Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
4 viewsObstructive Shock: Harrisons Principles of Internal Medicine
Obstructive Shock: Harrisons Principles of Internal Medicine
Uploaded by
Mohammad Jofa Rachman PObstructive shock is characterized by reduced cardiac output and oxygen delivery due to extracardiac processes that impair blood flow rather than problems with the heart itself. Common causes include tension pneumothorax, cardiac tamponade from fluid around the heart, and pulmonary embolism from blood clots in the lungs. Tension pneumothorax requires immediate needle decompression and chest tube placement. Cardiac tamponade may require bedside ultrasound and pericardiocentesis. Massive pulmonary embolism is treated with small fluid volumes, vasopressors, and potentially thrombolysis if it causes profound hypotension.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- ECG Mastery Yellow Belt WorkbookDocument118 pagesECG Mastery Yellow Belt WorkbookOana Anghel100% (9)
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Hasil Ujian KKD Mengenaal Sel Daan Hitung Jenis Blok Hematologi 2021Document9 pagesHasil Ujian KKD Mengenaal Sel Daan Hitung Jenis Blok Hematologi 2021Mohammad Jofa Rachman PNo ratings yet
- Dental Care For Patients With Heart Failure: An UpdateDocument9 pagesDental Care For Patients With Heart Failure: An UpdateGustavo A OrtegonNo ratings yet
- AirwayDocument25 pagesAirwayKURIMAONGNo ratings yet
- Valvular Heart Disease To TW FinalDocument13 pagesValvular Heart Disease To TW FinalMohammed ElSayedNo ratings yet
- Valvular Heart DiseseDocument41 pagesValvular Heart DisesefadhiliNo ratings yet
- Pathophysiology: Cardiovascular System Dr. Maen DweikDocument38 pagesPathophysiology: Cardiovascular System Dr. Maen DweikshoibyNo ratings yet
- ShockDocument14 pagesShockNatia UtmelidzeNo ratings yet
- AnginaDocument37 pagesAnginaSHAHALOMGIR AHMEDNo ratings yet
- Cardiovascular Disease and Anaesthesia: HypertensionDocument4 pagesCardiovascular Disease and Anaesthesia: Hypertensionsatria wibawaNo ratings yet
- Kardiogenik SyokDocument43 pagesKardiogenik SyokGalih Arief Harimurti WawolumajaNo ratings yet
- SHOCKDocument17 pagesSHOCKChithra Saju100% (1)
- Hypertrophic CardiomyopathyDocument32 pagesHypertrophic CardiomyopathyAbnet WondimuNo ratings yet
- Cardiac Tamponade (P)Document16 pagesCardiac Tamponade (P)CloudySkyNo ratings yet
- The Emergency ManagementDocument12 pagesThe Emergency ManagementWidya Surya AvantiNo ratings yet
- ShockDocument19 pagesShockasmyr6975No ratings yet
- AclsDocument4 pagesAclsAnusha Verghese100% (1)
- Management of The Patients WithDocument68 pagesManagement of The Patients WithДіна ШоріковаNo ratings yet
- Study Notes Emergency MedicineDocument12 pagesStudy Notes Emergency MedicineMedShare57% (7)
- Cardiogenic ShockDocument49 pagesCardiogenic Shockmaibejose0% (1)
- Cardiovascular DiseasesDocument67 pagesCardiovascular DiseasesokaciaNo ratings yet
- Patofisiologi Shock CardiogenicDocument44 pagesPatofisiologi Shock CardiogenicGalih Arief Harimurti Wawolumaja100% (1)
- Congestive Heart FailureDocument6 pagesCongestive Heart Failureseigelystic100% (1)
- Valvular Heart DiseasesDocument60 pagesValvular Heart DiseasesEthiopia TekdemNo ratings yet
- Cardiology Review SessionDocument139 pagesCardiology Review SessionNour LakisNo ratings yet
- Tetrology of Fallot 2Document25 pagesTetrology of Fallot 2KV18 KK5No ratings yet
- Structural Infectious and Inflammatory Cardiac Disorders and Medical ManagementDocument85 pagesStructural Infectious and Inflammatory Cardiac Disorders and Medical Managementmoncalshareen3No ratings yet
- Cardiac Tamponade and ManagementDocument42 pagesCardiac Tamponade and Managementأم حمدNo ratings yet
- Acute HF-IAIDocument49 pagesAcute HF-IAIAndita ListyannisaNo ratings yet
- PulmonaryDocument3 pagesPulmonaryBaha'aeddin HammadNo ratings yet
- ADHF Up To DateDocument25 pagesADHF Up To DateAndreas Agung KurniawanNo ratings yet
- Hemodynamic Unstable Patient Following ArrhythmiaDocument30 pagesHemodynamic Unstable Patient Following Arrhythmialew chin hongNo ratings yet
- CSS - Advanced Life SupportDocument16 pagesCSS - Advanced Life SupportnrahmaNo ratings yet
- Shock With Jugular Venous Distention: Clinical Review ArticleDocument9 pagesShock With Jugular Venous Distention: Clinical Review ArticlenevmerkaNo ratings yet
- Cardiogenic ShockDocument29 pagesCardiogenic ShockagnescheruseryNo ratings yet
- Pemicu 6 KGD DeniseDocument95 pagesPemicu 6 KGD DeniseVincent VandestyoNo ratings yet
- Myocarditis - PericarditisDocument21 pagesMyocarditis - PericarditisMahesh RathnayakeNo ratings yet
- Fluid Resuscitation in Haemorrhagic ShockDocument9 pagesFluid Resuscitation in Haemorrhagic ShockbashiruaminuNo ratings yet
- Unit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructureDocument37 pagesUnit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructurebtaleraNo ratings yet
- 3 - Valvular Heart DiseasesDocument31 pages3 - Valvular Heart DiseasesLobna ElkilanyNo ratings yet
- Cardiac EmergencyDocument56 pagesCardiac Emergency21rayhanf100% (1)
- Cardiac TamponadeDocument29 pagesCardiac Tamponadeanimesh pandaNo ratings yet
- 3 Three - Mitral RegurgeDocument23 pages3 Three - Mitral Regurgeمحمد بن الصادقNo ratings yet
- Cardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityDocument35 pagesCardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityBarlonga Yhan YogaNo ratings yet
- Case 5Document16 pagesCase 5Hany ElbarougyNo ratings yet
- STROKEDocument6 pagesSTROKEOxy GenNo ratings yet
- Thyroid StormDocument6 pagesThyroid StormCristina CenturionNo ratings yet
- Medical Surgery-2Document10 pagesMedical Surgery-2Wanjiku NderituNo ratings yet
- Model Answer -I & II سبتمبر 2015تحريريDocument12 pagesModel Answer -I & II سبتمبر 2015تحريريAmr El TaherNo ratings yet
- DR Ali Cardiology-MergedDocument684 pagesDR Ali Cardiology-MergedK PradhanNo ratings yet
- Media 115008 en PDFDocument12 pagesMedia 115008 en PDFsukandeNo ratings yet
- Cardiogenic Shock: Submitted ToDocument5 pagesCardiogenic Shock: Submitted Toal-obinay shereenNo ratings yet
- Topic:: Unstable AnginaDocument44 pagesTopic:: Unstable AnginaApurba100% (1)
- Medicine Osce Compiled and Solved - EcgsDocument46 pagesMedicine Osce Compiled and Solved - EcgsamashooquekubarNo ratings yet
- Intra Operative Considerations in Mitral Stenosis Patient: Salil MaheshwariDocument26 pagesIntra Operative Considerations in Mitral Stenosis Patient: Salil MaheshwarisalilNo ratings yet
- Cardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarDocument23 pagesCardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarD. Melba S.S ChinnaNo ratings yet
- CardioDocument9 pagesCardioVirgilio Reyes ManuelNo ratings yet
- 9 CsaDocument34 pages9 Csaمحمد بن الصادقNo ratings yet
- Critical Care in The Emergency Department: Shock and Circulatory SupportDocument10 pagesCritical Care in The Emergency Department: Shock and Circulatory SupportKhaled AbdoNo ratings yet
- Acute Coronary SyndromeDocument93 pagesAcute Coronary SyndromeissareinoNo ratings yet
- Cardiac TemponadeDocument18 pagesCardiac TemponadeDIVYA GANGWAR100% (1)
- CH 46 Complications of AnaesthesiaDocument29 pagesCH 46 Complications of AnaesthesiaChristian LeepoNo ratings yet
- Cardiac Tamponade (Suryani)Document72 pagesCardiac Tamponade (Suryani)Hamdani UsmanNo ratings yet
- John 2016Document3 pagesJohn 2016Mohammad Jofa Rachman PNo ratings yet
- Seizure Focal SeizuresDocument8 pagesSeizure Focal SeizuresMohammad Jofa Rachman PNo ratings yet
- Mel Zack 1975Document23 pagesMel Zack 1975Mohammad Jofa Rachman PNo ratings yet
- First Problem: Friday, 24 September 2021 Group 19 - 20Document69 pagesFirst Problem: Friday, 24 September 2021 Group 19 - 20Mohammad Jofa Rachman PNo ratings yet
- 19-20 Second ProblemDocument108 pages19-20 Second ProblemMohammad Jofa Rachman PNo ratings yet
- Seminar IDAI Protein Intake To Support Immune System Children With Allergy Disease PDFDocument39 pagesSeminar IDAI Protein Intake To Support Immune System Children With Allergy Disease PDFMohammad Jofa Rachman PNo ratings yet
- Tropical Fevers: C. Important Human Parasitic Fevers of The TropicsDocument25 pagesTropical Fevers: C. Important Human Parasitic Fevers of The TropicsMohammad Jofa Rachman PNo ratings yet
- Tabel Origo-Insersi Myologi (Ex. Superio & Inferior)Document8 pagesTabel Origo-Insersi Myologi (Ex. Superio & Inferior)Mohammad Jofa Rachman PNo ratings yet
- Tabel KinesiologiDocument4 pagesTabel KinesiologiMohammad Jofa Rachman PNo ratings yet
- PROBLEM 3 GIT Jeffrey 405170048Document162 pagesPROBLEM 3 GIT Jeffrey 405170048Mohammad Jofa Rachman PNo ratings yet
- Absensi Kakak Asuh 2020-2021 Fixxx PDFDocument7 pagesAbsensi Kakak Asuh 2020-2021 Fixxx PDFMohammad Jofa Rachman PNo ratings yet
- Yellowish Lesions of The Oral Cavity. Suggestion For A ClassificationDocument6 pagesYellowish Lesions of The Oral Cavity. Suggestion For A ClassificationMohammad Jofa Rachman PNo ratings yet
- Anatomi Abdominal, Viscera Abdomen Dan Regio AbdominalesDocument15 pagesAnatomi Abdominal, Viscera Abdomen Dan Regio AbdominalesMohammad Jofa Rachman PNo ratings yet
- Rangkuman CCS 1Document16 pagesRangkuman CCS 1Tesis Maruli Tua SianiparNo ratings yet
- Lesson 1 - Disease and InfectionDocument28 pagesLesson 1 - Disease and InfectionJohn Raiel OlarteNo ratings yet
- Pediatric Nursing: Prepared By: Adahlia T. Basco RN, MANDocument226 pagesPediatric Nursing: Prepared By: Adahlia T. Basco RN, MANMika SamsonNo ratings yet
- How To Measure Blood Pressure Using A SphygmomanometerDocument3 pagesHow To Measure Blood Pressure Using A SphygmomanometerpadritovechioNo ratings yet
- CURS 5 Abnormalities of The Umbilical Cord and Amniotic FluidDocument33 pagesCURS 5 Abnormalities of The Umbilical Cord and Amniotic FluidFayad AlmohamedNo ratings yet
- Emergency and Critical Care Procedures in Small AnimalsDocument9 pagesEmergency and Critical Care Procedures in Small AnimalsTessaNo ratings yet
- Anatomy and Physiology Veins of The Lower LimbsDocument3 pagesAnatomy and Physiology Veins of The Lower LimbsRoel John Atamosa CasilacNo ratings yet
- Chapter 21 AddqDocument12 pagesChapter 21 AddqLenel John Giban Bagunas100% (1)
- Genetics NotesDocument15 pagesGenetics NotesIshtiaque KhanNo ratings yet
- Management of Pregnancy at RiskDocument40 pagesManagement of Pregnancy at RiskMA. JYRELL BONITONo ratings yet
- Blood Gases and Acid-Base BalanceDocument11 pagesBlood Gases and Acid-Base BalanceREMAN ALINGASANo ratings yet
- 8 High Blood Pressure TreatmentDocument4 pages8 High Blood Pressure TreatmentMuhammad Talha AttariNo ratings yet
- Cambridge Checkpoint Notes ExcretionDocument3 pagesCambridge Checkpoint Notes Excretionanimemaster2kNo ratings yet
- Normal Fetal Growth and DevelopmentDocument38 pagesNormal Fetal Growth and DevelopmentArhum SiddiqiNo ratings yet
- Ainul Haq Report 2Document27 pagesAinul Haq Report 2Mohd AliNo ratings yet
- PDF Reyes Christine Mae DDDocument23 pagesPDF Reyes Christine Mae DDmelodia gandezaNo ratings yet
- History Taking and Ce of Cardiac PatientsDocument89 pagesHistory Taking and Ce of Cardiac Patientsapi-3858544100% (1)
- Complication of Dentoalveolar SurgeryDocument21 pagesComplication of Dentoalveolar Surgerywhussien7376No ratings yet
- Blumenfeld Neuroanatomy Ch. 5 SummaryDocument5 pagesBlumenfeld Neuroanatomy Ch. 5 SummaryMeeraNo ratings yet
- Congestive Heart Failure (PH 2 Bemdiji)Document1 pageCongestive Heart Failure (PH 2 Bemdiji)api-285694335No ratings yet
- Drug Study Atropine SulfateDocument1 pageDrug Study Atropine Sulfateirhizzp75% (8)
- DR Ahlquist - 0 - 0Document20 pagesDR Ahlquist - 0 - 0jinhan.chiengNo ratings yet
- Dihydrotestosterone (DHT) - DHT Stimulates Cell Growth in The Tissue That Lines The Prostate GlandDocument7 pagesDihydrotestosterone (DHT) - DHT Stimulates Cell Growth in The Tissue That Lines The Prostate GlandPeter Kenneth LampitocNo ratings yet
- ECG Interpretation For ACLSDocument27 pagesECG Interpretation For ACLSZH. omg sarNo ratings yet
- Radiology 165 3 3317501Document4 pagesRadiology 165 3 3317501Dzulfachri KurniawanNo ratings yet
- Chapter22 Assessment of Pheripheral Vascular SystemDocument33 pagesChapter22 Assessment of Pheripheral Vascular SystemMARY ANNE JUDE ANTHONYNo ratings yet
- What Is Hypertension? 6 Ways To Prevent HypertensionDocument3 pagesWhat Is Hypertension? 6 Ways To Prevent HypertensionAnastasya Gishella RorongNo ratings yet
Obstructive Shock: Harrisons Principles of Internal Medicine
Obstructive Shock: Harrisons Principles of Internal Medicine
Uploaded by
Mohammad Jofa Rachman P0 ratings0% found this document useful (0 votes)
4 views6 pagesObstructive shock is characterized by reduced cardiac output and oxygen delivery due to extracardiac processes that impair blood flow rather than problems with the heart itself. Common causes include tension pneumothorax, cardiac tamponade from fluid around the heart, and pulmonary embolism from blood clots in the lungs. Tension pneumothorax requires immediate needle decompression and chest tube placement. Cardiac tamponade may require bedside ultrasound and pericardiocentesis. Massive pulmonary embolism is treated with small fluid volumes, vasopressors, and potentially thrombolysis if it causes profound hypotension.
Original Description:
Original Title
Jofa_firstproblem
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentObstructive shock is characterized by reduced cardiac output and oxygen delivery due to extracardiac processes that impair blood flow rather than problems with the heart itself. Common causes include tension pneumothorax, cardiac tamponade from fluid around the heart, and pulmonary embolism from blood clots in the lungs. Tension pneumothorax requires immediate needle decompression and chest tube placement. Cardiac tamponade may require bedside ultrasound and pericardiocentesis. Massive pulmonary embolism is treated with small fluid volumes, vasopressors, and potentially thrombolysis if it causes profound hypotension.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
4 views6 pagesObstructive Shock: Harrisons Principles of Internal Medicine
Obstructive Shock: Harrisons Principles of Internal Medicine
Uploaded by
Mohammad Jofa Rachman PObstructive shock is characterized by reduced cardiac output and oxygen delivery due to extracardiac processes that impair blood flow rather than problems with the heart itself. Common causes include tension pneumothorax, cardiac tamponade from fluid around the heart, and pulmonary embolism from blood clots in the lungs. Tension pneumothorax requires immediate needle decompression and chest tube placement. Cardiac tamponade may require bedside ultrasound and pericardiocentesis. Massive pulmonary embolism is treated with small fluid volumes, vasopressors, and potentially thrombolysis if it causes profound hypotension.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 6
OBSTRUCTIVE SHOCK
• Obstructive shock is also characterized by a reduction in oxygen
delivery related to reduced CO, but in this case the etiology of the
reduced CO is an extracardiac processes impairing blood flow.
Processes that can impede venous return to the heart and reduce CO
include tension pneumothorax (PTX), cardiac tamponade, and
restrictive pericarditis. Similarly processes that obstruct cardiac
outflow, such as pulmonary embolism (right heart) or aortic dissection
(left heart), are included in this shock type category.
Harrisons Principles of Internal Medicine
• Tension pneumothorax is a clinical not radiographic diag-nosis
characterized by unilateral decreased breath sounds, unilateral chest
hyperresonance, and tracheal deviation in the setting of respiratory
distress and shock. Treatment is immediate needle decompression
followed by chest tube thoracostomy placement.
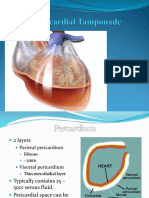
• Pericardial tamponade likewise should be considered early in the
evaluation of undifferentiated shock. Patients with blunt or penetrating
chest trauma can rapidly de-compensate with minimal bleeding into the
pericardium, while those with uremia and cancer usually develop an
effusion over time. Symptoms include hypotension, elevated right side
pressures (JVD) pulsus paradoxus (a fall in systolic blood pressure in
inspiration), and Kussmaul’s sign (increased jugular venous pressure on
inspiration). Bedside U/S is extremely sensitive in detecting pericardial
fluid and can be instrumental in guiding pericardiocentesis, although in
the patient in extremis, blind pericardiocentesis might be lifesaving
CURRENT Lange Diagnosis & Treatment Emergency
Medicine
• Massive PE presents as chest pain, syncope, tachypnea, and
hypotension with signs of acute right ventricular overload with JVD
and ECG changes. Fluid administration might worsen right ventricular
failure and should be given only cautiously. Blood pressure should be
augmented with an appropriate vasopressor such as norepinephrine
0.5–1 μg/min titrated to response. Immediate surgical embolectomy
is sometimes effective but not usually feasible. Shock complicating PE
is an indication for thrombolytics if no other contraindication exists.
CURRENT Lange Diagnosis & Treatment Emergency
Medicine
Treatment Obstructive Shock
• Cardiac Tamponade
Administer 1-2 L of normal saline followed by emergent bedside pericardiocentesis.
Perform an emergency department thoracotomy in patients with penetrating thoracic
trauma who fail to respond.
• Pulmonary Embolism
Administer small boluses of normal saline (250-500 mL) followed by vasopressor
support in unstable patients. Fibrinolysis is the treatment of choice for massive PE
presenting with profound hypotension (MAP <60), severe refractive hypoxemia (Sp02
<90 despite supplemental 02), or cardiac arrest.
• Tension Pneumothorax
Administer 1-2 L of normal saline while performing emergent needle thoracostomy
followed by chest tube placement.
Lange Clinical Emergency Medicine
You might also like
- ECG Mastery Yellow Belt WorkbookDocument118 pagesECG Mastery Yellow Belt WorkbookOana Anghel100% (9)
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Hasil Ujian KKD Mengenaal Sel Daan Hitung Jenis Blok Hematologi 2021Document9 pagesHasil Ujian KKD Mengenaal Sel Daan Hitung Jenis Blok Hematologi 2021Mohammad Jofa Rachman PNo ratings yet
- Dental Care For Patients With Heart Failure: An UpdateDocument9 pagesDental Care For Patients With Heart Failure: An UpdateGustavo A OrtegonNo ratings yet
- AirwayDocument25 pagesAirwayKURIMAONGNo ratings yet
- Valvular Heart Disease To TW FinalDocument13 pagesValvular Heart Disease To TW FinalMohammed ElSayedNo ratings yet
- Valvular Heart DiseseDocument41 pagesValvular Heart DisesefadhiliNo ratings yet
- Pathophysiology: Cardiovascular System Dr. Maen DweikDocument38 pagesPathophysiology: Cardiovascular System Dr. Maen DweikshoibyNo ratings yet
- ShockDocument14 pagesShockNatia UtmelidzeNo ratings yet
- AnginaDocument37 pagesAnginaSHAHALOMGIR AHMEDNo ratings yet
- Cardiovascular Disease and Anaesthesia: HypertensionDocument4 pagesCardiovascular Disease and Anaesthesia: Hypertensionsatria wibawaNo ratings yet
- Kardiogenik SyokDocument43 pagesKardiogenik SyokGalih Arief Harimurti WawolumajaNo ratings yet
- SHOCKDocument17 pagesSHOCKChithra Saju100% (1)
- Hypertrophic CardiomyopathyDocument32 pagesHypertrophic CardiomyopathyAbnet WondimuNo ratings yet
- Cardiac Tamponade (P)Document16 pagesCardiac Tamponade (P)CloudySkyNo ratings yet
- The Emergency ManagementDocument12 pagesThe Emergency ManagementWidya Surya AvantiNo ratings yet
- ShockDocument19 pagesShockasmyr6975No ratings yet
- AclsDocument4 pagesAclsAnusha Verghese100% (1)
- Management of The Patients WithDocument68 pagesManagement of The Patients WithДіна ШоріковаNo ratings yet
- Study Notes Emergency MedicineDocument12 pagesStudy Notes Emergency MedicineMedShare57% (7)
- Cardiogenic ShockDocument49 pagesCardiogenic Shockmaibejose0% (1)
- Cardiovascular DiseasesDocument67 pagesCardiovascular DiseasesokaciaNo ratings yet
- Patofisiologi Shock CardiogenicDocument44 pagesPatofisiologi Shock CardiogenicGalih Arief Harimurti Wawolumaja100% (1)
- Congestive Heart FailureDocument6 pagesCongestive Heart Failureseigelystic100% (1)
- Valvular Heart DiseasesDocument60 pagesValvular Heart DiseasesEthiopia TekdemNo ratings yet
- Cardiology Review SessionDocument139 pagesCardiology Review SessionNour LakisNo ratings yet
- Tetrology of Fallot 2Document25 pagesTetrology of Fallot 2KV18 KK5No ratings yet
- Structural Infectious and Inflammatory Cardiac Disorders and Medical ManagementDocument85 pagesStructural Infectious and Inflammatory Cardiac Disorders and Medical Managementmoncalshareen3No ratings yet
- Cardiac Tamponade and ManagementDocument42 pagesCardiac Tamponade and Managementأم حمدNo ratings yet
- Acute HF-IAIDocument49 pagesAcute HF-IAIAndita ListyannisaNo ratings yet
- PulmonaryDocument3 pagesPulmonaryBaha'aeddin HammadNo ratings yet
- ADHF Up To DateDocument25 pagesADHF Up To DateAndreas Agung KurniawanNo ratings yet
- Hemodynamic Unstable Patient Following ArrhythmiaDocument30 pagesHemodynamic Unstable Patient Following Arrhythmialew chin hongNo ratings yet
- CSS - Advanced Life SupportDocument16 pagesCSS - Advanced Life SupportnrahmaNo ratings yet
- Shock With Jugular Venous Distention: Clinical Review ArticleDocument9 pagesShock With Jugular Venous Distention: Clinical Review ArticlenevmerkaNo ratings yet
- Cardiogenic ShockDocument29 pagesCardiogenic ShockagnescheruseryNo ratings yet
- Pemicu 6 KGD DeniseDocument95 pagesPemicu 6 KGD DeniseVincent VandestyoNo ratings yet
- Myocarditis - PericarditisDocument21 pagesMyocarditis - PericarditisMahesh RathnayakeNo ratings yet
- Fluid Resuscitation in Haemorrhagic ShockDocument9 pagesFluid Resuscitation in Haemorrhagic ShockbashiruaminuNo ratings yet
- Unit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructureDocument37 pagesUnit 4 Coronary Artery Disease and Ischaemic Heart Disease: StructurebtaleraNo ratings yet
- 3 - Valvular Heart DiseasesDocument31 pages3 - Valvular Heart DiseasesLobna ElkilanyNo ratings yet
- Cardiac EmergencyDocument56 pagesCardiac Emergency21rayhanf100% (1)
- Cardiac TamponadeDocument29 pagesCardiac Tamponadeanimesh pandaNo ratings yet
- 3 Three - Mitral RegurgeDocument23 pages3 Three - Mitral Regurgeمحمد بن الصادقNo ratings yet
- Cardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityDocument35 pagesCardiac Tamponade: Pankaj Singh Rana Nurse Practitioner in Critical Care Swami Rama Himalayan UniversityBarlonga Yhan YogaNo ratings yet
- Case 5Document16 pagesCase 5Hany ElbarougyNo ratings yet
- STROKEDocument6 pagesSTROKEOxy GenNo ratings yet
- Thyroid StormDocument6 pagesThyroid StormCristina CenturionNo ratings yet
- Medical Surgery-2Document10 pagesMedical Surgery-2Wanjiku NderituNo ratings yet
- Model Answer -I & II سبتمبر 2015تحريريDocument12 pagesModel Answer -I & II سبتمبر 2015تحريريAmr El TaherNo ratings yet
- DR Ali Cardiology-MergedDocument684 pagesDR Ali Cardiology-MergedK PradhanNo ratings yet
- Media 115008 en PDFDocument12 pagesMedia 115008 en PDFsukandeNo ratings yet
- Cardiogenic Shock: Submitted ToDocument5 pagesCardiogenic Shock: Submitted Toal-obinay shereenNo ratings yet
- Topic:: Unstable AnginaDocument44 pagesTopic:: Unstable AnginaApurba100% (1)
- Medicine Osce Compiled and Solved - EcgsDocument46 pagesMedicine Osce Compiled and Solved - EcgsamashooquekubarNo ratings yet
- Intra Operative Considerations in Mitral Stenosis Patient: Salil MaheshwariDocument26 pagesIntra Operative Considerations in Mitral Stenosis Patient: Salil MaheshwarisalilNo ratings yet
- Cardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarDocument23 pagesCardiac Tamponade: Mrs. D.Melba Sahaya Sweety.D M.SC Nursing GimsarD. Melba S.S ChinnaNo ratings yet
- CardioDocument9 pagesCardioVirgilio Reyes ManuelNo ratings yet
- 9 CsaDocument34 pages9 Csaمحمد بن الصادقNo ratings yet
- Critical Care in The Emergency Department: Shock and Circulatory SupportDocument10 pagesCritical Care in The Emergency Department: Shock and Circulatory SupportKhaled AbdoNo ratings yet
- Acute Coronary SyndromeDocument93 pagesAcute Coronary SyndromeissareinoNo ratings yet
- Cardiac TemponadeDocument18 pagesCardiac TemponadeDIVYA GANGWAR100% (1)
- CH 46 Complications of AnaesthesiaDocument29 pagesCH 46 Complications of AnaesthesiaChristian LeepoNo ratings yet
- Cardiac Tamponade (Suryani)Document72 pagesCardiac Tamponade (Suryani)Hamdani UsmanNo ratings yet
- John 2016Document3 pagesJohn 2016Mohammad Jofa Rachman PNo ratings yet
- Seizure Focal SeizuresDocument8 pagesSeizure Focal SeizuresMohammad Jofa Rachman PNo ratings yet
- Mel Zack 1975Document23 pagesMel Zack 1975Mohammad Jofa Rachman PNo ratings yet
- First Problem: Friday, 24 September 2021 Group 19 - 20Document69 pagesFirst Problem: Friday, 24 September 2021 Group 19 - 20Mohammad Jofa Rachman PNo ratings yet
- 19-20 Second ProblemDocument108 pages19-20 Second ProblemMohammad Jofa Rachman PNo ratings yet
- Seminar IDAI Protein Intake To Support Immune System Children With Allergy Disease PDFDocument39 pagesSeminar IDAI Protein Intake To Support Immune System Children With Allergy Disease PDFMohammad Jofa Rachman PNo ratings yet
- Tropical Fevers: C. Important Human Parasitic Fevers of The TropicsDocument25 pagesTropical Fevers: C. Important Human Parasitic Fevers of The TropicsMohammad Jofa Rachman PNo ratings yet
- Tabel Origo-Insersi Myologi (Ex. Superio & Inferior)Document8 pagesTabel Origo-Insersi Myologi (Ex. Superio & Inferior)Mohammad Jofa Rachman PNo ratings yet
- Tabel KinesiologiDocument4 pagesTabel KinesiologiMohammad Jofa Rachman PNo ratings yet
- PROBLEM 3 GIT Jeffrey 405170048Document162 pagesPROBLEM 3 GIT Jeffrey 405170048Mohammad Jofa Rachman PNo ratings yet
- Absensi Kakak Asuh 2020-2021 Fixxx PDFDocument7 pagesAbsensi Kakak Asuh 2020-2021 Fixxx PDFMohammad Jofa Rachman PNo ratings yet
- Yellowish Lesions of The Oral Cavity. Suggestion For A ClassificationDocument6 pagesYellowish Lesions of The Oral Cavity. Suggestion For A ClassificationMohammad Jofa Rachman PNo ratings yet
- Anatomi Abdominal, Viscera Abdomen Dan Regio AbdominalesDocument15 pagesAnatomi Abdominal, Viscera Abdomen Dan Regio AbdominalesMohammad Jofa Rachman PNo ratings yet
- Rangkuman CCS 1Document16 pagesRangkuman CCS 1Tesis Maruli Tua SianiparNo ratings yet
- Lesson 1 - Disease and InfectionDocument28 pagesLesson 1 - Disease and InfectionJohn Raiel OlarteNo ratings yet
- Pediatric Nursing: Prepared By: Adahlia T. Basco RN, MANDocument226 pagesPediatric Nursing: Prepared By: Adahlia T. Basco RN, MANMika SamsonNo ratings yet
- How To Measure Blood Pressure Using A SphygmomanometerDocument3 pagesHow To Measure Blood Pressure Using A SphygmomanometerpadritovechioNo ratings yet
- CURS 5 Abnormalities of The Umbilical Cord and Amniotic FluidDocument33 pagesCURS 5 Abnormalities of The Umbilical Cord and Amniotic FluidFayad AlmohamedNo ratings yet
- Emergency and Critical Care Procedures in Small AnimalsDocument9 pagesEmergency and Critical Care Procedures in Small AnimalsTessaNo ratings yet
- Anatomy and Physiology Veins of The Lower LimbsDocument3 pagesAnatomy and Physiology Veins of The Lower LimbsRoel John Atamosa CasilacNo ratings yet
- Chapter 21 AddqDocument12 pagesChapter 21 AddqLenel John Giban Bagunas100% (1)
- Genetics NotesDocument15 pagesGenetics NotesIshtiaque KhanNo ratings yet
- Management of Pregnancy at RiskDocument40 pagesManagement of Pregnancy at RiskMA. JYRELL BONITONo ratings yet
- Blood Gases and Acid-Base BalanceDocument11 pagesBlood Gases and Acid-Base BalanceREMAN ALINGASANo ratings yet
- 8 High Blood Pressure TreatmentDocument4 pages8 High Blood Pressure TreatmentMuhammad Talha AttariNo ratings yet
- Cambridge Checkpoint Notes ExcretionDocument3 pagesCambridge Checkpoint Notes Excretionanimemaster2kNo ratings yet
- Normal Fetal Growth and DevelopmentDocument38 pagesNormal Fetal Growth and DevelopmentArhum SiddiqiNo ratings yet
- Ainul Haq Report 2Document27 pagesAinul Haq Report 2Mohd AliNo ratings yet
- PDF Reyes Christine Mae DDDocument23 pagesPDF Reyes Christine Mae DDmelodia gandezaNo ratings yet
- History Taking and Ce of Cardiac PatientsDocument89 pagesHistory Taking and Ce of Cardiac Patientsapi-3858544100% (1)
- Complication of Dentoalveolar SurgeryDocument21 pagesComplication of Dentoalveolar Surgerywhussien7376No ratings yet
- Blumenfeld Neuroanatomy Ch. 5 SummaryDocument5 pagesBlumenfeld Neuroanatomy Ch. 5 SummaryMeeraNo ratings yet
- Congestive Heart Failure (PH 2 Bemdiji)Document1 pageCongestive Heart Failure (PH 2 Bemdiji)api-285694335No ratings yet
- Drug Study Atropine SulfateDocument1 pageDrug Study Atropine Sulfateirhizzp75% (8)
- DR Ahlquist - 0 - 0Document20 pagesDR Ahlquist - 0 - 0jinhan.chiengNo ratings yet
- Dihydrotestosterone (DHT) - DHT Stimulates Cell Growth in The Tissue That Lines The Prostate GlandDocument7 pagesDihydrotestosterone (DHT) - DHT Stimulates Cell Growth in The Tissue That Lines The Prostate GlandPeter Kenneth LampitocNo ratings yet
- ECG Interpretation For ACLSDocument27 pagesECG Interpretation For ACLSZH. omg sarNo ratings yet
- Radiology 165 3 3317501Document4 pagesRadiology 165 3 3317501Dzulfachri KurniawanNo ratings yet
- Chapter22 Assessment of Pheripheral Vascular SystemDocument33 pagesChapter22 Assessment of Pheripheral Vascular SystemMARY ANNE JUDE ANTHONYNo ratings yet
- What Is Hypertension? 6 Ways To Prevent HypertensionDocument3 pagesWhat Is Hypertension? 6 Ways To Prevent HypertensionAnastasya Gishella RorongNo ratings yet