Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
9 viewsShare Endokrinologi Reproduksi Pria
Share Endokrinologi Reproduksi Pria
Uploaded by
Brama AtmajaThis document summarizes the hormonal control of male reproductive endocrinology. It discusses how the hypothalamus regulates the pituitary to secrete LH and FSH, which then stimulate testosterone production and spermatogenesis in the testes. A feedback loop exists where testosterone inhibits LH and FSH secretion. FSH controls spermatogenesis quantitatively while testosterone does so qualitatively. Clinical evaluation involves assessing hormone levels to diagnose endocrine causes of issues like oligospermia or azoospermia. Overall it provides an overview of the hormonal regulation of male fertility and approaches to diagnosis.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Yr 9 PASS The Body in Action PowerpointDocument77 pagesYr 9 PASS The Body in Action PowerpointKellie GuestNo ratings yet
- 1,4) HPG and Physiology of AndrogensDocument46 pages1,4) HPG and Physiology of AndrogensBHUWAN BASKOTANo ratings yet
- TestosteronDocument31 pagesTestosteronDessy AmalinaNo ratings yet
- Male Reproduction SystemDocument22 pagesMale Reproduction SystemSalman KhanNo ratings yet
- Reproductive EndocrinologyDocument95 pagesReproductive EndocrinologySamuel BaidooNo ratings yet
- Male Sex Hormones FunctionsDocument18 pagesMale Sex Hormones FunctionsPermanand BheemsinNo ratings yet
- PPPPPPPTTTTTTTTTTTTTTDocument16 pagesPPPPPPPTTTTTTTTTTTTTTfaisal_gondal786No ratings yet
- Presentation. Lec 11. Animal and Function 2Document42 pagesPresentation. Lec 11. Animal and Function 2diolechiNo ratings yet
- The Menstrual Cycle: Dr. Milvan Hadi, M. Ked (Og), SpogDocument41 pagesThe Menstrual Cycle: Dr. Milvan Hadi, M. Ked (Og), SpogEvi Liana BahriahNo ratings yet
- Pituitary GlandDocument25 pagesPituitary GlandIshaqNo ratings yet
- Spermatogenesisvs OogenesisDocument96 pagesSpermatogenesisvs OogenesisZerica JohnNo ratings yet
- Ovarian CycleDocument78 pagesOvarian CyclefasicaregroupNo ratings yet
- Hormonal Control of Spermatogenesis: by Abhinav BhardwajDocument10 pagesHormonal Control of Spermatogenesis: by Abhinav Bhardwajarthurggg429No ratings yet
- Male Reproductive SystemDocument28 pagesMale Reproductive SystemIshaqNo ratings yet
- Hormonal Control of SpermatogenesisDocument10 pagesHormonal Control of Spermatogenesisarthurggg429No ratings yet
- Endocrine System: Clarence L. Nuval, RMT, MDDocument66 pagesEndocrine System: Clarence L. Nuval, RMT, MDCla NuvalNo ratings yet
- RS-1 K5-K6 Hormon Repro Pria Dan Wanita, EditDocument57 pagesRS-1 K5-K6 Hormon Repro Pria Dan Wanita, EditfelixNo ratings yet
- L3-4. PubertyDocument28 pagesL3-4. Pubertypyinsta7it2No ratings yet
- Reproductive Male & FemaleDocument115 pagesReproductive Male & Femalekhorrami4No ratings yet
- Lesson 1.2 The Endocrine System CompleteDocument71 pagesLesson 1.2 The Endocrine System CompletesoriamarheenakatrineNo ratings yet
- Male Feedback MechanismDocument2 pagesMale Feedback Mechanismnelsonalec049No ratings yet
- Hormonal BiochemistryDocument82 pagesHormonal BiochemistryRuthNo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemMikaella Viador100% (2)
- Reproductive BehaviorDocument37 pagesReproductive BehaviorDan MaliwatNo ratings yet
- 1st Lecture - Hypothalamus Pituitary Gonadal Axis - Reproductive PhysiologyDocument8 pages1st Lecture - Hypothalamus Pituitary Gonadal Axis - Reproductive PhysiologyBHUWAN BASKOTANo ratings yet
- Endocrine System AnatomyDocument41 pagesEndocrine System Anatomypizzyray640No ratings yet
- Regulasi Endokrin 22 IntensifDocument25 pagesRegulasi Endokrin 22 IntensifWignes WarenNo ratings yet
- Male Reproductive PhysiologyDocument16 pagesMale Reproductive PhysiologySri WahyuniNo ratings yet
- EndocrineDocument94 pagesEndocrineHira NawazNo ratings yet
- Endocrine System: Endocrine: Which Have No Duct and ReleaseDocument36 pagesEndocrine System: Endocrine: Which Have No Duct and Releasedr_saleh77No ratings yet
- Hypothalamus and PituitaryDocument60 pagesHypothalamus and Pituitarydhruvdesai24No ratings yet
- Chemical Co Ordination.Document11 pagesChemical Co Ordination.PAK BTS ARMYNo ratings yet
- Anfis TestisDocument4 pagesAnfis TestisNandia SeptiyoriniNo ratings yet
- Hypothalamic-Pituitary-Gonadal AxisDocument82 pagesHypothalamic-Pituitary-Gonadal AxisIiiNo ratings yet
- Male Reproductive PhysiologyDocument18 pagesMale Reproductive Physiologykushluv38No ratings yet
- Endocrine SystemDocument52 pagesEndocrine SystemDishani DeyNo ratings yet
- Hypothalamus & Pituitary GlandDocument39 pagesHypothalamus & Pituitary GlandVishal DodejaNo ratings yet
- Reproductive SystemDocument30 pagesReproductive SystemmfaizchejamriNo ratings yet
- Anatomy Indocrine SystemsDocument59 pagesAnatomy Indocrine SystemsibrooavcNo ratings yet
- Reproductive System Biochemistry by ShahidDocument5 pagesReproductive System Biochemistry by ShahidSHAHIDNo ratings yet
- Hormones in Reproduction: Presented To: Dr. Akhtar Rasool Presented By: M Tayyab 2012-VA-300Document17 pagesHormones in Reproduction: Presented To: Dr. Akhtar Rasool Presented By: M Tayyab 2012-VA-300javeria choudharyNo ratings yet
- Hypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanDocument33 pagesHypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanherlinaNo ratings yet
- Endocrine PhysiologyDocument98 pagesEndocrine PhysiologyMohan GuptaNo ratings yet
- Hypothalamus, Pituitary, Thyroid & Parathyroid Glands-3Document70 pagesHypothalamus, Pituitary, Thyroid & Parathyroid Glands-3Benard NyaumaNo ratings yet
- 1 - HPG AxisDocument21 pages1 - HPG AxisBHUWAN BASKOTANo ratings yet
- 4 Male Reproductive SystemDocument19 pages4 Male Reproductive SystemaprilNo ratings yet
- EndocrinologyDocument136 pagesEndocrinologyShiela Torres100% (9)
- Ujjjju43ut3t3j3 I9Document3 pagesUjjjju43ut3t3j3 I9Ioana Maria DănilăNo ratings yet
- Endocrine GlandsDocument36 pagesEndocrine GlandsnasyitahnorzlanNo ratings yet
- Functional Anatomy of The Hypothalamicpituitarygonadal Axis andDocument10 pagesFunctional Anatomy of The Hypothalamicpituitarygonadal Axis andEvaNo ratings yet
- Hormones: Mark Angelo R. Jacosalem Faye Bernadette O. Reyes Ma. Elizabeth VerteraDocument40 pagesHormones: Mark Angelo R. Jacosalem Faye Bernadette O. Reyes Ma. Elizabeth VerteraGelo Robin JacosalemNo ratings yet
- CC2 SemifinalsDocument4 pagesCC2 SemifinalsAbc DefNo ratings yet
- Endocrinology Endocrinology: H. KibichoDocument370 pagesEndocrinology Endocrinology: H. KibichoMursal RashidNo ratings yet
- Human Preproduction Master CopyDocument72 pagesHuman Preproduction Master CopyShalini JhaNo ratings yet
- PD22 Hap1 L03Document33 pagesPD22 Hap1 L03Ka Yan LAUNo ratings yet
- EndocrinologyDocument74 pagesEndocrinologysyedahaleemajunaidsNo ratings yet
- HPG Axis:: A) in FemalesDocument5 pagesHPG Axis:: A) in FemalesHanan Al-HarthiNo ratings yet
- Male Reproduction: by Khairun NisaDocument4 pagesMale Reproduction: by Khairun NisaKurnia Fitri AprillianaNo ratings yet
- Hormones of The Reproductive SystemDocument9 pagesHormones of The Reproductive Systemkarthickmech1987No ratings yet
- Menstrual CyclelatestDocument27 pagesMenstrual Cyclelatestmamai elijahNo ratings yet
- DR - Purnabawa - Diagnosis - Terapi Ruptur PerineumDocument53 pagesDR - Purnabawa - Diagnosis - Terapi Ruptur PerineumBrama AtmajaNo ratings yet
- Dr. Shyam Babu Prasad: Course Code: ZOOL 4008 (Biochemistry and Metabolism)Document17 pagesDr. Shyam Babu Prasad: Course Code: ZOOL 4008 (Biochemistry and Metabolism)Brama AtmajaNo ratings yet
- HHS Public Access: HypothyroidismDocument27 pagesHHS Public Access: HypothyroidismBrama AtmajaNo ratings yet
- Obat Pada Bayi Dan AnakDocument47 pagesObat Pada Bayi Dan AnakBrama AtmajaNo ratings yet
- Biofilm in OtorhinolaryngologyDocument10 pagesBiofilm in OtorhinolaryngologyMohammed SahibNo ratings yet
- G11 - Third Term Examination (2020) - Leeds International SchoolDocument20 pagesG11 - Third Term Examination (2020) - Leeds International SchoolXiao ShadowlordNo ratings yet
- PunnettsquaresworksheetDocument3 pagesPunnettsquaresworksheetapi-346309092No ratings yet
- THEORYDocument32 pagesTHEORYKenneth PatronNo ratings yet
- AEX 102-Fundamentals of Agricultural Extension Education (2+1)Document14 pagesAEX 102-Fundamentals of Agricultural Extension Education (2+1)Sneha ThillaigovindhanNo ratings yet
- Virology MCQDocument62 pagesVirology MCQGazi Shahinur Akter ShampaNo ratings yet
- Objective Questions: Table 1Document9 pagesObjective Questions: Table 1LAKIESHA100% (1)
- Effect of Feeding Larvae To Nymph Cantheconidea FurcellataDocument4 pagesEffect of Feeding Larvae To Nymph Cantheconidea FurcellataEvawaty Sri UlinaNo ratings yet
- Abstracts - 2024 Ilafs ConferenceDocument30 pagesAbstracts - 2024 Ilafs Conferenceapi-237412703No ratings yet
- Card SortDocument11 pagesCard SortNellyRdzNo ratings yet
- Essentials of Molecular Genetics: January 2015Document24 pagesEssentials of Molecular Genetics: January 2015lavomo-simangoNo ratings yet
- Community Ecology by Gary G. Mittelbach: The Quarterly Review of Biology January 2013Document4 pagesCommunity Ecology by Gary G. Mittelbach: The Quarterly Review of Biology January 2013MonicaNo ratings yet
- Chiang 2016Document313 pagesChiang 2016Anil KumarNo ratings yet
- Carbohydrate Metabolism in Dairy CowsDocument4 pagesCarbohydrate Metabolism in Dairy CowsEduardo Bonilha100% (2)
- Grsmu - Byfilesfileuniversitycafedrynevrologiifileslfklin Protokol PDFDocument197 pagesGrsmu - Byfilesfileuniversitycafedrynevrologiifileslfklin Protokol PDFАнна ФоменкоNo ratings yet
- CHT WFLH Boys Z 0 5Document1 pageCHT WFLH Boys Z 0 5suciNo ratings yet
- CSI Wildlife: Analyzing Genetic EvidenceDocument4 pagesCSI Wildlife: Analyzing Genetic EvidenceInsaf MNo ratings yet
- Chapter 10 Classification of Living and Non-Living ThingsDocument11 pagesChapter 10 Classification of Living and Non-Living ThingsJulius MacaballugNo ratings yet
- Biomedical Engineering Graduate Concentrations: Advisor: Prof. Tim BrunsDocument8 pagesBiomedical Engineering Graduate Concentrations: Advisor: Prof. Tim BrunsDelfina HuangNo ratings yet
- UPSC IFS Zoology SyllabusDocument4 pagesUPSC IFS Zoology SyllabusAntar InenigogNo ratings yet
- Beauty - A-Solute Skincare R1Document39 pagesBeauty - A-Solute Skincare R1Rabby ChowdhuryNo ratings yet
- Human Reproduction: Points To RememberDocument9 pagesHuman Reproduction: Points To RememberPREM277272No ratings yet
- The Flowering Plants Handbook SampleDocument26 pagesThe Flowering Plants Handbook SampleClaramaria RodriguezNo ratings yet
- Egg Depositor of Ornamental FishesDocument4 pagesEgg Depositor of Ornamental FishesPieter SteenkampNo ratings yet
- IJOMRDocument11 pagesIJOMRDharmendra ThakurNo ratings yet
- Toksi PerilakuDocument52 pagesToksi PerilakuseptianasptrNo ratings yet
- Bioinformatic CoursesDocument2 pagesBioinformatic Coursesdenilw100% (1)
- Republic of The Philippines Province of RizalDocument4 pagesRepublic of The Philippines Province of RizalPearl Joy FrancoNo ratings yet
- Nucleotide Metabolism VivaDocument12 pagesNucleotide Metabolism Vivaallswell addoNo ratings yet
Share Endokrinologi Reproduksi Pria
Share Endokrinologi Reproduksi Pria
Uploaded by
Brama Atmaja0 ratings0% found this document useful (0 votes)
9 views24 pagesThis document summarizes the hormonal control of male reproductive endocrinology. It discusses how the hypothalamus regulates the pituitary to secrete LH and FSH, which then stimulate testosterone production and spermatogenesis in the testes. A feedback loop exists where testosterone inhibits LH and FSH secretion. FSH controls spermatogenesis quantitatively while testosterone does so qualitatively. Clinical evaluation involves assessing hormone levels to diagnose endocrine causes of issues like oligospermia or azoospermia. Overall it provides an overview of the hormonal regulation of male fertility and approaches to diagnosis.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes the hormonal control of male reproductive endocrinology. It discusses how the hypothalamus regulates the pituitary to secrete LH and FSH, which then stimulate testosterone production and spermatogenesis in the testes. A feedback loop exists where testosterone inhibits LH and FSH secretion. FSH controls spermatogenesis quantitatively while testosterone does so qualitatively. Clinical evaluation involves assessing hormone levels to diagnose endocrine causes of issues like oligospermia or azoospermia. Overall it provides an overview of the hormonal regulation of male fertility and approaches to diagnosis.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
9 views24 pagesShare Endokrinologi Reproduksi Pria
Share Endokrinologi Reproduksi Pria
Uploaded by
Brama AtmajaThis document summarizes the hormonal control of male reproductive endocrinology. It discusses how the hypothalamus regulates the pituitary to secrete LH and FSH, which then stimulate testosterone production and spermatogenesis in the testes. A feedback loop exists where testosterone inhibits LH and FSH secretion. FSH controls spermatogenesis quantitatively while testosterone does so qualitatively. Clinical evaluation involves assessing hormone levels to diagnose endocrine causes of issues like oligospermia or azoospermia. Overall it provides an overview of the hormonal regulation of male fertility and approaches to diagnosis.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 24
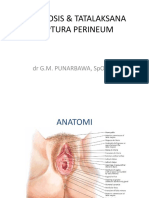
Endokrinologi Reproduksi Pria
Gede Wira Buanayuda
(Fakultas Kedokteran Universitas
Mataram)
Hypothalamus
• Receives neural input from many brain centers
and is the pulse generator for the cyclical
secretion of pituitary and gonadal hormones
• GnRH
synthesis and release of both gonadotropic
hormones,LH and FSH
Pulsatile : 1 pulse every 70 to 90 min
very short half-life in the blood of approx 2 to 5
min
ANTERIOR PITUITARY
• LH and FSH
• regulate testicular function
• secreted in an episodic manner
• FSH : longer half-life
• LH : rapidly metabolized
TESTES
• 2 fungsi : spermatogenesis, steroidogenesis
(sintesis androgens)
• LH melekat pada reseptor membran Sel leydig
testosteron
• FSH melekat pada reseptor membran sel
sertoli sintesis ABP (androgen binding
protein, inhibin, inisiasi spermatogenesis)
Kontrol Umpanbalik
• LH
• testosterone—is a primary inhibitor of LH
secretion in men
• Estrogens also inhibit LH secretion
• FSH
• both testosterone and estradiol are capable of
suppressing FSH serum levels
• Inhibin produced by the Sertoli cells of the testes
suppressing FSH release.
PROLACTIN AND GONADOTROPINS
• Hyperprolactinemia
• inhibit GnRH secretion directly
• Excessive prolactin may affect sexual functions
by having a direct effect on the central nervous
system and also from inhibition of androgen
secretion
• Bromocriptine, a dopamine agonist with
prolactin-lowering activities, improves sexual
function
ANDROGEN PHYSIOLOGY
• regulate gonadotropin secretion
• initiation and maintenance of
spermatogenesis
• formation of male phenotype during sexual
differentiation
• promotion of sexual maturation at puberty
• controlling sexual drive and potency
• In normal males
• 2% of testosterone is
free (unbound), 44% is
terikat kuat “sex
hormone-binding
globulin” (SHBG), sisanya
terikat ke albumin
• Free- and albumin-
bound portions
bioavailable testosterone
HORMONAL CONTROL OF
SPERMATOGENESIS
• Spermatogenesis is primarily controlled by the
gonadotropins—FSH and LH.
FSH
LH LC
SC
T ABP
Qualitative sperm production can be achieved by
replacement of either FSH or LH alone
both FSH and LH are necessary
to maintain quantitative normal spermatogenesis in humans
Initiation and maintenance of
spermatogenesis
• T & FSH SC (SINERGISTIK)
• Testosterone
Qualitatively will initiate and maintain spermatogenesis
in humans
• FSH
necessary for the maintenance of quantitatively normal
sperm production
initiating spermatogenesis in pubertal males and
reinitiating spermatogenesis in men whose germinal
epithelium has regressed after hypophysectomy
Spermatogenesis
• 3 TAHAP
SPERMATOSITOGENESIS
Mulai dari spermatogonium s/d spermatosit
primer.
MEIOSIS
Pembelahan reduki (meiosis) 2X, pd
spermatosit primer spermatosit sekunder
terbentuk spermatid.
SPERMIOGENESIS
Transformasi spermatid menjadi spermatozoon.
SPERMIOGENESIS
SPERMIASI
• PELEPASAN SPERMATOZOA DARI SEL SERTOLI
MEMASUKI LUMEN TUBULUS SEMINIFERUS.
• SPERMATOZOA INI SECARA MORPHOLOGIS
SUDAH MATANG, TETAPI SECARA
FUNGSIONAL.
Aspek klinis
• History
• Pemeriksaan pisik
• Evaluasi hormonal
diagnosis of endocrine causes
• Severe oligo/Azoospermia FSH, LH, T
• N T, N LH, N FSH : Nonendocrine
• T , LH , FSH : Primary testiscular failure
(Hipergonadotrophic-hipogonadism)
• T , LH , FSH : Secondary testiscular failure
(Hipogonadotrophic-hipogonadism)
• N T ,N LH , FSH : Isolated Germ Cell Failure
• T , LH , N FSH : Androgen Resistance
diagnosis of endocrine causes
• Hyperprolactinemia
• Libido , ED , T , Prol
Contoh Kasus
tks
You might also like
- Yr 9 PASS The Body in Action PowerpointDocument77 pagesYr 9 PASS The Body in Action PowerpointKellie GuestNo ratings yet
- 1,4) HPG and Physiology of AndrogensDocument46 pages1,4) HPG and Physiology of AndrogensBHUWAN BASKOTANo ratings yet
- TestosteronDocument31 pagesTestosteronDessy AmalinaNo ratings yet
- Male Reproduction SystemDocument22 pagesMale Reproduction SystemSalman KhanNo ratings yet
- Reproductive EndocrinologyDocument95 pagesReproductive EndocrinologySamuel BaidooNo ratings yet
- Male Sex Hormones FunctionsDocument18 pagesMale Sex Hormones FunctionsPermanand BheemsinNo ratings yet
- PPPPPPPTTTTTTTTTTTTTTDocument16 pagesPPPPPPPTTTTTTTTTTTTTTfaisal_gondal786No ratings yet
- Presentation. Lec 11. Animal and Function 2Document42 pagesPresentation. Lec 11. Animal and Function 2diolechiNo ratings yet
- The Menstrual Cycle: Dr. Milvan Hadi, M. Ked (Og), SpogDocument41 pagesThe Menstrual Cycle: Dr. Milvan Hadi, M. Ked (Og), SpogEvi Liana BahriahNo ratings yet
- Pituitary GlandDocument25 pagesPituitary GlandIshaqNo ratings yet
- Spermatogenesisvs OogenesisDocument96 pagesSpermatogenesisvs OogenesisZerica JohnNo ratings yet
- Ovarian CycleDocument78 pagesOvarian CyclefasicaregroupNo ratings yet
- Hormonal Control of Spermatogenesis: by Abhinav BhardwajDocument10 pagesHormonal Control of Spermatogenesis: by Abhinav Bhardwajarthurggg429No ratings yet
- Male Reproductive SystemDocument28 pagesMale Reproductive SystemIshaqNo ratings yet
- Hormonal Control of SpermatogenesisDocument10 pagesHormonal Control of Spermatogenesisarthurggg429No ratings yet
- Endocrine System: Clarence L. Nuval, RMT, MDDocument66 pagesEndocrine System: Clarence L. Nuval, RMT, MDCla NuvalNo ratings yet
- RS-1 K5-K6 Hormon Repro Pria Dan Wanita, EditDocument57 pagesRS-1 K5-K6 Hormon Repro Pria Dan Wanita, EditfelixNo ratings yet
- L3-4. PubertyDocument28 pagesL3-4. Pubertypyinsta7it2No ratings yet
- Reproductive Male & FemaleDocument115 pagesReproductive Male & Femalekhorrami4No ratings yet
- Lesson 1.2 The Endocrine System CompleteDocument71 pagesLesson 1.2 The Endocrine System CompletesoriamarheenakatrineNo ratings yet
- Male Feedback MechanismDocument2 pagesMale Feedback Mechanismnelsonalec049No ratings yet
- Hormonal BiochemistryDocument82 pagesHormonal BiochemistryRuthNo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemMikaella Viador100% (2)
- Reproductive BehaviorDocument37 pagesReproductive BehaviorDan MaliwatNo ratings yet
- 1st Lecture - Hypothalamus Pituitary Gonadal Axis - Reproductive PhysiologyDocument8 pages1st Lecture - Hypothalamus Pituitary Gonadal Axis - Reproductive PhysiologyBHUWAN BASKOTANo ratings yet
- Endocrine System AnatomyDocument41 pagesEndocrine System Anatomypizzyray640No ratings yet
- Regulasi Endokrin 22 IntensifDocument25 pagesRegulasi Endokrin 22 IntensifWignes WarenNo ratings yet
- Male Reproductive PhysiologyDocument16 pagesMale Reproductive PhysiologySri WahyuniNo ratings yet
- EndocrineDocument94 pagesEndocrineHira NawazNo ratings yet
- Endocrine System: Endocrine: Which Have No Duct and ReleaseDocument36 pagesEndocrine System: Endocrine: Which Have No Duct and Releasedr_saleh77No ratings yet
- Hypothalamus and PituitaryDocument60 pagesHypothalamus and Pituitarydhruvdesai24No ratings yet
- Chemical Co Ordination.Document11 pagesChemical Co Ordination.PAK BTS ARMYNo ratings yet
- Anfis TestisDocument4 pagesAnfis TestisNandia SeptiyoriniNo ratings yet
- Hypothalamic-Pituitary-Gonadal AxisDocument82 pagesHypothalamic-Pituitary-Gonadal AxisIiiNo ratings yet
- Male Reproductive PhysiologyDocument18 pagesMale Reproductive Physiologykushluv38No ratings yet
- Endocrine SystemDocument52 pagesEndocrine SystemDishani DeyNo ratings yet
- Hypothalamus & Pituitary GlandDocument39 pagesHypothalamus & Pituitary GlandVishal DodejaNo ratings yet
- Reproductive SystemDocument30 pagesReproductive SystemmfaizchejamriNo ratings yet
- Anatomy Indocrine SystemsDocument59 pagesAnatomy Indocrine SystemsibrooavcNo ratings yet
- Reproductive System Biochemistry by ShahidDocument5 pagesReproductive System Biochemistry by ShahidSHAHIDNo ratings yet
- Hormones in Reproduction: Presented To: Dr. Akhtar Rasool Presented By: M Tayyab 2012-VA-300Document17 pagesHormones in Reproduction: Presented To: Dr. Akhtar Rasool Presented By: M Tayyab 2012-VA-300javeria choudharyNo ratings yet
- Hypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanDocument33 pagesHypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanherlinaNo ratings yet
- Endocrine PhysiologyDocument98 pagesEndocrine PhysiologyMohan GuptaNo ratings yet
- Hypothalamus, Pituitary, Thyroid & Parathyroid Glands-3Document70 pagesHypothalamus, Pituitary, Thyroid & Parathyroid Glands-3Benard NyaumaNo ratings yet
- 1 - HPG AxisDocument21 pages1 - HPG AxisBHUWAN BASKOTANo ratings yet
- 4 Male Reproductive SystemDocument19 pages4 Male Reproductive SystemaprilNo ratings yet
- EndocrinologyDocument136 pagesEndocrinologyShiela Torres100% (9)
- Ujjjju43ut3t3j3 I9Document3 pagesUjjjju43ut3t3j3 I9Ioana Maria DănilăNo ratings yet
- Endocrine GlandsDocument36 pagesEndocrine GlandsnasyitahnorzlanNo ratings yet
- Functional Anatomy of The Hypothalamicpituitarygonadal Axis andDocument10 pagesFunctional Anatomy of The Hypothalamicpituitarygonadal Axis andEvaNo ratings yet
- Hormones: Mark Angelo R. Jacosalem Faye Bernadette O. Reyes Ma. Elizabeth VerteraDocument40 pagesHormones: Mark Angelo R. Jacosalem Faye Bernadette O. Reyes Ma. Elizabeth VerteraGelo Robin JacosalemNo ratings yet
- CC2 SemifinalsDocument4 pagesCC2 SemifinalsAbc DefNo ratings yet
- Endocrinology Endocrinology: H. KibichoDocument370 pagesEndocrinology Endocrinology: H. KibichoMursal RashidNo ratings yet
- Human Preproduction Master CopyDocument72 pagesHuman Preproduction Master CopyShalini JhaNo ratings yet
- PD22 Hap1 L03Document33 pagesPD22 Hap1 L03Ka Yan LAUNo ratings yet
- EndocrinologyDocument74 pagesEndocrinologysyedahaleemajunaidsNo ratings yet
- HPG Axis:: A) in FemalesDocument5 pagesHPG Axis:: A) in FemalesHanan Al-HarthiNo ratings yet
- Male Reproduction: by Khairun NisaDocument4 pagesMale Reproduction: by Khairun NisaKurnia Fitri AprillianaNo ratings yet
- Hormones of The Reproductive SystemDocument9 pagesHormones of The Reproductive Systemkarthickmech1987No ratings yet
- Menstrual CyclelatestDocument27 pagesMenstrual Cyclelatestmamai elijahNo ratings yet
- DR - Purnabawa - Diagnosis - Terapi Ruptur PerineumDocument53 pagesDR - Purnabawa - Diagnosis - Terapi Ruptur PerineumBrama AtmajaNo ratings yet
- Dr. Shyam Babu Prasad: Course Code: ZOOL 4008 (Biochemistry and Metabolism)Document17 pagesDr. Shyam Babu Prasad: Course Code: ZOOL 4008 (Biochemistry and Metabolism)Brama AtmajaNo ratings yet
- HHS Public Access: HypothyroidismDocument27 pagesHHS Public Access: HypothyroidismBrama AtmajaNo ratings yet
- Obat Pada Bayi Dan AnakDocument47 pagesObat Pada Bayi Dan AnakBrama AtmajaNo ratings yet
- Biofilm in OtorhinolaryngologyDocument10 pagesBiofilm in OtorhinolaryngologyMohammed SahibNo ratings yet
- G11 - Third Term Examination (2020) - Leeds International SchoolDocument20 pagesG11 - Third Term Examination (2020) - Leeds International SchoolXiao ShadowlordNo ratings yet
- PunnettsquaresworksheetDocument3 pagesPunnettsquaresworksheetapi-346309092No ratings yet
- THEORYDocument32 pagesTHEORYKenneth PatronNo ratings yet
- AEX 102-Fundamentals of Agricultural Extension Education (2+1)Document14 pagesAEX 102-Fundamentals of Agricultural Extension Education (2+1)Sneha ThillaigovindhanNo ratings yet
- Virology MCQDocument62 pagesVirology MCQGazi Shahinur Akter ShampaNo ratings yet
- Objective Questions: Table 1Document9 pagesObjective Questions: Table 1LAKIESHA100% (1)
- Effect of Feeding Larvae To Nymph Cantheconidea FurcellataDocument4 pagesEffect of Feeding Larvae To Nymph Cantheconidea FurcellataEvawaty Sri UlinaNo ratings yet
- Abstracts - 2024 Ilafs ConferenceDocument30 pagesAbstracts - 2024 Ilafs Conferenceapi-237412703No ratings yet
- Card SortDocument11 pagesCard SortNellyRdzNo ratings yet
- Essentials of Molecular Genetics: January 2015Document24 pagesEssentials of Molecular Genetics: January 2015lavomo-simangoNo ratings yet
- Community Ecology by Gary G. Mittelbach: The Quarterly Review of Biology January 2013Document4 pagesCommunity Ecology by Gary G. Mittelbach: The Quarterly Review of Biology January 2013MonicaNo ratings yet
- Chiang 2016Document313 pagesChiang 2016Anil KumarNo ratings yet
- Carbohydrate Metabolism in Dairy CowsDocument4 pagesCarbohydrate Metabolism in Dairy CowsEduardo Bonilha100% (2)
- Grsmu - Byfilesfileuniversitycafedrynevrologiifileslfklin Protokol PDFDocument197 pagesGrsmu - Byfilesfileuniversitycafedrynevrologiifileslfklin Protokol PDFАнна ФоменкоNo ratings yet
- CHT WFLH Boys Z 0 5Document1 pageCHT WFLH Boys Z 0 5suciNo ratings yet
- CSI Wildlife: Analyzing Genetic EvidenceDocument4 pagesCSI Wildlife: Analyzing Genetic EvidenceInsaf MNo ratings yet
- Chapter 10 Classification of Living and Non-Living ThingsDocument11 pagesChapter 10 Classification of Living and Non-Living ThingsJulius MacaballugNo ratings yet
- Biomedical Engineering Graduate Concentrations: Advisor: Prof. Tim BrunsDocument8 pagesBiomedical Engineering Graduate Concentrations: Advisor: Prof. Tim BrunsDelfina HuangNo ratings yet
- UPSC IFS Zoology SyllabusDocument4 pagesUPSC IFS Zoology SyllabusAntar InenigogNo ratings yet
- Beauty - A-Solute Skincare R1Document39 pagesBeauty - A-Solute Skincare R1Rabby ChowdhuryNo ratings yet
- Human Reproduction: Points To RememberDocument9 pagesHuman Reproduction: Points To RememberPREM277272No ratings yet
- The Flowering Plants Handbook SampleDocument26 pagesThe Flowering Plants Handbook SampleClaramaria RodriguezNo ratings yet
- Egg Depositor of Ornamental FishesDocument4 pagesEgg Depositor of Ornamental FishesPieter SteenkampNo ratings yet
- IJOMRDocument11 pagesIJOMRDharmendra ThakurNo ratings yet
- Toksi PerilakuDocument52 pagesToksi PerilakuseptianasptrNo ratings yet
- Bioinformatic CoursesDocument2 pagesBioinformatic Coursesdenilw100% (1)
- Republic of The Philippines Province of RizalDocument4 pagesRepublic of The Philippines Province of RizalPearl Joy FrancoNo ratings yet
- Nucleotide Metabolism VivaDocument12 pagesNucleotide Metabolism Vivaallswell addoNo ratings yet