Professional Documents
Culture Documents
Respiratory Failure
Respiratory Failure
Uploaded by
Ayan Ali0 ratings0% found this document useful (0 votes)
22 views18 pagesRespiratory failure occurs when the respiratory system fails to maintain adequate gas exchange, resulting in low oxygen (hypoxemia) and/or high carbon dioxide (hypercapnia) levels in the blood. It is classified into two types: type 1 involves hypoxemia with normal or low carbon dioxide, often due to lung tissue damage. Type 2 involves both hypoxemia and hypercapnia (high carbon dioxide), usually due to insufficient breathing to remove carbon dioxide. Management involves treating the underlying cause, correcting hypoxemia with oxygen supplementation, and correcting hypercapnia/acidosis with ventilatory support either non-invasively or invasively with intubation if needed.
Original Description:
Original Title
Presentation (1) (2)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRespiratory failure occurs when the respiratory system fails to maintain adequate gas exchange, resulting in low oxygen (hypoxemia) and/or high carbon dioxide (hypercapnia) levels in the blood. It is classified into two types: type 1 involves hypoxemia with normal or low carbon dioxide, often due to lung tissue damage. Type 2 involves both hypoxemia and hypercapnia (high carbon dioxide), usually due to insufficient breathing to remove carbon dioxide. Management involves treating the underlying cause, correcting hypoxemia with oxygen supplementation, and correcting hypercapnia/acidosis with ventilatory support either non-invasively or invasively with intubation if needed.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
22 views18 pagesRespiratory Failure
Respiratory Failure
Uploaded by
Ayan AliRespiratory failure occurs when the respiratory system fails to maintain adequate gas exchange, resulting in low oxygen (hypoxemia) and/or high carbon dioxide (hypercapnia) levels in the blood. It is classified into two types: type 1 involves hypoxemia with normal or low carbon dioxide, often due to lung tissue damage. Type 2 involves both hypoxemia and hypercapnia (high carbon dioxide), usually due to insufficient breathing to remove carbon dioxide. Management involves treating the underlying cause, correcting hypoxemia with oxygen supplementation, and correcting hypercapnia/acidosis with ventilatory support either non-invasively or invasively with intubation if needed.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 18
Respiratory Failure
Respiratory failure is a clinical condition that happens when the
respiratory system fails to maintain its main function, which is
gas exchange, in which PaO2 is lower than 60 mmHg and/or
PaCO2 higher than 50 mmHg.
Respiratory failure is classified according to blood gases
abnormalities into type 1 and type 2.
Type 1 - (hypoxemic) respiratory failure has a PaO2 < 60
mmHg with normal or subnormal PaCO2. In this type, the gas
exchange is impaired at the level of aveolo-capillary membrane.
Examples of type I respiratory failures are carcinogenic or non-
cardiogenic pulmonary edemaa, ARDs, COVID-19 and severe
pneumonia.
Type 2 - (hypercapnic) respiratory failure has a PaCO2 > 50
mmHg. Hypoxemia is common, and it is due to respiratory
pump failure.
•RF a major cause of mortality and morbidity and mortality
rates increase with age and presence of co-morbidities.
PATHOPHYSIOLOGY
Hypoventilation: in which PaCO2 and PaO2 and alveolar-arterial PO2 gradient (difference
between the calculated oxygen pressure available in the alveolus and the arterial oxygen tension,
measures the efficiency of gas exchange). are normal. Depression of CNS from drugs (eg
opiod use disorder) is an example of this condition.
V/P mismatch: this is the most common cause of hypoxemia. Administration of 100% O2
eliminates hypoxemia.
In respiratory physiology, the ventilation/perfusion ratio (V̇/Q̇ ratio or V/Q ratio) is a ratio used to
assess the efficiency and adequacy of the matching of two variables:V (ventilation) the air that
reaches the alveoli; Q (perfusion) the blood that reaches the alveoli via the capillaries. V/Q ratio is
defined as the ratio of the amount of air reaching the alveoli per minute to the amount of blood
reaching the alveoli per minute. These two variables, V & Q, constitute the main determinants of the
blood oxygen (O2) and carbon dioxide (CO2) concentration.
1.Type I respiratory failure involves low oxygen, and normal or
low carbon dioxide levels. Occurs because of damage to lung
tissue eg including pulmonary oedema, pneumonia, acute
respiratory distress syndrome, and chronic pulmonary fibrosing
alveoloitis. This lung damage prevents adequate oxygenation of
the blood (hypoxaemia); however, the remaining normal lung is
still sufficient to excrete the carbon dioxide being produced by
tissue metabolism. This is possible because less functioning
lung tissue is required for carbon dioxide excretion than is
needed for oxygenation of the blood.
Type II respiratory failure involves low oxygen, with high carbon dioxide (pump
failure). It occurs when alveolar ventilation is insufficient to excrete the carbon
dioxide being produced. The most common cause is chronic obstructive pulmonary
disease (COPD). Others include chest-wall deformities, respiratory muscle weakness
(e.g. Guillain-Barre syndrome) and central depression of the respiratory centre (e.g.
heroin overdose) Inadequate ventilation is due to reduced ventilatory effort, or
inability to overcome increased resistance to ventilation – it affects the lung as a
whole, and thus carbon dioxide accumulates. Complications include: damage to vital
organs due to hypoxaemia, CNS depression due to increased carbon dioxide levels,
respiratory acidosis (carbon dioxide retention). This is ultimately fatal unless treated.
Complications due to treatment may also occur.
Epidemiology
Overall frequency of respiratory failure is not well known as
respiratory failure is a syndrome not a single disease process
Respiratory failure may be due to pulmonary or extra-
pulmonary causes which include:
1-CNS causes due to depression of the neural drive to breath as
in cases of overdose of a narcotic and sedative.
2-Disorders of the peripheral nervous system: Respiratory
muscle and chest wall weakness as in cases of Guillian-Barre
syndrome and myasthenia gravis.
3-Upper and lower airways obstruction: due to various
causes as in cases of exacerbation of
chronic obstructive pulmonary diseases and acute severe
bronchial asthma
4-Abnormities of the alveoli that result in type 1 (hypoxemic)
respiratory failure as in cases of pulmonary edema and severe
pneumonia
Clinical Presentation
Presentation of respiratory failure is dependent on the
underlying cause and associated hypoxemia or hypercapnia.
Common presentations include:
•Dyspnoea
•Tachypnoea
•Restlessness
•Confusion
•Anxiety
•Cyanosis- central
•Tachycardia
•Pulmonary hypertension
•Loss of consciousness
Signs and symptoms of RF Type I (Hypoxemia) include:
•Dyspnea, irritability
•Confusion, fits, somnolence
•Tachycardia, arrhythmia
•Tachypnea
•Cyanosis
Signs and symptoms of RF Type II (Hypercapnia) include
•Change of behavior
•headache
•Coma
•Warm extremities
•Astrexis
•Papilloedema
Symptoms and signs of the underlying disease:eg
•Fever, cough, sputum production, chest pain in cases of
pneumonia.
•History of sepsis, polytrauma, burn, or blood transfusions
before the onset of acute respiratory failure may point to
acute respiratory distress syndrome
Evaluation:
Arterial blood gases- measures oxygen and carbon dioxide levels in the blood
Renal function tests and liver function tests- may indicate the etiology of respiratory failure or identify
complications associated with it.
Pulmonary Function Test- identifies obstruction, restriction, and gas diffusion abnormalities. Normal values
for forced expiratory volume in 1 second(FEV1) and forced vital capacity(FVC) suggest a disturbance in
respiratory control. Decrease in FEV1 to FVC ratio indicates airflow obstruction. A decrease in FEV1 and
FVC and maintenance of FEV1 to FVC ratio suggest restrictive lung disease.
Electrocardiography(ECG)
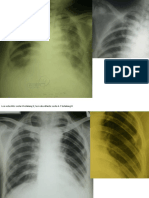
Chest radiography is needed as it can detect chest wall, pleural and lung parenchymal Lesions.
Other investigations needed for detecting the underlying cause of the respiratory failure may include:
Complete blood count (CBC)
Sputum, blood and urine culture
Blood electrolytes and thyroid function tests
Echocardiography
Bronchoscopy
Complications:
Pulmonary: pulmonary embolism, pulmonary fibrosis, complications secondary to the
use of mechanical ventilator
Cardiovascular: hypotension, reduced cardiac output, cor pulmonale, arrhythmias,
pericarditis and acute myocardial infarction
Gastrointestinal: haemorrhage, gastric distention, ileus, diarrhoea, pneumoperitoneum
and duodenal ulceration- caused by stress is common in patients with acute respiratory
failure
Infectious: noscomial- pneumonia, urinary tract infection and catheter-related sepsis.
Usually occurs with use of mechanical devices.
Renal: acute renal failure, abnormalities of electrolytes and acid-base balance.
Nutritional: malnutrition and complications relating to parenteral or enteral nutrition
and complications associated with NG tube- abdominal distention and diarrhea
MANAGEMENT
1-Correction of Hypoxemia
•The goal is to maintain adequate tissue oxygenation, generally
achieved with an arterial oxygen tension (PaO2) of 60 mm Hg
or arterial oxygen saturation (SaO2), about 90%.
•Un-controlled oxygen supplementation can result in oxygen
toxicity and CO2 (carbon dioxide) narcosis. Inspired oxygen
concentration should be adjusted at the lowest level, which is
sufficient for tissue oxygenation.
•Oxygen can be delivered by several routes depending on the
clinical situations in which we may use a nasal cannula, simple
face mask nonrebreathing mask, or high flow nasal cannula.
•Extracorporeal membrane oxygenation may be needed in
refractory cases
2-Correction of hypercapnia and respiratory acidosis
•This may be achieved by treating the underlying cause or
providing ventilatory support.
3. Ventilatory support for the patient with respiratory
failure
The goals of ventilatory support in respiratory failure are:
•Correct hypoxemia
•Correct acute respiratory acidosis
•Resting of ventilatory muscles.
Non-invasive respiratory support: is ventilatory support
without tracheal intubation/ via upper airway. Considered in
patients with mild to moderate respiratory failure. Patients
should be conscious, have an intact airway and airway
protective reflexes. Noninvasive positive pressure ventilation
(NIPPV) has been shown to reduce complications, duration of
ICU stay and mortality(). It has been suggested that NIPPV is
more effective in preventing endotracheal intubation in acute
respiratory failure due to COPD than other causes. The etiology
of respiratory failure is an important predictor of NIPPV failure
Invasive respiratory support: indicated in persistent
hypoxemia despite receiving maximum oxygen therapy,
hypercapnia with impairment of conscious level. Intubation is
associated with complications such as aspiration of gastric
content, trauma to the teeth, barotraumas, trauma to the trachea
etc
You might also like
- Nursing Care PlansDocument48 pagesNursing Care PlansJuliantiMamangkey86% (7)
- HRCT Pattern Recognition and Differential Diagnosis of Lung DiseaseDocument111 pagesHRCT Pattern Recognition and Differential Diagnosis of Lung DiseaseSrba100% (2)
- Respiratory System - ReviewerDocument8 pagesRespiratory System - ReviewerEva Marie GaaNo ratings yet
- Lab Report Bio Experiment 3 - Reproductive, Endocrine & Respiratory System (Group 4)Document15 pagesLab Report Bio Experiment 3 - Reproductive, Endocrine & Respiratory System (Group 4)FARHAH BATRISYIA ABDUL RAHIMNo ratings yet
- Respiratory FailureDocument8 pagesRespiratory FailureAnusha VergheseNo ratings yet
- RESPIRATORY FAILUREnewDocument26 pagesRESPIRATORY FAILUREnewmerin sunilNo ratings yet
- Cystic Fibrosis Disease Process WorksheetDocument4 pagesCystic Fibrosis Disease Process WorksheetDan Gil EstadillaNo ratings yet
- Lo Tropmed 1Document49 pagesLo Tropmed 1belleNo ratings yet
- Classification of Respiratory FailureDocument8 pagesClassification of Respiratory Failurerau_rauNo ratings yet
- Respiratory Failure: Barry WardleDocument28 pagesRespiratory Failure: Barry Wardleapi-19826220No ratings yet
- Acute Respiratory FailureDocument14 pagesAcute Respiratory FailureMahmoud KittNo ratings yet
- Respiratory FailureDocument41 pagesRespiratory FailureM HNo ratings yet
- Respiratory FailureDocument10 pagesRespiratory FailureharvardboyNo ratings yet
- RF - TypesDocument9 pagesRF - Typesjsamrnmd.ffiedNo ratings yet
- Respiratory Failure PDFDocument5 pagesRespiratory Failure PDFOxana Turcu100% (1)
- Kaynar2018 Medscape PDFDocument29 pagesKaynar2018 Medscape PDFberlianNo ratings yet
- Respiratory FailureDocument39 pagesRespiratory FailureMuntasir BashirNo ratings yet
- Respiratory Failure (1) .Document36 pagesRespiratory Failure (1) .Ibrahim HemdanNo ratings yet
- Respiratory Failure: Dr. Sat Sharma Univ of ManitobaDocument38 pagesRespiratory Failure: Dr. Sat Sharma Univ of ManitobaGonzalo Venegas RojasNo ratings yet
- Acute Respiratory Distress Syndrome (Ards) : Muamar Aldalaeen, RN, Mba, HCRM, Cic, Ipm, MSN, Phd. Haneen Alnuaimi, MSNDocument59 pagesAcute Respiratory Distress Syndrome (Ards) : Muamar Aldalaeen, RN, Mba, HCRM, Cic, Ipm, MSN, Phd. Haneen Alnuaimi, MSNAboodsha ShNo ratings yet
- Acute Respiratory Failure: R. Bhakialakshmi M.Sc. Nursing 2 Year PSG College of NursingDocument31 pagesAcute Respiratory Failure: R. Bhakialakshmi M.Sc. Nursing 2 Year PSG College of NursingassumptaNo ratings yet
- PBL #4 Respiratory Failure "Group A"Document57 pagesPBL #4 Respiratory Failure "Group A"mohammedNo ratings yet
- Acute Respiratory FailureDocument29 pagesAcute Respiratory FailurePurnima ChoudhuryNo ratings yet
- Acute Respiratory Failure 1Document7 pagesAcute Respiratory Failure 1Trish 0019No ratings yet
- Pathophysiologyofrespiratoryfailurefinal 130628075619 Phpapp01Document50 pagesPathophysiologyofrespiratoryfailurefinal 130628075619 Phpapp01Eller Tacud CollantesNo ratings yet
- Plasma University: Guriel-Galgadud RegionDocument17 pagesPlasma University: Guriel-Galgadud RegionDr AbdulkadirNo ratings yet
- Acute RFDocument7 pagesAcute RFLoren SangalangNo ratings yet
- Respiratory FailureDocument7 pagesRespiratory FailureJesse OnealNo ratings yet
- Respiration 16 Respiratory FailureDocument31 pagesRespiration 16 Respiratory Failureapi-19641337No ratings yet
- Acute Respiratory FailureDocument8 pagesAcute Respiratory FailureCayunk NorlianaNo ratings yet
- Article 301574-PrintDocument17 pagesArticle 301574-PrintRo RyNo ratings yet
- 1 RespiratoryFailureDocument60 pages1 RespiratoryFailureZainab HaniNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD)Document32 pagesChronic Obstructive Pulmonary Disease (COPD)matrixtrinityNo ratings yet
- Acute Respiratory Distress SyndromeDocument38 pagesAcute Respiratory Distress SyndromeMohamed HamdyNo ratings yet
- Respiratory Failure: by ArDocument39 pagesRespiratory Failure: by ArAleksei RomahovNo ratings yet
- Acute Respiratory Failure LectureDocument53 pagesAcute Respiratory Failure Lectureprototypeallhell100% (2)
- Running A Race at 12,000 FeetDocument39 pagesRunning A Race at 12,000 FeetAndela Ernesto HenriqueNo ratings yet
- Respiratory System: Oleh H. Errrasmus SoerasdiDocument12 pagesRespiratory System: Oleh H. Errrasmus SoerasdiAndi TurmudziNo ratings yet
- Quick Review of Some Medical TopicsDocument40 pagesQuick Review of Some Medical TopicsdoctormussieaberraNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument8 pagesChronic Obstructive Pulmonary DiseaseYessamin Paith RoderosNo ratings yet
- Pulmonary FailureDocument29 pagesPulmonary FailureWengel RedkissNo ratings yet
- Pathophysiology: Hypoxemic Respiratory FailureDocument6 pagesPathophysiology: Hypoxemic Respiratory FailurevidagurlNo ratings yet
- Acute Respiratory Failure - Approach To The Patient - DynaMedDocument114 pagesAcute Respiratory Failure - Approach To The Patient - DynaMedJosé Ángel Castillo ContrerasNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDocument12 pagesChronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDiana Jalaynie S. SambolawanNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDocument12 pagesChronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDiana Jalaynie S. SambolawanNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument12 pagesChronic Obstructive Pulmonary DiseaseibegbunamchinemeremNo ratings yet
- M V ICU: Echanical Entilation INDocument82 pagesM V ICU: Echanical Entilation INabhilashreddy45No ratings yet
- Basics of Mechanical Ventilation For Dogs and Cats PDFDocument15 pagesBasics of Mechanical Ventilation For Dogs and Cats PDFFelipe GonzalezNo ratings yet
- Hypoxemic Resp. FailureDocument52 pagesHypoxemic Resp. FailureLovely Acabado TampocoNo ratings yet
- Pemicu 6 KGD AldiDocument134 pagesPemicu 6 KGD AldiFirdaus AldyNo ratings yet
- ARDSDocument23 pagesARDSDumora FatmaNo ratings yet
- Respiratory Failure Workup: Approach ConsiderationsDocument8 pagesRespiratory Failure Workup: Approach Considerationsjeanie mae PangapalanNo ratings yet
- Copd-1 2023Document38 pagesCopd-1 2023grim reaperNo ratings yet
- ArdsDocument48 pagesArdsvmalik985No ratings yet
- Acute Respiratory Distress SyndromeDocument17 pagesAcute Respiratory Distress SyndromeSanjeet Sah100% (1)
- Alkalosis RespiratorikDocument4 pagesAlkalosis RespiratorikTony YuliantoNo ratings yet
- 4-1pulmonary DisordersDocument38 pages4-1pulmonary DisordersAbdallah AlasalNo ratings yet
- COPDs DR Moses KazevuDocument30 pagesCOPDs DR Moses KazevuMoses Jr KazevuNo ratings yet
- ACUTE RESPIRATORY DISTRESS SYNDROME by Dr. Monday ZaccheausDocument59 pagesACUTE RESPIRATORY DISTRESS SYNDROME by Dr. Monday ZaccheausDr. Amb. Monday ZaccheausNo ratings yet
- Restrictive and Obstructive Pulmonary DiseasesDocument10 pagesRestrictive and Obstructive Pulmonary DiseasesJANELLE GIFT SENARLONo ratings yet
- Go To:: Indications For Mechanical VentilationDocument25 pagesGo To:: Indications For Mechanical VentilationsakuraleeshaoranNo ratings yet
- Respiratory FailureDocument4 pagesRespiratory FailureMeey Mee100% (1)
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- Respiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsFrom EverandRespiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsJian-Xin ZhouNo ratings yet
- EmpyemaDocument13 pagesEmpyemaAyan AliNo ratings yet
- Pleurisy (PleuritisDocument11 pagesPleurisy (PleuritisAyan AliNo ratings yet
- Ischemic Heart Disease CADDocument22 pagesIschemic Heart Disease CADAyan AliNo ratings yet
- PresentationDocument5 pagesPresentationAyan AliNo ratings yet
- TuberclosisDocument16 pagesTuberclosisAyan AliNo ratings yet
- Anatomy of Pelvis PresentationDocument21 pagesAnatomy of Pelvis PresentationAyan AliNo ratings yet
- Case Emfisema ParuDocument3 pagesCase Emfisema ParuMuhammad SyukurNo ratings yet
- Bronchiolitis in ChildrenDocument16 pagesBronchiolitis in ChildrenNym Angga Santosa100% (1)
- Respiration: Mechanics of BreathingDocument3 pagesRespiration: Mechanics of BreathingTrajkovskaNo ratings yet
- Nursing Care Plan: Lopez, Maria Sofia B. 9/29/2020 3-BSN-B Prof. ZoletaDocument5 pagesNursing Care Plan: Lopez, Maria Sofia B. 9/29/2020 3-BSN-B Prof. ZoletaSofiaLopezNo ratings yet
- Tracheobronchial TreeDocument51 pagesTracheobronchial TreeravishNo ratings yet
- 27 Acvtivity SheetDocument6 pages27 Acvtivity SheetHart OlpendaNo ratings yet
- Lesi Osteolitic Costa 6 Belakang S Lesi Osteoblastic Costa 6-7 Belakang DDocument48 pagesLesi Osteolitic Costa 6 Belakang S Lesi Osteoblastic Costa 6-7 Belakang DLusi MunawarohNo ratings yet
- Diseases of External Nose & Nasal SeptumDocument20 pagesDiseases of External Nose & Nasal Septumggg225201No ratings yet
- Respiratory System ReviewerDocument7 pagesRespiratory System ReviewerDaniel DanielNo ratings yet
- Pedia ReviewDocument22 pagesPedia ReviewDebbie LanceroNo ratings yet
- Nigeria Certificate in Education Science ProgrammeDocument215 pagesNigeria Certificate in Education Science Programmemuhammadbinali77_465No ratings yet
- College Chemistry Lab (CHEM 120L) List of Chemicals: Acetic Acid, 20%Document4 pagesCollege Chemistry Lab (CHEM 120L) List of Chemicals: Acetic Acid, 20%Farah AhmadNo ratings yet
- Chapter 20 REVIEW OF THORACIC IMAGINGDocument8 pagesChapter 20 REVIEW OF THORACIC IMAGINGZahra Margrette SchuckNo ratings yet
- Anatomy Chapter 23 Respiratory SystemDocument86 pagesAnatomy Chapter 23 Respiratory SystemLagunamedical PharmacyNo ratings yet
- Breathing ExerciseDocument29 pagesBreathing ExerciseJawad Mohammad100% (1)
- Study GuideDocument17 pagesStudy GuideKellie PacanowskiNo ratings yet
- Noninvasive Strategies For Management of Respiratory Problems in NeonatesDocument12 pagesNoninvasive Strategies For Management of Respiratory Problems in NeonatesGaby RiveraNo ratings yet
- Pleural EffusionDocument4 pagesPleural Effusionrezairfan221No ratings yet
- Physical Education Class 11 Short Answers Chapter 8Document3 pagesPhysical Education Class 11 Short Answers Chapter 8Peyush NeneNo ratings yet
- Ingles StudyDocument23 pagesIngles StudyMatiasUrraNo ratings yet
- MSDS - Premix Marine ClearDocument7 pagesMSDS - Premix Marine CleargmNo ratings yet
- Zoo HandbookDocument50 pagesZoo HandbookSakinat MuhammadNo ratings yet
- X Class Diagram Based QuestionsDocument12 pagesX Class Diagram Based QuestionsAnonymous XYRuJZNo ratings yet
- Jawapan Strategi A - Sains Tingkatan 3Document159 pagesJawapan Strategi A - Sains Tingkatan 3helenafrancis245No ratings yet
- Makalah Bhs Inggris Sistem RespirasiDocument13 pagesMakalah Bhs Inggris Sistem RespirasiDewa Ayu Made FebriariNo ratings yet