Professional Documents
Culture Documents
Impetigo: Idowu O. A RN, M.SC
Impetigo: Idowu O. A RN, M.SC
Uploaded by
Debby Love Goodluck0 ratings0% found this document useful (0 votes)
2 views15 pagesImpetigo is a common bacterial skin infection in children caused by Staphylococcus aureus or Streptococcus pyogenes. It presents as either nonbullous or bullous lesions. Nonbullous impetigo features small pustules that rupture and form crusts, while bullous impetigo features fragile fluid-filled blisters. Diagnosis is usually clinical but cultures can help guide antibiotic treatment. Management involves wound cleaning, topical or systemic antibiotics, and prevention of transmission through good hygiene.
Original Description:
Original Title
IMPETIGO
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentImpetigo is a common bacterial skin infection in children caused by Staphylococcus aureus or Streptococcus pyogenes. It presents as either nonbullous or bullous lesions. Nonbullous impetigo features small pustules that rupture and form crusts, while bullous impetigo features fragile fluid-filled blisters. Diagnosis is usually clinical but cultures can help guide antibiotic treatment. Management involves wound cleaning, topical or systemic antibiotics, and prevention of transmission through good hygiene.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
2 views15 pagesImpetigo: Idowu O. A RN, M.SC
Impetigo: Idowu O. A RN, M.SC
Uploaded by
Debby Love GoodluckImpetigo is a common bacterial skin infection in children caused by Staphylococcus aureus or Streptococcus pyogenes. It presents as either nonbullous or bullous lesions. Nonbullous impetigo features small pustules that rupture and form crusts, while bullous impetigo features fragile fluid-filled blisters. Diagnosis is usually clinical but cultures can help guide antibiotic treatment. Management involves wound cleaning, topical or systemic antibiotics, and prevention of transmission through good hygiene.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 15
IMPETIGO
IDOWU O. A RN, M.Sc
IMPETIGO
• Impetigo is the most common bacterial
infection in children. This acute, highly
contagious infection of the superficial layers of
the epidermis is primarily caused
by Streptococcus pyogenes or Staphylococcus
aureus.
• Secondary skin infections of existing skin
lesions (eg, cuts, abrasions, insect bites,
chickenpox) can also occur.
Classification of Impetigo
• Impetigo is classified as either nonbullous
(impetigo contagiosa) (about 70% of cases ) or
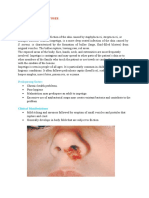
bullous, as shown in the image below.
Bullous Impetigo
Clinical Manisfestations
• Children with nonbullous impetigo commonly
have multiple coalescing lesions on their face
(perioral, perinasal) and extremities or in areas
with a break in the natural skin defense barrier.
The initial lesions are small vesicles or pustules (<
2 cm) that rupture and become a honey-colored
crust with a moist erythematous base. Pharyngitis
is absent, but mild regional lymphadenopathy is
commonly present. Nonbullous impetigo is usually
a self-limited process that resolves within 2 weeks
Bullous
• Bullous impetigo is considered to be less contagious than the
nonbullous form.
• It tends to affect the face, extremities, axillae, trunk, and
perianal region of neonates, but older children and adults
can also be infected.
• The initial lesions are fragile thin-roofed, flaccid, and
transparent bullae (< 3 cm) with a clear, yellow fluid that
turns cloudy and dark yellow.
• Once the bullae rupture, they leave behind a rim of scale
around an erythematous moist base but no crust, followed
by a brown-lacquered or scalded-skin appearance, with a
collarette of scale or a peripheral tubelike rim.
Bullous
• Bullous impetigo also differs from nonbullous
impetigo in that bullous impetigo may involve
the buccal mucous membranes, and regional
adenopathy rarely occurs.
Diagnosis
• The diagnosis of impetigo is usually made on the basis
of the history and physical examination. However,
bacterial culture and sensitivity can be used to confirm
the diagnosis and are recommended in the following
scenarios:
• When MRSA is suspected
• In the presence of an impetigo outbreak
• In the presence of poststreptococcal
glomerulonephritis (PSGN); in such cases, urinalysis is
also necessary
Management
• Treatment of impetigo typically involves local wound
care in conjunction with either a topical antibiotic or a
combination of systemic and topical agents.
• In general, the antibiotic selection has coverage
against both S aureus and S pyogenes.
• In areas with a high prevalence of community-
acquired MRSA with susceptible isolates, children
older than 8 years may take clindamycin or
doxycycline in cases. Trimethoprim-sulfamethoxazole
can be used in situations in which group A
streptococci are unlikely.
Management
• Gentle cleansing, removal of the honey-colored
crusts of nonbullous impetigo using antibacterial
soap and a washcloth, and frequent application of
wet dressings to areas affected by lesions are
recommended.
• Good hygiene with antibacterial washes, such as
chlorhexidine or sodium hypochlorite baths, may
prevent the transmission of impetigo and prevent
recurrences, but the efficacy of this has not been
proven.
Management
• In patients with bullous impetigo who present
to the emergency department with large areas
of involvement resulting in denuded skin from
ruptured bullae, management also includes
intravenous fluid resuscitation.
• Fluid is given at a volume and rate similar to
standard volume replacement for burns.
Prevention and Control
• Children with impetigo should avoid close
contact with other children if possible.
• Inspect household members for impetiginous
lesions. Failure to treat other infected persons
may result in continued transmission.
• Treat traumatized skin with mupirocin because
this has been shown to decrease the rates of
impetigo spread.
Prevention and Control
• Antihistamines and topical steroids help decrease
scratching.
• Treating the underlying disease has also been shown to
decrease the pathogen count on the skin.
• Teach good personal hygiene. For example, keep nails
short and clean and wash hands frequently with
antibacterial soap and water or waterless antibacterial
cleansers.
• Advise patients about improving environmental
conditions through the addition of air conditioning and
by keeping surroundings clean.
Prevention and Control
• For patients with recurrent impetigo,
asymptomatic family members, and S
aureus nasal carriers, prescribe 2% mupirocin
cream or ointment (Bactroban) for application
inside nostrils 3 times per day for 5 days each
month to reduce colonization in the nose.
Appreciation
• THANKS FOR LISTENING
You might also like
- TetanusDocument32 pagesTetanusVinotheran MichaelNo ratings yet
- Sharon Packer - Movies and Modern PsycheDocument217 pagesSharon Packer - Movies and Modern PsycheZoran Kosjerina100% (2)
- Final Argumentative EssayDocument8 pagesFinal Argumentative EssayMatthew EbaluNo ratings yet
- Case Discussion ImpetigoDocument3 pagesCase Discussion ImpetigolouisNo ratings yet
- ImpetigoDocument24 pagesImpetigoIvan Sitohang100% (2)
- Scabies and ImpetigoDocument13 pagesScabies and ImpetigoValabhoju Bindu MadhaviNo ratings yet
- Epidemiology: Aureus and GABHS 10% of The Time. Methicillin-Resistant S Aureus (MRSA) HasDocument8 pagesEpidemiology: Aureus and GABHS 10% of The Time. Methicillin-Resistant S Aureus (MRSA) HasPutra YdpaNo ratings yet
- Skin Diseases Presentation2Document40 pagesSkin Diseases Presentation2DaniTadeNo ratings yet
- ImpetigoDocument13 pagesImpetigoTasya SyafhiraNo ratings yet
- N11 Chan Chloe Micropara 103 Compilation of Microbial Diseases Final RequirementDocument46 pagesN11 Chan Chloe Micropara 103 Compilation of Microbial Diseases Final RequirementCHLOE CATHERINE CHANNo ratings yet
- DERMATOLOGY QuinterDocument177 pagesDERMATOLOGY QuinterstaceyatienoomaNo ratings yet
- Erbil Polythecnic University Soran Technical Insititute Midwifery Dipartment First Stage (M)Document13 pagesErbil Polythecnic University Soran Technical Insititute Midwifery Dipartment First Stage (M)Kubra ĖdrisNo ratings yet
- Desquamative GingivitisDocument41 pagesDesquamative Gingivitislucents100% (1)
- Cutaneous Abscess Furuncles and CarbuclesDocument25 pagesCutaneous Abscess Furuncles and Carbuclesazmmatgowher_1219266No ratings yet
- Background: Group A StreptococcusDocument4 pagesBackground: Group A StreptococcusCoral Srinivasa RamaluNo ratings yet
- Tinea Cruris Imp Points With ReferencesDocument35 pagesTinea Cruris Imp Points With ReferencesSyed Saqib AliNo ratings yet
- Integument - Self StudyDocument4 pagesIntegument - Self Studystudyhard001No ratings yet
- 2F and 2H Lecture 10Document50 pages2F and 2H Lecture 10Mark PalomarNo ratings yet
- Skin Diseases PresentationDocument23 pagesSkin Diseases PresentationDaniTadeNo ratings yet
- Mycotic Diseases and PeriodontiumDocument43 pagesMycotic Diseases and PeriodontiumAhmed Tawfig GamalNo ratings yet
- Communicable Disease Lectures 2Document2 pagesCommunicable Disease Lectures 2Sheana TmplNo ratings yet
- Neonatal InfectionsDocument18 pagesNeonatal InfectionsSanthosh.S.U100% (1)
- Erbil Polythecnic University Soran Technical Insititute Midwifery Dipartment First Stage (M)Document14 pagesErbil Polythecnic University Soran Technical Insititute Midwifery Dipartment First Stage (M)Kubra ĖdrisNo ratings yet
- Superficial Mycoses Group 4Document38 pagesSuperficial Mycoses Group 4prudence azenaborNo ratings yet
- IZZ - PiodermaDocument51 pagesIZZ - PiodermavivilmNo ratings yet
- (Impetigo) : Erbil Polythecnic University Soran Technical Insititute Nuraing Department First StageDocument14 pages(Impetigo) : Erbil Polythecnic University Soran Technical Insititute Nuraing Department First StageKubra ĖdrisNo ratings yet
- Artikan 3Document1 pageArtikan 3Rivan San JayaNo ratings yet
- 11 SinusitisDocument14 pages11 SinusitisCabdiNo ratings yet
- Seminar 13Document10 pagesSeminar 13TusharNo ratings yet
- Dermatology Cutaneous Bacterial InfectionsDocument139 pagesDermatology Cutaneous Bacterial InfectionsArianne Joy C. TamarayNo ratings yet
- Conjunctivitis: Justine S. VillanuevaDocument96 pagesConjunctivitis: Justine S. VillanuevaTee VillanuevaNo ratings yet
- Infectious DermatosesDocument41 pagesInfectious DermatosesJuma SammyNo ratings yet
- Jurnal EditDocument18 pagesJurnal EditSabriadi NursalNo ratings yet
- PEMPHIGUSDocument20 pagesPEMPHIGUSAshish SNo ratings yet
- Guideline For Management of Scabies in Adults and ChildrenDocument20 pagesGuideline For Management of Scabies in Adults and ChildrenDharmaMaya ChandrahasNo ratings yet
- Benign Vulvar Lesions: DR Sally Sayed El-Tawab Lecturer of Gyne-Oncology Alexandria UniversityDocument34 pagesBenign Vulvar Lesions: DR Sally Sayed El-Tawab Lecturer of Gyne-Oncology Alexandria Universitysalah subbahNo ratings yet
- OTITIS EXTERNA Continuing Medical EducationDocument4 pagesOTITIS EXTERNA Continuing Medical EducationhanumzniiNo ratings yet
- Skin Bacterial Diseases - Part - IDocument9 pagesSkin Bacterial Diseases - Part - IElijah WoodNo ratings yet
- Impetigo - MSF Medical GuidelinesDocument4 pagesImpetigo - MSF Medical GuidelinesHamza RiazNo ratings yet
- Skin and Soft Tissue Infectons 1Document51 pagesSkin and Soft Tissue Infectons 1AISHWARYA T DNo ratings yet
- FimosisDocument9 pagesFimosiselsa relandaNo ratings yet
- Mucous Membrane PemphigoidDocument47 pagesMucous Membrane PemphigoidIoana DănilăNo ratings yet
- ConjunctivitisDocument113 pagesConjunctivitisHussam AliNo ratings yet
- Impetigo: Signs and SymptomsDocument3 pagesImpetigo: Signs and Symptomspragna novaNo ratings yet
- Impetigo & Ecthyma Treatment, Symptoms & Causes Merck Manuals - Dermatologic Disorders - MSD ManuaDocument5 pagesImpetigo & Ecthyma Treatment, Symptoms & Causes Merck Manuals - Dermatologic Disorders - MSD ManuaFarid Fauzi A ManwanNo ratings yet
- 3.bacterial Infection-2Document146 pages3.bacterial Infection-2Biruk WorkuNo ratings yet
- GranulomatousDocument55 pagesGranulomatoussisirachandranNo ratings yet
- ACTINOMYCETESDocument22 pagesACTINOMYCETESDaniel WaweruNo ratings yet
- ImmunoBullous DisordersDocument18 pagesImmunoBullous DisordersNali peterNo ratings yet
- Integumentary Disorders (New)Document41 pagesIntegumentary Disorders (New)coosa liquorsNo ratings yet
- Cutaneous InfectionsDocument148 pagesCutaneous InfectionsPratzNo ratings yet
- Overview of Skin InfectionsDocument53 pagesOverview of Skin Infectionsadamu mohammadNo ratings yet
- Dermatitis Conjuntivitis UmbilicitisDocument12 pagesDermatitis Conjuntivitis UmbilicitisNeo CzxNo ratings yet
- Fungi PDFDocument59 pagesFungi PDFChaku LambarNo ratings yet
- Derma 2Document40 pagesDerma 2tyleree3No ratings yet
- Impetigo Is Caused by Bacteria, Specifically TwoDocument6 pagesImpetigo Is Caused by Bacteria, Specifically Twoivy2910324No ratings yet
- Epidemiology of TrachomaDocument46 pagesEpidemiology of TrachomaaanandhiNo ratings yet
- 13otitis ExternaDocument14 pages13otitis ExternaCabdiNo ratings yet
- Zoe Yichang Central People's HospitalDocument32 pagesZoe Yichang Central People's HospitalMohsin Tanmoy100% (1)
- Bullous Skin Disorders: Assist Prof. DR - Ali Elethawi Specialist Dermatologist C.A.B.D, F .I .C.M.SDocument47 pagesBullous Skin Disorders: Assist Prof. DR - Ali Elethawi Specialist Dermatologist C.A.B.D, F .I .C.M.SBurcu KimNo ratings yet
- Impetigo, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandImpetigo, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (3)
- Sebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandSebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Holistic Client Assessment For SeniorsDocument9 pagesHolistic Client Assessment For Seniorscynthia muaauNo ratings yet
- IAH AC Introduction To HomotoxicologyDocument60 pagesIAH AC Introduction To HomotoxicologywurtukukNo ratings yet
- Bioavailability - of MGDocument13 pagesBioavailability - of MGRatanieriNo ratings yet
- FluconazoleDocument3 pagesFluconazoleapi-3797941100% (1)
- Characteristics of NewbornDocument102 pagesCharacteristics of NewbornSusan HepziNo ratings yet
- Natural Ventilation PDFDocument133 pagesNatural Ventilation PDFSamiYousifNo ratings yet
- Non-Restorative Cavity TreatmentDocument8 pagesNon-Restorative Cavity TreatmentQurrat-ul-AinNo ratings yet
- CBRS-Self-Report Assessment ReportDocument24 pagesCBRS-Self-Report Assessment ReportRafael Sanchez0% (3)
- A Disease, Disorder, Illness or Condition: How To Label Epilepsy?Document5 pagesA Disease, Disorder, Illness or Condition: How To Label Epilepsy?HaniNo ratings yet
- Case Study GoiterDocument11 pagesCase Study GoiterJason Napatdan VergaraNo ratings yet
- จมน้ำdrowningถถDocument21 pagesจมน้ำdrowningถถRungtip RuangnaparatNo ratings yet
- Persons With Disabilities: I. Profile / Rationale of The Health ProgramDocument2 pagesPersons With Disabilities: I. Profile / Rationale of The Health ProgrammaryannemacaraigNo ratings yet
- The Triage ProcessDocument3 pagesThe Triage ProcessepingNo ratings yet
- Clonidine Stimulation For GH Secretion in ChildrenDocument2 pagesClonidine Stimulation For GH Secretion in ChildrenMulyono Aba AthiyaNo ratings yet
- MANAGEMENT OF VERTICAL MAXILLARY EXCESS WWWDocument24 pagesMANAGEMENT OF VERTICAL MAXILLARY EXCESS WWWsweetieNo ratings yet
- C-Type Natriuretic Peptide Analogue Therapy in Children With AchondroplasiaDocument11 pagesC-Type Natriuretic Peptide Analogue Therapy in Children With AchondroplasiajakelinelagoadvNo ratings yet
- My Mothers StoryDocument6 pagesMy Mothers Storybde_gnasNo ratings yet
- Journal of The California Dental Hygienists' Association (Summer 2011)Document34 pagesJournal of The California Dental Hygienists' Association (Summer 2011)khaders6682No ratings yet
- Cefalea en El Embarazo y PuerperioDocument21 pagesCefalea en El Embarazo y PuerperioKARINA BASTIDAS IBARRANo ratings yet
- Flushing AgentDocument15 pagesFlushing AgentSalman KhanNo ratings yet
- Pt. Dhainako Putra Sejati: Daftar Harga Jual BarangDocument16 pagesPt. Dhainako Putra Sejati: Daftar Harga Jual BarangBambang TriyonoNo ratings yet
- How To Write A Research Paper: Andrei V. AlexandrovDocument4 pagesHow To Write A Research Paper: Andrei V. AlexandrovdghadaghNo ratings yet
- Ujian Semester IIDocument7 pagesUjian Semester IIYan's GhilehNo ratings yet
- Recreation and Procreation: A Critical View of Sex in The Human FemaleDocument16 pagesRecreation and Procreation: A Critical View of Sex in The Human FemaleVictor MocioiuNo ratings yet
- Types of Economic and Humanistic Outcomes Assessments: Kathleen M. Bungay, Pharm.D. and Lisa A. Sanchez, Pharm.DDocument48 pagesTypes of Economic and Humanistic Outcomes Assessments: Kathleen M. Bungay, Pharm.D. and Lisa A. Sanchez, Pharm.DDrx ahmed MaherNo ratings yet
- Childrens FBC Reference RangesDocument1 pageChildrens FBC Reference RangesmfaddhilNo ratings yet
- Moa Hmo SampleDocument6 pagesMoa Hmo SampleKid ShowNo ratings yet
- Cancer Lung Chemotherapy Regimen 3.4 March 2015Document69 pagesCancer Lung Chemotherapy Regimen 3.4 March 2015Jenny MárquezNo ratings yet