Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
14 viewsOral Mucosa
Oral Mucosa
Uploaded by
Lobna ElkilanyThe document defines stomatitis as inflammation of the mucous membrane in the mouth. It describes the symptoms as red patches, mouth ulcers, blisters, swelling, soreness and numbness. The causes include bacterial, fungal or viral infections, systemic disorders, drugs, physical irritation or allergies. Investigations may include bacterial/viral swabs, biopsies or blood tests. Treatment depends on the cause but includes antibiotics, antifungals, correcting deficiencies, corticosteroids and symptomatic relief.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Dermatology Questions and AnsDocument147 pagesDermatology Questions and AnsEl FaroukNo ratings yet
- BAKER, William J. The Making of A Working-Class Football CultureDocument12 pagesBAKER, William J. The Making of A Working-Class Football CultureGabriela Marta Marques de Oliveira100% (1)
- Chapter 5 Cdi 1 Final EditedDocument16 pagesChapter 5 Cdi 1 Final EditedBelinda Viernes50% (2)
- Histology of Oral Mucous Membrane and GingivaDocument86 pagesHistology of Oral Mucous Membrane and GingivahazeemmegahedNo ratings yet
- Histologi Epitel Dan Mukosa Rongga Mulut-2021Document49 pagesHistologi Epitel Dan Mukosa Rongga Mulut-2021Cat cuteNo ratings yet
- Oral Mucous Membrane: by - Arindam MondalDocument92 pagesOral Mucous Membrane: by - Arindam MondalMohammed hisham khanNo ratings yet
- Oral Mucous Membrane: by - Arindam MondalDocument92 pagesOral Mucous Membrane: by - Arindam MondalMohammed hisham khanNo ratings yet
- Oral Mucous MembraneDocument200 pagesOral Mucous MembraneKush Pathak100% (3)
- Oral Mucosa: (Ten Cates)Document14 pagesOral Mucosa: (Ten Cates)Vanshika SethiNo ratings yet
- Oral Mucous MembraneDocument71 pagesOral Mucous MembraneHarleen GrewalNo ratings yet
- Oral Mucosa Oral MucosaDocument31 pagesOral Mucosa Oral Mucosaroqaia roqaiaNo ratings yet
- نسخة نسخة نسخة ريميDocument6 pagesنسخة نسخة نسخة ريميAhmed QahtaniNo ratings yet
- Cavum Oris Blok 3 PDFDocument63 pagesCavum Oris Blok 3 PDFShaffa Aprilia Amanda PutriNo ratings yet
- Cavum Oris & Salivary Gland Block 3Document63 pagesCavum Oris & Salivary Gland Block 3Muhammad HammamNo ratings yet
- Oral MucosaDocument109 pagesOral Mucosashahzeb memonNo ratings yet
- 11 Oral Mucous MembraneDocument53 pages11 Oral Mucous MembraneMohammed rezgallahNo ratings yet
- Oral Mucosa: Iryn A. LagartoDocument8 pagesOral Mucosa: Iryn A. LagartoVarenLagartoNo ratings yet
- 5 - Oral Mucosa and Salivary Glands (Mahmoud Bakr)Document115 pages5 - Oral Mucosa and Salivary Glands (Mahmoud Bakr)MobarobberNo ratings yet
- Periodontology Lec 2Document24 pagesPeriodontology Lec 2Ali MONo ratings yet
- نسخة PerioDocument6 pagesنسخة PerioAhmed QahtaniNo ratings yet
- Gingi VaDocument225 pagesGingi VaJoji IsacNo ratings yet
- Digestive System Part 1Document12 pagesDigestive System Part 1عبدالرحمن عدي عبدالفتاحNo ratings yet
- ANA 222 Intergumentry System HistologyDocument7 pagesANA 222 Intergumentry System HistologyprincessmakklisNo ratings yet
- Integumentary SystemDocument24 pagesIntegumentary SystemWadabiNo ratings yet
- Lecture Presented by:-ALI Waheed /yasmin Falah /zainab Mazin Supervised By:-Dr. Sattar Jabbar Jasim /cell and Tissue BiomedicalDocument24 pagesLecture Presented by:-ALI Waheed /yasmin Falah /zainab Mazin Supervised By:-Dr. Sattar Jabbar Jasim /cell and Tissue BiomedicalAli Waheed jolan100% (1)
- GENERAL HISTOLOGY pdf-1Document22 pagesGENERAL HISTOLOGY pdf-1Dany Samuel100% (1)
- Oral Mucous Membrane: DR Saurabh Juneja Professor and Head Dept of Oral Pathology SBBDCDocument54 pagesOral Mucous Membrane: DR Saurabh Juneja Professor and Head Dept of Oral Pathology SBBDCPuneet KaurNo ratings yet
- Vertebrate Integument and DerivativesDocument16 pagesVertebrate Integument and DerivativesNarasimha MurthyNo ratings yet
- Unit 5 Skin and Integumentary SystemDocument104 pagesUnit 5 Skin and Integumentary SystemSino McakoNo ratings yet
- Characteristics of Living Organisms and The Integumentary SystemDocument11 pagesCharacteristics of Living Organisms and The Integumentary SystemSHYRE COLEEN CATAYAONo ratings yet
- Lecture 2 Non Keratinizedmucosa Non KeratinocytesDocument29 pagesLecture 2 Non Keratinizedmucosa Non KeratinocytesAMIT GUPTANo ratings yet
- Piel NormalDocument17 pagesPiel NormalfrankyelitNo ratings yet
- Practical Class 5Document73 pagesPractical Class 5Chahinez HabibNo ratings yet
- Skin Structure and Function: Figure 1.1 Cross-Section of The SkinDocument11 pagesSkin Structure and Function: Figure 1.1 Cross-Section of The SkinfunmugNo ratings yet
- 11 B IntegumenttextDocument41 pages11 B IntegumenttextAbu Ibtihal OsmanNo ratings yet
- CHP 12 - Oral Mucosa-1Document83 pagesCHP 12 - Oral Mucosa-1Areej Fatima100% (2)
- Histology Structure of SkinDocument4 pagesHistology Structure of SkinLIEBERKHUNNo ratings yet
- Upper Git FinalDocument11 pagesUpper Git Finalgergeskamal020No ratings yet
- Oral Mucous MembraneDocument79 pagesOral Mucous MembraneKarthik MungamuriNo ratings yet
- Anatomy and PhysiologyDocument25 pagesAnatomy and PhysiologyNaidin Catherine De Guzman-AlcalaNo ratings yet
- Maya Tejasari Histology Department Faculty of Medicine Bandung Islamic UniversityDocument65 pagesMaya Tejasari Histology Department Faculty of Medicine Bandung Islamic UniversitydeasyahNo ratings yet
- Histo ALLDocument59 pagesHisto ALLoday25No ratings yet
- Chapter 1Document31 pagesChapter 1cabdinuux32No ratings yet
- Lit SkinStruct Bensouillah Ch01 PDFDocument11 pagesLit SkinStruct Bensouillah Ch01 PDFisaco1531012No ratings yet
- Digestive Tract: Esophagus, Stomach, Small and Large Intestines, Rectum, and Anus and ItsDocument10 pagesDigestive Tract: Esophagus, Stomach, Small and Large Intestines, Rectum, and Anus and Itsحوراء عارف الموسويNo ratings yet
- Meth Elab Topic N1Document23 pagesMeth Elab Topic N1Group M1869No ratings yet
- Skin LayersDocument3 pagesSkin LayersCrackmcat CrackmcatNo ratings yet
- Digestive SYSTEMDocument53 pagesDigestive SYSTEMPrincess AnnNo ratings yet
- IntegumentaryDocument7 pagesIntegumentarySimone ApostolNo ratings yet
- Oral Mucous Membrane (Oral Mucosa)Document7 pagesOral Mucous Membrane (Oral Mucosa)روان امير غني عبد عونNo ratings yet
- Lecture 27 - Histology of The Integumentary System 2Document89 pagesLecture 27 - Histology of The Integumentary System 2spitzmark2030No ratings yet
- 5 - Skin Mucous MembraneDocument32 pages5 - Skin Mucous MembranecheckmateNo ratings yet
- Skin and Body Membranes HahaDocument6 pagesSkin and Body Membranes Hahaقى قىNo ratings yet
- The Integumentary System and HomeostasisDocument9 pagesThe Integumentary System and HomeostasisJohn Paul ArcillaNo ratings yet
- EPITHELIUMDocument38 pagesEPITHELIUMAstridNo ratings yet
- Salivary GlandDocument112 pagesSalivary GlandSwati SawalNo ratings yet
- The Digestive System IDocument55 pagesThe Digestive System IYousef KhallafNo ratings yet
- IntegumentarysystemDocument99 pagesIntegumentarysystemkuro hanabusaNo ratings yet
- Tob 3.2Document33 pagesTob 3.2LT DRAGONXNo ratings yet
- 1.integumentary System - HistologyDocument34 pages1.integumentary System - Histologyqty9jgkpnzNo ratings yet
- Dermatology FirecrackerDocument28 pagesDermatology FirecrackerKeham LeogNo ratings yet
- Morphology of SKIN LesionsDocument32 pagesMorphology of SKIN LesionsLobna ElkilanyNo ratings yet
- 4 - (CHF), IschemicDocument31 pages4 - (CHF), IschemicLobna ElkilanyNo ratings yet
- 2 - RH Fev, Inf EndoDocument37 pages2 - RH Fev, Inf EndoLobna ElkilanyNo ratings yet
- 3 - Valvular Heart DiseasesDocument31 pages3 - Valvular Heart DiseasesLobna ElkilanyNo ratings yet
- 1 - HypertensionDocument35 pages1 - HypertensionLobna ElkilanyNo ratings yet
- Vonnegut 1st Printings W Numbers of Copies PrintedDocument6 pagesVonnegut 1st Printings W Numbers of Copies PrintedBrad BoothNo ratings yet
- Chapter2 PDFDocument88 pagesChapter2 PDFVanwesly Prayoga100% (1)
- Defense of The AncientsDocument3 pagesDefense of The AncientsNissa CleopatraNo ratings yet
- HIS3MHI - Silence Is Golden - Final EssayDocument5 pagesHIS3MHI - Silence Is Golden - Final EssaySascha McNulty100% (1)
- Research ReviewerDocument14 pagesResearch ReviewerSnowball MeowwNo ratings yet
- Erdogan Visits WashingtonDocument3 pagesErdogan Visits WashingtonPatrick SnellNo ratings yet
- Terrepedia: A Project Report For The Course Lean Startup Management (Mgt1022) Under The Guidance of Prof. Thiagarajan SDocument20 pagesTerrepedia: A Project Report For The Course Lean Startup Management (Mgt1022) Under The Guidance of Prof. Thiagarajan SSamyak DoshiNo ratings yet
- TNCT Q3ExamDocument7 pagesTNCT Q3ExamREY ANN RUBIONo ratings yet
- To BeDocument7 pagesTo BeSamuel Celedonio RodriguezNo ratings yet
- Kandiyoti. Women, Islam and The StateDocument8 pagesKandiyoti. Women, Islam and The StateArticulación ProvincialNo ratings yet
- Mindanao Community School, Inc.: Empowerment TechnologiesDocument11 pagesMindanao Community School, Inc.: Empowerment TechnologiesavinmanzanoNo ratings yet
- Microcontroller Based Automated Voltage Pulse TesterDocument3 pagesMicrocontroller Based Automated Voltage Pulse TesterInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- AeroShell Grease 7 PDFDocument2 pagesAeroShell Grease 7 PDFAnonymous oAbjbl4HNo ratings yet
- Summative Test English 8Document2 pagesSummative Test English 8Cristina SarmientoNo ratings yet
- Deleuze - Description of Woman For A Philosophy of The Sexed OtherDocument9 pagesDeleuze - Description of Woman For A Philosophy of The Sexed OtherMichael SchwartzNo ratings yet
- English 10-Q4-M7Document13 pagesEnglish 10-Q4-M7Joemar De Pascion NovillaNo ratings yet
- Flatpack McuDocument2 pagesFlatpack McuAVkucher1983No ratings yet
- The Misunderstood StorytellerDocument11 pagesThe Misunderstood Storyteller50_BMGNo ratings yet
- Guidance On The Compilation of Safety Data SheetsDocument138 pagesGuidance On The Compilation of Safety Data SheetsAlexEcnomNo ratings yet
- Wellbeing at Work A Practical GuideDocument38 pagesWellbeing at Work A Practical GuideFahad SiddiqNo ratings yet
- 2) There Was A Murder Last Night. What Were They Doing When The Murder Happened?Document2 pages2) There Was A Murder Last Night. What Were They Doing When The Murder Happened?Pilar Gonzalez PinillaNo ratings yet
- A Weavers Cooperative: A Boon To Weavers ... : Koustavi ChakrabortyDocument4 pagesA Weavers Cooperative: A Boon To Weavers ... : Koustavi ChakrabortyKoustavi ChakrabortyNo ratings yet
- Temple of GodDocument4 pagesTemple of GodNathan ChrisNo ratings yet
- Financial Highlights: Hinopak Motors LimitedDocument6 pagesFinancial Highlights: Hinopak Motors LimitedAli ButtNo ratings yet
- Ethics in PracticeDocument14 pagesEthics in PracticedanielktingNo ratings yet
- 09 Chapter IDocument45 pages09 Chapter ISYED TAYYABNo ratings yet
- Generate Visitors - Google DiscoverDocument8 pagesGenerate Visitors - Google DiscoverJohn CenaNo ratings yet
- Module Ramadan 3Document6 pagesModule Ramadan 3Darkant TnakradNo ratings yet
Oral Mucosa
Oral Mucosa
Uploaded by
Lobna Elkilany0 ratings0% found this document useful (0 votes)
14 views40 pagesThe document defines stomatitis as inflammation of the mucous membrane in the mouth. It describes the symptoms as red patches, mouth ulcers, blisters, swelling, soreness and numbness. The causes include bacterial, fungal or viral infections, systemic disorders, drugs, physical irritation or allergies. Investigations may include bacterial/viral swabs, biopsies or blood tests. Treatment depends on the cause but includes antibiotics, antifungals, correcting deficiencies, corticosteroids and symptomatic relief.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document defines stomatitis as inflammation of the mucous membrane in the mouth. It describes the symptoms as red patches, mouth ulcers, blisters, swelling, soreness and numbness. The causes include bacterial, fungal or viral infections, systemic disorders, drugs, physical irritation or allergies. Investigations may include bacterial/viral swabs, biopsies or blood tests. Treatment depends on the cause but includes antibiotics, antifungals, correcting deficiencies, corticosteroids and symptomatic relief.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
14 views40 pagesOral Mucosa
Oral Mucosa
Uploaded by
Lobna ElkilanyThe document defines stomatitis as inflammation of the mucous membrane in the mouth. It describes the symptoms as red patches, mouth ulcers, blisters, swelling, soreness and numbness. The causes include bacterial, fungal or viral infections, systemic disorders, drugs, physical irritation or allergies. Investigations may include bacterial/viral swabs, biopsies or blood tests. Treatment depends on the cause but includes antibiotics, antifungals, correcting deficiencies, corticosteroids and symptomatic relief.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 40
ORAL MUCOSA
DR/ MAHA HUSSUIEN
KANDIL
Professor of Dermatology – Faculty of
Medicine –Minia University
Definition:
The mucous membrane that lines the
structures within the oral cavity.
This is a wet soft tissue membrane that
extends from the vermilion border of the lips
anteriorly to the palatopharyngeal folds
posteriorly.
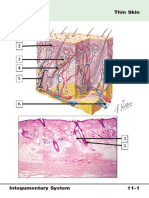
Histologically:
The oral mucosa is formed by three layers:
1-Stratified squamous epithelium (oral
epithelium): whose thickness and degree of
keratinization depend on the location and
functional requirements.
2- Lamina propria: is an underlying
connective tissue.
3- Submucosa: a dense irregular connective
tissue at the deepest level, which is absent in
some regions, where the lamina propria is
directly bound to the bone or muscle.
Oral Epithelium:
Thisis a highly organized, avascular, and
semipermeable tissue.
An interdigitated interface connects the
epithelium and the lamina propria.
The undulating projections of the deeper
layer of the epithelium, known as rete pegs,
attach to the underlying papillary
projections of the lamina propria.
Between these two tissues, there is a non-
cellular basement membrane to which the
epithelium is tightly bound.
The basement membrane provides support
to the epithelium and connects them to the
connective tissue.
It is seen as a line of demarcation between
the epithelium and connective tissue of the
lamina propria.
The oral mucosa is classified into three
types:
1- The lining mucosa:
Lines the mobile structures of the mouth.
It is found on the soft palate, cheeks, lips,
alveolar mucosa, the floor of the mouth,
and vestibular fornix.
It is covered by non-keratinized stratified
squamous epithelium.
2- The masticatory mucosa:
The rigid mucosa tightly bound to the
underlying bone.
In the attached gingiva and hard palate.
It is covered with a keratinized stratified
squamous epithelium; which provides the
better support during mastication.
3- Specialized mucosa:
On the dorsum of the tongue that shows
a stratified squamous epithelium that
receives different types of lingual papillae
and taste buds that allow taste perception.
Epithelium of Masticatory Mucosa:
Is a multilayered epithelium, Keratinocytes
constitute more than 95% of the epithelial
cells and they are arranged in four layers:
1-Basal layer(stratum basale):
Comprise stem and amplifying cells. These
cells sit on the basal membrane and provide
cell supply for above lying layers.
The cells are cuboidal and contain typical
organelles (mitochondria, ribosomes, ER,
Golgi).
2- Prickle cell layer : (stratum spinosum)
It has a prick-like appearance, which is
caused by numerous desmosomes that
connect the neighboring cells.
The cells polygonal in shape and contain all
regular organelles.
3- Granular cell layer (stratum
granulosum):
Consists of flatter cells that contain
keratinohyalin granules.
These granules are closely associated with
tonofilaments.
Tonofilaments and tonofibrils occupy large
regions of the cytoplasm.
Thus, cells comprise less organelles and
their nuclei show signs of degeneration.
4- Horny layer (stratum corneum) :
In this layer the cells dehydrate, lose their
organelles including the nucleus and are
completely filled with keratin until they
desquamates.
Epithelium of Lining Mucosa:
Organization of the epithelium differs from those at
the masticatory mucosa.
Although stratum basale und spinosum are largely
comparable.
Stratum intermedium is used instead of stratum
granulosum.
This stratum intermedium is characterized by no or
few keratohyalin granules.
It makes up the main layers of the epithelium and
The outermost superficial layer contains flatten cells
with an impaired number of organelles.
In contrast to stratifying epithelium, those cells stay
alive although their nuclei are shrunken and pyknotic.
Non-keratinocyte Cell Population:
Besides keratinocytes, other specialized
cells permanently reside within the oral
epithelium, referred to as non-keratinocyte
cells, including melanocytes, Langerhan
cells, and Merkel cells.
Melanocytes:
It is the melanin producing cells.
It lies between the basal keratinocytes.
It is derived from neural crest.
It is a dendritic cell. The dendrites transfer
melanin pigment to keratinocytes.
The ratio of melanocytes to keratinocytes in the oral
epithelium's ranges from 1:10 to 1:15.
The different skin colors and pigmentation of the
oral mucosa are determined by the size and quantity
of the melanosomes and the type of melanin
synthesized, eumelanin or pheomelanin.
With age, there is an increased extent and
intensity of oral pigmentations that are
considered physiological.
It is suspected that this augmentation may
result from cumulative possible
melanogenic stimuli such as inflammatory
conditions, medications, recurrent and mild
functional injuries, or smoking.
Langerhans Cells:
Dendritic cells derived from the bone marrow
that migrate to the oral epithelium, where they
reside within the stratum spinosum.
They function as antigen-presenting cells by
phagocytosing antigens in the epithelium and
migrating to the underlying lamina propria,
from where they can reach the regional lymph
nodes.
Here the antigenic peptides, are presented to T
cells.
Therefore, Langerhans cells are the link between
the oral mucosa and the immune system.
Merkel cells:
It is found in the basal layer.
It is considered a mechanoreceptor.
Lamina Propria:
Consists of cells, blood vessels, nerve fibers,
collagen and elastin fibres in an amorphous
ground substance, it reflects the dermis of the
skin.
It is formed 2 layers:
A superficial papillary layer: collagen fibers
are thin and loose organized.
The reticular layer: collagen fibers are thick and
often parallel to the surface.
Fibroblasts: are the cells that produce the
fibers and ground substance.
Other cells : macrophages and mast cells.
Submucosa:
Composed of loose fatty connective tissue,
minor salivary, glands, nerves and blood
vessels.
Not present in all parts of the oral cavity,
especially in masticatory mucosa, as the
lamina propria is directly attached to the
underlying bone.
Functions of the Oral Mucosa:
1- Protection: - Mechanical protection
- Barrier function
2- Perception: - Taste
- Temperature
- Mechano perception
(pressure, vibration)
3- Nutrition: - Mastication
- Absorption
4- Secretion: - Saliva
- Sebum
Keratinocytes constitute more than 95% of the
epidermal cells, they are arranged in four layers:
1- Basal cell layer :
- It's the lowermost layer.
- It's composed of a single row of columnar cells
and responsible for the formation of KCs.
2- Spinous (Prickle) cell layer:
Consists of 5-7 rows of polygonal cells.
3- Granular cell layer
Consists of 2-3 rows of flattened cells.
4- Horny (Keratinous) cell layer:
Consists of dead KCs (losing their nuclei).
STOMATITIS
Definition:
Stomatitis is inflammation of
the mucous membrane of the mouth,
including the inner aspect of the lips, cheeks,
gums, tongue, and throat.
It can be acute or chronic, mild or severe.
Symptoms of stomatitis:
It can present with:
Red patches
Mouth ulcers
Blisters
Swelling
Oral numbness
Soreness.
These can lead to dehydration and
malnutrition.
Causes stomatitis:
1- Bacterial infection
2- Fungal infection
3- Viral infection
4- Systemic disorder (Behcets, Pemphigus ,
nutritional deficiencies and Erythema
multiforme).
5- Drugs: ( methotrexate, chemoterapy)
6- Physical irritation ( theraml burns due to hot or
cold drinks) or (denture stomatitis).
7- Contact stomatitis: due to allergies or irritants .
8- Others: as SLE and Lichen planus.
Investigations:
It may include:
Bacterial swabs.
Viral swabs.
Tissue scrapings for fungal infections.
Biopsy for histology and
direct immunofluorescence.
Blood tests.
Patch test to identify contact allergy.
Treatment of stomatitis:
- Depends on the cause.
If it is due to allergy to a medication, the
medication must be promptly stopped.
Infections may require specific treatment
such as antibiotics or antifungals .
Nutritional deficiencies should be
corrected.
Systemic corticosteroids for immunologic
systemic diseases.
Symptomatic treatment: include:
Antiseptic mouthwashes.
Protective pastes
Local anaethetic mouthwashes or spray
Oral analgesics. (pain killers)
Topical or intralesional corticosteroids.
You might also like
- Dermatology Questions and AnsDocument147 pagesDermatology Questions and AnsEl FaroukNo ratings yet
- BAKER, William J. The Making of A Working-Class Football CultureDocument12 pagesBAKER, William J. The Making of A Working-Class Football CultureGabriela Marta Marques de Oliveira100% (1)
- Chapter 5 Cdi 1 Final EditedDocument16 pagesChapter 5 Cdi 1 Final EditedBelinda Viernes50% (2)
- Histology of Oral Mucous Membrane and GingivaDocument86 pagesHistology of Oral Mucous Membrane and GingivahazeemmegahedNo ratings yet
- Histologi Epitel Dan Mukosa Rongga Mulut-2021Document49 pagesHistologi Epitel Dan Mukosa Rongga Mulut-2021Cat cuteNo ratings yet
- Oral Mucous Membrane: by - Arindam MondalDocument92 pagesOral Mucous Membrane: by - Arindam MondalMohammed hisham khanNo ratings yet
- Oral Mucous Membrane: by - Arindam MondalDocument92 pagesOral Mucous Membrane: by - Arindam MondalMohammed hisham khanNo ratings yet
- Oral Mucous MembraneDocument200 pagesOral Mucous MembraneKush Pathak100% (3)
- Oral Mucosa: (Ten Cates)Document14 pagesOral Mucosa: (Ten Cates)Vanshika SethiNo ratings yet
- Oral Mucous MembraneDocument71 pagesOral Mucous MembraneHarleen GrewalNo ratings yet
- Oral Mucosa Oral MucosaDocument31 pagesOral Mucosa Oral Mucosaroqaia roqaiaNo ratings yet
- نسخة نسخة نسخة ريميDocument6 pagesنسخة نسخة نسخة ريميAhmed QahtaniNo ratings yet
- Cavum Oris Blok 3 PDFDocument63 pagesCavum Oris Blok 3 PDFShaffa Aprilia Amanda PutriNo ratings yet
- Cavum Oris & Salivary Gland Block 3Document63 pagesCavum Oris & Salivary Gland Block 3Muhammad HammamNo ratings yet
- Oral MucosaDocument109 pagesOral Mucosashahzeb memonNo ratings yet
- 11 Oral Mucous MembraneDocument53 pages11 Oral Mucous MembraneMohammed rezgallahNo ratings yet
- Oral Mucosa: Iryn A. LagartoDocument8 pagesOral Mucosa: Iryn A. LagartoVarenLagartoNo ratings yet
- 5 - Oral Mucosa and Salivary Glands (Mahmoud Bakr)Document115 pages5 - Oral Mucosa and Salivary Glands (Mahmoud Bakr)MobarobberNo ratings yet
- Periodontology Lec 2Document24 pagesPeriodontology Lec 2Ali MONo ratings yet
- نسخة PerioDocument6 pagesنسخة PerioAhmed QahtaniNo ratings yet
- Gingi VaDocument225 pagesGingi VaJoji IsacNo ratings yet
- Digestive System Part 1Document12 pagesDigestive System Part 1عبدالرحمن عدي عبدالفتاحNo ratings yet
- ANA 222 Intergumentry System HistologyDocument7 pagesANA 222 Intergumentry System HistologyprincessmakklisNo ratings yet
- Integumentary SystemDocument24 pagesIntegumentary SystemWadabiNo ratings yet
- Lecture Presented by:-ALI Waheed /yasmin Falah /zainab Mazin Supervised By:-Dr. Sattar Jabbar Jasim /cell and Tissue BiomedicalDocument24 pagesLecture Presented by:-ALI Waheed /yasmin Falah /zainab Mazin Supervised By:-Dr. Sattar Jabbar Jasim /cell and Tissue BiomedicalAli Waheed jolan100% (1)
- GENERAL HISTOLOGY pdf-1Document22 pagesGENERAL HISTOLOGY pdf-1Dany Samuel100% (1)
- Oral Mucous Membrane: DR Saurabh Juneja Professor and Head Dept of Oral Pathology SBBDCDocument54 pagesOral Mucous Membrane: DR Saurabh Juneja Professor and Head Dept of Oral Pathology SBBDCPuneet KaurNo ratings yet
- Vertebrate Integument and DerivativesDocument16 pagesVertebrate Integument and DerivativesNarasimha MurthyNo ratings yet
- Unit 5 Skin and Integumentary SystemDocument104 pagesUnit 5 Skin and Integumentary SystemSino McakoNo ratings yet
- Characteristics of Living Organisms and The Integumentary SystemDocument11 pagesCharacteristics of Living Organisms and The Integumentary SystemSHYRE COLEEN CATAYAONo ratings yet
- Lecture 2 Non Keratinizedmucosa Non KeratinocytesDocument29 pagesLecture 2 Non Keratinizedmucosa Non KeratinocytesAMIT GUPTANo ratings yet
- Piel NormalDocument17 pagesPiel NormalfrankyelitNo ratings yet
- Practical Class 5Document73 pagesPractical Class 5Chahinez HabibNo ratings yet
- Skin Structure and Function: Figure 1.1 Cross-Section of The SkinDocument11 pagesSkin Structure and Function: Figure 1.1 Cross-Section of The SkinfunmugNo ratings yet
- 11 B IntegumenttextDocument41 pages11 B IntegumenttextAbu Ibtihal OsmanNo ratings yet
- CHP 12 - Oral Mucosa-1Document83 pagesCHP 12 - Oral Mucosa-1Areej Fatima100% (2)
- Histology Structure of SkinDocument4 pagesHistology Structure of SkinLIEBERKHUNNo ratings yet
- Upper Git FinalDocument11 pagesUpper Git Finalgergeskamal020No ratings yet
- Oral Mucous MembraneDocument79 pagesOral Mucous MembraneKarthik MungamuriNo ratings yet
- Anatomy and PhysiologyDocument25 pagesAnatomy and PhysiologyNaidin Catherine De Guzman-AlcalaNo ratings yet
- Maya Tejasari Histology Department Faculty of Medicine Bandung Islamic UniversityDocument65 pagesMaya Tejasari Histology Department Faculty of Medicine Bandung Islamic UniversitydeasyahNo ratings yet
- Histo ALLDocument59 pagesHisto ALLoday25No ratings yet
- Chapter 1Document31 pagesChapter 1cabdinuux32No ratings yet
- Lit SkinStruct Bensouillah Ch01 PDFDocument11 pagesLit SkinStruct Bensouillah Ch01 PDFisaco1531012No ratings yet
- Digestive Tract: Esophagus, Stomach, Small and Large Intestines, Rectum, and Anus and ItsDocument10 pagesDigestive Tract: Esophagus, Stomach, Small and Large Intestines, Rectum, and Anus and Itsحوراء عارف الموسويNo ratings yet
- Meth Elab Topic N1Document23 pagesMeth Elab Topic N1Group M1869No ratings yet
- Skin LayersDocument3 pagesSkin LayersCrackmcat CrackmcatNo ratings yet
- Digestive SYSTEMDocument53 pagesDigestive SYSTEMPrincess AnnNo ratings yet
- IntegumentaryDocument7 pagesIntegumentarySimone ApostolNo ratings yet
- Oral Mucous Membrane (Oral Mucosa)Document7 pagesOral Mucous Membrane (Oral Mucosa)روان امير غني عبد عونNo ratings yet
- Lecture 27 - Histology of The Integumentary System 2Document89 pagesLecture 27 - Histology of The Integumentary System 2spitzmark2030No ratings yet
- 5 - Skin Mucous MembraneDocument32 pages5 - Skin Mucous MembranecheckmateNo ratings yet
- Skin and Body Membranes HahaDocument6 pagesSkin and Body Membranes Hahaقى قىNo ratings yet
- The Integumentary System and HomeostasisDocument9 pagesThe Integumentary System and HomeostasisJohn Paul ArcillaNo ratings yet
- EPITHELIUMDocument38 pagesEPITHELIUMAstridNo ratings yet
- Salivary GlandDocument112 pagesSalivary GlandSwati SawalNo ratings yet
- The Digestive System IDocument55 pagesThe Digestive System IYousef KhallafNo ratings yet
- IntegumentarysystemDocument99 pagesIntegumentarysystemkuro hanabusaNo ratings yet
- Tob 3.2Document33 pagesTob 3.2LT DRAGONXNo ratings yet
- 1.integumentary System - HistologyDocument34 pages1.integumentary System - Histologyqty9jgkpnzNo ratings yet
- Dermatology FirecrackerDocument28 pagesDermatology FirecrackerKeham LeogNo ratings yet
- Morphology of SKIN LesionsDocument32 pagesMorphology of SKIN LesionsLobna ElkilanyNo ratings yet
- 4 - (CHF), IschemicDocument31 pages4 - (CHF), IschemicLobna ElkilanyNo ratings yet
- 2 - RH Fev, Inf EndoDocument37 pages2 - RH Fev, Inf EndoLobna ElkilanyNo ratings yet
- 3 - Valvular Heart DiseasesDocument31 pages3 - Valvular Heart DiseasesLobna ElkilanyNo ratings yet
- 1 - HypertensionDocument35 pages1 - HypertensionLobna ElkilanyNo ratings yet
- Vonnegut 1st Printings W Numbers of Copies PrintedDocument6 pagesVonnegut 1st Printings W Numbers of Copies PrintedBrad BoothNo ratings yet
- Chapter2 PDFDocument88 pagesChapter2 PDFVanwesly Prayoga100% (1)
- Defense of The AncientsDocument3 pagesDefense of The AncientsNissa CleopatraNo ratings yet
- HIS3MHI - Silence Is Golden - Final EssayDocument5 pagesHIS3MHI - Silence Is Golden - Final EssaySascha McNulty100% (1)
- Research ReviewerDocument14 pagesResearch ReviewerSnowball MeowwNo ratings yet
- Erdogan Visits WashingtonDocument3 pagesErdogan Visits WashingtonPatrick SnellNo ratings yet
- Terrepedia: A Project Report For The Course Lean Startup Management (Mgt1022) Under The Guidance of Prof. Thiagarajan SDocument20 pagesTerrepedia: A Project Report For The Course Lean Startup Management (Mgt1022) Under The Guidance of Prof. Thiagarajan SSamyak DoshiNo ratings yet
- TNCT Q3ExamDocument7 pagesTNCT Q3ExamREY ANN RUBIONo ratings yet
- To BeDocument7 pagesTo BeSamuel Celedonio RodriguezNo ratings yet
- Kandiyoti. Women, Islam and The StateDocument8 pagesKandiyoti. Women, Islam and The StateArticulación ProvincialNo ratings yet
- Mindanao Community School, Inc.: Empowerment TechnologiesDocument11 pagesMindanao Community School, Inc.: Empowerment TechnologiesavinmanzanoNo ratings yet
- Microcontroller Based Automated Voltage Pulse TesterDocument3 pagesMicrocontroller Based Automated Voltage Pulse TesterInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- AeroShell Grease 7 PDFDocument2 pagesAeroShell Grease 7 PDFAnonymous oAbjbl4HNo ratings yet
- Summative Test English 8Document2 pagesSummative Test English 8Cristina SarmientoNo ratings yet
- Deleuze - Description of Woman For A Philosophy of The Sexed OtherDocument9 pagesDeleuze - Description of Woman For A Philosophy of The Sexed OtherMichael SchwartzNo ratings yet
- English 10-Q4-M7Document13 pagesEnglish 10-Q4-M7Joemar De Pascion NovillaNo ratings yet
- Flatpack McuDocument2 pagesFlatpack McuAVkucher1983No ratings yet
- The Misunderstood StorytellerDocument11 pagesThe Misunderstood Storyteller50_BMGNo ratings yet
- Guidance On The Compilation of Safety Data SheetsDocument138 pagesGuidance On The Compilation of Safety Data SheetsAlexEcnomNo ratings yet
- Wellbeing at Work A Practical GuideDocument38 pagesWellbeing at Work A Practical GuideFahad SiddiqNo ratings yet
- 2) There Was A Murder Last Night. What Were They Doing When The Murder Happened?Document2 pages2) There Was A Murder Last Night. What Were They Doing When The Murder Happened?Pilar Gonzalez PinillaNo ratings yet
- A Weavers Cooperative: A Boon To Weavers ... : Koustavi ChakrabortyDocument4 pagesA Weavers Cooperative: A Boon To Weavers ... : Koustavi ChakrabortyKoustavi ChakrabortyNo ratings yet
- Temple of GodDocument4 pagesTemple of GodNathan ChrisNo ratings yet
- Financial Highlights: Hinopak Motors LimitedDocument6 pagesFinancial Highlights: Hinopak Motors LimitedAli ButtNo ratings yet
- Ethics in PracticeDocument14 pagesEthics in PracticedanielktingNo ratings yet
- 09 Chapter IDocument45 pages09 Chapter ISYED TAYYABNo ratings yet
- Generate Visitors - Google DiscoverDocument8 pagesGenerate Visitors - Google DiscoverJohn CenaNo ratings yet
- Module Ramadan 3Document6 pagesModule Ramadan 3Darkant TnakradNo ratings yet