNS by ascending along the peripheral nerves
from the wound site
– Incubation usually a few months
• Initially, malaise, fever, headache
• Advances to extreme CNS excitability
– Slightest touch is painful
– Violent motor responses
– Aversion to swallowing (hydrophobia)
• Progresses to alternating mania and stupor
• Coma and death from respiratory center failure
• Negri bodies: viral inclusions seen in pyramidal cells in
the hippocampus and Purkinje cells of cerebellum
HIV
• Patterns of direct injury to brain
– Aseptic HIV-1 meningitis
• 10% of individuals 1-2 weeks after seroconversion
– HIV-1 meningoencephalitis (subacute
encephalitis)
• AIDS-dementia complex
• Microglial nodules, multinucleated giant cells
• Neuronal death from cytokines and chemokines
– Vacuolar myelopathy
• Resembles combined subacute degeneration
Progressive Multifocal
Leukoencephalopathy
• Caused by JC virus
• Infects oligodendrocytes
– Demyelination is primary effect
• Immunocompromised individuals
– Reactivation of virus
• Focal and relentlessly progressive
neurological symptoms and signs
Fungal Encephalitis
• Usually in the immunosuppressed
• Granulomas or abscesses often with meningitis
• Organisms
– Candida albicans: microabscesses
– Mucor: direct extension in diabetics with ketoacidosis
– Aspergillus fumigatus: widespread hemorrhagic
infarcts, angioinvasive
– Cryptococcus neoformans: AIDS (can be fulminant or
indolent), India ink prep of CSF to visualize
– Also: Histoplasma, Coccidioides, Blastomyces
Other Meningoencephalitides
• Cerebral Toxoplasmosis
– AIDS
• Cysticercosis
– Tenia solium (tapeworm)
– Cysts in brain and meninges
• Amebic
– Naegleria
• Swimming in non-flowing warm fresh water
– Acanthamoeba
• Chronic granulomatous meningoencephalitis
Prion Diseases
• Disorders associated with abnormal forms
of a normal cellular protein called prion
protein (PrPc)
• Abnormal form acts as an infectious agent
– It propagates itself and damages cells that
contain it
• Most cases are sporadic or associated
with mutations in the gene that encodes
PrPc
Prion Diseases
• PrPc changes conformation to PrPsc
• PrPsc can then induce conformational change in
other PrPc molecules to PrPsc
• PrPsc is resistant to protease digestion
• PrPsc aggregates and damages the cell
• Leads to cytoplasmic vacuoles and eventual
neuronal death
• PrPc to PrPsc change occurs spontaneously at an
extremely low rate (sporadic cases)
• Mutation of gene for PrPc allows change at a
high rate (familial cases)
Prion Diseases
• Creutzfeldt-Jakob Disease (CJD)
– Rapidly progressive dementia
• Begins with subtle changes in memory and
behavior
– 85% of cases are sporadic
– 1 in 1 million annual incidence
– Peak incidence in seventh decade
– Uniformly fatal, average 7 months
– Spongiform transformation of the cerebral
cortex and deep gray matter
Prion Diseases
• Variant Creutzfeldt-Jakob Disease (vCJD)
– Starting in 1995, a series of cases of a CJD-like
illness appeared in the United Kingdom
– Differed from CJD
• Young adults
• Behavioral disorders were prominent in early disease stages
• Slower progression
– New disease was the consequence of exposure to
bovine spongiform encephalopathy
– Spongiform change and absence of inflammation, like
CJD, plus cortical amyloid plaques surrounded by
spongiform change
Tumors
• ½ to ¾ are primary, the rest are metastatic
– Annual incidence
• 10-17/100,000 intracranial
• 1-2/100,000 intraspinal
– Larger proportion of childhood cancers (20%)
• Adult and childhood tumors differ in
histological subtype and location
– Childhood: more likely posterior fossa
– Adults: more likely supratentorial
Tumors
• Unique characteristics
– Histological distinction between benign and malignant
is more subtle
– Low-grade lesions (low mitotic rate, cellular uniformity,
slow growth) may still infiltrate large regions of the
brain → serious deficits and poor prognosis
– Anatomic site can have lethal consequences even if
the tumor is benign histologically
– Pattern of spread
• Rarely metastasize outside of the CNS
• Seeding through the subarachnoid space can occur
Gliomas
• Astrocytomas
– Fibrillary astrocytomas
• 80% of adult primary tumors
• 4th through 6th decades
• Cerebral hemispheres
• Seizures, headache, focal deficits
• Histological differentiation correlates with clinical
course and outcome
– Astrocytoma (grade I and II)
– Anaplastic astrocytoma (grade III)
– Glioblastoma multiforme (grade IV)
Gliomas
• Astrocytomas
– Fibrillary astrocytomas
• Well differentiated
– Static or slowly progressive
– Mean survival >5 years
– Tumor usually progresses to higher grade with time
• Gliobastoma
– Mean survival 8-10 months
– <10% at 2 years
Gliomas
• Astrocytomas
– Fibrillary astrocytomas
• Infiltrative tumors that extend beyond grossly
apparent margins expanding and distorting brain
• Gray, high grade tumors have necrosis and
hemorrhage
• High grade tumors are contrast enhancing on
imaging studies
Gliomas
• Astrocytomas
– Pilocytic astrocytomas
• Relatively benign, often cystic tumors
• Children and young adults
• Cerebellum, usually
• Also 3rd ventricle, optic nerves, occasionally
cerebral hemispheres
• Symptomatic recurrence is often due to cyst
enlargement rather than solid component
Gliomas
• Oligodendroglioma
– 5-15% of gliomas
– 4th and 5th decades
– Cerebral hemispheres, white matter preference
– Several years of neurological complaints, often with
seizures
– Better prognosis than astrocytomas
• Mean survival 5-10 years
– “Fried egg” appearance of tumor cells, delicate
network of capillaries
– 90% have calcifications
Gliomas
• Ependymomas
– Arise next to ventricular system and central canal of
spinal cord
– In 1st two decades, occur near 4th ventricle
– Adults, occur in spinal cord most commonly
• Neurofibromatosis type 2 association
– CSF dissemination is common
– Supratentorial and spinal cord tumors have better
outcome than posterior fossa tumors
– Solid or papillary mass
– Rosettes and perivascular pseudorosettes
Neuronal Tumors
• Central neurocytoma
– Low grade adjacent to ventricular system
• Ganglioneuromas
– Mature looking neurons with a mixture of glial
elements
• Dysembryoplastic neuroepithelial tumor
– Distinctive low grade tumor of childhood
– Superficial temporal lobe
– “Floating neurons” in myxoid background
Medulloblastoma
• 20% of pediatric brain tumors
• Occurs exclusively in the cerebellum
– Children, midline tumors
– Adults, lateral tumors
• Largely undifferentiated, highly malignant
• Untreated, dismal prognosis
– Tumor is very radiosensitive
– Resection and radiation, 75% 5 year survival
• Similar tumors called CNS primitive
neuroectodermal tumors can occur elsewhere in
the CNS
Primary CNS Lymphoma
• 2% of extranodal lymphomas, 1% of intracranial
tumors
• Most common CNS neoplasm in
immunosuppressed individuals
– Nearly all EBV driven
• Most are diffuse large B cell lymphomas
• Aggressive, poor response to chemotherapy
• Multiple sites within the CNS are often involved
– Outside involvement is a rare and late complication
Germ Cell Tumors
• Primary brain germ cell tumors occur
along the midline
– Pineal (male predominance) and suprasellar
region
• 90% occur in first 2 decades
• Classification is similar to that used in the
testes (seminoma is called germinoma in
CNS)
Meningiomas
• Benign tumors of adults
• Attached to the dura usually, also can be seen in
the ventricles
• Derived from arachnoid meningothelial cells
• Vague non-localizing or focal symptoms from
brain compression
• Prognosis depends on size, location, surgical
accessibility, and histological grade
• Many histological patterns
– Psammoma bodies
Metastatic Tumors
• ¼ to ½ of intracranial tumors
• Most common primaries (80%)
– Lung, breast, skin (melanoma), kidney, GI
tract
• In the brain
– Sharply demarcated masses
– Often at gray matter-white matter junction
– Usually surrounded by a zone of edema
– Surrounded by reactive gliosis
Paraneoplastic Syndromes
• Most commonly associated with small cell
carcinoma of the lung
• Some characteristic patterns affecting the
CNS and PNS
– Subacute cerebellar degeneration → ataxia
– Limbic encephalitis → subacute dementia
– Subacute sensory neuropathy → altered pain
sensation
Diseases of Myelin
• Most diseases of CNS myelin do not
significantly involve the peripheral nerves,
and vice versa
• Two broad groups
– Demyelinating diseases
• Preferential damage to previously normal myelin
– Dysmyelinating diseases (leukodystrophies)
• Myelin is not properly formed or has abnormal
turnover kinetics
Multiple Sclerosis
• Autoimmune demyelinating disorder
• Distinct episodes of neurological deficits,
separated in time, attributable to white
matter lesions that are separated in space
• Prevalence 1/1000
• Age of onset: young adulthood to 50
• Twice as common in women
Multiple Sclerosis
• Believed to be caused by a combination of
environmental and genetic factors
– 1st degree relative: 15x risk
– 25% concordance rate among monozygotic twins
– Link to HLA-DR2
• T cell mediated delayed type hypersensitivity
reaction to myelin proteins is thought to be
central to the pathogenesis of MS
Multiple Sclerosis
• Morphology
– MS is a white matter disease
– Affected areas show plaques
• Well-circumscribed, glassy, gray-tan, irregularly-
shaped lesions
• Commonly occur beside ventricles
• Also frequent in optic nerves, optic chiasm, brain
stem, ascending and descending fiber tracts,
cerebellum, and spinal cord
Multiple Sclerosis
• Clinical
– Relapsing-remitting disease with gradual neurological
deterioration
– Common neurological symptoms and signs
• Unilateral visual impairment (optic neuritis)
• Cranial nerve signs
• Ataxia
• Disruption in conjugate eye movement (internuclear
ophthalmoplegia)
• Motor and sensory impairment of trunk and limbs
• Problems with voluntary control of bladder function
Multiple Sclerosis
– CSF
• Mildly elevated protein, increased gamma-globulin
• Oligoclonal bands
– Antibodies directed against a variety of targets
– Marker of disease activity
– Unclear of role in disease mechanism
Other Acquired Demyelinating
Diseases
• Post-infectious immune-mediated
demyelination
– Acute disseminated encephalomyelitis
• Acute onset, diffuse involvement a week or two
after antecedent infection
• May be fatal in 20% of cases
– Acute necrotizing hemorrhagic
encephalomyelitis
• More devastating disorder
• Young adults and children
Other Acquired Demyelinating
Diseases
• Central pontine myelinolysis
– Non-immune process resulting in loss of
myelin in central pons
– Most often due to rapid correction of
hyponatremia
– Seen in alcoholism and severe electrolyte or
osmolar imbalance
– Often presents with rapidly evolving
quadraplegia
Leukodystrophies
• Inherited dysmyelinating diseases
– Abnormal myelin synthesis or turnover
– Lysosomal enzymes, peroxisomal enzymes,
mutations in myelin proteins
• Much of the pathology is found in the white
matter
• Affected children are normal at birth but then
begin to miss developmental milestones
– Wide range of problems develop due to diffuse
involvement of white matter
Nutritional Diseases
• Thiamine deficiency
– Wernicke encephalopathy
• Abrupt development of confusion, abnormalities of eye
movement, and ataxia
• Hemorrhage and necrosis in mammillary bodies
– Korsakoff syndrome
• Consequence of untreated Wernicke encephalopathy
• Profound memory disturbances
• Largely irreversible
• Lesions in medial dorsal nucleus of thalamus
– Wernicke-Korsakoff syndrome is often applied
because of the link
– Chronic alcoholism association
Nutritional Diseases
• Vitamin B12 deficiency
– Subacute combined degeneration of the
spinal cord
• Involves ascending and descending fiber bundles
• Symptoms develop over weeks
– Slight ataxia
– Numbness and tingling in lower extremities
– Can progress to spastic weakness of lower extremities
– Complete paraplegia can occur
– Improvement with vitamin replacement therapy
– Poor recovery if complete paraplegia has developed
Degenerative Diseases and
Dementias
• Dementia
– Memory impairment and other cognitive deficits with
preservation of a normal level of consciousness
– Dementia always represents a pathologic process
– Not all forms of dementia are degenerative
• Degenerative disorders represent an underlying cellular
degeneration of neurons in the brain
• Vascular disorders are an important cause of dementia
Alzheimer Disease
• Most common cause of dementia in the elderly
• Clinical course
– Insidious impairment of higher intellectual functions,
with alterations in mood and behavior
– Progressive disorientation, memory loss, and aphasia
indicate severe cortical dysfunction
– Over the next 5 to 10 years, profoundly disabled,
mute, immobile
– Death usually occurs from pneumonia or other
infection
Alzheimer Disease
• Incidence
– 3% for age 65-74
– 19% for age 75-84
– 47% for age >85
• Clinical assessment and imaging allow for
accurate diagnosis in 80-90% of cases
– Pathological examination of brain needed for
definitive diagnosis
• Most cases are sporadic, some familial (5-10%)
• Rarely symptomatic before age 50
Alzheimer Disease
• Morphologic changes in brain and
dementia are initiated by the accumulation
of a peptide, β amyloid (Aβ)
• Aβ is derived from a larger membrane
protein, amyloid precursor protein (APP)
– Two processing paths
• Cleaved by α- and γ-secretase → no Aβ
• Cleaved by β- and γ-secretase → Aβ
• Generation and accumulation of Aβ occurs slowly
with advancing age
Alzheimer Disease
• Familial
– Mutations in APP or components of γ-secretase (presenilin-1 or
presenilin-2) increase rate of Aβ accumulation
• Alzheimer disease occurs in almost all individuals with
trisomy 21 (Down syndrome) who survive beyond age 45
– APP gene is on chromosome 21
• Sporadic
– Allele of apolipoprotein, ε4 (ApoE4), associated with 30% of
cases—how is unknown
– SORL1 associated with late onset, deficiency of SORL1 protein
may alter intercellular trafficking of APP
Alzheimer Disease
• Affects of Aβ on neurons
– Small aggregates alter neurotransmission and
can be toxic to neurons and synaptic endings
– Larger deposits, plaques, lead to neuronal
death, inflammatory response, may have
mechanical effects on axons and dendrites
altering region to region communication
– Leads neurons to hyperphosphorylate the
microtubule binding protein tau
Alzheimer Disease
• Tau protein
– Hyperphosphorylated tau redistributes within the
neuron
• From axon to dendrites and cell body
• Aggregates into tangles
• Results in neuronal dysfunction and cell death
• Development of plaques and tangles occur in
parallel are responsible for the development of
the clinical signs and symptoms
– They develop well in advance of clinical presentation
Alzheimer Disease
• Morphology
– Neuritic plaques, diffuse plaques,
neurofibrillary tangles, neuronal loss, and glial
reaction
– Pattern of progression
• Entorhinal cortex, hippocampal formation and
isocortex, then neocortex
Frontotemporal Dementias
• Degeneration and atrophy of the frontal
and temporal lobes
– Deterioration of language and changes in
personality
– Followed by memory disturbances
• Some caused by mutations of gene for tau
protein
• Some have disease defining inclusions of
abnormal accumulations of tau
Parkinsonism
• Clinical syndrome characterized by diminished
facial expression (masked facies), stooped
posture, slowness of voluntary movement,
festinating gait (progressive, shortened,
accelerated steps), rigidity, and “pill-rolling”
tremor
• Seen in a number of conditions that have
damage to dopaminergic neurons in the
substantia nigra or their projections to the
striatum
Idiopathic Parkinson Disease
• Most common neurodegenerative disorder associated
with Parkinsonism
• Progressive Parkinsonism in absence of a toxic or other
known etiology and clinical response to L-
dihydroxyphenylalanine (L-DOPA)
• Most cases are sporadic
– Autosomal dominant and recessive forms exist
– AD form associated with α-synuclein mutations
• Lewy bodies
– A diagnostic histological feature of Parkinson disease
– Neuronal inclusions containing α-synuclein
– Suggests defective degradation in the proteosome may play a
role in the disease (other genes support this, parkin and UCHL-
1)
Idiopathic Parkinson Disease
• Morphology
– Pallor of substantia nigra and locus ceruleus
• Loss of pigmented neurons and gliosis
– Lewy bodies
• Contain α-synuclein and other proteins including
neurofilament and ubiquitin
• Seen in remaining neurons of substantia nigra and locus
ceruleus
• Also seen in cholinergic cells of basal nucleus of Meynert
and other brain stem nuclei
• Similar structures can be seen in cerebral cortical neurons,
esp. cingulate and parahippocampal gyri
Idiopathic Parkinson Disease
• Clinical
– L-DOPA is effective for symptomatic relief but doesn’t
change progressive nature of the disease
– 10-15 years of progressive motor slowing until near
immobility
– Death usually result of infection or trauma from falls
– 10-15% develop dementia
• Fluctuating course and hallucinations
• Attributed to widely disseminated Lewy bodies in the cerebral
cortex
Huntington Disease
• Inherited autosomal dominant disorder
• Progressive movement disorders and
dementia, with degeneration of striatum
(caudate and putamen)
– Chorea affecting all parts of the body
– May develop Parkinsonism
• Relentlessly progressive resulting in death
after an average of 15 years
Huntington Disease
• All have a trinucleotide repeat expansion
in the gene for huntingtin located on
4p16.3
• Polymorphic CAG trinucleotide repeat in
the gene that encodes a polyglutamine
tract in the protein
– Normal alleles have 11 to 34 copies
– Disease alleles this can increase to hundreds
– More repeats earlier onset of disease
Huntington Disease
• Unclear how expanded polyglutamine tract
causes disease
– Binds to and sequesters transcription factors
– Functional abnormalities in mitochondria
– Aggregates of abnormal protein trigger
apoptosis
• Huntingtin is expressed widely throughout
the body
Huntington Disease
• Morphology
– Striking atrophy of the caudate nucleus
– Less dramatic atrophy of putamen
– Secondary ventricular dilation (lateral and 3rd)
– Neurons that use GABA are especially
affected
Huntington Disease
• Clinical
– Onset in 4th or 5th decade
– Motor symptoms precede cognitive
impairment
– Choreiform movements
– Forgetfulness and thought and affective
disorders, may progress to severe dementia
– Increased risk of suicide
– Infection most common cause of death
Spinocerebellar Degenerations
• Heterogeneous group of disorders
– Includes several distinct diseases
• Affects cerebellar cortex, spinal cord, other
brain regions, and peripheral nerves
• Degeneration of neurons without distinct
pathological changes in the affected areas
with mild gliosis
• Many are caused by expansion of CAG
repeats
Friedreich Ataxia
• Autosomal recessive
• Begins in 1st decade with gait ataxia and
followed by hand clumsiness and
dysarthria
– Deep tendon reflexes are diminished to
absent, extensor plantar reflex is present
– Loss of joint position and vibratory sense
– Pain, temperature, and light touch may be
diminished
Friedreich Ataxia
– High incidence of cardiac disease and
diabetes
– Most patients are wheelchair bound within 5
years
• Caused by a GAA trinucleotide repeat
expansion (intronic) in a protein that is
involved in determining iron levels in cells
– Results in low protein levels
Motor Neuron Diseases
• Series of diseases that affect lower motor
neurons in the spinal cord and brain stem
and upper motor neurons in the motor
cortex
• Sensory systems and cognitive functions
are usually unaffected
• Types with dementia do occur
Amyotrophic Lateral Sclerosis
• Most common form of neurodegeneration
affecting the motor system
– Loss of both upper and lower motor neurons
– Men slightly more than women
– Onset in 5th decade or later
– Most are sporadic, 5-10% familial (AD)
• Half of familial cases have mutation of superoxide
dismutase, SOD1
Amyotrophic Lateral Sclerosis
• Morphology
– Loss of anterior horn neurons
– Degeneration of lateral corticospinal tracts
• Clinical
– Weakness of hands
– Cramping and spasticity of arms and legs
– Diminished muscle strength and bulk with
fasciculations
– 50% 5 year survival
Bulbospinal Atrophy
• Kennedy disease
• X-linked adult onset disease affecting
lower motor neurons
• Affected individuals manifest androgen
insensitivity
– Gynecomastia, testicular atrophy,
oligospermia
• Trinucleotide repeat disorder
– Polyglutamine repeat in androgen receptor
Spinal Muscular Atrophy
• Distinctive group of autosomal recessive motor
neuron diseases that begin in childhood and
adolescence
• Loss of motor neurons and weakness
associated with muscle fiber atrophy that often
involves entire fascicles
• Werdnig-Hoffmann disease (SMA1) is the most
common form
– Onset at birth or within 4 months
– Leads to death within 3 years
• All forms are associated with mutations of SMN
gene on chromosome 5
Familial Tumor Syndromes
• Inherited diseases characterized by the
development of hamartomas and neoplasms
throughout the body
• Those with particular involvement of the nervous
system follow
• Because of involvement of the nervous system
and cutaneous manifestations, they have been
grouped under the term “neurophakomatoses”
• Most are linked to loss of tumor suppressor
genes
Neurofibromatosis Type 1
• Autosomal dominant
• Characterized by
– Neurofibromas (plexiform and solitary)
– Gliomas of the optic nerve
– Pigmented nodules of the iris (Lisch nodules)
– Cutaneous hyperpigmented macules (café au
lait spots)
• One of the more common genetic
disorders, 1 in 3000
Neurofibromatosis Type 1
• Neurofibromas have a propensity to undergo
malignant change
• NF1 gene is a tumor suppressor gene
– Thought to be involved in G-protein dependent signal
transduction pathways
• Disease is highly variable
– Individuals with a mutated gene may have no
symptoms while others have progressive with spinal
deformities, disfiguring lesions, and compression of
vital structures including the spinal cord
Neurofibromatosis Type 2
• Autosomal dominant
• Tumors
– Bilateral vestibular schwannomas (acoustic
neuromas)
– Multiple meningiomas
– Gliomas (ependymomas) of spinal cord
• Frequency of 1 in 40,000-50,000
• NF2 gene on chromosome 22
– Also mutated in sporadic meningiomas and
schwannomas
Tuberous Sclerosis
• Autosomal dominant
• Hamartomas and benign tumors
– Cortical and subependymal hamartomas
• Seizures are associated with cortical lesions
– Renal angiomyolipomas
– Retinal glial hamartomas
– Pulmonary lesions
– Cardiac rhabdomyomas
Tuberous Sclerosis
• Cysts of liver, kidneys, pancreas
• Cutaneous lesions
– Angiofibromas
– Shagreen patches (leathery thickenings)
– Hypopigmented areas (ash-leaf patches)
– Subungual fibromas
• Mutations of tumor suppressor genes,
TSC1 (hamartin) and TSC2 (tuberin)
– Interact and regulate signaling pathways
von Hippel-Lindau Disease
• Autosomal dominant
• Hemangioblastomas involving the cerebellar
hemispheres, retina, and less commonly the
brain stem and spinal cord
• Cysts of pancreas, liver, kidney
• High risk of renal cell carcinoma
• Frequency of 1 in 30,000-40,000
• Mutations in tumor suppressor gene VHL
– Also associated with adrenal pheochromocytoma
– Gene controls angiogenesis, esp. in response to
hypoxia
You might also like
- Brain CTDocument83 pagesBrain CTArvind Jha100% (2)
- Protocol Hybridization Capture of Dna Libraries Using Xgen Lockdown Probes and Reagents Version 3Document16 pagesProtocol Hybridization Capture of Dna Libraries Using Xgen Lockdown Probes and Reagents Version 3Rodger12No ratings yet
- NS1881 EXAM PREP Flashcards - QuizletDocument3 pagesNS1881 EXAM PREP Flashcards - QuizletLaetitia ReyesNo ratings yet
- HINDMAN, Hillbilly Yeast Propagation ProjectDocument40 pagesHINDMAN, Hillbilly Yeast Propagation ProjectDoug HindmanNo ratings yet
- Pathology of CNS: Eric M. Mirandilla MD, DPSPDocument71 pagesPathology of CNS: Eric M. Mirandilla MD, DPSPDhruva PatelNo ratings yet
- Stroke Intracranial Hypertension Cerebral EdemaDocument67 pagesStroke Intracranial Hypertension Cerebral EdemabettyNo ratings yet
- Cns Pathology: Cerebral InfarctionDocument24 pagesCns Pathology: Cerebral InfarctionElvisNo ratings yet
- Pathology of The Central Nervous System (CNS)Document53 pagesPathology of The Central Nervous System (CNS)Rikizu HobbiesNo ratings yet
- Acquired Central Nervous System Vascular Disorders-1Document39 pagesAcquired Central Nervous System Vascular Disorders-1Jake MillerNo ratings yet
- Stroke 1Document69 pagesStroke 1Berk HalilbeyoğluNo ratings yet
- The CNS CVADocument21 pagesThe CNS CVAfatima.noor0747No ratings yet
- Cerebral CirculationDocument28 pagesCerebral CirculationMac Del Ro RebNo ratings yet
- Stroke (Encephalitis/Meningitis) Trauma Kepala Trauma Medulla SpinalisDocument61 pagesStroke (Encephalitis/Meningitis) Trauma Kepala Trauma Medulla SpinalisUmar MukhtarNo ratings yet
- Lecture 3Document41 pagesLecture 3issrafil mussaNo ratings yet
- CNS VascularDocument36 pagesCNS Vascularapi-3705408No ratings yet
- Cerebrovascular DiseasesDocument69 pagesCerebrovascular Diseaseshuda dotNo ratings yet
- Stroke: Abyot From Harrison, DR Belachew and DR Yared HandoutDocument32 pagesStroke: Abyot From Harrison, DR Belachew and DR Yared HandoutashuNo ratings yet
- Brain EdemaDocument13 pagesBrain Edema王懷華No ratings yet
- Pediatric StrokeDocument90 pagesPediatric StrokeJanaki SethuramanNo ratings yet
- Cerebral-Vascular Diseases (CVD) Ischemic Heart Diseases (IHD)Document38 pagesCerebral-Vascular Diseases (CVD) Ischemic Heart Diseases (IHD)Faheem MusthafaNo ratings yet
- Cerebrovascular DiseasesDocument15 pagesCerebrovascular DiseaseskiflomNo ratings yet
- Cerebrovascular DiseasesDocument15 pagesCerebrovascular DiseaseskiflomNo ratings yet
- Neuroradiology Sah and StrokeDocument81 pagesNeuroradiology Sah and StrokeJujhar BoparaiNo ratings yet
- Cerebrovascular Pathology: Abel B. (MD) Pathology Lectures, NMEI, DBUDocument59 pagesCerebrovascular Pathology: Abel B. (MD) Pathology Lectures, NMEI, DBUdenekeNo ratings yet
- Stroke: Dr. Alberto CampodónicoDocument17 pagesStroke: Dr. Alberto CampodónicoJohn Domínguez MedinaNo ratings yet
- Bleed Vs Infarct ComparisonDocument7 pagesBleed Vs Infarct ComparisonJed ContrerasNo ratings yet
- C VADocument25 pagesC VAsudeepminz15No ratings yet
- Patho StrokeDocument14 pagesPatho StrokeKyla R. PinedaNo ratings yet
- Patofisiologi StrokeDocument14 pagesPatofisiologi Strokenatalia alexandraNo ratings yet
- Vascular Disorder: DR Nur Asyilla Che Jalil Pathology Department PPSP HusmDocument140 pagesVascular Disorder: DR Nur Asyilla Che Jalil Pathology Department PPSP HusmHaziq KamardinNo ratings yet
- Cerebral Aneurysm: By: Cristi Ne Reyes Al-Sundal, RN, MN NCM 118 InstuctorDocument21 pagesCerebral Aneurysm: By: Cristi Ne Reyes Al-Sundal, RN, MN NCM 118 InstuctorVhince Norben PiscoNo ratings yet
- Stroke HemoragikDocument34 pagesStroke HemoragikTeuku AndyNo ratings yet
- Oral Rev MS Notes 1Document37 pagesOral Rev MS Notes 1Fan XiaoNo ratings yet
- Vascular System PathologyDocument63 pagesVascular System PathologyrohitNo ratings yet
- Cardiovascular Pathology 1:: Blood VesselsDocument48 pagesCardiovascular Pathology 1:: Blood VesselsRaiver CadenNo ratings yet
- Lacunar Infarct and SyndromesDocument40 pagesLacunar Infarct and Syndromeslovelots1234100% (1)
- Cardiovascular Pathology 2024Document132 pagesCardiovascular Pathology 2024Chen HouyuNo ratings yet
- Head InjuriesDocument39 pagesHead Injurieslionel andreaNo ratings yet
- Fluid and Hemodynamic DisordersDocument19 pagesFluid and Hemodynamic DisordersapplesncoreNo ratings yet
- Disease of Nervous System Lect 2Document62 pagesDisease of Nervous System Lect 2Monirul IslamNo ratings yet
- CerebrumDocument26 pagesCerebrumsanthiyasandy100% (1)
- Jeffreyasalonga, PTRPDocument72 pagesJeffreyasalonga, PTRPasdNo ratings yet
- 5 - Pathology of CADDocument58 pages5 - Pathology of CADregeti bhargavNo ratings yet
- Neuropathology: Fajar L. Gultom Patologi Anatomik FK-UKI 2018Document28 pagesNeuropathology: Fajar L. Gultom Patologi Anatomik FK-UKI 2018Fitri Yani Putri NingsihNo ratings yet
- 11.sudden Natural Death 3Document55 pages11.sudden Natural Death 3Hasabo AwadNo ratings yet
- Group 4 - Hemorrhagic StrokeDocument60 pagesGroup 4 - Hemorrhagic StrokeKitz T AnasarioNo ratings yet
- Pathophysiology of Diabetic RetinopathyDocument40 pagesPathophysiology of Diabetic RetinopathyGetLyricsNo ratings yet
- Pathology Preclinic #5 Assignment - CNSDocument7 pagesPathology Preclinic #5 Assignment - CNSaimy.palawataraNo ratings yet
- Cvs BCMDocument117 pagesCvs BCMjaniceli0207No ratings yet
- Cerebrovascular DseDocument303 pagesCerebrovascular DsejjamadriagaNo ratings yet
- Cerebrospinal Fluid and Blood Brain BarrierDocument29 pagesCerebrospinal Fluid and Blood Brain BarrierSaiAlekhaBabuNo ratings yet
- HNI 310 - Cardiovascular System BB 2015Document59 pagesHNI 310 - Cardiovascular System BB 2015Mohammad Usman QureshiNo ratings yet
- Cerebrovascular Disease and Coronary Artery Disease: DR Masona-MutitiDocument28 pagesCerebrovascular Disease and Coronary Artery Disease: DR Masona-MutitiShaun MazorodzeNo ratings yet
- The Ventricular System1Document44 pagesThe Ventricular System1emmakooffNo ratings yet
- Taufan Arif, S.Kep., NS., M.KepDocument85 pagesTaufan Arif, S.Kep., NS., M.KepputriNo ratings yet
- Head Trauma: Victor LibertoDocument40 pagesHead Trauma: Victor LibertoMuhamad Fernando MahardikaNo ratings yet
- Abnormalities Associated With Nervous SystemDocument17 pagesAbnormalities Associated With Nervous SystemroseNo ratings yet
- Brain Injury: Closed (Blunt) Brain Injury Occurs When The Head Accelerates and ThenDocument7 pagesBrain Injury: Closed (Blunt) Brain Injury Occurs When The Head Accelerates and Thencute_tineeNo ratings yet
- Ischaemic Heart DiseaseDocument25 pagesIschaemic Heart DiseaseKelvinTMaikanaNo ratings yet
- Pathology of Stroke: Dr. Isnaniah, Sp. SDocument51 pagesPathology of Stroke: Dr. Isnaniah, Sp. SFiladelfia sariNo ratings yet
- STROKE: Handbook with activities, exercises and mental challengesFrom EverandSTROKE: Handbook with activities, exercises and mental challengesNo ratings yet
- Neurology Equations Made Simple: Differential Diagnosis and NeuroemergenciesFrom EverandNeurology Equations Made Simple: Differential Diagnosis and NeuroemergenciesNo ratings yet
- Cerebral Edema, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCerebral Edema, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- DR B. Neuroanatomy BookDocument134 pagesDR B. Neuroanatomy BookMURESAN MARIANo ratings yet
- Pathfit 1Document23 pagesPathfit 1Sep TemNo ratings yet
- L.a.plant ReproductionDocument2 pagesL.a.plant ReproductionFlopez LópezNo ratings yet
- Reaction Time To Neutral & Emotional Word: Psychology 101 Lab ExperimentDocument12 pagesReaction Time To Neutral & Emotional Word: Psychology 101 Lab ExperimentMalihaHaqueNo ratings yet
- EP Diamandis Website-Full CV Edited 2009Document88 pagesEP Diamandis Website-Full CV Edited 2009porfyra_No ratings yet
- Agar To GrainDocument3 pagesAgar To GrainSorath MezaNo ratings yet
- Introduction To Anatomy and PhysiologyDocument24 pagesIntroduction To Anatomy and PhysiologyJan MichaelNo ratings yet
- 19msent083 T.n.v.vidya SagarDocument8 pages19msent083 T.n.v.vidya SagarmanojNo ratings yet
- 11 Biology Notes Ch06 Anatomy of Flowering PlantsDocument8 pages11 Biology Notes Ch06 Anatomy of Flowering PlantsSyamala NatarajanNo ratings yet
- Er The Est Er More The Most: BetterDocument1 pageEr The Est Er More The Most: BetterTokai IbolyaNo ratings yet
- 10 11646@zootaxa 4543 2 3Document20 pages10 11646@zootaxa 4543 2 3CoNo ratings yet
- TNF-dental PulpDocument3 pagesTNF-dental PulpNicolas PintoNo ratings yet
- Instinct Theory of MotivationDocument4 pagesInstinct Theory of MotivationpavaniNo ratings yet
- Circulatory SystemDocument30 pagesCirculatory SystemScheherazade CNo ratings yet
- Overview of Self - Identity.Document6 pagesOverview of Self - Identity.Jefferson Madridano LotivioNo ratings yet
- Hussain et al_NEJM_2020Document13 pagesHussain et al_NEJM_2020zdmoorNo ratings yet
- MovSciLec MSC 2101 Week16Document11 pagesMovSciLec MSC 2101 Week16Mary SotoNo ratings yet
- Tropical ForestDocument11 pagesTropical ForestAnthony MoleñoNo ratings yet
- BioChemReportFINAL WITH EXMPLESDocument9 pagesBioChemReportFINAL WITH EXMPLESDaryl AquinoNo ratings yet
- Development: Dr. Nagwa GadDocument37 pagesDevelopment: Dr. Nagwa GadKholoud KholoudNo ratings yet
- Study File 1Document18 pagesStudy File 1Leones JessiejuneNo ratings yet
- Chapter 7: Pelvis and PerineumDocument22 pagesChapter 7: Pelvis and PerineumAlaz NellyNo ratings yet
- Assignment PDFDocument5 pagesAssignment PDFDipesh TerseNo ratings yet
- General Characteristics of Viruses PDFDocument2 pagesGeneral Characteristics of Viruses PDFabdulNo ratings yet
- Dendrelaphis Schokari (Schokar's Bronzeback) - PredationDocument31 pagesDendrelaphis Schokari (Schokar's Bronzeback) - PredationH.Krishantha Sameera de ZoysaNo ratings yet
- Meroplankton Part IDocument5 pagesMeroplankton Part IMuhammad Nur SaidNo ratings yet
- PolymersDocument13 pagesPolymerspradeepkumar221095gmailNo ratings yet