Professional Documents
Culture Documents
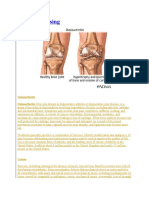
Rheumatoid Arthritis
Rheumatoid Arthritis
Uploaded by
NAMREEN0 ratings0% found this document useful (0 votes)
18 views22 pagesRheumatoid arthritis is an autoimmune disease that causes inflammation of the synovial lining of joints. It is characterized by periods of active disease and remission. Left untreated, it can cause painful joint deformities. The disease involves symmetric inflammation of multiple small joints, especially in the hands and feet. Treatment focuses on reducing inflammation during active periods, protecting joints, exercising within limits, and educating patients on joint care. The goals are to relieve symptoms, maintain function, and prevent further joint damage.
Original Description:
Original Title
RA
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRheumatoid arthritis is an autoimmune disease that causes inflammation of the synovial lining of joints. It is characterized by periods of active disease and remission. Left untreated, it can cause painful joint deformities. The disease involves symmetric inflammation of multiple small joints, especially in the hands and feet. Treatment focuses on reducing inflammation during active periods, protecting joints, exercising within limits, and educating patients on joint care. The goals are to relieve symptoms, maintain function, and prevent further joint damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
18 views22 pagesRheumatoid Arthritis
Rheumatoid Arthritis
Uploaded by
NAMREENRheumatoid arthritis is an autoimmune disease that causes inflammation of the synovial lining of joints. It is characterized by periods of active disease and remission. Left untreated, it can cause painful joint deformities. The disease involves symmetric inflammation of multiple small joints, especially in the hands and feet. Treatment focuses on reducing inflammation during active periods, protecting joints, exercising within limits, and educating patients on joint care. The goals are to relieve symptoms, maintain function, and prevent further joint damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 22
Rheumatoid arthritis
• Rheumatoid arthritis (RA) is an autoimmune, chronic, inflammatory,
systemic disease primarily of unknown etiology affecting the synovial
lining of joints as well as other connective tissue.
• It is characterized by a fluctuating course, with periods of active
disease and remission.
• The onset and progression vary from mild joint symptoms with aching
and stiffness to abrupt swelling, stiffness, and progressive deformity.
Characteristics of RA
• This disease is characterized by symmetric, erosive synovitis with
periods of exacerbation (flare) and remission.
• Joints are characteristically involved with early inflammatory changes in
the synovial membrane, peripheral portions of the articular cartilage,
and subchondral marrow spaces. In response, granulation tissue
(pannus) forms, covers, and erodes the articular cartilage, bone, and
ligaments in the joint capsule.
• Adhesions may form, restricting joint mobility. With progression of the
disease, cancellous bone becomes exposed. Fibrosis, ossific ankylosis, or
subluxation may eventually cause deformity and disability.
1. Migration
of immune 2. WBC
cell in the releases 3. Cytokines attack the
Joint cytokine synovial membrane which
causes synovial cell to
release of other
destructive substances
from synovial membrane
4.Cytokines also causes
synovial membrane to
grow new blood vessel
and form thicken area
called pannus
5. Pannus
grows and
destroy
cartilage
6.Inflammation and
fluid build up
7. Narrow joint
space and
ankylosed
https://www.youtube.com/watch?v=Yc-9dfem3lM
Characteristics of RA
■ Inflammatory changes also occur in tendon sheaths (tenosynovitis); if subjected to recurring
friction, the tendons may rupture.
■ Extra-articular pathological changes sometimes occur; they include rheumatoid nodules, atrophy
and fibrosis of muscles with associated muscular weakness, fatigue, and mild cardiac changes.
■ Progressive deterioration and decline in the functional level of the individual attributed to the
muscular changes and progressive muscle weakness is often seen, leading to major economic loss
and significant impact on families.
■ The degree of involvement varies. Some individuals experience mild symptoms that require
minor lifestyle changes and mild anti-inflammatory medications. Others experience significant
pathological changes in the joints that require major adaptations in lifestyle.
Loss of joint function is irreversible, and often surgery is needed to decrease pain and improve
function. Early recognition is essential during the initial stages, with referral to a rheumatologist for
diagnosis and medical management to control the inflammation and minimize joint damage
Signs and Symptoms: Periods of Active
Disease
■ With synovial inflammation, there is effusion and swelling of the joints, which cause
aching and limited motion. Joint stiffness is prominent in the morning. Usually there is
pain on motion, and a slight increase in skin temperature can be detected over the
joints. Pain and stiffness worsen after strenuous activity.
■ Onset is usually in the smaller joints of the hands and feet, most commonly in the
proximal interphalangeal joints. Usually symptoms are bilateral.
■ With progression, the joints become deformed and may ankylose or subluxate.
■ Pain is often felt in adjoining muscles, and eventually muscle atrophy and weakness
occur. Asymmetry in muscle strength and alterations in the line of pull of muscles and
tendons add to the deforming forces.
■ The person often experiences nonspecific symptoms such as low-grade fever, loss of
appetite and weight, malaise, and fatigue.
Treatment: Acute stage:
• Protect: use resting splints, brace joint during ADLs, adaptive tools to reduce
joint strain during ADLs
• NO STRETCHING as it may stretch the synovial membrane and cause
irreversible damage
• Energy conservation – decrease exercise
• Gentle ROM- pain free
• No lifting heavy weights or doing activities that stress joints
• Ice to reduce inflammation
• Heat only applied briefly in AM to reduce morning stiffness
• Hydrotherapy
Treatment: Chronic stage
• Chronic- no disease flare up
• Capitalize on decreased pain and increased energy
• ROM- full and pain free x Increase cardiovascular activity - aquatics is a
great suggestion
• Strength and endurance activities - pain free: lighter weights, high reps
• Continue joint protection strategies
• Use splints/braces while exercising
• Ice after activity to reduce inflammation
• Heat before activity if needed for stiffness
Principles of Management: Active
Inflammatory Period of RA
■ Patient education. Because periods of active disease may last several months to more than a
year, begin education in the overall treatment plan, safe activity, and joint protection as soon as
possible. It is vital to involve the patient in the management, so he or she learns how to conserve
energy and avoid potential deforming stresses during activities and when exercising.
■ Joint protection and energy conservation. It is important that the patient learns to respect
fatigue and, when tired, rests to minimize undue stress to all the body systems. Because inflamed
joints are easily damaged and rest is encouraged to protect the joints, teach the patient how to
rest the joints in nondeforming positions and to intersperse rest with ROM.
■ Joint mobility. Use gentle grade I and II distraction and oscillation techniques to inhibit pain and
minimize fluid stasis. Stretching techniques are not performed when joints are swollen.
■ Exercise. The type and intensity of exercise vary depending on the symptoms. Encourage the
patient to do active exercises through as much ROM as possible (not stretching). If active exercises
are not tolerated due to pain and swelling, passive ROM is used. Once symptoms of pain and
signs of swelling are controlled with medication, progress exercises as if subacute.
Principles of Management: Subacute and
Chronic Stages of RA
■ Joint protection and activity modification. Continue to emphasize the importance of
protecting the joints by adapting the environment, and by modifying activity, using
orthoses, and assistive devices.
■ Flexibility and strength. To improve function, exercises should be aimed at improving
flexibility, muscle strength, and muscle endurance within the tolerance of the joints.
■ Cardiopulmonary endurance. Nonimpact or low-impact conditioning exercises—such
as aquatic exercise, cycling, aerobic dancing, and walking/running—performed within
the tolerance of the individual improve aerobic capacity and physical activity and
decrease depression and anxiety. Group activities, such as water aerobics, also provide
social support in conjunction with the activity. One randomized review suggested that
aerobic training also has a positive impact on the cardiovascular status of patients with
RA.
CONTRAINDICATIONS:
• Do not perform stretching techniques across swollen joints. When
there is effusion, limited motion is the result of excessive fluid in the
joint space. Forcing motion on the distended capsule overstretches it,
leading to subsequent hypermobility (or subluxation) when the
swelling abates. It may also increase the irritability of the joint and
prolong the joint reaction.
You might also like
- 8 Sample Care Plans For ACDFDocument11 pages8 Sample Care Plans For ACDFacasulla98No ratings yet
- CPT CodesDocument25 pagesCPT Codessureshdass100% (2)
- MTRH I.Med ProtocolsDocument42 pagesMTRH I.Med ProtocolsRoberto Maina100% (3)
- NANDA NursingDocument13 pagesNANDA NursingWaqas Javed0% (1)
- Letter of Recommendation For MacyDocument1 pageLetter of Recommendation For Macyapi-316576287No ratings yet
- University of Cape Town Division of Occupational Therapy - Ahs3107W ArthritisDocument7 pagesUniversity of Cape Town Division of Occupational Therapy - Ahs3107W ArthritisAlexaNo ratings yet
- Physical Therapy and FracturesDocument20 pagesPhysical Therapy and Fracturespasha100% (1)
- OSTEOARTHRITITSDocument25 pagesOSTEOARTHRITITSAnu Magar100% (1)
- Materi D'secret Dr. Tanti Ajoe Kesoema, SP.K.F.R., M.S. (K), M.Si - Med (FIN)Document38 pagesMateri D'secret Dr. Tanti Ajoe Kesoema, SP.K.F.R., M.S. (K), M.Si - Med (FIN)dina rialdiNo ratings yet
- Mobility and ImmobilityDocument35 pagesMobility and ImmobilityLORENZO GABRIEL TUAZONNo ratings yet
- Rehabilitation Management For Rheumatoid Arthritis Patients 2Document19 pagesRehabilitation Management For Rheumatoid Arthritis Patients 2Jothiprasanna KNo ratings yet
- Ankylosing SpondylitisDocument24 pagesAnkylosing SpondylitisSiva ShanmugamNo ratings yet
- Ward 3a PresentationDocument29 pagesWard 3a Presentationevaristfuko02No ratings yet
- Lect 6Document37 pagesLect 6eslambasuony98No ratings yet
- Joint DiseaseDocument5 pagesJoint DiseaseKimrose TampusNo ratings yet
- MwdicineDocument13 pagesMwdicineRohit raj 71No ratings yet
- Rheumatoid HandsDocument144 pagesRheumatoid HandsSushil VijayNo ratings yet
- Rheumatoid Arthritis: Pawan Kumar Nursing Tutor Jietcon JodhpurDocument19 pagesRheumatoid Arthritis: Pawan Kumar Nursing Tutor Jietcon JodhpurBharat Singh BanshiwalNo ratings yet
- Rheumatoid ArthritisDocument3 pagesRheumatoid ArthritisGanah PeterNo ratings yet
- Osteoarthritis: Prepared by Dr/Mohammed AlshehariDocument17 pagesOsteoarthritis: Prepared by Dr/Mohammed AlsheharimosaNo ratings yet
- Case Study Foot FractureDocument4 pagesCase Study Foot Fracturetamsmadjad18No ratings yet
- Arthritis Group 7 (FINAL)Document58 pagesArthritis Group 7 (FINAL)Roxanne Olnosen SimonNo ratings yet
- Sprains and StrainsDocument23 pagesSprains and StrainsokaciaNo ratings yet
- Juvenile Rheumatoid Arthritis: Jeffrey A. LuceroDocument10 pagesJuvenile Rheumatoid Arthritis: Jeffrey A. LucerojamilliumNo ratings yet
- Osteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Document64 pagesOsteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Linda SugiartoNo ratings yet
- The Musculoskeletal HandoutsDocument3 pagesThe Musculoskeletal Handouts_Advernice_No ratings yet
- Musculoskeletal Involvement in Systemic Diseases: - Duru ÇelenoğluDocument93 pagesMusculoskeletal Involvement in Systemic Diseases: - Duru ÇelenoğluDuru ÇelenoğluNo ratings yet
- نسخة light blue creative modern medical clinic presentationDocument33 pagesنسخة light blue creative modern medical clinic presentationFaresNo ratings yet
- OsteoarthritisDocument45 pagesOsteoarthritisMar ClrNo ratings yet
- Health Assessment SAS Session 20Document6 pagesHealth Assessment SAS Session 20Maria Jub MangrubanNo ratings yet
- 43-44 - Muscuskeletal DisordersDocument39 pages43-44 - Muscuskeletal DisordersTaif SalimNo ratings yet
- Reumathoid ArthritisDocument11 pagesReumathoid ArthritisYAny R Setyawati100% (1)
- Assignment Submitted To DR Iqra Naz 70063678 Habiba Jameel DPT 10 Semester. Topic: ArthritisDocument10 pagesAssignment Submitted To DR Iqra Naz 70063678 Habiba Jameel DPT 10 Semester. Topic: ArthritisMuiz SaddozaiNo ratings yet
- Osteoarthritis: Dr. C. C. VisserDocument85 pagesOsteoarthritis: Dr. C. C. VisserAhmad Fathira FitraNo ratings yet
- Passivce Range of Motion ExercisesDocument29 pagesPassivce Range of Motion Exercisesvidyasagar pagilla100% (1)
- 4 Common Musculoskeletal ProblemDocument54 pages4 Common Musculoskeletal ProblemMaria Lynne ParambitaNo ratings yet
- Adhesive Capsulitis or Frozen SholderDocument24 pagesAdhesive Capsulitis or Frozen Sholdersanalcrazy100% (1)
- PDF DocumentDocument94 pagesPDF Documentqqttff18No ratings yet
- THERA2Document1 pageTHERA2olliston.ellieNo ratings yet
- Treatment of Rheumatoid Arthritis ,.Document8 pagesTreatment of Rheumatoid Arthritis ,.sufian JaganyNo ratings yet
- Arthritis (Cabansag, Ma. Flor-And-Cabansag, Joyce)Document38 pagesArthritis (Cabansag, Ma. Flor-And-Cabansag, Joyce)Carlojay IniegoNo ratings yet
- Medical Nutrition Therapy For Diseases of The MusculoskeletalDocument55 pagesMedical Nutrition Therapy For Diseases of The MusculoskeletalAnonymous keDlQbNo ratings yet
- 68 DISEASES 2nd Semsester 3rd Year 1 PDFDocument117 pages68 DISEASES 2nd Semsester 3rd Year 1 PDFJimlord GarciaNo ratings yet
- Athritis, Kelainan Regional Jaringan Ikat Sendi, Infeksi Sendi Dan Kelainan Metabolik Tulang Dan SendiDocument85 pagesAthritis, Kelainan Regional Jaringan Ikat Sendi, Infeksi Sendi Dan Kelainan Metabolik Tulang Dan SendiamaliakhaNo ratings yet
- Joint, Connective Tissue, and Bone Disorders and ManagementDocument47 pagesJoint, Connective Tissue, and Bone Disorders and ManagementAmbreen TariqNo ratings yet
- Neurorehabilitasi Nyeri KronisDocument60 pagesNeurorehabilitasi Nyeri KronisWegrimel AriegaraNo ratings yet
- Muscle Disease ٠٥١٥٢٧Document23 pagesMuscle Disease ٠٥١٥٢٧nagmxxmNo ratings yet
- Ankylosing SpondylytisDocument6 pagesAnkylosing SpondylytisMurad KurdiNo ratings yet
- Muscleoveractivityinthe Uppermotorneuron Syndrome: Conceptualizing A Treatment Plan and Establishing Meaningful GoalsDocument18 pagesMuscleoveractivityinthe Uppermotorneuron Syndrome: Conceptualizing A Treatment Plan and Establishing Meaningful GoalsNacho MicheloniNo ratings yet
- Medical Nursing II Term PaperDocument15 pagesMedical Nursing II Term PaperAdaeze DouglasNo ratings yet
- Geron AssignmentDocument16 pagesGeron AssignmentDERRICKKEANNo ratings yet
- Care of The Client With Rheumatoid Arthritis: A. Pusey Murray (MRS)Document29 pagesCare of The Client With Rheumatoid Arthritis: A. Pusey Murray (MRS)okacia100% (1)
- Weebly Questions Week ElevenDocument4 pagesWeebly Questions Week Elevenapi-459697337No ratings yet
- Medical Nutrition Therapy For Diseases of The MusculoskeletalDocument55 pagesMedical Nutrition Therapy For Diseases of The MusculoskeletalSie ningsih100% (1)
- Basic of Manual TherapyDocument30 pagesBasic of Manual Therapycamy bhagatNo ratings yet
- Fracture RehabilitationDocument43 pagesFracture Rehabilitationnanahossam12345No ratings yet
- V.Lokeesan, BSN T.Assistant Lecturer FHCS, EuslDocument39 pagesV.Lokeesan, BSN T.Assistant Lecturer FHCS, EuslMourian AmanNo ratings yet
- MS 36Document7 pagesMS 36jefrocNo ratings yet
- Ransverse Myelitis TM: by Rusu DumitritaDocument16 pagesRansverse Myelitis TM: by Rusu DumitritaBraga MihaelaNo ratings yet
- Migraine ProjectDocument42 pagesMigraine ProjectprajaktaNo ratings yet
- Natural Solutions for Joint Pain: The Benefits of Alternative Medicine for Optimal Joint HealthFrom EverandNatural Solutions for Joint Pain: The Benefits of Alternative Medicine for Optimal Joint HealthNo ratings yet
- Rheumatoid Arthritis: Natural Approaches to Pain-Free LivingFrom EverandRheumatoid Arthritis: Natural Approaches to Pain-Free LivingNo ratings yet
- Grade 7 Argument Writing: (Continues)Document4 pagesGrade 7 Argument Writing: (Continues)api-441580653No ratings yet
- Assessment Tool For The Geriatric PatientDocument5 pagesAssessment Tool For The Geriatric PatientGlaizalyn Fabella Tagoon100% (1)
- Demostration of Wound DressingDocument10 pagesDemostration of Wound DressingDanish00rizviNo ratings yet
- AlgorithmBLS Ped CA Single RescuerCOVID 200406Document1 pageAlgorithmBLS Ped CA Single RescuerCOVID 200406Karla HernandezNo ratings yet
- Questions and Answers A Guide To Fitness and Wellness 3Rd Edition Liguori Test Bank Full Chapter PDFDocument48 pagesQuestions and Answers A Guide To Fitness and Wellness 3Rd Edition Liguori Test Bank Full Chapter PDFmathewsandersa13j100% (9)
- Executive Summary (1-3)Document3 pagesExecutive Summary (1-3)Jennelyn Solomon PaduaNo ratings yet
- CompetencesDocument16 pagesCompetencesimaguestuserNo ratings yet
- The End Atom171222projectDocument54 pagesThe End Atom171222projectSP AL AMINNo ratings yet
- The Causes and Effects of Water Pollution in Vietnam: Group "Daughters of Mother Nature"Document19 pagesThe Causes and Effects of Water Pollution in Vietnam: Group "Daughters of Mother Nature"Diem SuongNo ratings yet
- Pre-Requisite Programs (PRP) & Critical Control Points (CCP) PDFDocument55 pagesPre-Requisite Programs (PRP) & Critical Control Points (CCP) PDFVenkat SujithNo ratings yet
- Health Education CourseDocument2 pagesHealth Education CourseAmiel Francisco Reyes100% (2)
- The Placebo EffectDocument14 pagesThe Placebo EffectMichelle WenasNo ratings yet
- Print Kil DavidDocument9 pagesPrint Kil Davidapi-3806285No ratings yet
- Performance Monitoring IndicatorsDocument52 pagesPerformance Monitoring IndicatorsannaNo ratings yet
- Medicine's Armory: COVID-19 Vaccines and DrugsDocument56 pagesMedicine's Armory: COVID-19 Vaccines and Drugsjia wenNo ratings yet
- Family Assessment ToolsDocument26 pagesFamily Assessment ToolsFAMED RESIDENTS CESMEDNo ratings yet
- ABC of Choosing An Early Childhood Development Centre For Your ChildDocument2 pagesABC of Choosing An Early Childhood Development Centre For Your ChildjosephNo ratings yet
- Quality Improvement Goals For AKIDocument13 pagesQuality Improvement Goals For AKISoniamartilovaNo ratings yet
- سمنار الاشعة ct scanDocument13 pagesسمنار الاشعة ct scanDiana DedoNo ratings yet
- America's Teen Girls Are Not OkayDocument4 pagesAmerica's Teen Girls Are Not OkayBrenton OwesleyNo ratings yet
- Pathogens and Pathways, and Small Drinking-Water SuppliesDocument22 pagesPathogens and Pathways, and Small Drinking-Water SuppliesZari Sofia Leviste100% (1)
- The Full Time Job VirusDocument40 pagesThe Full Time Job VirusAnkit KumarNo ratings yet
- Malignant Neoplasm (Ovarian Cancer)Document4 pagesMalignant Neoplasm (Ovarian Cancer)nursing concept mapsNo ratings yet
- Chikungunya Virus DiseaseDocument25 pagesChikungunya Virus DiseasemamaluNo ratings yet
- 4885 CriticalReasoning PDFDocument12 pages4885 CriticalReasoning PDFpushpendra kumar vashishthaNo ratings yet
- Strategies in Liver TraumaDocument9 pagesStrategies in Liver TraumaLuis Miguel Díaz VegaNo ratings yet
- Itzayana Carranza ResumeDocument3 pagesItzayana Carranza Resumeapi-612292594No ratings yet