Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
0 viewsRSV Presentation Chibueze
RSV Presentation Chibueze
Uploaded by
Chibueze AfugbuomRSV is a common virus that infects the respiratory tract of children and adults. It commonly causes upper respiratory infections but can sometimes lead to bronchiolitis and pneumonia in young children. Treatment is generally supportive care, though high-risk infants may receive immunoprophylaxis. RSV spreads through respiratory droplets and presents with cough, congestion and sometimes fever. While most recover without complications, high-risk infants are at greater risk of severe disease.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Respiratory Infections 1Document62 pagesRespiratory Infections 1Eduardo Valdez RodríguezNo ratings yet
- Nursing Care Plan - Pericarditis PatientDocument2 pagesNursing Care Plan - Pericarditis Patientsandie_best78% (9)
- Bronchiolitis EtiologyDocument6 pagesBronchiolitis EtiologyRonNo ratings yet
- Respiratory Syn-Cytial Virus: Rosal, Ija Lourice PDocument21 pagesRespiratory Syn-Cytial Virus: Rosal, Ija Lourice PIja Lourice RosalNo ratings yet
- Respiratory Syncytial VirusDocument16 pagesRespiratory Syncytial VirusAradhanaRamchandaniNo ratings yet
- SRH Case Study 1 - RSVDocument7 pagesSRH Case Study 1 - RSVapi-721737872No ratings yet
- File 18586Document6 pagesFile 18586Mohammed MuthanaNo ratings yet
- MK BronchiolitisDocument6 pagesMK BronchiolitisMoses Jr Kazevu100% (1)
- Nursing-Management A Respriotry Syncytial Bronchiolitis PDFDocument7 pagesNursing-Management A Respriotry Syncytial Bronchiolitis PDFAdarsh MuniNo ratings yet
- 15 PertusisDocument15 pages15 Pertusisaxlaamabdisamed20No ratings yet
- Crup 3Document22 pagesCrup 3Wilber Martin BaltodanoNo ratings yet
- Viral Infection of The Respiratory TractDocument29 pagesViral Infection of The Respiratory TractPritha BhuwapaksophonNo ratings yet
- RSV Pneumonitis: (Treatment and Prevention)Document6 pagesRSV Pneumonitis: (Treatment and Prevention)Ija Lourice RosalNo ratings yet
- Bronchiolitis PDFDocument5 pagesBronchiolitis PDFjuniorebindaNo ratings yet
- Respiratory Syncytial Virus Infection and Bronchiolitis: Practice GapsDocument14 pagesRespiratory Syncytial Virus Infection and Bronchiolitis: Practice GapsAnge CerónNo ratings yet
- K.3 Pediatri-Virologi 3 2018-2019 PDFDocument76 pagesK.3 Pediatri-Virologi 3 2018-2019 PDFandi firdha restuwatiNo ratings yet
- Bronchiolitis: Ms AnamDocument56 pagesBronchiolitis: Ms AnamdmaulidaNo ratings yet
- Etiology & EpidemiologyDocument3 pagesEtiology & EpidemiologyHandre PutraNo ratings yet
- MRCPCH Guide InfDocument19 pagesMRCPCH Guide InfRajiv Kabad100% (1)
- (Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Document43 pages(Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Haider Nadhem AL-rubaiNo ratings yet
- Respiratory SystemDocument30 pagesRespiratory SystemHani El-asferNo ratings yet
- Pediatrics in Review 2014 Piedimonte 519 30Document15 pagesPediatrics in Review 2014 Piedimonte 519 30Felipe CeaNo ratings yet
- Community health nursing حمزه PDFDocument22 pagesCommunity health nursing حمزه PDFHusseini ElghamryNo ratings yet
- Bronchiolitis ManagementDocument21 pagesBronchiolitis ManagementboojectNo ratings yet
- Bronchiolitis FdneDocument27 pagesBronchiolitis FdneRonit ChandNo ratings yet
- Acute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) NovemberDocument28 pagesAcute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) Novemberزكريا عمرNo ratings yet
- Respiratory Viral Infection: Microbiology UnitDocument17 pagesRespiratory Viral Infection: Microbiology UnitFabasyira JamalNo ratings yet
- DR Channa Senanayake Dept of MicrobiologyDocument19 pagesDR Channa Senanayake Dept of MicrobiologyTharinduNo ratings yet
- Parainfluenza VirusDocument9 pagesParainfluenza VirusLia Ayu Nur'ainiNo ratings yet
- Respiratory SyncytialDocument32 pagesRespiratory Syncytialtummalapalli venkateswara rao100% (2)
- 584 1130 1 PBDocument3 pages584 1130 1 PBAlden Lui SevillaNo ratings yet
- BronchiolitisDocument29 pagesBronchiolitisMalueth AnguiNo ratings yet
- Clinical Review: Pulmonary Tuberculosis: Diagnosis and TreatmentDocument4 pagesClinical Review: Pulmonary Tuberculosis: Diagnosis and TreatmentEdgard Eduardo Azañero EstradaNo ratings yet
- Influenza Bhasa InggrisDocument11 pagesInfluenza Bhasa InggrisandiniNo ratings yet
- Bronchiolitis: Dr. Mustafa Mohamed Ahmed MBBS, MDDocument37 pagesBronchiolitis: Dr. Mustafa Mohamed Ahmed MBBS, MDYuusuf MubarikNo ratings yet
- Epidemiology of TBDocument4 pagesEpidemiology of TByam pdNo ratings yet
- Acute Bronchiolitis and Wheezing ChildDocument22 pagesAcute Bronchiolitis and Wheezing Childhusenbrz4No ratings yet
- BronchioitisDocument24 pagesBronchioitismitiku aberaNo ratings yet
- Pneumonia 24Document18 pagesPneumonia 24Rabea DiaNo ratings yet
- 17 PneumoniaDocument30 pages17 PneumoniaCabdiNo ratings yet
- Fatal Pulmonary Infection With Respiratory SyncytiDocument5 pagesFatal Pulmonary Infection With Respiratory Syncyti21701101046 Devi NavilaNo ratings yet
- BQL RX ConsDocument3 pagesBQL RX ConsAwe Angga WirahmadiNo ratings yet
- RSVDocument8 pagesRSVilyas9558No ratings yet
- File 18587Document10 pagesFile 18587Mohammed MuthanaNo ratings yet
- URTI (DR Hemin Khalid)Document21 pagesURTI (DR Hemin Khalid)Darawan MirzaNo ratings yet
- Herpes ZosterDocument6 pagesHerpes ZosterRonan suhendraNo ratings yet
- Practice Essentials: View Media GalleryDocument22 pagesPractice Essentials: View Media GalleryAza Patullah ZaiNo ratings yet
- Pediatric RSV Amidst COVID-19 PandemicDocument12 pagesPediatric RSV Amidst COVID-19 Pandemiczula74No ratings yet
- Influenza, Pandemics and SARSDocument24 pagesInfluenza, Pandemics and SARSObatoye SeyiNo ratings yet
- Journal Reading ParuDocument53 pagesJournal Reading ParuDaniel IvanNo ratings yet
- 5th Sem Lecture MeaslesDocument22 pages5th Sem Lecture Measlessouvikmaity2024No ratings yet
- Infectious Diseases: by Group 3Document85 pagesInfectious Diseases: by Group 3Zarah ManaliliNo ratings yet
- Pediatric Community-Acquired PneumoniaDocument60 pagesPediatric Community-Acquired PneumoniaIkea Balhon100% (1)
- Pneumonia PDFDocument7 pagesPneumonia PDFmist73No ratings yet
- BronquiolitisDocument6 pagesBronquiolitisIliana GarcíaNo ratings yet
- Infection PICU 1Document33 pagesInfection PICU 1Mohamed ElgayarNo ratings yet
- GripeDocument10 pagesGripeSCIH HFCPNo ratings yet
- Meningitis: N Meningitidis Are Gram-Negative, Kidney Bean-Shaped Organisms and Frequently AreDocument7 pagesMeningitis: N Meningitidis Are Gram-Negative, Kidney Bean-Shaped Organisms and Frequently AreKhryss Paula BaldonadoNo ratings yet
- Presentation - PPTX CoronavirusDocument11 pagesPresentation - PPTX Coronaviruss4frhtcdmmNo ratings yet
- Jurnal DidanosineDocument8 pagesJurnal DidanosineRia DeviNo ratings yet
- ArticleText 56658 1 10 20191129Document10 pagesArticleText 56658 1 10 20191129gposh60No ratings yet
- Bender Gestalt TestDocument3 pagesBender Gestalt TestAleena ThakurtaNo ratings yet
- Community Health Nursing ReviewerDocument4 pagesCommunity Health Nursing ReviewerCamille GuintoNo ratings yet
- Formatif NBSSDocument17 pagesFormatif NBSSCYNTHIA ARISTANo ratings yet
- KSM Orthopedi New1Document20 pagesKSM Orthopedi New1rspku mayongNo ratings yet
- CGHS Enclosure 1Document77 pagesCGHS Enclosure 1bhupendrapawar279No ratings yet
- HB 1166 003 1095837 HB DNeasy Plant 0615 WWDocument56 pagesHB 1166 003 1095837 HB DNeasy Plant 0615 WWAlexandra GalanNo ratings yet
- Rai Work Experience SheetDocument2 pagesRai Work Experience Sheetmark langcayNo ratings yet
- Almanac Start A GardenDocument21 pagesAlmanac Start A GardenHarish Sankar100% (3)
- Clinical MedicineDocument58 pagesClinical Medicinesachin pandaoNo ratings yet
- " Crop Protection" Pesticide UseDocument25 pages" Crop Protection" Pesticide UseEthyle Morales LingbawanNo ratings yet
- Concept of Shortened Dental Arch An OverviewDocument3 pagesConcept of Shortened Dental Arch An OverviewHarold CamargoNo ratings yet
- Soal Tryout EnglishDocument16 pagesSoal Tryout EnglishSAYYAF NIZAM KNo ratings yet
- Issue Overview: Continuum: Lifelong Learning in Neurology® Is Designed To Help Practicing Neurologists StayDocument314 pagesIssue Overview: Continuum: Lifelong Learning in Neurology® Is Designed To Help Practicing Neurologists StayLorena DiasNo ratings yet
- Concepts of ProsthoDocument22 pagesConcepts of ProsthoKirti SharmaNo ratings yet
- LIC Health Plus Plan No.901 Full FormDocument15 pagesLIC Health Plus Plan No.901 Full FormDhaval SarvaiyaNo ratings yet
- Case Study On PneumoniaDocument12 pagesCase Study On PneumoniaRintu JenaNo ratings yet
- Clams Thesis PaperDocument20 pagesClams Thesis PaperhiltonrtNo ratings yet
- Ophthalmology Product CenterDocument11 pagesOphthalmology Product CenterJihad Elias ChahlaNo ratings yet
- Roles of Community Health NurseDocument6 pagesRoles of Community Health NurseAmisha KumarNo ratings yet
- Asava and Aristha An Ayurvedic Medicine - An OvervDocument8 pagesAsava and Aristha An Ayurvedic Medicine - An OvervGarima KhandelwalNo ratings yet
- 1983 Garner EDIDocument22 pages1983 Garner EDIAzyan ShahiraNo ratings yet
- Stiles Et Al (2020) Impact of COVID 19 On Health and Safety in The Construction SectorDocument13 pagesStiles Et Al (2020) Impact of COVID 19 On Health and Safety in The Construction SectorCeline DupontNo ratings yet
- Cranial Nerve Assessment: Nerve Name Function Test IDocument9 pagesCranial Nerve Assessment: Nerve Name Function Test IBecky Mariñas ReducaNo ratings yet
- Health 10 Week4 AnabellegonzalezDocument8 pagesHealth 10 Week4 AnabellegonzalezROBIN HulipasNo ratings yet
- Lifting Equation For Manual LiftingDocument10 pagesLifting Equation For Manual LiftingShafiqul IslamNo ratings yet
- Grow Save BeansDocument2 pagesGrow Save BeansPUBG HackerNo ratings yet
- Undertaking Declaration: Examination in Physics For Class Xii Aatthe Millennium School, IndoreDocument29 pagesUndertaking Declaration: Examination in Physics For Class Xii Aatthe Millennium School, IndoreAnirudh VermaNo ratings yet
RSV Presentation Chibueze
RSV Presentation Chibueze
Uploaded by
Chibueze Afugbuom0 ratings0% found this document useful (0 votes)
0 views13 pagesRSV is a common virus that infects the respiratory tract of children and adults. It commonly causes upper respiratory infections but can sometimes lead to bronchiolitis and pneumonia in young children. Treatment is generally supportive care, though high-risk infants may receive immunoprophylaxis. RSV spreads through respiratory droplets and presents with cough, congestion and sometimes fever. While most recover without complications, high-risk infants are at greater risk of severe disease.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRSV is a common virus that infects the respiratory tract of children and adults. It commonly causes upper respiratory infections but can sometimes lead to bronchiolitis and pneumonia in young children. Treatment is generally supportive care, though high-risk infants may receive immunoprophylaxis. RSV spreads through respiratory droplets and presents with cough, congestion and sometimes fever. While most recover without complications, high-risk infants are at greater risk of severe disease.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
0 views13 pagesRSV Presentation Chibueze
RSV Presentation Chibueze
Uploaded by
Chibueze AfugbuomRSV is a common virus that infects the respiratory tract of children and adults. It commonly causes upper respiratory infections but can sometimes lead to bronchiolitis and pneumonia in young children. Treatment is generally supportive care, though high-risk infants may receive immunoprophylaxis. RSV spreads through respiratory droplets and presents with cough, congestion and sometimes fever. While most recover without complications, high-risk infants are at greater risk of severe disease.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 13
RESPIRATORY SYNCYTIAL
VIRUS INFECTION
AFUGBUOM CHIBUEZE IKENNA
GROUP 640
INTRODUCTION
• The human respiratory syncytial virus (RSV) is one of the most common viruses to infect
children worldwide and increasingly is recognized as an important pathogen in adults, especially
the elderly.
• The most common clinical scenario encountered in RSV infection is an upper respiratory
infection, but RSV commonly presents in young children as bronchiolitis, a lower respiratory
tract illness with small airway obstruction, and can rarely progress to pneumonia, respiratory
failure, apnea, and death.
• The mainstay of treatment for the vast majority of RSV infections is supportive, but passive
preventive immunization is available for at-risk children, including premature infants and infants
with a history of cardiac, pulmonary, or neuromuscular diseases. There is a single antiviral
treatment for RSV currently approved, but its use is limited by questionable efficacy, side effects,
and cost, and it is recommended that it be used only for patients at risk for severe disease, on a
case-by-case basis.
ETIOLOGY
• RSV is a single-stranded, negative-strand, RNA virus belonging to
the Paramyxoviridae family, and is in the genus Pneumovirus. RSV was discovered in
chimpanzees in 1955 and subsequently confirmed to be a human pathogen shortly after
that. There are several animal respiratory syncytial viruses in the same genus as human
RSV, which do not infect humans, and which will not be further referenced in this
article.
• The structure of RSV is that of a bilipid-layer-envelope surrounding a ribonucleoprotein
core, with several membrane proteins, one of which functions in attachment to host
cells, and one of which functions in fusion to host cells. There is only one serotype of
RSV, but it is classified into two strains, "A" and "B," with differences consisting of
variation in the structure of several structural membrane proteins, most especially the
attachment protein.
EPIDEMIOLOGY
• RSV is a widespread pathogen in humans, due in part to the lack of long-term
immunity after infection, making reinfection frequent. It infects 90% of children
within the first 2 years of life and frequently reinfects older children and adults.
Most patients with RSV will have an upper respiratory illness, but a significant
minority will develop lower respiratory tract illness, predominantly in the form of
bronchiolitis.
• Children under the age of one year are especially likely to develop lower
respiratory involvement, with up to 40% of primary infections resulting in
bronchiolitis. Worldwide, it is estimated that RSV is responsible for approximately
33 million lower respiratory tract illnesses, three million hospitalizations, and up
to 199,000 childhood deaths; most deaths are in resource-limited countries
PATHOPHYSIOLOGY
• RSV is spread from person to person via respiratory droplet, and the incubation period after
inoculation with RSV ranges from 2 to 8 days, with a mean incubation of 4 to 6 days, depending
on host factors such as the age of the patient and whether it is the patient's primary infection with
RSV.
• After inoculation into the nasopharyngeal or conjunctival mucosa, the virus rapidly spreads into
the respiratory tract, where it targets its preferred growth medium: apical ciliated epithelial cells.
There it binds to cellular receptors using the RSV-G glycoprotein, then uses the RSV-F fusion
glycoprotein to fuse with host cell membranes and insert its nucleocapsid into the host cell to
begin its intracellular replication.
• Host inflammatory immune response is triggered, including both humoral and cytotoxic T-cell
activation, and a combination of viral cytotoxicity and the host's cytotoxic response cause
necrosis of respiratory epithelial cells, leading to downstream consequences of small airway
obstruction and plugging by mucus, cellular debris, and DNA.
HISTORY AND PHYSICAL
• RSV typically manifests as an upper respiratory illness, with the possibility of lower
respiratory tract involvement, and historical and examination findings differ based
on the location and severity of the disease.
• If limited to the upper respiratory tract, RSV presents with rhinorrhea, nasal
congestion, cough, sneezing, and sometimes fever and myalgia. In some patients,
especially those with risk factors for severe disease who are under the age of 2
years, RSV will progress to lower respiratory tract involvement with various
permutations of the classic findings of bronchiolitis: rhonchorous breath sounds,
tachypnea, accessory muscle use, wheezes, and prolonged expiration.
• In severe cases, it may also present with findings of viral pneumonia, hypoxia,
lethargy, apnea, and acute respiratory failure.
EVALUATION
• The diagnosis of RSV and subsequent bronchiolitis is clinical and does not require
confirmatory testing or imaging. Testing for RSV is discouraged unless the fact of its
presence would alter medical decision-making. Specific testing for RSV may be useful
to differentiate from other disorders and is available in two commonly used forms:
rapid antigen testing and polymerase-chain-reaction-based (PCR) testing. Antigen
testing is quick, inexpensive, specific, and is easily performed on nasal secretions.
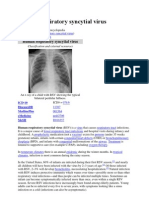
• Radiographic findings in RSV are identical to bronchiolitis in general, and are non-
specific, and require interpretation in the context of the patient's illness. Chest x-ray
findings of RSV bronchiolitis may include hyperinflation, patchy atelectasis, and
peribronchial thickening; however, these may be difficult to distinguish from bacterial
pneumonia.
TREATMENT
• Treatment for RSV falls into three categories: supportive care, immune prophylaxis, and
antiviral medication. The majority of RSV and bronchiolitis cases require no specific medical
intervention, and many attempted treatments throughout history are ineffective. Vaccines for
RSV and therapeutic interventions in RSV remain a target of intense scientific interest.
• The mainstay of treatment for patients with RSV is supportive care. The spectrum of supportive
care includes nasal suction and lubrication to provide relief from nasal congestion, antipyretics
for fever, assisted hydration in the event of dehydration (assistance may be by mouth, by
nasogastric tube, or intravenously), and oxygen for patients experiencing hypoxia. Patients with
severe presentation and respiratory compromise/failure may require ventilatory support in the
form of a high-flow nasal cannula, CPAP, or intubation, and mechanical ventilation.
Hospitalization is recommended for patients who are experiencing or are at risk for moderate to
severe disease, patients requiring supplemental fluids, and patients requiring respiratory
support.
TREATMENT
• Effective passive immune prophylaxis for RSV exists in the form of palivizumab, a
humanized murine monoclonal antibody with activity against the RSV membrane
fusion protein required for fusion with host cell membranes. Palivizumab must be
administered monthly for the duration of the RSV season. Palivizumab is relatively
expensive and is the subject of some debate regarding cost-effectiveness.
• The American Academy of Pediatrics publishes guidelines regarding which patients are
candidates for palivizumab and its discontinuation in breakthrough infection, and we
refer readers to those guidelines for specific recommendations regarding palivizumab
eligibility. Broadly, these recommendations include prophylaxis for children in the first
year of life with: prematurity less than or equal to 29 weeks gestational age, chronic
lung disease of prematurity, congenital heart disease, or neuromuscular disorders.
SOME DIFFERENTIAL DIAGNOSIS
• Asthma
• Bronchiolitis
• Influenza
• Croup
• Bronchitis
• Pneumonia
PROGNOSIS
• Children hospitalized secondary to RSV infection usually recover without
sequelae. They are discharged in 3 to 4 days. High-risk infants have longer
hospitalizations and have higher rates of mechanical ventilation and
admission to the intensive care unit.
• People infected with RSV are contagious for 3 to 8 days. However, some
infants, and people with weakened immune systems, can continue to spread
the virus even after they stop showing symptoms for as long as 4 weeks.
OUTCOMES OF RSV
• The majority of children with RSV have an excellent outcome. Even those who
need admission are usually discharged in several days. However, high-risk
infants with other co-morbidities may require longer admission and some may
even require mechanical ventilation.
• The overall mortality for RSV is less than 1%, and in the United States, less than
400 deaths are attributed to RSV each year. Infants with congenital heart disease,
prematurity or chronic lung disease tend to have the highest mortality. Further
infants who are immunocompromised also tend to have longer admissions
compared to normal infants. In the long run, some infants with RSV may
develop wheezing, but this is debatable. Recent studies do not show an increased
risk of asthma.
You might also like
- Respiratory Infections 1Document62 pagesRespiratory Infections 1Eduardo Valdez RodríguezNo ratings yet
- Nursing Care Plan - Pericarditis PatientDocument2 pagesNursing Care Plan - Pericarditis Patientsandie_best78% (9)
- Bronchiolitis EtiologyDocument6 pagesBronchiolitis EtiologyRonNo ratings yet
- Respiratory Syn-Cytial Virus: Rosal, Ija Lourice PDocument21 pagesRespiratory Syn-Cytial Virus: Rosal, Ija Lourice PIja Lourice RosalNo ratings yet
- Respiratory Syncytial VirusDocument16 pagesRespiratory Syncytial VirusAradhanaRamchandaniNo ratings yet
- SRH Case Study 1 - RSVDocument7 pagesSRH Case Study 1 - RSVapi-721737872No ratings yet
- File 18586Document6 pagesFile 18586Mohammed MuthanaNo ratings yet
- MK BronchiolitisDocument6 pagesMK BronchiolitisMoses Jr Kazevu100% (1)
- Nursing-Management A Respriotry Syncytial Bronchiolitis PDFDocument7 pagesNursing-Management A Respriotry Syncytial Bronchiolitis PDFAdarsh MuniNo ratings yet
- 15 PertusisDocument15 pages15 Pertusisaxlaamabdisamed20No ratings yet
- Crup 3Document22 pagesCrup 3Wilber Martin BaltodanoNo ratings yet
- Viral Infection of The Respiratory TractDocument29 pagesViral Infection of The Respiratory TractPritha BhuwapaksophonNo ratings yet
- RSV Pneumonitis: (Treatment and Prevention)Document6 pagesRSV Pneumonitis: (Treatment and Prevention)Ija Lourice RosalNo ratings yet
- Bronchiolitis PDFDocument5 pagesBronchiolitis PDFjuniorebindaNo ratings yet
- Respiratory Syncytial Virus Infection and Bronchiolitis: Practice GapsDocument14 pagesRespiratory Syncytial Virus Infection and Bronchiolitis: Practice GapsAnge CerónNo ratings yet
- K.3 Pediatri-Virologi 3 2018-2019 PDFDocument76 pagesK.3 Pediatri-Virologi 3 2018-2019 PDFandi firdha restuwatiNo ratings yet
- Bronchiolitis: Ms AnamDocument56 pagesBronchiolitis: Ms AnamdmaulidaNo ratings yet
- Etiology & EpidemiologyDocument3 pagesEtiology & EpidemiologyHandre PutraNo ratings yet
- MRCPCH Guide InfDocument19 pagesMRCPCH Guide InfRajiv Kabad100% (1)
- (Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Document43 pages(Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Haider Nadhem AL-rubaiNo ratings yet
- Respiratory SystemDocument30 pagesRespiratory SystemHani El-asferNo ratings yet
- Pediatrics in Review 2014 Piedimonte 519 30Document15 pagesPediatrics in Review 2014 Piedimonte 519 30Felipe CeaNo ratings yet
- Community health nursing حمزه PDFDocument22 pagesCommunity health nursing حمزه PDFHusseini ElghamryNo ratings yet
- Bronchiolitis ManagementDocument21 pagesBronchiolitis ManagementboojectNo ratings yet
- Bronchiolitis FdneDocument27 pagesBronchiolitis FdneRonit ChandNo ratings yet
- Acute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) NovemberDocument28 pagesAcute Bronchiolitis: Zakaria Omar Elzwie Najwa Abdulallah Alfergany (Mub) Novemberزكريا عمرNo ratings yet
- Respiratory Viral Infection: Microbiology UnitDocument17 pagesRespiratory Viral Infection: Microbiology UnitFabasyira JamalNo ratings yet
- DR Channa Senanayake Dept of MicrobiologyDocument19 pagesDR Channa Senanayake Dept of MicrobiologyTharinduNo ratings yet
- Parainfluenza VirusDocument9 pagesParainfluenza VirusLia Ayu Nur'ainiNo ratings yet
- Respiratory SyncytialDocument32 pagesRespiratory Syncytialtummalapalli venkateswara rao100% (2)
- 584 1130 1 PBDocument3 pages584 1130 1 PBAlden Lui SevillaNo ratings yet
- BronchiolitisDocument29 pagesBronchiolitisMalueth AnguiNo ratings yet
- Clinical Review: Pulmonary Tuberculosis: Diagnosis and TreatmentDocument4 pagesClinical Review: Pulmonary Tuberculosis: Diagnosis and TreatmentEdgard Eduardo Azañero EstradaNo ratings yet
- Influenza Bhasa InggrisDocument11 pagesInfluenza Bhasa InggrisandiniNo ratings yet
- Bronchiolitis: Dr. Mustafa Mohamed Ahmed MBBS, MDDocument37 pagesBronchiolitis: Dr. Mustafa Mohamed Ahmed MBBS, MDYuusuf MubarikNo ratings yet
- Epidemiology of TBDocument4 pagesEpidemiology of TByam pdNo ratings yet
- Acute Bronchiolitis and Wheezing ChildDocument22 pagesAcute Bronchiolitis and Wheezing Childhusenbrz4No ratings yet
- BronchioitisDocument24 pagesBronchioitismitiku aberaNo ratings yet
- Pneumonia 24Document18 pagesPneumonia 24Rabea DiaNo ratings yet
- 17 PneumoniaDocument30 pages17 PneumoniaCabdiNo ratings yet
- Fatal Pulmonary Infection With Respiratory SyncytiDocument5 pagesFatal Pulmonary Infection With Respiratory Syncyti21701101046 Devi NavilaNo ratings yet
- BQL RX ConsDocument3 pagesBQL RX ConsAwe Angga WirahmadiNo ratings yet
- RSVDocument8 pagesRSVilyas9558No ratings yet
- File 18587Document10 pagesFile 18587Mohammed MuthanaNo ratings yet
- URTI (DR Hemin Khalid)Document21 pagesURTI (DR Hemin Khalid)Darawan MirzaNo ratings yet
- Herpes ZosterDocument6 pagesHerpes ZosterRonan suhendraNo ratings yet
- Practice Essentials: View Media GalleryDocument22 pagesPractice Essentials: View Media GalleryAza Patullah ZaiNo ratings yet
- Pediatric RSV Amidst COVID-19 PandemicDocument12 pagesPediatric RSV Amidst COVID-19 Pandemiczula74No ratings yet
- Influenza, Pandemics and SARSDocument24 pagesInfluenza, Pandemics and SARSObatoye SeyiNo ratings yet
- Journal Reading ParuDocument53 pagesJournal Reading ParuDaniel IvanNo ratings yet
- 5th Sem Lecture MeaslesDocument22 pages5th Sem Lecture Measlessouvikmaity2024No ratings yet
- Infectious Diseases: by Group 3Document85 pagesInfectious Diseases: by Group 3Zarah ManaliliNo ratings yet
- Pediatric Community-Acquired PneumoniaDocument60 pagesPediatric Community-Acquired PneumoniaIkea Balhon100% (1)
- Pneumonia PDFDocument7 pagesPneumonia PDFmist73No ratings yet
- BronquiolitisDocument6 pagesBronquiolitisIliana GarcíaNo ratings yet
- Infection PICU 1Document33 pagesInfection PICU 1Mohamed ElgayarNo ratings yet
- GripeDocument10 pagesGripeSCIH HFCPNo ratings yet
- Meningitis: N Meningitidis Are Gram-Negative, Kidney Bean-Shaped Organisms and Frequently AreDocument7 pagesMeningitis: N Meningitidis Are Gram-Negative, Kidney Bean-Shaped Organisms and Frequently AreKhryss Paula BaldonadoNo ratings yet
- Presentation - PPTX CoronavirusDocument11 pagesPresentation - PPTX Coronaviruss4frhtcdmmNo ratings yet
- Jurnal DidanosineDocument8 pagesJurnal DidanosineRia DeviNo ratings yet
- ArticleText 56658 1 10 20191129Document10 pagesArticleText 56658 1 10 20191129gposh60No ratings yet
- Bender Gestalt TestDocument3 pagesBender Gestalt TestAleena ThakurtaNo ratings yet
- Community Health Nursing ReviewerDocument4 pagesCommunity Health Nursing ReviewerCamille GuintoNo ratings yet
- Formatif NBSSDocument17 pagesFormatif NBSSCYNTHIA ARISTANo ratings yet
- KSM Orthopedi New1Document20 pagesKSM Orthopedi New1rspku mayongNo ratings yet
- CGHS Enclosure 1Document77 pagesCGHS Enclosure 1bhupendrapawar279No ratings yet
- HB 1166 003 1095837 HB DNeasy Plant 0615 WWDocument56 pagesHB 1166 003 1095837 HB DNeasy Plant 0615 WWAlexandra GalanNo ratings yet
- Rai Work Experience SheetDocument2 pagesRai Work Experience Sheetmark langcayNo ratings yet
- Almanac Start A GardenDocument21 pagesAlmanac Start A GardenHarish Sankar100% (3)
- Clinical MedicineDocument58 pagesClinical Medicinesachin pandaoNo ratings yet
- " Crop Protection" Pesticide UseDocument25 pages" Crop Protection" Pesticide UseEthyle Morales LingbawanNo ratings yet
- Concept of Shortened Dental Arch An OverviewDocument3 pagesConcept of Shortened Dental Arch An OverviewHarold CamargoNo ratings yet
- Soal Tryout EnglishDocument16 pagesSoal Tryout EnglishSAYYAF NIZAM KNo ratings yet
- Issue Overview: Continuum: Lifelong Learning in Neurology® Is Designed To Help Practicing Neurologists StayDocument314 pagesIssue Overview: Continuum: Lifelong Learning in Neurology® Is Designed To Help Practicing Neurologists StayLorena DiasNo ratings yet
- Concepts of ProsthoDocument22 pagesConcepts of ProsthoKirti SharmaNo ratings yet
- LIC Health Plus Plan No.901 Full FormDocument15 pagesLIC Health Plus Plan No.901 Full FormDhaval SarvaiyaNo ratings yet
- Case Study On PneumoniaDocument12 pagesCase Study On PneumoniaRintu JenaNo ratings yet
- Clams Thesis PaperDocument20 pagesClams Thesis PaperhiltonrtNo ratings yet
- Ophthalmology Product CenterDocument11 pagesOphthalmology Product CenterJihad Elias ChahlaNo ratings yet
- Roles of Community Health NurseDocument6 pagesRoles of Community Health NurseAmisha KumarNo ratings yet
- Asava and Aristha An Ayurvedic Medicine - An OvervDocument8 pagesAsava and Aristha An Ayurvedic Medicine - An OvervGarima KhandelwalNo ratings yet
- 1983 Garner EDIDocument22 pages1983 Garner EDIAzyan ShahiraNo ratings yet
- Stiles Et Al (2020) Impact of COVID 19 On Health and Safety in The Construction SectorDocument13 pagesStiles Et Al (2020) Impact of COVID 19 On Health and Safety in The Construction SectorCeline DupontNo ratings yet
- Cranial Nerve Assessment: Nerve Name Function Test IDocument9 pagesCranial Nerve Assessment: Nerve Name Function Test IBecky Mariñas ReducaNo ratings yet
- Health 10 Week4 AnabellegonzalezDocument8 pagesHealth 10 Week4 AnabellegonzalezROBIN HulipasNo ratings yet
- Lifting Equation For Manual LiftingDocument10 pagesLifting Equation For Manual LiftingShafiqul IslamNo ratings yet
- Grow Save BeansDocument2 pagesGrow Save BeansPUBG HackerNo ratings yet
- Undertaking Declaration: Examination in Physics For Class Xii Aatthe Millennium School, IndoreDocument29 pagesUndertaking Declaration: Examination in Physics For Class Xii Aatthe Millennium School, IndoreAnirudh VermaNo ratings yet