Professional Documents
Culture Documents
Chapter 020
Chapter 020
Uploaded by
Mar3RDi Music0 ratings0% found this document useful (0 votes)
11 views54 pagesOriginal Title
Chapter_020 (1)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
11 views54 pagesChapter 020
Chapter 020
Uploaded by
Mar3RDi MusicCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 54
Chapter 20
Heart and Neck Vessels
Copyright © 2020 by Elsevier Inc. All rights reserved.
Position and Surface Landmarks
Precordium: area on anterior chest overlying heart and
great vessels
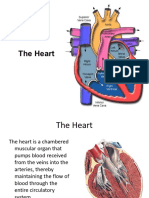
Heart has four chambers:
Atria and ventricles
Great vessels: major arteries and veins connected to the
heart
Blood vessels arranged in two continuous loops:
Pulmonary circulation and systemic circulation
Copyright © 2020 by Elsevier Inc. All rights reserved.
Precordium, Apex, and Base
Copyright © 2020 by Elsevier Inc. All rights reserved.
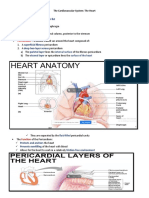
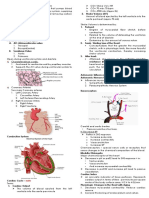
Heart Wall, Chambers, and Valves
Heart wall has numerous layers.
Pericardium: tough, fibrous, double-walled sac that surrounds
and protects heart
Myocardium: muscular wall of heart
Endocardium: thin layer of endothelial tissue that lines inner
surface of heart chambers and valves
Heart has two pump systems.
Each side of the heart has an atrium and a ventricle.
Atrium: thin-walled reservoir for holding blood
Ventricle: thick-walled, muscular pumping chamber
Copyright © 2020 by Elsevier Inc. All rights reserved.
Heart Chambers and Valves
Four chambers separated by valves, whose
main purpose is to prevent backflow of blood
Valves are unidirectional.
Valves open and close passively in response to
pressure gradients in moving blood.
Four valves in heart:
Two atrioventricular (AV) valves
Two semilunar (SL) valves
Copyright © 2020 by Elsevier Inc. All rights reserved.
AV Valves
Two AV valves separate atria and ventricles:
Tricuspid valve: right AV valve
Bicuspid, or mitral valve: left AV valve
• Valves’ thin leaflets are anchored by collagenous fibers
(chordae tendineae) to papillary muscles embedded in
ventricle floor.
AV valves open during heart’s filling phase, or
diastole, to allow ventricles to fill with blood.
During pumping phase, or systole, AV valves close to
prevent regurgitation of blood back up into atria.
Copyright © 2020 by Elsevier Inc. All rights reserved.
SL Valves
SL valves are set between ventricles and arteries.
Each valve has three cusps that look like half moons.
Pulmonic valve: SL valve in right side of heart
Aortic valve: SL valve in left side of heart
• Open during pumping, or systole, to allow blood to be ejected
from heart
No valves are present between vena cava and right atrium, or
between pulmonary veins and left atrium:
• Abnormally high pressure in left side of heart gives a person
symptoms of pulmonary congestion.
• Abnormally high pressure in right side of heart shows in neck
veins and abdomen.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Chambers and Valves
Copyright © 2020 by Elsevier Inc. All rights reserved.
Direction of Blood Flow
Unoxygenated red blood drains into vena cava, follows
route of venous blood.
From liver to right atrium (RA) through inferior vena cava
From RV, venous blood flows through pulmonic valve to
pulmonary artery.
Lungs oxygenate blood.
From left atrium (LA), arterial blood travels through mitral valve
to left ventricle (LV).
From LA, arterial blood travels through mitral valve to LV.
Aorta delivers oxygenated blood to body.
Circulation is continuous loop; moving by continuous shifting
pressure gradients.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Route of Blood Flow
Copyright © 2020 by Elsevier Inc. All rights reserved.
Cardiac Cycle
Diastole: ventricles relax and fill with blood; 2/3 of cardiac cycle
Protodiastolic filling: early passive phase
Presystole or atrial systole: atrial kick
Systole: heart’s contraction, blood pumped from ventricles fills
pulmonary and systemic arteries; 1/3 of cardiac cycle
Note that atrial systole occurs during ventricular diastole, a
confusing but important point.
For a very brief moment, all four valves are closed and ventricular walls
undergo:
• Isometric contraction: this contraction against closed system works to build
high level pressure in ventricles
• Isometric relaxation: all four valves closed and ventricles relax
Same events occur on both sides of heart.
Right side requires lower pressure and sequence occurs slightly later.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Heart Sounds
First heart sound (S1)
Occurs with closure of AV valves—signals beginning of systole
Mitral component of first sound (M1) slightly precedes tricuspid
component (T1).
Second heart sound (S2)
Occurs with closure of semilunar valves—signals end of systole
Aortic component of second sound (A2) slightly precedes pulmonic
component (P2).
• S2 loudest at base
Effects of respiration
Volume of right and left ventricular systole is just about equal but can be
affected by respiration.
Consider phrase: MoRe to the Right heart, Less to the Left
Copyright © 2020 by Elsevier Inc. All rights reserved.
Extra Heart Sounds
Third heart sound (S3)
Occurs when ventricles resistant to filling during early
rapid filling phase (protodiastole)
Occurs immediately after S2, when AV valves open
and atrial blood first pours into ventricles.
Fourth heart sound (S4)
Occurs at end of diastole, at presystole, when
ventricle resistant to filling
S4 occurs just before S1.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Extra Heart Sounds: Murmurs
Gentle, blowing, swooshing sound that can be
heard on chest wall
Conditions that create turbulent blood flow and
collision currents
Conditions that can result in murmurs:
Velocity of blood increases.
Viscosity of blood decreases.
Structural defects in valves
Copyright © 2020 by Elsevier Inc. All rights reserved.
Characteristics of Sound
All heart sounds are described by:
Frequency or pitch: high or low
Intensity or loudness: loud or soft
Duration: very short for heart sounds; silent periods
are longer
Timing: systole or diastole
Copyright © 2020 by Elsevier Inc. All rights reserved.
Conduction
Heart has unique ability: automaticity
Can contract by itself, independent of any signals or
stimulation from body
Contracts in response to an electrical current
conveyed by a conduction system
Specialized cells in sinoatrial (SA) node, near
superior vena cava initiate an electric impulse.
Because SA node has intrinsic rhythm, it is called the
pacemaker.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Electrocardiograph (ECG)
ECG waves arbitrarily labeled PQRST, which stand for
P wave: depolarization of atria
P-R interval: from beginning of P wave to beginning of
QRS complex (time necessary for atrial depolarization plus time
for impulse to travel through AV node to ventricles)
QRS complex: depolarization of ventricles
T wave: repolarization of ventricles
Electrical events slightly precede mechanical events in
heart.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Pumping Ability
Cardiac output: In resting adult, heart normally pumps between 4
and 6 L of blood per minute throughout body
CO= HR x SV
Heart can alter its cardiac output to adapt to metabolic needs of body.
Preload and afterload affect heart’s ability to increase cardiac output.
Preload: venous return that builds during diastole
According to Frank-Starling law, greater the stretch, the stronger the
heart’s contraction.
This increased contractility results in an increased volume of blood
ejected, increased stroke volume.
Afterload: opposing pressure ventricle must generate to open aortic
valve against higher aortic pressure
Resistance against which ventricle must pump its blood
Copyright © 2020 by Elsevier Inc. All rights reserved.
Neck Vessels
Carotid artery pulse
Note characteristics of its waveform.
• Smooth rapid upstroke
• Summit rounded and smooth
• Downstroke more gradual and has a dicrotic notch caused
by closure of aortic valve
Jugular Venous pulse and pressure
Empty unoxygenated blood directly into superior vena
cava.
Two jugular veins present on each side of neck.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Jugular Pulse: Five Components
A wave reflects atrial contraction because some blood flows
backward to vena cava during right atrial contraction.
C wave, or ventricular contraction, is backflow from bulging
upward of tricuspid valve when it closes at beginning of
ventricular systole.
X wave descent shows atrial relaxation when right ventricle
contracts during systole and pulls bottom of atria downward.
V wave occurs with passive atrial filling because of increasing
volume in right atria and increased pressure.
Y descent reflects passive ventricular filling when tricuspid
valve opens and blood flows from RA to RV.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Developmental Competence
Pregnant woman
Blood volume increases by 30% to 40% during pregnancy.
Despite increased cardiac output, arterial blood pressure
decreases in pregnancy as a result of peripheral vasodilation.
Infants and children
Fetal heart begins to beat after 3 weeks’ gestation.
Inflation and aeration of lungs at birth produces circulatory
changes.
Aging adult
Closely interrelated with lifestyle, habits, and diseases
Lifestyle, smoking, diet, alcohol use, exercise patterns, and
stress have an influence on coronary artery disease.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Hemodynamic Changes with
Aging (1 of 2)
Pressure/pulse changes
Isolated systolic HTN: Increase in systolic BP due to
thickening and stiffening of the arteries
Left ventricular wall becomes thicker but the overall
size of the heart does not change.
Pulse pressure increases.
No change in resting heart rate or cardiac output at
rest
Ability of heart to augment cardiac output with
exercise is decreased.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Hemodynamic Changes with
Aging (2 of 2)
Dysrhythmias
Presence of supraventricular and ventricular dysrhythmia increases
with age.
Ectopic beats common in aging people; usually asymptomatic in healthy
older people, may compromise cardiac output and blood pressure when
disease present
Tachyarrhythmias may not be tolerated as well in older people.
Electrocardiogram:
Occur as result of histologic changes in conduction system; these
changes include:
• Prolonged P-R interval (first-degree AV block) and prolonged Q-T interval,
but the QRS interval is unchanged
• Left axis deviation from age-related mild LV hypertrophy and fibrosis in left
bundle branch
• Increased incidence of bundle branch block
Copyright © 2020 by Elsevier Inc. All rights reserved.
Cardiac Disease and Aging Adult
Incidence of coronary artery disease increases sharply
with advancing age and accounts for about half of
deaths of older people.
Hypertension and heart failure also increase with age.
Lifestyle habits play a significant role in the acquisition of heart
disease.
Increasing the physical activity of older adults associated
with a reduced risk for death from cardiovascular
diseases and respiratory illnesses
Both points underscore need for health teaching as an
important treatment parameter.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Culture and Genetics
CVD: most common underlying cause of death globally
CVD data have a geographic difference
Although all adults have some potential CVD risk, some groups,
defined by race, ethnicity, gender, socioeconomic status, and
educational level carry an excess burden of CVD.
Recommend favorable lifestyle: no current smoking, no obesity, physical
activity at least once a week and a healthy diet
Consider access to care
Risk factors - Identification, early treatment, and health promotion:
HTN
Smoking
Serum cholesterol
Physical activity
Sex and gender differences
Copyright © 2020 by Elsevier Inc. All rights reserved.
Subjective Data
Chest pain
Dyspnea
Orthopnea
Cough
Fatigue
Cyanosis or pallor
Edema
Nocturia
Past cardiac history
Family cardiac history
Patient-centered care(cardiac risk factors)
Copyright © 2020 by Elsevier Inc. All rights reserved.
Chest Pain Questions
Any chest pain or tightness? Ask about
onset and location.
characteristics.
precipitating events.
associated symptoms.
relieved by or made worse by.
medication or treatments.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Dyspnea Questions
Any shortness of breath? Ask about
type of activity and occurrence.
onset and duration.
affect of positional changes and interruption of sleep.
presence of orthopnea.
affect ADLs.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Questions: Cough and Fatigue
Do you have a cough? Ask about
duration and frequency.
characteristics of type and productive versus non-productive.
affect of positional change.
affect ADLS.
alleviating factors or precipitating factors.
medications or treatments.
Do you seem to tire easily? Ask about
onset and any recent changes in energy level.
r/t time of day.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Additional Subjective History
Questions
Ask about occurrence of
orthopnea.
cyanosis or pallor.
nocturia.
Edema
Onset and timing
Amount and location
Relief of symptoms
Presence of associated symptoms
Copyright © 2020 by Elsevier Inc. All rights reserved.
Cardiac History Questions
Ask about
past cardiac history- medical and surgical.
diagnostic testing and imaging studies.
family history.
Patient-centered care: determine information relative to
patient history for:
Nutrition
Smoking
Alcohol
Exercise
Medication
Copyright © 2020 by Elsevier Inc. All rights reserved.
Additional History:
Infants, Children and Pregnant Women
Infants
Maternal health: How was mother’s health during pregnancy?
Feeding pattern: Any cyanotic changes during nursing or crying?
Growth and activity: Meeting developmental outcomes?
Children
Growth and activity: Meeting developmental outcomes?
Evidence of any chest pain?
History of respiratory infections
Significant family history—genetic abnormalities
Pregnant women
HTN during pregnancy?
Associated clinical symptoms—proteinuria, weight gain, edema?
Experiencing faintness or dizziness?
Copyright © 2020 by Elsevier Inc. All rights reserved.
Additional History for Aging Adult
Medical history
Review presence of comorbidities.
Medication profile history
Rx or OTC
Aware of side effects
Compliance with therapy
Environment
Impact on ADLs
Copyright © 2020 by Elsevier Inc. All rights reserved.
Preparation and Equipment
Preparation
To evaluate carotid arteries, a person can be sitting.
To assess jugular veins and precordium, the person should be
supine with head and chest slightly elevated.
Ensure woman’s privacy by keeping her breasts draped.
Equipment
Marking pen
Small centimeter ruler
Stethoscope with diaphragm and bell endpieces
Alcohol wipe to clean endpiece
Copyright © 2020 by Elsevier Inc. All rights reserved.
Neck Vessels:
Palpation and Auscultation
Palpate carotid artery
Palpate only one carotid artery at a time to avoid compromising
arterial blood to brain.
Feel contour and amplitude of pulse, normal strength 2+.
Findings should be same bilaterally
Auscultate carotid artery.
Assess for presence of carotid bruit.
• avoid compressing the artery which can create an artificial bruit.
Keep neck in neutral position and lightly apply stethoscope at
• angle of jaw, midcervical area, and base of neck.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Neck Vessels: Inspection
Inspect jugular venous pulse.
From jugular veins you can assess central venous pressure
(CVP) and judge heart’s efficiency as a pump.
Position a person supine anywhere from a 30- to a 45-degree
angle, wherever you can best see pulsations.
Estimate pressure.
Observe for possible distention.
Characteristics of jugular versus carotid pulsations
Differentiate between: location, quality, respiration, palpable,
pressure, and position of patient
Copyright © 2020 by Elsevier Inc. All rights reserved.
Neck Vessels: Vascular Structure
Copyright © 2020 by Elsevier Inc. All rights reserved.
Precordium
Inspect anterior chest.
Arrange tangential lighting to accentuate any flicker
of movement.
Observe for any possible pulsations.
Palpate apical impulse: note location, size, amplitude
and duration.
Palpate across precordium to assess for any
possible pulsations.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Precordium Auscultation
Identify auscultatory areas associated with valves.
Sound radiates with blood flow direction; valve areas are:
• Second right interspace: aortic valve area
• Second left interspace: pulmonic valve area
• Left lower sternal border: tricuspid valve area
• Fifth interspace at around left midclavicular line: mitral valve area
Note rate and rhythm: describe characteristics
Identify S1 and S2.
Listen for extra heart sounds: describe characteristics.
Listen for murmurs: Timing, loudness, pitch, pattern,
quality, location, radiation posture and change of
position.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Auscultatory Areas
Copyright © 2020 by Elsevier Inc. All rights reserved.
Procedures for Advanced Practice
Standing to squatting: screening measure to
detect hypertrophic cardiomyopathy
Estimation of central venous pressure (CVP) by
assessing jugular venous distention
If venous pressure is elevated or heart failure
suspected perform abdominojugular test.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Developmental Competence:
Infants
Transition from fetal to pulmonic circulation occurs in immediate
newborn period
Heart rate may range from 100 to 180 beats per minute (bpm)
immediately after birth
Note any extracardiac signs that may reflect heart status
Skin, liver size, and respiratory status
Murmurs in the immediate newborn period do not necessarily
indicate congenital heart disease seen due to shunt closure.
Murmurs are usually grade 1 or 2, systolic, no other signs of heart
disease and disappear in 2 to 3 days.
Absence of murmurs in the immediate newborn period does not ensure
a healthy heart.
Best to listen frequently and to note and describe any murmur
according to characteristics.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Developmental Competence:
Children
Note any extracardiac or cardiac signs that may indicate
heart disease.
Poor weight gain, developmental delay, persistent tachycardia,
tachypnea, dyspnea on exertion, cyanosis, and clubbing
• Note that clubbing of fingers and toes usually does not appear until
late in first year, even with severe cyanotic defects.
Palpate apical pulse
Be aware of location by age.
Rhythm remains characterized by sinus dysrhythmia.
Physiologic S3 is common in children.
Venous hum has no pathologic significance.
Assess for carotid bruit
Copyright © 2020 by Elsevier Inc. All rights reserved.
Developmental Competence:
Children Heart Murmurs
Innocent (or functional)
Very common through childhood
Some say they have 30% occurrence, and some say nearly
all children may demonstrate murmur.
Most innocent murmurs have these characteristics:
• Soft, relatively short systolic ejection murmur
• Medium pitch; vibratory
• Best heard at left lower sternal or midsternal border, with no
radiation to apex, base, or back
Patient teaching:
• Need to believe that this murmur is just a “noise” and has no
pathologic significance
• Knowledge through education to prevent overprotection and
limit activity for child
Copyright © 2020 by Elsevier Inc. All rights reserved.
Developmental Competence:
Pregnant Woman and Aging Adult
Pregnant woman:
Vital signs increase in resting pulse rate of 10 to 15 bpm and drop in BP
from normal prepregnancy level.
Palpation of apical impulse is higher and lateral compared with normal
position.
Heart sounds: Changes due to increased volume and workload
Mammary soufflé: occurs near term or when woman is lactating
Aging adult:
Gradual rise in systolic blood pressure common with aging; widening of
pulse pressure—be alert for orthostatic hypotension
Left ventricular wall thickness increase.
Presence of supraventricular and ventricular dysrhythmias increases
with age.
Age-related ECG changes occur due to histologic changes in the
conduction system.
Copyright © 2020 by Elsevier Inc. All rights reserved.
Health Promotion and Patient Teaching
Appropriate aspirin therapy
Blood pressure control
Cholesterol control
Smoking cessation
Lifestyle changes
Diet
Physical activity
Weight control
Copyright © 2020 by Elsevier Inc. All rights reserved.
Differential Diagnosis of Chest Pain
Cardiovascular
Ischemic: Angina pectoris, Prinzmetal or variant angina, and acute coronary
syndrome (ACS)
Non-ischemic: Pericarditis, mitral valve prolapse, aortic dissection, and
secondary pulmonary HTN
Pulmonary
Pulmonary embolism, pneumonia, and pneumothorax
Gastrointestinal
Gastroesophageal reflux, esophageal spasm, cholecystitis, and pancreatitis
Dermatologic
Herpes Zoster
Musculoskeletal/neurologic
Costochondritis and chest wall muscle strain
Psychogenic
Depression and anxiety
Copyright © 2020 by Elsevier Inc. All rights reserved.
Clinical Portrait of Heart Failure
Copyright © 2020 by Elsevier Inc. All rights reserved.
Variations in Heart Sounds
S1
Loud (accentuated)
Faint (diminished)
Varying intensity
Split
S2
Accentuated
Diminished
Normal splitting
• Fixed split, paradoxical split, and wide split
Copyright © 2020 by Elsevier Inc. All rights reserved.
Abnormal Findings:
Systolic and Diastolic Extra Sounds
Systolic
Ejection click
Aortic prosthetic valve sounds
Midsystolic click
Diastolic
Opening snap
Mitral prosthetic valve sound
Third heart sound
Fourth heart sound
Summation sound
Pericardial friction rub
Copyright © 2020 by Elsevier Inc. All rights reserved.
Abnormal Findings:
Abnormal Pulsations: Precordium
Thrill at the base
Lift (heave) at the left sternal border
Volume overload at the apex
Pressure overload at the apex
Copyright © 2020 by Elsevier Inc. All rights reserved.
Abnormal Findings:
Congenital Heart Defects
Patent ductus arteriosus (PDA)
Atrial septal defect (ASD)
Ventricular septal defect (VSD)
Tetralogy of Fallot
Coarctation of the aorta
Copyright © 2020 by Elsevier Inc. All rights reserved.
Abnormal Findings:
Murmurs Caused by Valvular Defects
Midsystolic ejection murmurs
Aortic stenosis
Pulmonic stenosis
Pansystolic regurgitant murmurs
Mitral regurgitation
Tricuspid regurgitation
Diastolic rumbles of atrioventricular valves
Mitral stenosis
Tricuspid stenosis
Early diastolic murmurs
Aortic regurgitation
Pulmonic regurgitation
Copyright © 2020 by Elsevier Inc. All rights reserved.
Summary Checklist: Heart and
Neck Vessels Examination
Neck
Carotid pulse—observe and palpate
Observe jugular venous pulse.
Estimate jugular venous pressure.
Precordium
Inspection and palpation
• Describe location of apical pulse.
• Note any heave (lift) or thrill.
Auscultation
• Identify anatomic areas noting rate and rhythm.
• Listen in systole and diastole for murmurs.
• Repeat with bell.
• Listen at apex and base.
Copyright © 2020 by Elsevier Inc. All rights reserved.
You might also like
- BTKV - Cardiac - Carpentier's Reconstructive Valve SurgeryDocument363 pagesBTKV - Cardiac - Carpentier's Reconstructive Valve SurgeryDavid Christian100% (1)
- Medical Terminology Cardiovascular SystemDocument35 pagesMedical Terminology Cardiovascular Systemapi-26819951486% (7)
- Cardiac Cycle by Bala GoyalDocument14 pagesCardiac Cycle by Bala Goyaltee su lingNo ratings yet
- Bojar PediatricDocument123 pagesBojar PediatricLuqman AlwiNo ratings yet
- Chapter 20 Heart and Neck VesselsDocument10 pagesChapter 20 Heart and Neck Vesselsannoja selvaNo ratings yet
- Cardiovascular Physiology: Heart and CirculationDocument25 pagesCardiovascular Physiology: Heart and Circulationyuhuma_qyu6841No ratings yet
- Functions of Cardiovascular System:: The Gross AnatomyDocument6 pagesFunctions of Cardiovascular System:: The Gross AnatomyShreyasi PatankarNo ratings yet
- Ch.20 Heart and Neck VesselsDocument10 pagesCh.20 Heart and Neck VesselsJose R. MendozaNo ratings yet
- Heart As A Pump: Departemen Fisiologi Fakultas Kedokteran Universitas Sumatera UtaraDocument33 pagesHeart As A Pump: Departemen Fisiologi Fakultas Kedokteran Universitas Sumatera UtaraXeniel AlastairNo ratings yet
- Cardiac Diseases and Cardiac RehabilitationDocument49 pagesCardiac Diseases and Cardiac RehabilitationHenri Benedict VillafloresNo ratings yet
- Chapter 020Document4 pagesChapter 020lish9990No ratings yet
- Cvs PPT 2) BpehssDocument35 pagesCvs PPT 2) BpehssAmbreen GhafoorNo ratings yet
- AP Chapter 16BDocument35 pagesAP Chapter 16BJay Patel100% (1)
- Riya Arya - 21msc1279 - Biology For ChemistsDocument13 pagesRiya Arya - 21msc1279 - Biology For ChemistsSwadesh SenNo ratings yet
- Heart Anatomy: LocationDocument45 pagesHeart Anatomy: LocationZaira100% (1)
- محاظرة تشريح وفسلجة القلب والاوعية الدمويهDocument29 pagesمحاظرة تشريح وفسلجة القلب والاوعية الدمويهfaroq AlromimahNo ratings yet
- 8.1 The Circulatory SystemDocument172 pages8.1 The Circulatory Systemnie20060301No ratings yet
- Week 11 THE HEART 2021Document60 pagesWeek 11 THE HEART 2021Huffy PotterNo ratings yet
- Chapter-7 - Cardiovascular SystemDocument8 pagesChapter-7 - Cardiovascular SystemAaQib Ali RaZaNo ratings yet
- The Cardiac Cycle 2Document7 pagesThe Cardiac Cycle 2Abigail ChristisnNo ratings yet
- Hand OutDocument5 pagesHand OutJaninie BallonNo ratings yet
- Broc PatBrocENG 01 Us EpDocument16 pagesBroc PatBrocENG 01 Us EpAchmad Deddy FatoniNo ratings yet
- Structure and Function of The HeartDocument5 pagesStructure and Function of The HeartThereseNo ratings yet
- CardiovascularDocument6 pagesCardiovascularMabes100% (1)
- Exam 4 Study Guide (1386)Document11 pagesExam 4 Study Guide (1386)S. MartinezNo ratings yet
- PDF FileDocument11 pagesPDF FilepearsonmatemoNo ratings yet
- Chapter 2 - CardiovascularDocument74 pagesChapter 2 - CardiovascularNoriani ZakariaNo ratings yet
- Anatomy of The HeartDocument28 pagesAnatomy of The HeartHerman DjawaNo ratings yet
- Circulatory SystemDocument44 pagesCirculatory Systemayman.hazem66No ratings yet
- Cardiac Cycle: DR Rakesh JainDocument97 pagesCardiac Cycle: DR Rakesh JainKemoy FrancisNo ratings yet
- Valve SurgeriesDocument13 pagesValve SurgeriesShreeja SajitNo ratings yet
- CardiologyDocument62 pagesCardiologyLaura Kathrine Simpson92% (12)
- Components of The Cardiovascular SystemDocument23 pagesComponents of The Cardiovascular SystemMr. DummyNo ratings yet
- 81: Mammalian Heart and Its RegulationDocument75 pages81: Mammalian Heart and Its RegulationIt's Ika100% (1)
- Transport in Humans 2 Heart and Cardiac CycleDocument74 pagesTransport in Humans 2 Heart and Cardiac Cycleloycoy008No ratings yet
- Cardiovascular SystemDocument12 pagesCardiovascular SystemDevendra RawatNo ratings yet
- Electrical Conduction in The HeartDocument35 pagesElectrical Conduction in The HeartNormasnizam Mohd NoorNo ratings yet
- Heart Sounds PDFDocument38 pagesHeart Sounds PDFZennon Blaze ArceusNo ratings yet
- Cardiovascular SystemDocument101 pagesCardiovascular SystemBanessa Mae GarcianoNo ratings yet
- Cardiac CycleDocument6 pagesCardiac CycleShahina ShayneNo ratings yet
- The Heart: Basis of Life .?Document94 pagesThe Heart: Basis of Life .?Diksha AgrawalNo ratings yet
- The HeartDocument65 pagesThe HeartMichael SamaniegoNo ratings yet
- The Heart PDFDocument13 pagesThe Heart PDFMary Ann SacramentoNo ratings yet
- C8 (Transport System)Document26 pagesC8 (Transport System)nurhasinahabrahimNo ratings yet
- Jantung Sebagai PompaDocument54 pagesJantung Sebagai PompaIndraYudhiNo ratings yet
- Cardiovascular SystemDocument74 pagesCardiovascular Systemاسامة محمد السيد رمضانNo ratings yet
- Anatomy & Physiology of Heart: BY: Mr. Anurag Lecturer College of Nursing DMC & H, LudhianaDocument56 pagesAnatomy & Physiology of Heart: BY: Mr. Anurag Lecturer College of Nursing DMC & H, Ludhianapreet kaurNo ratings yet
- The Cardiac CycleDocument19 pagesThe Cardiac CycleRebi NesroNo ratings yet
- Oral PathologyDocument23 pagesOral PathologyRuba AbbassNo ratings yet
- Cardiovascular SystemDocument14 pagesCardiovascular SystemAthena Huynh100% (1)
- Circulatory System IIDocument13 pagesCirculatory System IIsmbdy tbhhhNo ratings yet
- Patho - 21 HeartAdv - 211005 - 230536Document91 pagesPatho - 21 HeartAdv - 211005 - 230536Puranjay ChandelNo ratings yet
- H.A. Assessing Heart and Neck VesselsDocument55 pagesH.A. Assessing Heart and Neck VesselsMc Ramil B. PraderoNo ratings yet
- Cardiovascular DiseaseDocument66 pagesCardiovascular DiseaseManohar SinghNo ratings yet
- CV 2 Heart As A Pump Notes CopyrightDocument7 pagesCV 2 Heart As A Pump Notes Copyrightmaxwell amponsahNo ratings yet
- TM 8 TM 8only Clinical Exam of Heart and Circulatory System AGWEnglishDocument66 pagesTM 8 TM 8only Clinical Exam of Heart and Circulatory System AGWEnglishcellin rubianti azzharaNo ratings yet
- CardiovascularDocument30 pagesCardiovascularKristine Joy Librando EscalanteNo ratings yet
- Paul Cardiac Lecture 2015 OutlineDocument6 pagesPaul Cardiac Lecture 2015 OutlineMichalis KantartzisNo ratings yet
- Chapter 11 Cardiovascular SystemDocument6 pagesChapter 11 Cardiovascular SystemClarisse Anne QuinonesNo ratings yet
- EKG Study Guide RevisedDocument29 pagesEKG Study Guide Revisedflashyboy506No ratings yet
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- A Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisFrom EverandA Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisRating: 5 out of 5 stars5/5 (1)
- Cardiovascular SystemDocument8 pagesCardiovascular SystemDawnmurph Dharlene Wag-eNo ratings yet
- Chapter 29 - Management of Patients With Structural, Infectious, andDocument6 pagesChapter 29 - Management of Patients With Structural, Infectious, andMichael BoadoNo ratings yet
- Abrevieri EchoDocument3 pagesAbrevieri EchoAndreea MihaelaNo ratings yet
- 19 Cardiac DisordersDocument51 pages19 Cardiac DisordersChessie Garcia100% (1)
- Chapter 5 Cardiology - Cardiovascular System: Medical Language, 5e (Turley)Document66 pagesChapter 5 Cardiology - Cardiovascular System: Medical Language, 5e (Turley)Maria VictoriaNo ratings yet
- Multiple Choice TestsDocument50 pagesMultiple Choice TestsSalih AslaNo ratings yet
- Mitral Stenosis PDFDocument3 pagesMitral Stenosis PDFshanthNo ratings yet
- Heart Sounds: Pabish Joe P S KGMCDocument29 pagesHeart Sounds: Pabish Joe P S KGMCsangeedhNo ratings yet
- (Mahesh Chandra) Objective Cardiology PDFDocument609 pages(Mahesh Chandra) Objective Cardiology PDFfajarNo ratings yet
- CardiomyopathyDocument93 pagesCardiomyopathyAbnet WondimuNo ratings yet
- Pediatric EchoDocument17 pagesPediatric Echoraviks34No ratings yet
- Medmastery Cardiac CT Essentials HandbookDocument61 pagesMedmastery Cardiac CT Essentials HandbookVladlena CaraimanNo ratings yet
- Heart SoundsDocument4 pagesHeart SoundsEros ThanatosNo ratings yet
- 001 Block 1 SDocument56 pages001 Block 1 SAlan DaaboulNo ratings yet
- Heart Sound .Mid Systolic Click-Mitral ProlapseDocument2 pagesHeart Sound .Mid Systolic Click-Mitral ProlapseTeti AndriNo ratings yet
- Basic Echocardiography: Presentor:-Dr. Ashutosh DATE: - 14/09/2017Document71 pagesBasic Echocardiography: Presentor:-Dr. Ashutosh DATE: - 14/09/2017Ms. ISHA SHARMANo ratings yet
- Heart Dissection: Year 12 AS BiologyDocument9 pagesHeart Dissection: Year 12 AS BiologyBio SciencesNo ratings yet
- Pharmacokinetics and Pharmacodynamics PDFDocument166 pagesPharmacokinetics and Pharmacodynamics PDFCarolina PosadaNo ratings yet
- PathologyDocument28 pagesPathologyakkashamrishNo ratings yet
- Equine Diagnostic Ultrasound PDFDocument556 pagesEquine Diagnostic Ultrasound PDFSara Perez PastranaNo ratings yet
- Medical Terminology LicentaDocument75 pagesMedical Terminology LicentaGabriel BarbarasaNo ratings yet
- CHF FC III Ec Mitral StenosisDocument36 pagesCHF FC III Ec Mitral Stenosisbroken18bear100% (1)
- Chapter 9 CARDIOVASCULAR SYSTEMDocument21 pagesChapter 9 CARDIOVASCULAR SYSTEMAlexander Santiago ParelNo ratings yet
- Cardiovascular SystemDocument26 pagesCardiovascular SystemRismawatiNo ratings yet
- NCM 112 MidtermDocument25 pagesNCM 112 MidtermJan Charlie Sophia100% (1)
- POCUS ProceduresDocument123 pagesPOCUS Proceduresjaimin 666100% (1)
- Research Open Access: Singh Et Al. Critical Care (2020) 24:65Document16 pagesResearch Open Access: Singh Et Al. Critical Care (2020) 24:65BrîndușaPetcariuNo ratings yet
- Pathophysiology Q's 1Document68 pagesPathophysiology Q's 1alibel_belloNo ratings yet