Professional Documents
Culture Documents
Cell Cycle, Apoptosis, Oncogenesis
Cell Cycle, Apoptosis, Oncogenesis
Uploaded by
Insyirah Johari0 ratings0% found this document useful (0 votes)
120 views41 pagesUploaded from Google Docs
Original Title
cell cycle,apoptosis,oncogenesis
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentUploaded from Google Docs
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
0 ratings0% found this document useful (0 votes)
120 views41 pagesCell Cycle, Apoptosis, Oncogenesis
Cell Cycle, Apoptosis, Oncogenesis
Uploaded by
Insyirah JohariUploaded from Google Docs
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
You are on page 1of 41
THE CELL CYCLE
It is the period from the time a cell
comes into existence until cell divides
into 2 daughter cells.
It takes 20 to 24 hours in rapidly
growing cell cultures.
In the human body it may be
fast as in cell culture (hemopoietic cells)
may take 6-12 months (liver cells).
Phases of Cell Cycle
1. The gap 1 (G1) phase
Cell growth occurs.
It takes 9 hours in rapidly growing
cells.
It may take several months(G0 phase).
2. The synthetic (S) phase
DNA synthesis occurs.
It takes 6-9 hours.
3. The gap 2 (G2 )phase
The cell prepares itself for mitosis
It takes 4 hours.
4. The mitotic (M) phase
Cell division occurs
It takes 1-2 hours.
It includes nuclear division ( karyokinesis)
followed by cytoplasmic division (cytokinesis).
NB. The Gl, S, and G2 phases are called the interphase.
REGULATION OF THE CELL CYCLE
Cyclins (family of proteins) regulate the
transition of a cell from one phase to another.
The cyclins concentration increases and
decreases during different phases of the cell
cycle
The cyclins activate certain cyclin-
dependent protein kinases (CDKs) that
phosphorylate substrates essential for the
passage of the cell from one phase to another.
Initiation of cell cycle
It is initiated by the binding of a growth factor
to its receptor on the plasma membrane of the
cell.
The growth factor receptor undergoes auto-
phosphorylation on tyrosine residues and
becomes active protein tyrosine kinase that
can catalyze phosphorylation of certain target
proteins on tyrosine residues.
An intracellular signal finally induces the
production of cyclins.
During the Gl phase: cyclin D increases late
in the Gl phase
It forms a complex with CDK4 and
CDK6, called mitosis promoting factor
(MPF)
MPF catalyzes phosphorylation of the
retinoblastoma (Rb) protein.
The Rb protein is separated from transcription
factor E2F required for the transcription of
genes that code for proteins required to traverse
the Gl-S restriction point, (point beyond which
the cell continues to divide even in the absence of
the growth factor) which becomes active.
MPF can be inhibited by cyclin kinase inhibitory
proteins (CIP) (p16 & p21) which are also known
as cyclin kinase inhibitor (CKI).
NB: The dephosphorylated Rb protein binds to and
inactivates E2F
In early S phase: The E and A cyclins
activate CDK-2, which activates DNA
synthesis.
During the S phase: cells contain large
quantities of enzymes required for DNA
synthesis.
enzymes required for the synthesis of dNTPs
thymidine kinase
dihydrofolate reductase
ribonucleotide reductase
DNA polymerases
In G2 phase : B cyclins are produced late in the G2
phase.
*They activate CDK-1, a protein kinase
responsible for traversing the G2-M checkpoint.
*CDK-1 catalyzes the phosphorylation of:
(1) Histones: leading to condensation of chromosomes.
(2) Nuclear lamins: leading to disassembly of nuclear
membrane.
(3) Actin attachment proteins: leading to loss of
attachment and cell rounding up.
(4) Microtubules and cytoskeleton proteins: leading to
formation of mitotic spindle.
Daughter cells should receive the same
genetic information possessed by the parent
cell to maintain genetic stability ( replication
must be complete and carried out with high
fidelity).
Nuclear DNA is replicated only once during
the S phase .
A pair of chromosomes replicates
simultaneously within a fixed period of the S
phase.
DNA integrity is continuously monitored
throughout the cell cycle in 4 checkpoints.
In G1 phase : Check DNA damage
In G2 phase : Check DNA damage
In S phase : Check completeness of replication
In M phase : Check the proper chromosomal segregation
If the damage could be repaired the cell cycle
continues, if it cannot be repaired the cell
undergoes apoptosis (programmed cell death).
Apoptosis
Apoptosis (dropping off) or cell suicide is a
programmed cell death that occurs during
Embryogenesis
Development
Adult life.
Necrotic cell death caused by cell injury due to
anoxia or radiation.
Death receptors on the plasma membrane bind
death signals, instructing the cell to initiate
apoptosis.
Death signals as tumor necrosis factor
(TNF) and Fas-ligand (CD 95 L) bind the
extracellular domain of the death receptor
and this allows binding of specific proteins
to the intracellular domain and promotes a
cascade of protein-protein interactions.
This activates caspases 8 and 9, which then
activate other caspases.
Caspases are proteases enzymes, they catalyze
the breakdown of cellular proteins.
They activate a specific DNase called caspase-
activated DNase (CAD), which hydrolyzes the
linker DNA between the nucleosomes,
breaking the DNA into fragments.
On electrophoresis, these fragments show a
characteristic ladder appearance.
Apoptosis is also caused by intracellular
stress.
Disruption of mitochondrial membrane
leads to the release of cytochrome c, which
along with apoptosis factor 1 (apaf-1),
activate caspase 9 and initiates the cell
death cascade.
The tumor suppressor protein p53
(unstable protein) is a DNA-binding
transcription factor becomes stabilized by
DNA damage.
In mild DNA damage, p53 induces the production
of the p21 that inhibits the action of all CDKs,
stopping the cell cycle and allowing for DNA
repair.
If DNA damage cannot be repaired, p53 activates a
number of genes that induce apoptosis.
Mutation in the p53 gene inhibits apoptosis and
predisposes to cancer.
The bax protein shares in protein-protein
interaction ending in activation of apoptosis.
The bax protein is inactivated by b-cell lymphoma-
2 (bcl-2) protein.
bax is proapoptotic while bcl-2 is antiapoptotic
(oncogenic).
Examples for apoptosis
Menstruation: Estrogens and progesterone are the
main stimulators of endometrial growth. Withdrawal
of these hormones, due to atrophy of the corpus
luteum causes apoptosis and degeneration of the
endometrium and precipitates menstruation.
Thymus gland atrophy: Glucocorticoids induce
apoptosis in thymocytes and causes atrophy of the
thymus gland in adult life. This action is mediated by
an intracellular glucocorticoid receptor.
ONCOGENESIS
Definition:
Conversion of a regulated cell into a
cancerous one with uncontrolled
growth and metastasis.
Causes:
mutations or underexpression of tumor
suppressor genes.
mutations or overexpression of
protooncogenes.
TUMOR SUPPRESSOR GENES
Products of these genes block abnormal
growth and malignant transformation.
They are usually recessive; both copies of
the gene must undergo mutation to allow
for malignant transformation.
Examples of Tumor Supressor Genes
1. The p53, p21, p16, and bax Genes
About 50% of human cancers have a mutated
p53 gene.
Cells with a mutated gene fail to undergo
apoptosis upon damage of DNA.
A mutation in the p16 gene known as
multiple tumor suppressor 1 (MTS 1) gene,
occurs in a wide variety of cancers.
2. Retinoblastoma (Rb) Gene
Tissues express Rb gene:
retina, osteoblasts and fibroblasts.
Mutation of the gene may be inherited or acquired.
Retinoblastoma is a rare childhood tumor of the
retina.
The child inherits one mutated gene through the
germline and tumor results from acquired
mutation of the remaining normal gene.
3. WT1 and NF1 Genes
WT1 gene
Mutation causes Wilms tumor ( kidney tumor in
children).
The protein product of this gene suppress the
transcription of certain growth factors involved in
the regulation of kidney development.
NF1 gene
One of the most commonly mutated genes in the
population.
Mutation causes neurofibromatosis (1:3000
births ; 97% of cases are benign).
4. Genes of DNA Repair Enzymes
Enzymes of DNA repair prevent tumor
formation by repairing DNA.
Defective genes may cause tumors :
Hereditary Nonpolyposis Colon Cancer (HNPCC)
Xeroderma Pigmentosa
ONCOGENES & PROTOONCOGENES
Oncogenes
They are genes that cause cancer.
Viruses causing cancer in animals
Rous sarcoma virus which causes sarcoma in
chickens.
It is a retrovirus with a DNA intermediate that
integrates into the host genome as a provirus.
The viral DNA contains a gene called src (sarcoma
causing) that encodes a protein-tyrosine kinase
(PTK), which phosphorylates several proteins in
transformed cells.
Some viruses are oncogenic in humans.
These include DNA viruses
Epstein-barr virus (EBV, may cause Burkitt's
lymphoma and nasopharyngeal carcinoma)
human papilloma virus (HPV, may cause cervical
carcinoma)
hepatitis B virus (HBV, may cause HCC)
human herpes virus (HHV, may cause Kaposi sarcoma).
They also include RNA viruses
hepatitis C virus (HCV, may cause HCC)
human T cell lymphotropic virus (HTLV, may
cause T-cell leukemia).
Protooncogenes
They are normal nonmalignant cells contain
DNA sequences homologous to viral oncogenes.
They are active at some stage of development.
Their product proteins are important for cell
growth and differentiation. They include:
growth factors
growth factor receptors
signal transduction proteins
transcription factors
Causes of Conversion of a
protooncogene to an oncogene
1. Promoter or Enhancer Insertion
Retroviruses insert their DNA into the host genome.
If the viral DNA promoter or enhancer is inserted
near a protooncogene in the host cell it becomes a
hyperactive oncogene.
An example is the insertion of a viral promoter or
enhancer near the inactive c-myc gene, leading to
avian leukemia.
2. Gene Amplification
Increased number of copies of genes.
Microscopically appear as homogeneously
staining regions (HSR) on the chromosome
or as extrachromosomal double minute
(dmin) chromosomes.
A growth factor oncogene (hst) is amplified
in some cases of breast cancer.
ErbB2 (HER2/neu) gene is amplified in 20-
30% of human breast cancer and is
associated with poor prognosis.
N-myc is amplified in neuroblastoma and is
associated with poor prognosis.
Dihydrofolate reductase gene is amplified in
cancer patients receiving methotrexate, an
inhibitor of the dihydrofolate reductase
enzyme.
3. Point Mutation
Ras protein (product of the ras protooncogene) is
found in all nucleated cells.
It consists of the αs subunit of the G protein, which
has Intrinsic GTPase activity.
Point mutation converts this gene into ras oncogene
with reduced GTPase activity.
The effect of growth factors acting through G protein
continues after the growth factor dissociates from the
receptor.
This mutation is observed in about 15% of cancers.
4. Chromosomal Translocation
Reciprocal translocation between chromosome 9 and
chromosome 22 produces a fusion BCR-abl gene that encodes
a protein with high PTK activity.
The new chromosome 22 is known as the Philadelphia
chromosome.
Thank you
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5820)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Readers Theater Life FlightDocument5 pagesReaders Theater Life FlightCaurrine Monsalud93% (14)
- Case Study M&SDocument3 pagesCase Study M&S68Rohan Chopra0% (1)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Oncogene EtcDocument48 pagesOncogene EtcInsyirah JohariNo ratings yet
- Apoptosis: Proliferation, Differentiation and Apoptosis Are Crucial To DevelopmentDocument21 pagesApoptosis: Proliferation, Differentiation and Apoptosis Are Crucial To DevelopmentInsyirah JohariNo ratings yet
- At The Forearm.: Biceps Tendon Supinator Pronator Teres Insertion FDS OriginDocument27 pagesAt The Forearm.: Biceps Tendon Supinator Pronator Teres Insertion FDS OriginInsyirah JohariNo ratings yet
- It Enter Between Separates: Flexor RetinaculumDocument20 pagesIt Enter Between Separates: Flexor RetinaculumInsyirah JohariNo ratings yet
- Muscles of Back of ForearmDocument15 pagesMuscles of Back of ForearmInsyirah JohariNo ratings yet
- Flexor & Extensor RetinaculumDocument13 pagesFlexor & Extensor RetinaculumInsyirah Johari100% (1)
- Beginning:: It Is The Larger of Two Terminal Branches of Brachial ArteryDocument18 pagesBeginning:: It Is The Larger of Two Terminal Branches of Brachial ArteryInsyirah JohariNo ratings yet
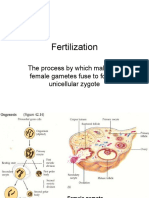
- Fertilization: The Process by Which Male and Female Gametes Fuse To Form A Unicellular ZygoteDocument24 pagesFertilization: The Process by Which Male and Female Gametes Fuse To Form A Unicellular ZygoteInsyirah JohariNo ratings yet
- Front of Forearm LecturesDocument19 pagesFront of Forearm LecturesInsyirah JohariNo ratings yet
- 3rd Week of Embryo DevelopmentDocument20 pages3rd Week of Embryo DevelopmentInsyirah JohariNo ratings yet
- Folding, EmbryoDocument19 pagesFolding, EmbryoInsyirah JohariNo ratings yet
- Embryology: Is The Study of Human DevelopmentDocument16 pagesEmbryology: Is The Study of Human DevelopmentInsyirah Johari100% (1)
- Thorax 1Document109 pagesThorax 1Insyirah JohariNo ratings yet
- Dont Be Fuuld by JuuLDocument3 pagesDont Be Fuuld by JuuLGabriel ParksNo ratings yet
- 哈佛商业评论 (Harvard Business Review)Document7 pages哈佛商业评论 (Harvard Business Review)h68f9trq100% (1)
- Gorillas 191314 0Document2 pagesGorillas 191314 0Marisabel SernaNo ratings yet
- Ajava 6C 2160707 PDFDocument4 pagesAjava 6C 2160707 PDFanon4819No ratings yet
- Vis Tra Frost Beard The HardyDocument13 pagesVis Tra Frost Beard The HardyBrianNo ratings yet
- Clarisse Gulosino and Jonah Liebert 2012 - Review of The Way of The Future, Education Savings Accounts For Every American FamilyDocument12 pagesClarisse Gulosino and Jonah Liebert 2012 - Review of The Way of The Future, Education Savings Accounts For Every American Familyluiz carvalhoNo ratings yet
- Soal Kalimat Prohibition SMP Kelas 7Document3 pagesSoal Kalimat Prohibition SMP Kelas 7yura chanNo ratings yet
- Open-Source Software For Automated Rodent Behavioral AnalysisDocument12 pagesOpen-Source Software For Automated Rodent Behavioral AnalysisGonzalo OrtegaNo ratings yet
- Pantone PDFDocument55 pagesPantone PDFMj Jack Rachmanto100% (1)
- Full Download pdf of (eBook PDF) The Global Casino: An Introduction to Environmental Issues 6th Edition all chapterDocument43 pagesFull Download pdf of (eBook PDF) The Global Casino: An Introduction to Environmental Issues 6th Edition all chapternahoonabid100% (5)
- The Elusive Butterfly: Groove..Document5 pagesThe Elusive Butterfly: Groove..Nasciturus666No ratings yet
- Mole Concept DPP-2 - 501352Document1 pageMole Concept DPP-2 - 501352Vatsal BhargavaNo ratings yet
- Adonis SaturnoDocument6 pagesAdonis SaturnoRaymond G. PanhonNo ratings yet
- 10 Female Superheroes Who Depict Women EmpowermentDocument3 pages10 Female Superheroes Who Depict Women EmpowermentSharjeel ZamanNo ratings yet
- Heatmaster - Hot Water BoilerDocument1 pageHeatmaster - Hot Water BoilerNorbertoNo ratings yet
- International Business: Case Study-Report-3 18-02-2022Document5 pagesInternational Business: Case Study-Report-3 18-02-2022swapnil anandNo ratings yet
- Fuji ManualDocument166 pagesFuji Manualasbel gamNo ratings yet
- DLL All Subjects 2 q2 w9 d1Document9 pagesDLL All Subjects 2 q2 w9 d1Nicole AragonNo ratings yet
- Phlebotomist TrackerDocument62 pagesPhlebotomist Trackertarun sharmaNo ratings yet
- Introduction To Business ResearchDocument23 pagesIntroduction To Business ResearchKhalid ElGhazouliNo ratings yet
- BBPS Kennedy03 PDFDocument8 pagesBBPS Kennedy03 PDFCyz RobertNo ratings yet
- OceanofPDF - Com Return To The Carnival of Horrors - RL StineDocument170 pagesOceanofPDF - Com Return To The Carnival of Horrors - RL Stinedinulaka kaluthanthireeNo ratings yet
- RahmaDocument3 pagesRahmaAyyub RamadanNo ratings yet
- 2018 Bibliography I. Calvin's Life and TimesDocument25 pages2018 Bibliography I. Calvin's Life and Timesmoreirajanne545No ratings yet
- COP2800 MidtermStudyGuideDocument31 pagesCOP2800 MidtermStudyGuideCatherine CrutcherNo ratings yet
- Multimodal Transport Law - The Law Applicable To Multimodal Contract For The Carriage of Goods (PDFDrive)Document561 pagesMultimodal Transport Law - The Law Applicable To Multimodal Contract For The Carriage of Goods (PDFDrive)Isaac Joshua AganonNo ratings yet
- Project Report Dam Level WarningDocument8 pagesProject Report Dam Level Warningpankaj_yadav007No ratings yet
- Rural - India Oct 10 EDELWEISSDocument89 pagesRural - India Oct 10 EDELWEISSpkn04100% (1)