Professional Documents
Culture Documents
Malpositions and Malpresentations
Malpositions and Malpresentations
Uploaded by
iqra Hassan0 ratings0% found this document useful (0 votes)
20 views30 pagesThis document discusses obstetric complications arising from abnormal fetal positions and presentations during labor and delivery. Malpositions refer to abnormal positions of the fetal head, while malpresentations are any non-vertex presentations. Management may include monitoring labor progress, encouraging rotation or descent of the fetal position, and surgical delivery if needed due complications like obstructed labor. Specific approaches are outlined for managing occiput posterior positions, brow/face/compound presentations, and breech births. Caesarean delivery is usually recommended if the fetus is alive for non-vertex or obstructed positions.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses obstetric complications arising from abnormal fetal positions and presentations during labor and delivery. Malpositions refer to abnormal positions of the fetal head, while malpresentations are any non-vertex presentations. Management may include monitoring labor progress, encouraging rotation or descent of the fetal position, and surgical delivery if needed due complications like obstructed labor. Specific approaches are outlined for managing occiput posterior positions, brow/face/compound presentations, and breech births. Caesarean delivery is usually recommended if the fetus is alive for non-vertex or obstructed positions.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
20 views30 pagesMalpositions and Malpresentations
Malpositions and Malpresentations
Uploaded by
iqra HassanThis document discusses obstetric complications arising from abnormal fetal positions and presentations during labor and delivery. Malpositions refer to abnormal positions of the fetal head, while malpresentations are any non-vertex presentations. Management may include monitoring labor progress, encouraging rotation or descent of the fetal position, and surgical delivery if needed due complications like obstructed labor. Specific approaches are outlined for managing occiput posterior positions, brow/face/compound presentations, and breech births. Caesarean delivery is usually recommended if the fetus is alive for non-vertex or obstructed positions.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 30
Obstetric Complications
MALPOSITIONS AND MALPRESENTATIONS
MALPOSITIONS AND
MALPRESENTATIONS
Malpositions are abnormal positions of the
vertex of the fetal head (with the occiput as the
reference point) relative to the maternal pelvis.
Malpresentations are all presentations of the
fetus other than vertex.
The fetus is in an abnormal position or
presentation that may result in prolonged or
obstructed labour.
GENERAL MANAGEMENT
• Perform a rapid evaluation of the general condition of the
woman, fetal heart rate
• If the membranes have ruptured, note the colour of the
draining amniotic fluid:
• The presence of thick meconium indicates the need for
close monitoring
• The absence of fluid draining after rupture of the
membranes is an indication of reduced volume of
amniotic fluid, which may be associated with fetal
distress
• Provide encouragement and supportive care.
• Review progress of labour using a partograph.
DIAGNOSIS
• The most common presentation is the vertex of
the fetal head. If the vertex is not the presenting
part is called malpresentation.
• If the vertex is the presenting part, use
landmarks of the fetal skull to determine the
position of the fetal head.
DIAGNOSIS
DETERMINE THE POSITION OF THE
FETAL HEAD
• The fetal head normally engages in the maternal
pelvis in an occiput transverse position, with the
fetal occiput transverse in the maternal pelvis.
DETERMINE THE POSITION OF THE
FETAL HEAD
• With descent, the fetal
head rotates so that the
fetal occiput is
anterior in the
maternal pelvis. Failure
of an occiput
transverse position to
rotate to an occiput
anterior position should
be managed as an
occiput posterior
position.
ETERMINE THE POSITION OF THE
FETAL HEAD
• If the fetal head is well-flexed with
occiput anterior or occiput
transverse (in early labour), proceed
with birth of the baby.
• If the fetal head is not occiput
anterior, identify and manage the
malposition.
• If the fetal head is not the
presenting part or the fetal head is
not well-flexed, identify and
manage the malpresentation.
Diagnosis of malpositions
• Occiput posterior position occurs
when the fetal occiput is posterior in
relation to the maternal pelvis.
• On abdominal examination, the
lower part of the abdomen is
flattened, fetal limbs are palpable
anteriorly and the fetal heart may be
heard in the flank.
• On vaginal examination, the
posterior fontanelle is towards the
sacrum and the anterior fontanelle
may be easily felt if the head is
deflexed.
• Occiput transverse position occurs when the fetal
occiput is transverse to the maternal pelvis.
• If an occiput transverse position persists into the later
part of the first stage of labour, it should be managed as
an occiput posterior position.
SPECIFIC MANAGEMENT
OCCIPUT POSTERIOR POSITIONS
• Spontaneous rotation to the anterior position occurs in
90% of cases.
• Arrested labour may occur when the head does not
rotate and/or descend.
• Birth of the baby may be complicated by perineal tears
or extension of an episiotomy.
• If there are signs of obstruction but the fetal heart rate
is normal, allow the woman to walk around or change
position to encourage spontaneous rotation.
• If there are signs of obstruction and the fetal heart
rate is abnormal at any stage, perform a caesarean.
SPECIFIC MANAGEMENT
OCCIPUT POSTERIOR POSITIONS
• If the cervix is not fully dilated and there are no signs
of obstruction, augment labour with oxytocin.
• If the cervix is fully dilated but there is no descent in
the expulsive of the second stage of labour, assess for
signs of obstruction. If there are no signs of
obstruction, augment labour with oxytocin
• If the cervix is fully dilated:
• - If the fetal head is no more than 2/5 above the
symphysis pubis, or the leading bony edge of the fetal
head is at 0 station, assist birth of the baby using an
obstetric vacuum or forcep. - Otherwise, perform a
caesarean.
• In brow presentation, engagement is usually
impossible and arrested labour is common.
Spontaneous conversion to either vertex
presentation or face presentation can rarely
occur, particularly when the fetus is small or
when
• there is fetal death with maceration. It is unusual
for spontaneous conversion to occur with an
average-sized live fetus once the membranes
have ruptured.
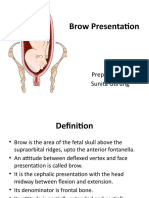
Brow presentation
• Brow presentation is caused
by partial extension of the
fetal head so that the occiput
is higher than the sinciput.
• On abdominal examination,
more than half the fetal head
is above the symphysis
pubis and the occiput is
palpable at a higher level than
the sinciput.
• On vaginal examination, the
anterior fontanelle and the
orbits are felt.
SPECIFIC MANAGEMENT
brow presentation
• If the fetus is alive, perform a caesarean.
• If the fetus is dead:
- If the cervix is not fully dilated, perform a
caesarean.
• - If the cervix is fully dilated:
• – Perform a craniotomy.
• – If the operator is not proficient in craniotomy,
perform a caesarean.
Face presentation
• Face presentation is caused by
hyperextension of the fetal head
so that neither the occiput nor the
sinciput is palpable on vaginal
examination
• On abdominal examination, a
groove may be felt between the
occiput and the back.
• On vaginal examination, the face
is palpated, the examiner’s finger
enters the mouth easily and the
bony jaws are felt.
Specific Management
Face presentation
• CHIN-ANTERIOR POSITION:
• If the cervix is fully dilated:
• - Allow normal childbirth to proceed.
• - If there is slow progress and no sign of obstruction,
augment labour with oxytocin.
• - If descent is unsatisfactory, assist the birth of the baby
using forceps.
• If the cervix is not fully dilated and there are no signs
of obstruction, augment labour using oxytocin, Review
progress as with vertex presentation.
Specific Management
Face presentation
• CHIN-POSTERIOR POSITION:
• • If the cervix is fully dilated or not fully dilated perform a
caesarean.
• • If the fetus is dead:
• - Perform a craniotomy
• - If the operator is not proficient in craniotomy, perform a
caesarean.
Compound presentation
• Compound presentation occurs
when an arm prolapses
alongside the presenting part.
• Both the prolapsed arm and
the fetal head present in the
pelvis simultaneously.
Specific Managemant
Compound presentation
• Spontaneous vaginal birth can occur only when the fetus
is very small or dead and macerated.
• Arrested labour occurs in the expulsive phase of the
second stage of labour.
• Replacement of the prolapsed arm is sometimes
possible:
• - Assist the woman in assuming the knee-chest
position.
• - Push the arm above the pelvic brim and hold it there
until a contraction pushes the head into the pelvis.
• - Proceed with management for normal childbirth
Specific Managemant
Compound presentation
Breech presentation
•
Breech presentation occurs when the buttocks and/or
the feet are the presenting parts.
• On abdominal examination, the head is felt in the
upper abdomen and the breech in the pelvic brim.
• Auscultation locates the fetal heart higher than
expected with a vertex presentation.
• On vaginal examination during labour, the buttocks
and/or feet are felt; thick, dark meconium is normal.
Types of Breech
Complete (flexed) breech
presentation occurs when both legs
are flexed at the hips and knees.
Frank (extended) breech
presentation occurs when both legs
are flexed at the hips and extended at
the knees.
Footling breech presentation occurs
when a leg is extended at the hip and
the knee.
Specific Management
Breech Presentation
• EARLY LABOUR:
• Attempt external cephalic version
• vaginal birth is possible;
• there are no complications (e.g. fetal growth restriction,
uterine bleeding, previous caesarean birth, fetal
abnormalities, twin pregnancy, hypertension, fetal death).
• If external version is successful, proceed with normal
childbirth.
• • If external version fails, proceed with vaginal breech
birth (below) or caesarean.
Specific Management
Breech Presentation
• VAGINAL BREECH BIRTH:
• A vaginal breech birth by a skilled health care provider is
safe and feasible under the following conditions:
- complete or frank breech
- adequate clinical pelvimetry;
- fetus is not too large;
- no previous caesarean for cephalopelvic disproportion;
- fetal head is flexed.
Specific Management
Breech Presentation
• Examine the woman regularly and record progress on a
partograph
• • If the membranes rupture, examine the woman
immediately to exclude cord prolapse.
• • Note: Do not rupture the membranes.
• • If the cord prolapses and birth is not imminent, perform
a caesarean
• • If there are fetal heart rate abnormalities ) or prolonged
labour, perform a caesarean
• Note: Meconium is common with breech labour and is
not a sign of fetal distress if the fetal heart rate is normal.
COMPLICATIONS
Fetal complications of breech presentation include:
• cord prolapse;
• birth trauma as a result of extended arm or
head, incomplete dilatation of the cervix, or
cephalopelvic disproportion;
• asphyxia from cord prolapse, cord
compression, placental detachment or
entrapped head;
• damage to abdominal organs; and
• broken neck.
Specific Management
Breech Presentation
• CAESAREAN BIRTH FOR BREECH PRESENTATION
• • A caesarean birth is safer than vaginal breech birth and
recommended in cases of:
- double footling breech;
- a small or malformed pelvis;
- a very large fetus;
- a previous caesarean for cephalopelvic disproportion
- a hyperextended or deflexed head.
• Note: Elective caesarean does not improve the outcome
in preterm breech birth.
Transverse presentation
• Transverse lie and shoulder
presentation occur when the long axis
of the fetus is transverse. shoulder is
typically the presenting part.
• On abdominal examination, neither
the head nor the buttocks can be felt at
the symphysis pubis and the head is
usually felt in the flank.
• On vaginal examination, a shoulder
may be felt, but not always. An arm
may prolapse, and the elbow, arm or
hand may be felt in the vagina.
Specific Management
Transverse Presentation
• If a woman is in early labour and the membranes are
intact, attempt external version
• In modern practice, persistent transverse lie in labour is
managed by performing a caesarean whether the fetus
is alive or dead.
You might also like
- Dragon Mother A New Look at The Female Psyche by Michael Tsarion - Z Lib - OrgDocument219 pagesDragon Mother A New Look at The Female Psyche by Michael Tsarion - Z Lib - OrgRod P100% (1)
- Preparing for a Gentle Birth: The Pelvis in PregnancyFrom EverandPreparing for a Gentle Birth: The Pelvis in PregnancyRating: 4 out of 5 stars4/5 (8)
- Detailed Lesson Plan in Science 10Document8 pagesDetailed Lesson Plan in Science 10Sheena Salvador100% (6)
- Core Functions: 80 %: 5 - Outstanding 4 - Very Satisfactory 3 - Satisfactory 2 - Unsatisfactory 1 - PoorDocument3 pagesCore Functions: 80 %: 5 - Outstanding 4 - Very Satisfactory 3 - Satisfactory 2 - Unsatisfactory 1 - PoorChuchai Balili100% (1)
- MalpresentationDocument37 pagesMalpresentationLovely SarangiNo ratings yet
- Problems With The PassengerDocument65 pagesProblems With The Passengermark Orpilla100% (1)
- Dystocia Fetal Malposition and Malpresentation DescriptionDocument7 pagesDystocia Fetal Malposition and Malpresentation Descriptionemi readNo ratings yet
- Malpresentation and MalpositionDocument33 pagesMalpresentation and MalpositionPeprah Ondiba100% (1)
- Abnormal Lie and PresentationsDocument31 pagesAbnormal Lie and PresentationsNattasha StephenNo ratings yet
- Complications With The Passenger 2Document77 pagesComplications With The Passenger 2JudyNo ratings yet
- 3 Problems With The Passenger and Powers of LaborDocument105 pages3 Problems With The Passenger and Powers of LaborRaquel M. Mendoza100% (1)
- MalpresentationDocument37 pagesMalpresentationLovely SarangiNo ratings yet
- Fetal MalpresentationDocument83 pagesFetal MalpresentationArianJubaneNo ratings yet
- Module 10 COMMON OBSTETRIC EMERGENCIESDocument53 pagesModule 10 COMMON OBSTETRIC EMERGENCIESSPE CommitteeNo ratings yet
- MK Fetal Lie and Presentation (OBGY)Document9 pagesMK Fetal Lie and Presentation (OBGY)Moses Jr KazevuNo ratings yet
- Problems With Passenger and PowerDocument6 pagesProblems With Passenger and PowerhoohooNo ratings yet
- MAL PRESENTATIONS BreechDocument43 pagesMAL PRESENTATIONS Breechrachael annorNo ratings yet
- CHAPTER 2 High Risk Labor and DeliveryDocument26 pagesCHAPTER 2 High Risk Labor and Deliveryjacobprince0016No ratings yet
- Normal and Abnormal Present IonDocument31 pagesNormal and Abnormal Present IondeemNo ratings yet
- Obstetrics & Gyn II PDF Abnormal PDFDocument305 pagesObstetrics & Gyn II PDF Abnormal PDFmaezu100% (3)
- Malposition/Malpresentation: DR - Nagina Bibi Ap Obgyn CMCDocument27 pagesMalposition/Malpresentation: DR - Nagina Bibi Ap Obgyn CMCAli SohailNo ratings yet
- Tdmu Edu - UaDocument48 pagesTdmu Edu - UaCoral Srinivasa Ramalu100% (1)
- Abnormal Labor Lec 2Document40 pagesAbnormal Labor Lec 2Zahraa HasanNo ratings yet
- BreechDocument44 pagesBreechnohazz0% (1)
- Ob Mal PresentationsDocument13 pagesOb Mal PresentationsabigailmalicadNo ratings yet
- Abnormal Labour: Perceptor: Dr. Nurul Islamy, M. Kes., Sp. OGDocument54 pagesAbnormal Labour: Perceptor: Dr. Nurul Islamy, M. Kes., Sp. OGramadhiena destia100% (1)
- Fetal MalpresentationDocument28 pagesFetal MalpresentationAhmed Gh Al-zechrawiNo ratings yet
- MalpositionDocument29 pagesMalpositionhacker ammerNo ratings yet
- Problems With The PassengerDocument58 pagesProblems With The PassengerJim NavarroNo ratings yet
- Fetal Malpresentations - IIDocument11 pagesFetal Malpresentations - IIAhmed Gh Al-zechrawiNo ratings yet
- Cord Prolapse Final (Dr. P Garai)Document33 pagesCord Prolapse Final (Dr. P Garai)Akash ChakrabortyNo ratings yet
- Module 5 Part 1Document65 pagesModule 5 Part 1D A M N E R ANo ratings yet
- Abnormal Lie: - Abnormal Lie Consists of Two Types: Transverse Lie Oblique LieDocument21 pagesAbnormal Lie: - Abnormal Lie Consists of Two Types: Transverse Lie Oblique LieBharat ThapaNo ratings yet
- Cephalopelvic Disproportion and Obstructed LabourDocument40 pagesCephalopelvic Disproportion and Obstructed Labournighat khanNo ratings yet
- Lecture 6 Breach Presentation Transversal Oblique LieDocument51 pagesLecture 6 Breach Presentation Transversal Oblique Lietanmai nooluNo ratings yet
- Malpositions and Malpresentations FinalDocument47 pagesMalpositions and Malpresentations Finalsanthiyasandy83% (12)
- Breech Presentation: - by Drtejaswini K.RDocument41 pagesBreech Presentation: - by Drtejaswini K.Rjssamc prasootitantraNo ratings yet
- Lecture 5 - Obsteric Emergencies-1Document103 pagesLecture 5 - Obsteric Emergencies-1Priscilla Sarah PayneNo ratings yet
- Mal Positions and Mal PresentationsDocument229 pagesMal Positions and Mal PresentationsPriscilla Sarah PayneNo ratings yet
- Mechanism of LabourDocument31 pagesMechanism of Labourrachael annorNo ratings yet
- Breech & MalpositionDocument41 pagesBreech & MalpositionAnuradha Roopchand100% (1)
- Assisted Vaginal DeliveryDocument26 pagesAssisted Vaginal Deliveryapi-3705046100% (5)
- Operative Vaginal Delivery: Presenter: Mbi Mbi Year of Study: MBBS V Rotation: OBGYN Date: 25/02/15Document35 pagesOperative Vaginal Delivery: Presenter: Mbi Mbi Year of Study: MBBS V Rotation: OBGYN Date: 25/02/15A MusaverNo ratings yet
- Malpresentation and Malposition - BreechDocument21 pagesMalpresentation and Malposition - BreechNishaThakuri100% (1)
- Breech presentation G2Document21 pagesBreech presentation G2Rose NyamburaNo ratings yet
- Malposition AND Malpresentat ION: Regala, Bianca Ysabelle M. BSN Ii - B Rle Group IiiDocument57 pagesMalposition AND Malpresentat ION: Regala, Bianca Ysabelle M. BSN Ii - B Rle Group IiiBiway RegalaNo ratings yet
- William Reading Abnormal LaborDocument14 pagesWilliam Reading Abnormal LaborLeo SSNo ratings yet
- Normal Labor: Kevin Marcial I. Aralar, MD 1 Year ResidentDocument46 pagesNormal Labor: Kevin Marcial I. Aralar, MD 1 Year ResidentKevin AralarNo ratings yet
- Case Presentation On Normal LaborDocument62 pagesCase Presentation On Normal LaborB34-YvesJethro ReyesNo ratings yet
- Complications During Labor and BirthDocument108 pagesComplications During Labor and BirthAlphine DalgoNo ratings yet
- Module 7 ASSISTED DELIVERYDocument18 pagesModule 7 ASSISTED DELIVERYSPE CommitteeNo ratings yet
- Normal Abnormal LabourDocument63 pagesNormal Abnormal LabourFelicianna Ashwinie StanleyNo ratings yet
- Intrapartum EmergenciesDocument34 pagesIntrapartum EmergenciesDrChauhanNo ratings yet
- Brow PresentationDocument9 pagesBrow PresentationGROOT GamingYTNo ratings yet
- Dystocia V2Document12 pagesDystocia V2Aljon AgustinNo ratings yet
- Cephalopelvic Disproportion, Obstructed Lab Our, UterineDocument49 pagesCephalopelvic Disproportion, Obstructed Lab Our, UterineKerod AbebeNo ratings yet
- Fetal MalpresentationDocument13 pagesFetal MalpresentationJhing Rodriguez Borjal75% (4)
- Forceps DeliveryDocument34 pagesForceps DeliveryBharat ThapaNo ratings yet
- Obstetric Forceps: Dr. Sourav Chowdhury Senior Resident OBG, IQCMCDocument22 pagesObstetric Forceps: Dr. Sourav Chowdhury Senior Resident OBG, IQCMCRitik AgarsenNo ratings yet
- Breech Presenta, On: Persists at Term in 3 - 4 % of Singleton DeliveriesDocument47 pagesBreech Presenta, On: Persists at Term in 3 - 4 % of Singleton DeliveriesBom TnaNo ratings yet
- Group II Makati Medical Center m8 1Document107 pagesGroup II Makati Medical Center m8 1CASSANDRAJUL VARINNo ratings yet
- zBREECH PRESENTATION AND DELIVERYDocument5 pageszBREECH PRESENTATION AND DELIVERYAlbert Francis BialaNo ratings yet
- Holistic Childbirth Manual: Maternal Health Manuals, #2From EverandHolistic Childbirth Manual: Maternal Health Manuals, #2No ratings yet
- Biology Practice Questions - 1Document66 pagesBiology Practice Questions - 1Slick Life VlogsNo ratings yet
- OB GYN CasePre FinalDocument82 pagesOB GYN CasePre FinalMarjorie Lahaylahay AlabataNo ratings yet
- AaryajananiDocument3 pagesAaryajananijananisasi68No ratings yet
- Neonatal Vitamin K Administration and Childhood Cancer in The North of EnglandDocument17 pagesNeonatal Vitamin K Administration and Childhood Cancer in The North of EnglandMilko HristovNo ratings yet
- Child Birth Practices Across Cultures and Their ImplicationsDocument14 pagesChild Birth Practices Across Cultures and Their ImplicationsChintu ZoboloNo ratings yet
- UNIT - II - Organization, Staffing and Functions of Urban Health Services - AnandDocument38 pagesUNIT - II - Organization, Staffing and Functions of Urban Health Services - AnandAnand gowda73% (15)
- Parents' Perception On Teenage Pregnancy: A Qualitative ResearchDocument15 pagesParents' Perception On Teenage Pregnancy: A Qualitative ResearchErica Mae Rivarez100% (1)
- Journal Reading II - Dr. Yuda LutfiadiDocument13 pagesJournal Reading II - Dr. Yuda LutfiadiTegar Dwi Prakoso NurdionoNo ratings yet
- Research RefDocument18 pagesResearch Refbibibebebaby leeleeNo ratings yet
- Case Study (Preeclampsia)Document6 pagesCase Study (Preeclampsia)Jobelle AcenaNo ratings yet
- Oligohydramnios: DR Mona Shroff WWW - Obgyntoday.infoDocument32 pagesOligohydramnios: DR Mona Shroff WWW - Obgyntoday.infoNinaNo ratings yet
- Prenatal DevelopmentDocument66 pagesPrenatal DevelopmentBlessie NgitngitNo ratings yet
- NCM 104 Lec Reviewer FinalsDocument11 pagesNCM 104 Lec Reviewer FinalsFERNANDEZ, RELLY ANDREWNo ratings yet
- Bioethics and Its Application in Various Health SettingsDocument4 pagesBioethics and Its Application in Various Health SettingsXandra BasnilloNo ratings yet
- Antepartal Care: Prepared By: Shalini Santiago-Barroso, RN MANDocument11 pagesAntepartal Care: Prepared By: Shalini Santiago-Barroso, RN MANJabelle Mae DoteNo ratings yet
- 1 Anatomy and Physiology of ReproductionDocument31 pages1 Anatomy and Physiology of Reproductionjose mari chanNo ratings yet
- Secondary - Health 78 - Lesson 2 - Family PlanningDocument13 pagesSecondary - Health 78 - Lesson 2 - Family PlanningGiselle TapawanNo ratings yet
- 11882-Article Text-58480-1-10-20220915Document8 pages11882-Article Text-58480-1-10-20220915Belle Denniese FontelarNo ratings yet
- Vampire: The Masquerade Revised FAQDocument9 pagesVampire: The Masquerade Revised FAQGnomeMadeIonNo ratings yet
- Endometrial BiopsyDocument13 pagesEndometrial BiopsyChanta MaharjanNo ratings yet
- Maternal Child CareDocument4 pagesMaternal Child Carecialina AlvezSevillaNo ratings yet
- Anemia in PregnancyDocument24 pagesAnemia in PregnancyAzwanie Ali100% (1)
- 2945 de Costa & Howat 2007 Front Pages PDFDocument15 pages2945 de Costa & Howat 2007 Front Pages PDFleh.mo9315No ratings yet
- Mmeanoba-V KursiDocument91 pagesMmeanoba-V KursinatitukaNo ratings yet
- The Reliability of The Neonatal Oral-Motor Assessment Scale: KeywordsDocument6 pagesThe Reliability of The Neonatal Oral-Motor Assessment Scale: KeywordsJosé Ignacio SepúlvedaNo ratings yet
- Chap 5 Hormonal Response To ExerciseDocument53 pagesChap 5 Hormonal Response To ExerciseAnnie KhanNo ratings yet
- Lalana Newborn ResuscitationDocument55 pagesLalana Newborn ResuscitationAthenaeum Scientific PublishersNo ratings yet