Professional Documents
Culture Documents
Assessment and Management of Patients With Hepatic Disorders
Assessment and Management of Patients With Hepatic Disorders
Uploaded by
Noor Majali0 ratings0% found this document useful (0 votes)
6 views31 pagesThe document provides an overview of liver function and disorders, including their causes, manifestations, and management approaches. Specifically, it discusses ascites, a common complication of portal hypertension seen in patients with hepatic dysfunction. Ascites results from fluid accumulation in the abdominal cavity due to increased portal pressure and other factors. Symptoms include abdominal swelling and discomfort. Diagnosis involves physical examination to detect shifting dullness or a fluid wave. Treatment focuses on sodium restriction, diuretics like spironolactone, and large volume paracentesis combined with IV albumin infusion for severe cases.
Original Description:
Original Title
4_5848118429050997468
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document provides an overview of liver function and disorders, including their causes, manifestations, and management approaches. Specifically, it discusses ascites, a common complication of portal hypertension seen in patients with hepatic dysfunction. Ascites results from fluid accumulation in the abdominal cavity due to increased portal pressure and other factors. Symptoms include abdominal swelling and discomfort. Diagnosis involves physical examination to detect shifting dullness or a fluid wave. Treatment focuses on sodium restriction, diuretics like spironolactone, and large volume paracentesis combined with IV albumin infusion for severe cases.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
6 views31 pagesAssessment and Management of Patients With Hepatic Disorders
Assessment and Management of Patients With Hepatic Disorders
Uploaded by
Noor MajaliThe document provides an overview of liver function and disorders, including their causes, manifestations, and management approaches. Specifically, it discusses ascites, a common complication of portal hypertension seen in patients with hepatic dysfunction. Ascites results from fluid accumulation in the abdominal cavity due to increased portal pressure and other factors. Symptoms include abdominal swelling and discomfort. Diagnosis involves physical examination to detect shifting dullness or a fluid wave. Treatment focuses on sodium restriction, diuretics like spironolactone, and large volume paracentesis combined with IV albumin infusion for severe cases.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 31
Assessment and Management of
Patients With Hepatic Disorders
Dr. Lubna Dwerij
Introduction
Liver function is complex, and liver dysfunction affects all
body systems.
For this reason, the nurse must understand how the liver
functions and must have expert clinical assessment and
management skills to care for patients undergoing complex
diagnostic and treatment procedures.
Liver disorders are common and may result from a virus,
exposure to toxic substances such as alcohol, or tumors.
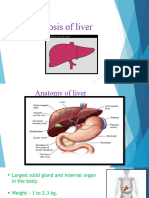
The liver is a large, highly vascular organ located behind the
ribs in the upper right portion of the abdominal cavity.
It weighs between 1200 and 1500 g and is divided into four
lobes.
Anatomic and Physiologic Overview
The liver, the largest gland of the body, can be considered
a chemical factory that manufactures, stores, alters, and
excretes a large number of substances involved in
metabolism.
The location of the liver is essential in this function
because it receives nutrient-rich blood directly from the
gastrointestinal (GI) tract and then either stores or
transforms these nutrients into chemicals that are used
elsewhere in the body for metabolic needs.
Anatomic and Physiologic Overview
The liver is especially important in the regulation of
glucose and protein metabolism.
The liver manufactures and secretes bile, which has a
major role in the digestion and absorption of fats in the GI
tract.
The liver removes waste products from the bloodstream
and secretes them into the bile.
The bile produced by the liver is stored temporarily in the
gallbladder until it is needed for digestion, at which time
the gallbladder empties and bile enters the intestine
Functions of the Liver
Glucose Metabolism
Ammonia Conversion: The liver converts ammonia, a
potential toxin, into urea, a compound that is excreted in
the urine
Protein Metabolism
Fat Metabolism
Vitamin and Iron Storage
Bile Formation
Bilirubin Excretion
Drug Metabolism
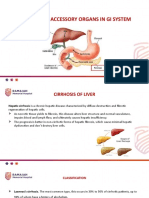
MANIFESTATIONS OF HEPATIC DYSFUNCTION
Hepatic dysfunction results from damage to the liver’s
parenchymal cells, directly from primary liver diseases, or
indirectly from either obstruction of bile flow or
derangements of hepatic circulation.
Liver dysfunction may be acute or chronic; the latter is far
more common.
The rate of chronic liver disease for men is twice that for
women, and chronic liver disease is more common in Asian
and African countries than it is in Europe and the United
States.
MANIFESTATIONS OF HEPATIC DYSFUNCTION
Disease processes that lead to hepatocellular dysfunction
may be caused by infectious agents such as bacteria and
viruses and by anoxia, metabolic disorders, toxins and
medications, nutritional deficiencies, and hypersensitivity
states.
The most common cause of parenchymal damage is
malnutrition, especially that related to alcoholism.
Among the most common and significant manifestations of
liver disease are jaundice, portal hypertension, ascites
and varices, nutritional deficiencies (resulting from the
inability of damaged liver cells to metabolize certain
vitamins), and hepatic encephalopathy or coma.
MANIFESTATIONS OF HEPATIC
DYSFUNCTION
The consequences of liver disease are numerous and
varied. Their ultimate effects are often incapacitating or
life-threatening, and their presence is ominous. Treatment
often is difficult.
Portal Hypertension
Portal hypertension is the increased pressure throughout
the portal venous system that results from obstruction of
blood flow through the damaged liver.
Commonly associated with hepatic cirrhosis, it can also
occur with non-cirrhotic liver disease.
Although splenomegaly (enlarged spleen) with possible
hypersplenism is a common manifestation of portal
hypertension, the two major consequences of portal
hypertension are
Ascites and varices.
Ascites
The mechanisms responsible for the development of
ascites are not completely understood.
Portal hypertension and the resulting increase in capillary
pressure and obstruction of venous blood flow through the
damaged liver are contributing factors.
The vasodilation that occurs in the splanchnic circulation
is also a suspected causative factor.
The failure of the liver to metabolize aldosterone
increases sodium and water retention by the kidney.
Ascites
Sodium and water retention, increased intravascular fluid
volume, increased lymphatic flow, and decreased
synthesis of albumin by the damaged liver all contribute
to the movement of fluid from the vascular system into
the peritoneal space.
As a result of liver damage, large amounts of albumin rich
fluid, 15 L or more, may accumulate in the peritoneal
cavity as ascites.
Ascites may also occur with disorders such as cancer,
kidney disease, and heart failure.)
Clinical Manifestations
Increased abdominal girth and rapid weight gain are
common presenting symptoms of ascites.
The patient may be short of breath and uncomfortable
from the enlarged abdomen, and striae and distended
veins may be visible over the abdominal wall.
Umbilical hernias also occur frequently in those patients
with cirrhosis. Fluid and electrolyte imbalances are
common.
Assessment and Diagnostic Findings
The presence and extent of ascites are assessed by
percussion of the abdomen.
When fluid has accumulated in the peritoneal cavity, the
flanks bulge when the patient assumes a supine position.
The presence of fluid can be confirmed either by
percussing for shifting dullness or by detecting a fluid
wave.
Assessing for abdominal fluid wave.
The examiner places the hands along the sides
of the patient’s flanks, then strikes one flank
sharply, detecting any fluid wave with the other
hand.
An assistant’s hand is placed (ulnar side down)
along the patient’s midline to prevent the fluid
wave from being transmitted through the tissues
of the abdominal wall.
Medical Management
Dietary Modification
The goal of treatment for the patient with ascites is a
negative sodium balance to reduce fluid retention.
Table salt, salty foods, salted butter and margarine, and
all ordinary canned and frozen foods that are not
specifically prepared for low-sodium (2-g sodium) diets
should be avoided.
It may take 2 to 3 months for the patient’s taste buds to
adjust to unsalted foods.
In the meantime, the taste of unsalted foods can be
improved by using salt substitutes such as lemon juice,
oregano, and thyme.
Medical Management
Commercial salt substitutes need to be approved by the
physician, because those that contain ammonia could
precipitate hepatic coma.
Most salt substitutes contain potassium and should be
avoided if the patient has impaired renal function.
If fluid accumulation is not controlled with this regimen,
the daily sodium allowance may be reduced further to 500
mg, and diuretics may be administered.
Medical Management
Diuretics
Use of diuretics along with sodium restriction is successful
in 90% of patients with ascites.
Spironolactone (Aldactone), an aldosterone-blocking
agent, is most often the first-line therapy in patients with
ascites from cirrhosis.
When used with other diuretics, spironolactone helps
prevent potassium loss.
Medical MaAnagement
Diuretics
Oral diuretics such as furosemide (Lasix) may be added but
should be used cautiously, because long-term use may induce
severe sodium depletion (hyponatremia).
Daily weight loss should not exceed 1 to 2 kg (2.2 to 4.4 lb) in
patients with ascites and peripheral edema or 0.5 to 0.75 kg
(1.1 to 1.65 lb) in patients without edema.
Possible complications of diuretic therapy include
Fluid and electrolyte disturbances (including hypovolemia,
hypokalemia, hyponatremia, and hypochloremic alkalosis)
Encephalopathy.
Medical Management
Diuretics
Encephalopathy may be precipitated by dehydration and
hypovolemia. In addition, when potassium stores are
depleted, the amount of ammonia in the systemic
circulation increases, which may cause impaired cerebral
functioning and encephalopathy.
Medical Management
Bed Rest
In patients with ascites, an upright posture is associated
with activation of the renin–angiotensin–aldosterone
system and sympathetic nervous system.
This causes reduced renal glomerular filtration and sodium
excretion and a decreased response to loop diuretics.
Therefore, bed rest may be a useful therapy, especially for
patients whose condition is refractory to diuretics.
Medical Management
Paracentesis
Paracentesis is the removal of fluid (ascites) from the
peritoneal cavity through a puncture or a small surgical
incision through the abdominal wall under sterile
conditions.
Paracentesis was once considered a routine form of
treatment for ascites.
However, it is now performed primarily for diagnostic
examination of ascitic fluid; for treatment of massive
ascites that is resistant to nutritional and diuretic therapy
and that is causing severe problems to the patient.
Medical Management
A sample of the ascitic fluid may be sent to the laboratory
for cell count, albumin and total protein levels, culture,
and other tests.
Large-volume (5 to 6 L) paracentesis has been shown to be
a safe method for treating patients with severe ascites.
This technique, in combination with the IV infusion of salt-
poor albumin or other colloid, has become a standard
management strategy yielding an immediate effect.
Medical Management
Refractive, massive ascites is unresponsive to multiple
diuretics and sodium restriction for 2 weeks or more and
can result in severe sequelae such as respiratory distress,
which requires rapid intervention.
Albumin infusions help to correct decreases in effective
arterial blood volume that lead to sodium retention.
Use of this colloid reduces the incidence of
postparacentesis circulatory dysfunction with renal
dysfunction, hyponatremia, and rapid reaccumulation of
ascites associated with decreased effective arterial
volume.
Medical Management
Therapeutic paracentesis provides only temporary removal
of fluid; ascites rapidly recurs, necessitating repeated
fluid removal.
Nursing Management
If a patient with ascites from liver dysfunction is
hospitalized, nursing measures include assessment and
documentation of intake and output, abdominal girth, and
daily weight to assess fluid status.
The nurse monitors serum ammonia and electrolyte levels
to assess electrolyte balance, response to therapy, and
indicators of encephalopathy.
Nursing Management
Teaching Patients Self-Care
The patient treated for ascites is likely to be discharged with
some ascites still present.
Before hospital discharge, the nurse teaches the patient and
family about the treatment plan, including
The need to avoid all alcohol intake.
Adhere to a low-sodium diet.
Take medications as prescribed.
Check with the physician before taking any new medications.
Additional patient and family teaching addresses skin care and
the need to weigh the patient daily and to watch for and
report signs and symptoms of complications.
Reference
Hinkle, J. L., & Cheever, K. H. (2014). Brunner & Suddarth's textbook of
medical-surgical nursing (Edition 13.). Wolters Kluwer Health/Lippincott
Williams & Wilkins.
You might also like
- Geist The Sin-Eaters - One Foot in The GraveDocument92 pagesGeist The Sin-Eaters - One Foot in The GraveHenry Bensley100% (3)
- BAMF LinkedIn Influencer ProgramDocument45 pagesBAMF LinkedIn Influencer ProgramAlina Zhoga100% (1)
- Case Study Liver CirrhosisDocument6 pagesCase Study Liver CirrhosisAngelica Barcelona Yumang67% (3)
- Acute Renal FailureDocument35 pagesAcute Renal FailureKaelyn Bello Giray100% (1)
- Liver Cirrhosis Nursing Care PlansDocument17 pagesLiver Cirrhosis Nursing Care Plansmarsan12No ratings yet
- Liver CirrhosisDocument2 pagesLiver CirrhosisAzette Agpi100% (3)
- Week 1 Handout 3 Contempt of CourtDocument5 pagesWeek 1 Handout 3 Contempt of CourtMatNo ratings yet
- The World Atlas of Street Art and Graffiti PDFDocument400 pagesThe World Atlas of Street Art and Graffiti PDFBob Agnetio100% (4)
- Business English SyllabusDocument2 pagesBusiness English SyllabusAde anugrahNo ratings yet
- Revised New PTLLS Assignment 1 Levels 3 and 4 Nov 2011Document3 pagesRevised New PTLLS Assignment 1 Levels 3 and 4 Nov 2011dave_perry189218No ratings yet
- Presentation On Cirrhosis of LiverDocument34 pagesPresentation On Cirrhosis of LiverAnshu kumariNo ratings yet
- Sirrhosis HatiDocument6 pagesSirrhosis HatikimokberusungNo ratings yet
- Disorders of Accesssory Organs in GI SystemDocument29 pagesDisorders of Accesssory Organs in GI SystemY. Beatrice AbigailNo ratings yet
- Done By: Dana Othman: AscitesDocument28 pagesDone By: Dana Othman: Ascitesraed faisalNo ratings yet
- Management and Care of Patients With Ascites: Prepared by Nisha Thomas MspuDocument12 pagesManagement and Care of Patients With Ascites: Prepared by Nisha Thomas MspuShilpaNo ratings yet
- HyperuricemiaDocument10 pagesHyperuricemianinroseNo ratings yet
- Chronic Liver FailureDocument4 pagesChronic Liver FailureJasmine Faith SilvaNo ratings yet
- Cirrhosis of Liver: Shemil Clinical Instructor DmwimsDocument25 pagesCirrhosis of Liver: Shemil Clinical Instructor DmwimsSrihari DivyaNo ratings yet
- CirrhoisDocument6 pagesCirrhoisAslimah RakimNo ratings yet
- Fulminant Hepatic FailureDocument10 pagesFulminant Hepatic FailureAira Anne Tonee VillaminNo ratings yet
- Cirrhosis of LiverDocument22 pagesCirrhosis of LiverKrini Tandel50% (2)
- Hepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijDocument69 pagesHepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Acute Renal FailureDocument30 pagesAcute Renal FailureJerinNo ratings yet
- Acute Renal Failure & Chronic Renal FailureDocument38 pagesAcute Renal Failure & Chronic Renal FailureArti GondNo ratings yet
- Acute Kidney DiseaseDocument2 pagesAcute Kidney DiseaseJeff CorpuzNo ratings yet
- Cirrhosis of Liver, Liver Cancer, HepatitisDocument72 pagesCirrhosis of Liver, Liver Cancer, HepatitisBabita DhruwNo ratings yet
- Osmotic Diarrhoea: Difficile)Document4 pagesOsmotic Diarrhoea: Difficile)Marwan M.No ratings yet
- Liver Cirrhosis Marking KeyDocument5 pagesLiver Cirrhosis Marking KeyChristone “Zuluzulu” ZuluNo ratings yet
- Chronic Renal FailureDocument3 pagesChronic Renal FailureNurol-Ainah Hafizah U. PimpingNo ratings yet
- Activity 8-Liver Cirrhosis-DonghitDocument8 pagesActivity 8-Liver Cirrhosis-DonghitAllona Jane Beatrice DonghitNo ratings yet
- Acute Renal Failure & Chronic Renal FailureDocument39 pagesAcute Renal Failure & Chronic Renal FailureMarie MayNo ratings yet
- Ikp 4-MavzuDocument13 pagesIkp 4-Mavzubegzodrahmonberdiyev03No ratings yet
- Liver CirrhosisDocument8 pagesLiver CirrhosisgoyaNo ratings yet
- Dietary Dialysis With Acacia Gum: Intestinal Dialysis TechnologyDocument8 pagesDietary Dialysis With Acacia Gum: Intestinal Dialysis TechnologyAamir Jalal Al-MosawiNo ratings yet
- Group 1 HypokalemiaDocument6 pagesGroup 1 HypokalemiaAdegboye AdedayoNo ratings yet
- Define Acute Renal FailureDocument4 pagesDefine Acute Renal FailureSonalika PatelNo ratings yet
- polycystic-kidney-diseaseDocument87 pagespolycystic-kidney-diseaseChei Ann Marie HernandezNo ratings yet
- Acute Renal Failure8Document35 pagesAcute Renal Failure8Andrew MidaNo ratings yet
- Chronic Kidney DiseaseDocument21 pagesChronic Kidney Disease속강대No ratings yet
- NCM 3114 - Altered Urinary PatternsDocument18 pagesNCM 3114 - Altered Urinary PatternsKoleen Lhyte UyNo ratings yet
- AscitesDocument35 pagesAscitesAmna FarhatNo ratings yet
- Metabolism and EndocrineDocument156 pagesMetabolism and EndocrineGren May Angeli MagsakayNo ratings yet
- Cirrhosis Hours: 5. Working Place: Classroom, Hospital Wards. QuestionsDocument5 pagesCirrhosis Hours: 5. Working Place: Classroom, Hospital Wards. QuestionsNahanNo ratings yet
- Nutr 409 Case Study 12Document5 pagesNutr 409 Case Study 12api-314354953100% (2)
- المستندDocument18 pagesالمستندAndrew MidaNo ratings yet
- Chapter 8Document89 pagesChapter 8Harith AtrisNo ratings yet
- Hepatological Diseases in AnimalsDocument34 pagesHepatological Diseases in AnimalsRICHARD RODERICK OLMEDONo ratings yet
- Acuterenalfailure2filesmerged 190509071023Document85 pagesAcuterenalfailure2filesmerged 190509071023ellise abundoNo ratings yet
- Seminar On Cirrhosis of LiverDocument9 pagesSeminar On Cirrhosis of Liverrufusprasanth_rachaproluNo ratings yet
- Cholesterol Stone. People Are at Most Risk For Cholecystitis or Cholelithiasis Is Obese Women Who HaveDocument4 pagesCholesterol Stone. People Are at Most Risk For Cholecystitis or Cholelithiasis Is Obese Women Who HavePatriot DolorNo ratings yet
- Liver Cirrhosis Case PresDocument77 pagesLiver Cirrhosis Case Presmarlx580% (5)
- Liver CirrhosisDocument5 pagesLiver CirrhosisRLLTNo ratings yet
- Module 15 Diets For Diseases of The Liver 2Document13 pagesModule 15 Diets For Diseases of The Liver 2WendellNo ratings yet
- Chronic Renal FailureDocument18 pagesChronic Renal FailureJoan Carla BocoNo ratings yet
- Intestinal Failure and Short Bowel SyndromeDocument5 pagesIntestinal Failure and Short Bowel SyndromesivaNo ratings yet
- AscitesDocument46 pagesAscitesRahul Kumar VermaNo ratings yet
- Approach To A Patient With Diarrhea Dr. Mohamed Abu HmaidDocument61 pagesApproach To A Patient With Diarrhea Dr. Mohamed Abu Hmaidoss-20502745No ratings yet
- NCP CKD From CaneDocument74 pagesNCP CKD From CaneSheela Khrystyn LeeNo ratings yet
- Management of Renale Disease-1Document20 pagesManagement of Renale Disease-1Abdur RehmanNo ratings yet
- Dietary Management of Liver Diseases-4Document6 pagesDietary Management of Liver Diseases-4nanbam007No ratings yet
- Cirrhosisoftheliver 2016Document4 pagesCirrhosisoftheliver 2016Nazimr RazaNo ratings yet
- Liver DiseasesDocument7 pagesLiver DiseasesGurleen KaurNo ratings yet
- Ecologic ModelDocument6 pagesEcologic ModelAdrian OrpiaNo ratings yet
- Medical Surgical Fluid and Electrolytes FVD FVEDocument7 pagesMedical Surgical Fluid and Electrolytes FVD FVEMichaelaKatrinaTrinidadNo ratings yet
- Ascites, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandAscites, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- The Renal Diet Kitchen: 60+ Quick and Delicious Renal Diet Recipes to Improve Kidney FunctionFrom EverandThe Renal Diet Kitchen: 60+ Quick and Delicious Renal Diet Recipes to Improve Kidney FunctionNo ratings yet
- محاسبة 1Document37 pagesمحاسبة 1Noor MajaliNo ratings yet
- شاشات انجليزي 99 ادعولناDocument74 pagesشاشات انجليزي 99 ادعولناNoor MajaliNo ratings yet
- First Lecture - Nursing ProcessDocument57 pagesFirst Lecture - Nursing ProcessNoor MajaliNo ratings yet
- شاشات عربي 99Document11 pagesشاشات عربي 99Noor MajaliNo ratings yet
- The Sound Patterns of LanguageDocument17 pagesThe Sound Patterns of LanguageNoor MajaliNo ratings yet
- Hepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijDocument69 pagesHepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Management of Patients With Urinary Disorders: Dr. Lubna DwerijDocument74 pagesManagement of Patients With Urinary Disorders: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Osteoporosis: Dr. Lubna DwerijDocument26 pagesOsteoporosis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Citation 323943933Document1 pageCitation 323943933Noor MajaliNo ratings yet
- Autoimmune Processes: Dr. Lubna DwerijDocument46 pagesAutoimmune Processes: Dr. Lubna DwerijNoor MajaliNo ratings yet
- 31.chronic Diarrhea and MalabsorbtionDocument14 pages31.chronic Diarrhea and MalabsorbtionSajjal AliNo ratings yet
- 8 Grammar, Vocabulary, and Pronunciation B: Name - ClassDocument7 pages8 Grammar, Vocabulary, and Pronunciation B: Name - ClassDIEGO TORRES NINANo ratings yet
- Saudi drama: Commencements, efforts, and progression (4) - المسرح السعودي: البدايات، والجهود والتطورDocument14 pagesSaudi drama: Commencements, efforts, and progression (4) - المسرح السعودي: البدايات، والجهود والتطورYahya Saleh Hasan Dahami (يحيى صالح دحامي)No ratings yet
- Meta Ads Video FrameworkDocument4 pagesMeta Ads Video FrameworkFakhzan BadiranNo ratings yet
- Schmitt & Kremmel (2016) Interpreting Vocabulary Test Scores What Do Various Item Formats Tell Us About Learners' Ability To Employ WordsDocument17 pagesSchmitt & Kremmel (2016) Interpreting Vocabulary Test Scores What Do Various Item Formats Tell Us About Learners' Ability To Employ WordsEdward FungNo ratings yet
- What I Need To Know: Other Types of SequencesDocument14 pagesWhat I Need To Know: Other Types of SequencesLourdes MangahasNo ratings yet
- The 5 Step Blueprint PDFDocument39 pagesThe 5 Step Blueprint PDFNikkie DetaroNo ratings yet
- cp3505 Error Messages PDFDocument24 pagescp3505 Error Messages PDFbehzadNo ratings yet
- Dimensional AnalysisDocument27 pagesDimensional AnalysisOwais EngrNo ratings yet
- Kaushthubh MPhil Thesis - Finally Final CompleteDocument99 pagesKaushthubh MPhil Thesis - Finally Final CompleteKaustubh Das Dehlvi0% (1)
- Crowley - Liber RV Vel Spiritus Sub Figurâ CCVIDocument10 pagesCrowley - Liber RV Vel Spiritus Sub Figurâ CCVICelephaïs Press / Unspeakable Press (Leng)100% (3)
- Question Bank - : Reservoir EngineeringDocument2 pagesQuestion Bank - : Reservoir Engineeringshubham prasadNo ratings yet
- động từ bất quy tắc cấp 2Document2 pagesđộng từ bất quy tắc cấp 2Thu HuyềnNo ratings yet
- A Student's Contributions To Second Language Learning - Part II - Affective VariablesDocument12 pagesA Student's Contributions To Second Language Learning - Part II - Affective VariablesQuoc Bao MaiNo ratings yet
- Mutual Compromise Deed FormatDocument19 pagesMutual Compromise Deed Formatमहाराष्ट्र माझाNo ratings yet
- Four Against Darkness Fiction Heart of The LizardDocument93 pagesFour Against Darkness Fiction Heart of The LizardNixDieAlley0% (1)
- Micromaster Drive On Rockwell ControlLogix v10 enDocument52 pagesMicromaster Drive On Rockwell ControlLogix v10 enLuis Chuquimia GuillenNo ratings yet
- Trasitional Hypothermia PDFDocument3 pagesTrasitional Hypothermia PDFDella Putri Ariyani NasutionNo ratings yet
- Samkhya - Map of The Universe1Document1 pageSamkhya - Map of The Universe1Disha TNo ratings yet
- Psych Unit 4 Study GuideDocument16 pagesPsych Unit 4 Study GuideLauren ThompsonNo ratings yet
- How To Write Your ReusmeDocument7 pagesHow To Write Your ReusmeBrian Israel Avila FloresNo ratings yet
- Meetings With Remarkable Men: Commentary by Terry Winter OwensDocument7 pagesMeetings With Remarkable Men: Commentary by Terry Winter OwensManjushree777No ratings yet
- Simple Linear Regression With ExcelDocument39 pagesSimple Linear Regression With ExcelAbimanyu ShenilNo ratings yet
- Triboluminescence of Wintergreen Lifesavers Candy Edu 214Document8 pagesTriboluminescence of Wintergreen Lifesavers Candy Edu 214api-570743058No ratings yet