Professional Documents
Culture Documents
Cerebrovascular Diseases
Cerebrovascular Diseases
Uploaded by
kiflom0 ratings0% found this document useful (0 votes)
14 views15 pagesCerebrovascular diseases disrupt blood flow to the brain and can cause ischemia or hemorrhage. Ischemic strokes occur when a blood vessel is blocked, cutting off oxygen to brain tissue, while hemorrhagic strokes involve bleeding within or around the brain. The clinical effects depend on the location and severity of injury, ranging from transient symptoms to permanent disability or death. Imaging tests are used to diagnose the specific type and location of damage.
Original Description:
Original Title
Cerebrovascular Diseases (1)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCerebrovascular diseases disrupt blood flow to the brain and can cause ischemia or hemorrhage. Ischemic strokes occur when a blood vessel is blocked, cutting off oxygen to brain tissue, while hemorrhagic strokes involve bleeding within or around the brain. The clinical effects depend on the location and severity of injury, ranging from transient symptoms to permanent disability or death. Imaging tests are used to diagnose the specific type and location of damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
14 views15 pagesCerebrovascular Diseases
Cerebrovascular Diseases
Uploaded by
kiflomCerebrovascular diseases disrupt blood flow to the brain and can cause ischemia or hemorrhage. Ischemic strokes occur when a blood vessel is blocked, cutting off oxygen to brain tissue, while hemorrhagic strokes involve bleeding within or around the brain. The clinical effects depend on the location and severity of injury, ranging from transient symptoms to permanent disability or death. Imaging tests are used to diagnose the specific type and location of damage.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 15
CEREBROVASCULAR DISEASES
• The brain is a highly oxygen-dependent tissue that
requires a continual supply of glucose and oxygen
from the blood.
• Although it constitutes no more than 2% of body
weight, the brain receives 15% of the resting cardiac
output and is responsible for 20% of total body oxygen
consumption.
• Cerebral blood flow normally remains stable over a
wide range of blood pressure and intracranial pressure
because of autoregulation of vascular resistance.
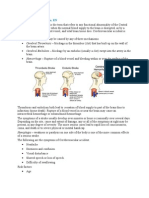
Global Cerebral Ischemia
• Widespread ischemic-hypoxic injury can occur in the setting of
severe systemic hypotension, usually when systolic pressures fall
below 50 mm Hg, as in
cardiac arrest,
shock, and
severe hypotension.
• The clinical outcome varies with the severity and duration of the
insult
• When the insult is mild, there may be only a transient
postischemic confusional state, with eventual complete recovery.
• In severe global cerebral ischemia, widespread
neuronal death occurs
• Patients who survive
often remain severely impaired neurologically and in a
persistent vegetative state OR
brain death, including evidence of diffuse cortical injury
(isoelectric, or “flat,” electroencephalogram) and brain stem
damage, including absence of reflexes and respiratory drive.
Focal Cerebral Ischemia (Ischemic Stroke)
• Cerebral arterial occlusion leads first to focal ischemia and then
to infarction in the distribution of the compromised vessel.
• The size, location, and shape of the infarct and the extent of
tissue damage that results may be modified by collateral blood
flow through
circle of Willis or
cortical-leptomeningeal anastomoses
• However, there is little if any collateral flow to structures such as
the thalamus, basal ganglia, and deep white matter, which are
supplied by deep penetrating vessels.
• Embolic infarctions are more common than
infarctions due to thrombosis.
• The territory of the middle cerebral artery, a
direct extension of the internal carotid artery, is
most frequently affected by embolic infarction.
• Emboli tend to lodge where vessels branch or
in areas of stenosis, usually caused by
atherosclerosis.
• Thrombotic occlusions causing cerebral
infarctions usually are superimposed on
atherosclerotic plaques;
• Common sites are the carotid bifurcation, the
origin of the middle cerebral artery, and at
either end of the basilar artery.
• Infarcts can be divided into two broad groups based on
their macroscopic and corresponding radiologic
appearance
Nonhemorrhagic infarcts result from acute vascular
occlusions and can be treated with thrombolytic therapies,
especially if identified shortly after presentation.
Hemorrhagic infarcts, which result from reperfusion of
ischemic tissue, either through collaterals or after
dissolution of emboli, and often produce multiple,
sometimes confluent petechial hemorrhages
Intracranial Hemorrhage
• Hemorrhages within the brain are associated with
(1)hypertension and other diseases leading to vascular wall injury,
(2) structural lesions such as arteriovenous and cavernous
malformations, and
(3) tumors.
• Subarachnoid hemorrhages most commonly are caused by ruptured
aneurysms but also occur with other vascular malformations.
• Subdural or epidural hemorrhages usually are associated with
trauma.
• Primary Brain Parenchymal Hemorrhage
• Spontaneous (nontraumatic) intraparenchymal
hemorrhages are most common in mid- to late adult life,
with a peak incidence at about 60 years of age.
• Most are due to the rupture of a small intraparenchymal
vessel
• underlying causes include
Hypertension – leading cause and typically occur in the basal
ganglia, thalamus, pons, and cerebellum
Cerebral Amyloid Angiopathy - often occur in the lobes of the
cerebral cortex (lobar hemorrhages).
– Whereas, Spontaneous subarachnoid hemorrhage
usually is caused by
Saccular Aneurysms
Nonsaccular aneurysms (atherosclerotic mycotic,
traumatic, and dissecting aneurysms) - The last three
typesmost often are found in the anterior circulation
whereas atherosclerotic aneurysms most commonly
involve the basilar artery
Vascular Malformations such as arteriovenous
malformations (AVMs)
Vasculitis – could cause both SAH and parenchymal
infarction or hemorrhage.
Clinical Features
• Stroke is a sudden onset of neurologic deficit ,usually on one side ,
that is of vascular cause
• Clinical manifestations depend on the affected arterial distribution.
Egs of focal neurologic deficit include Hemiplegia,aphasia,sensory loss
• Transient ischemic attack (TIA) is due to small platelet thrombi or
atheroemboli and is characteristically reversible, with symptoms
lasting less <24 hours.
• Althogh it is difficult to clinically tell between the two types of stroke,
severe headache, projectile vomiting, rapid deterioration of mentation
and markedly elevated BP are suggestive of hemorrhagic stroke.
• Diagnosis
• Imaging (CT or MRI of the brain)
• Routine lab. Tests and lipid profile
• Coagulation profile
• CXR …..
You might also like
- NCP - Knowledge DeficitDocument2 pagesNCP - Knowledge Deficitjanelee282484% (32)
- SDM - Workshop Book ws1Document28 pagesSDM - Workshop Book ws1容一维0% (1)
- Cerebrovascular DiseasesDocument15 pagesCerebrovascular DiseaseskiflomNo ratings yet
- Cerebrovascular DseDocument303 pagesCerebrovascular DsejjamadriagaNo ratings yet
- BAU PTR-Neurology-Lecture 11-StrokeDocument133 pagesBAU PTR-Neurology-Lecture 11-Strokeerfan mohammadiNo ratings yet
- Cerebrovascular Pathology: Abel B. (MD) Pathology Lectures, NMEI, DBUDocument59 pagesCerebrovascular Pathology: Abel B. (MD) Pathology Lectures, NMEI, DBUdenekeNo ratings yet
- Acquired Central Nervous System Vascular Disorders-1Document39 pagesAcquired Central Nervous System Vascular Disorders-1Jake MillerNo ratings yet
- The CNS CVADocument21 pagesThe CNS CVAfatima.noor0747No ratings yet
- Stroke 1Document69 pagesStroke 1Berk HalilbeyoğluNo ratings yet
- Stroke UgDocument76 pagesStroke Ug74. Shravani VNo ratings yet
- Lecture 3Document41 pagesLecture 3issrafil mussaNo ratings yet
- Stroke HemoragikDocument34 pagesStroke HemoragikTeuku AndyNo ratings yet
- Taufan Arif, S.Kep., NS., M.KepDocument85 pagesTaufan Arif, S.Kep., NS., M.KepputriNo ratings yet
- Stroke: DR Abdirahman AbibDocument40 pagesStroke: DR Abdirahman AbibMahad IbrahemNo ratings yet
- Acute StrokeDocument13 pagesAcute StrokeJoel CanenciaNo ratings yet
- Stroke: DR Abdirahman AbibDocument43 pagesStroke: DR Abdirahman AbibMahad IbrahemNo ratings yet
- REPORTDocument34 pagesREPORTClaire GidoNo ratings yet
- Cerebral Vascular AccidentDocument70 pagesCerebral Vascular AccidentSheda BondNo ratings yet
- StrokeDocument17 pagesStrokeJo CanensNo ratings yet
- Stroke: Etiology, Classification, and EpidemiologyDocument34 pagesStroke: Etiology, Classification, and EpidemiologySteffNo ratings yet
- Stroke (Encephalitis/Meningitis) Trauma Kepala Trauma Medulla SpinalisDocument61 pagesStroke (Encephalitis/Meningitis) Trauma Kepala Trauma Medulla SpinalisUmar MukhtarNo ratings yet
- C VADocument25 pagesC VAsudeepminz15No ratings yet
- INTRODUCTION - The Two Broad Categories of Stroke, Hemorrhage and IschemiaDocument11 pagesINTRODUCTION - The Two Broad Categories of Stroke, Hemorrhage and IschemiaJose Enrique OrtizNo ratings yet
- Pathology of Stroke: Dr. Isnaniah, Sp. SDocument51 pagesPathology of Stroke: Dr. Isnaniah, Sp. SFiladelfia sariNo ratings yet
- Stroke: Clinical Presentation and Anatomical LocalizationDocument36 pagesStroke: Clinical Presentation and Anatomical LocalizationYusuf JoganNo ratings yet
- Stroke: Etiology, Classification, and EpidemiologyDocument34 pagesStroke: Etiology, Classification, and EpidemiologySteffNo ratings yet
- Batul StrokeDocument20 pagesBatul StrokeBatul JoharNo ratings yet
- Definitions: PathophysiologyDocument5 pagesDefinitions: PathophysiologyeduardNo ratings yet
- Lecture 2 Ischemic Heart DiseasesDocument19 pagesLecture 2 Ischemic Heart DiseasesOsama MalikNo ratings yet
- Stroke: Joan Marie Amamio BSN IV Report byDocument35 pagesStroke: Joan Marie Amamio BSN IV Report byAnjo Marie AmamioNo ratings yet
- Cerebral Vascular AccidentDocument16 pagesCerebral Vascular AccidentTeba AhmedNo ratings yet
- Pathology of CNS: Eric M. Mirandilla MD, DPSPDocument71 pagesPathology of CNS: Eric M. Mirandilla MD, DPSPDhruva PatelNo ratings yet
- Stroke MsDocument57 pagesStroke MsAishwarya ShahNo ratings yet
- PBL 2 - StrokeDocument14 pagesPBL 2 - StrokeKong Pei IngNo ratings yet
- Ischemic StrokeDocument17 pagesIschemic StrokejamalNo ratings yet
- Cardiovascular Pathology 2024Document132 pagesCardiovascular Pathology 2024Chen HouyuNo ratings yet
- Myocardial InfarctionDocument6 pagesMyocardial InfarctionMaicie Rose Bautista VallesterosNo ratings yet
- Pathophysiology of StrokeDocument9 pagesPathophysiology of StrokeAnj MandeoyaNo ratings yet
- Stroke: Abyot From Harrison, DR Belachew and DR Yared HandoutDocument32 pagesStroke: Abyot From Harrison, DR Belachew and DR Yared HandoutashuNo ratings yet
- By. ScribdDocument3 pagesBy. Scribdchreazy__021906No ratings yet
- Myocardial InfarctionDocument19 pagesMyocardial InfarctionkiflomNo ratings yet
- PATHO-II Unit V Cardiovascular DisordersDocument52 pagesPATHO-II Unit V Cardiovascular DisordersMuhammad ShayanNo ratings yet
- Stroke: Pathophysiology, Types, Management Categories, and Vascular SyndromesDocument49 pagesStroke: Pathophysiology, Types, Management Categories, and Vascular Syndromesrabia khalidNo ratings yet
- CVADocument11 pagesCVACla100% (4)
- Etiology and Classification of StrokeDocument10 pagesEtiology and Classification of Strokeaeiou33No ratings yet
- Sudden DeathDocument26 pagesSudden DeathAbang AzharNo ratings yet
- The Cardiovascular SystemDocument43 pagesThe Cardiovascular Systemtravis efraimNo ratings yet
- Stroke: DefinitionDocument8 pagesStroke: DefinitionKasuganti koteshwar raoNo ratings yet
- LP Stroke Hemoragik OkDocument18 pagesLP Stroke Hemoragik OkramidahNo ratings yet
- StrokeDocument50 pagesStrokeABREHAM BUKULONo ratings yet
- Embolism and Infarction: Dr. Marwa Ali AbdulnabiDocument37 pagesEmbolism and Infarction: Dr. Marwa Ali Abdulnabiعلي حميد فريحNo ratings yet
- Clinical DiscussionDocument18 pagesClinical DiscussionKia MojicaNo ratings yet
- Myocardial InfarctionDocument20 pagesMyocardial Infarction* mokhtar !!50% (2)
- Stroke: Dr. Alberto CampodónicoDocument17 pagesStroke: Dr. Alberto CampodónicoJohn Domínguez MedinaNo ratings yet
- 8-_StrokeDocument55 pages8-_StrokeAldood Al NatarNo ratings yet
- Stroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Document19 pagesStroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Yusi RizkyNo ratings yet
- MEDSURG-FINAL-NOTESDocument54 pagesMEDSURG-FINAL-NOTESMary Ann BaliliNo ratings yet
- Hemorraghic StrokeDocument4 pagesHemorraghic StrokeRachelle Delantar100% (1)
- Cerebral AneurysmDocument69 pagesCerebral AneurysmDiksha chaudharyNo ratings yet
- STROKE: Handbook with activities, exercises and mental challengesFrom EverandSTROKE: Handbook with activities, exercises and mental challengesNo ratings yet
- Foreign Body in The LungDocument13 pagesForeign Body in The LungkiflomNo ratings yet
- Shock and AkiDocument22 pagesShock and AkikiflomNo ratings yet
- Glomerular DiseasesDocument37 pagesGlomerular DiseaseskiflomNo ratings yet
- HTN and CHFDocument29 pagesHTN and CHFkiflomNo ratings yet
- Myocardial InfarctionDocument19 pagesMyocardial InfarctionkiflomNo ratings yet
- HEMATOPATHOLOGYDocument33 pagesHEMATOPATHOLOGYkiflomNo ratings yet
- Cerebrovascular DiseasesDocument15 pagesCerebrovascular DiseaseskiflomNo ratings yet
- Renal and Urinary System PathologyDocument70 pagesRenal and Urinary System PathologykiflomNo ratings yet
- A Brief Introduction To Basic FunctionalDocument50 pagesA Brief Introduction To Basic FunctionalkiflomNo ratings yet
- Renal and Urinary System Pathology: by Dr. Kiflom H. Sep, 2021 GCDocument258 pagesRenal and Urinary System Pathology: by Dr. Kiflom H. Sep, 2021 GCkiflomNo ratings yet
- Kill A DogDocument2 pagesKill A DogkenshahNo ratings yet
- Imci Introduction Danger Signs 2023Document61 pagesImci Introduction Danger Signs 2023Nathaniel NograNo ratings yet
- Hospital Inventory Management Ca2Document5 pagesHospital Inventory Management Ca2Sneha MukherjeeNo ratings yet
- Antimicrobial ResistenceDocument23 pagesAntimicrobial Resistencelayal mrowehNo ratings yet
- Professor: Submitted To: Ms. Mary Grace L. SagunDocument7 pagesProfessor: Submitted To: Ms. Mary Grace L. SagunlalaNo ratings yet
- Cholecystectomy: Cholecystectomy (Pronounced / Kɒləsɪs Tɛktəmi/, Plural: Cholecystectomies) Is TheDocument3 pagesCholecystectomy: Cholecystectomy (Pronounced / Kɒləsɪs Tɛktəmi/, Plural: Cholecystectomies) Is Thejosias_jorgio1No ratings yet
- ISOLATION - Hand HygieneDocument16 pagesISOLATION - Hand HygieneAnna Carmela Pillora MelendezNo ratings yet
- Drug StudyDocument15 pagesDrug StudyDavid RefuncionNo ratings yet
- Clinical Laboratory Blood Banking and TransfusionDocument492 pagesClinical Laboratory Blood Banking and TransfusionSaima IramNo ratings yet
- Critical Review of Ritu Seasons With Special ReferDocument3 pagesCritical Review of Ritu Seasons With Special ReferAJ StokerNo ratings yet
- CHN-RLE Module 1 (Hand Washing)Document7 pagesCHN-RLE Module 1 (Hand Washing)Ems Rio BalNo ratings yet
- Semi Detailed Lesson Plan Eed Tle 2Document7 pagesSemi Detailed Lesson Plan Eed Tle 2Lopez Rhen DaleNo ratings yet
- Definition, Risk Factors and Epidemiology of Colorectal CancerDocument3 pagesDefinition, Risk Factors and Epidemiology of Colorectal Cancerdeer muNo ratings yet
- Practice Tests - First Term English 10 PRACTICE TEST (Unit 1: Family Life) Time Allowed: 60 MinutesDocument21 pagesPractice Tests - First Term English 10 PRACTICE TEST (Unit 1: Family Life) Time Allowed: 60 MinutesLương NguyễnNo ratings yet
- Nursing Process: CYCLIC-regularly Repeated Events DYNAMIC - Continuously ChangingDocument16 pagesNursing Process: CYCLIC-regularly Repeated Events DYNAMIC - Continuously ChangingHeide Basing-aNo ratings yet
- Windshield Survey ComponentDocument1 pageWindshield Survey ComponentMavi RomadaniNo ratings yet
- ENG - Metalgial PDFDocument6 pagesENG - Metalgial PDFRiriNo ratings yet
- Bombay Hospital: Medical CertificateDocument1 pageBombay Hospital: Medical CertificateSandeep ShahNo ratings yet
- Modern TimesDocument58 pagesModern TimesMicah DomingoNo ratings yet
- Gastric Resection: General Surgical and Anesthetic ConsiderationsDocument26 pagesGastric Resection: General Surgical and Anesthetic ConsiderationsBlanchette ChNo ratings yet
- Ahmed Project YSU (1) FINAL EDITION 2016 2017-1Document28 pagesAhmed Project YSU (1) FINAL EDITION 2016 2017-1Yakubu Adamu JajereNo ratings yet
- Chronic DiseaseDocument13 pagesChronic DiseaseDanielle MadeNo ratings yet
- Module 1 Part 2 Eco ModelDocument22 pagesModule 1 Part 2 Eco ModelZaren James D. RacaNo ratings yet
- A Systematic Review of Running-Related Musculoskeletal Injuries in RunnersDocument10 pagesA Systematic Review of Running-Related Musculoskeletal Injuries in RunnersInfo-qe QualityenergyNo ratings yet
- Daftar Pasien Neurologi SELASA, 02 MARET 2021: Lontara 3 Saraf Kamar 1Document5 pagesDaftar Pasien Neurologi SELASA, 02 MARET 2021: Lontara 3 Saraf Kamar 1Louis MailuhuNo ratings yet
- Healing of Oral WoundsDocument73 pagesHealing of Oral WoundsMadhvendra Singh80% (5)
- AKI and Collapsing Glomerulopathy Associated With.10Document8 pagesAKI and Collapsing Glomerulopathy Associated With.10Arista RachmaNo ratings yet
- MEDICAL TERMINOLOGY PRAKTIKUM.2020docxDocument17 pagesMEDICAL TERMINOLOGY PRAKTIKUM.2020docxmawarNo ratings yet