Professional Documents
Culture Documents
Pheochromocytoma
Pheochromocytoma
Uploaded by
nemo sh0 ratings0% found this document useful (0 votes)
6 views19 pagesPheochromocytoma is a rare tumor that arises from chromaffin cells in the adrenal medulla or sympathetic ganglia. It secretes excess catecholamines, causing symptoms like headaches, sweating, and tachycardia. The document discusses the definition, causes, clinical presentations, diagnostic workup, management, and familial syndromes associated with pheochromocytoma. Genetic testing is recommended if the patient has bilateral or early-onset pheochromocytoma, paraganglioma, or a family history of these tumors. Surgery is the treatment of choice and requires preoperative preparation to control blood pressure.
Original Description:
Original Title
Pheochromocytoma copy
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPheochromocytoma is a rare tumor that arises from chromaffin cells in the adrenal medulla or sympathetic ganglia. It secretes excess catecholamines, causing symptoms like headaches, sweating, and tachycardia. The document discusses the definition, causes, clinical presentations, diagnostic workup, management, and familial syndromes associated with pheochromocytoma. Genetic testing is recommended if the patient has bilateral or early-onset pheochromocytoma, paraganglioma, or a family history of these tumors. Surgery is the treatment of choice and requires preoperative preparation to control blood pressure.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
6 views19 pagesPheochromocytoma
Pheochromocytoma
Uploaded by
nemo shPheochromocytoma is a rare tumor that arises from chromaffin cells in the adrenal medulla or sympathetic ganglia. It secretes excess catecholamines, causing symptoms like headaches, sweating, and tachycardia. The document discusses the definition, causes, clinical presentations, diagnostic workup, management, and familial syndromes associated with pheochromocytoma. Genetic testing is recommended if the patient has bilateral or early-onset pheochromocytoma, paraganglioma, or a family history of these tumors. Surgery is the treatment of choice and requires preoperative preparation to control blood pressure.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 19
Pheochromocytoma
Supervised by: dr. Intessar sultan
Presented by:
•Neama shabib 1621161
•Dalal alnajjar 1621149
•Jana babaqi 1621162
Learning objectives
At the end of the lecture the student will be able to:
• Define pheochromocytoma- paraganglioma
• Identify underlying causes of pheochromocytoma
• Identify the associated familial syndromes with pheochromocytoma
• Recognize the different clinical presentations of pheochromocytoma
• Identify how to diagnose pheochromocytoma
• Identify how to manage pheochromocytoma
Cromaffine cells (pheochromocyte) : orginate from the neural crust (embryo)
Neuroendocrine cell > neurohormones ( chemicals produced from neuron cells released on the blood)
- adrenaline
- noradrenaline
Migrates to areas adjacent to the sympathetic ganglia:
adrenal medulla : phenochromocytoma
Others : paraganglioma or extra-adrenal
Definition
,Pheochromocytoma is a rare benign neuroendocrine tumor •
Arise from •
chromaffin cells of the adrenal medulla
sympathetic ganglia (extra-adrenal pheochromocytomas ‘’paraganglioma’’)
.Active tumor : Secretion of excess catecholamines •
Prevalence among hypertensive patients is only 0.2% •
of cases are discovered incidentally during abdominal CT or MRI 60% •
serious cardiovascular complications •
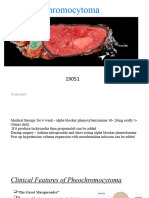
:Tumor characteristics Rule f 10
• 10% multiple.
• 10% extraadrenal (catecholamine-secreting paragangliomas.
• 10% malignant:
• known only by local invasion or metastases not by Histopathology
• So long-term follow-up is indicated in all patients to exclude malignancy
• Patients with the succinate dehydrogenase (SDH) subunit B mutations are
more likely to develop metastatic disease
Symptoms (50% of cases)
• the clinical presentation may be variable
• the classic triad: episodic headache, sweating, and tachycardia in association with
hypertension.
• Paroxysmal elevations in blood pressure
• Orthostatic hypotension: low plasma volume – secretion of epinephrine
• Cardiomyopathy
• insulin resistance- diabetes
• Rare: pheochromocytoma multisystem crisis.
• hypertension or hypotension, hyperthermia (temperature >40°C), mental status
changes, and organ dysfunction
Familial cases
of pheochromocytoma cases 40% •
Bilateral adrenal tumors or multiple paragangliomas •
Autosomal dominant •
Succinate dehydrogenase subunit gene variants SDH •
Multiple endocrine neoplasia type 2 (MEN2): RET oncogen -1
MEN2A: 1ry hyperparathyroidism, medullary thyroid carcinoma, pheochromocytoma •
MEN2B: medullary thyroid carcinoma, pheochromocytoma, mucocutanous neuroma •
von Hippel-Lindau (VHL-II) disease (retinal angiomas,rena cell carcinoma, -2
hemangioblastoma) 3- Neurofibromatosis NF 1: neurofibroma, café au lait spots,
axillary freckling
Neurofibromatosis
Differential diagnosis
• Anxiety
• Thyrotoxicosis
• Angina
• Hypoglycaemia
Indication for Evaluation
• Suspected cases (low and high index)
• Adrenal incidentalome
• paroxysmal elevations in blood pressure ( precipitating factors)
• diagnostic procedures as colonoscopy
• induction of anaesthesia
• Surgery
• consumption of food high in tyramine
• with certain drugs (beta blockers, tricyclic antidepressants, corticosteroids,
metoclopramide or MAOIs
Initial biochemical tests
1- Low index of suspicion: 24-hour urinary catecholamines and metanephrines.
• Resistant hypertension
• Hyperadrenergic spells
2- High index of suspicion: plasma metanephrines
• Family history of pheochromocytoma
• Genetic syndrome as MEN2
• Past history of pheochromocytoma
• Imaging criteria of adrenal incidentalome
Imaging
Imaging studies should be performed only after biochemical studies have confirmed
the diagnosis of pheochromocytoma.
• CT/MRI can detect tumors but non specific due to high prevalence of adrenal
incidentalomas
•If CT/MRI negative with high suspicions: MIBG scan
•If suspect metastasis: PET scan
MRI
MIBG PET
Genetic testing
if a patient has one or more of the following •
Paraganglioma .1
Bilateral adrenal pheochromocytoma .2
Unilateral adrenal pheochromocytoma and a family history of .3
pheochromocytoma/paraganglioma
Unilateral adrenal pheochromocytoma onset at a young age less than 45 .4
Other clinical findings suggestive of one of the syndromic disorders .5
Surgery for adrenal pheochromocytomas
• Surgery is indicated for patients with biochemical documentation
• Laparoscopic adrenalectomy is better than open surgery
• Complete bilateral adrenalectomy in familial cases with diffuse disease to
avoid recurrence
Perioperative preparation
• Start with alpha-adrenergic blockade: phenoxybenzamine is the first-line
• Add low dose beta blocker cautiously after adequate alpha blockade
• Increase dose to control tachycardia (goal 60 - 80 BPM).
• NEVER start with beta-adrenergic blocker.
• Intraoperative:
• manage with intravenous saline to hydrate patient as after removal of the
tumour severe hypotension and shock may develop
REFERENCE
You might also like
- Hema 2 - Prelim Topic 1-Intro To HemostasisDocument4 pagesHema 2 - Prelim Topic 1-Intro To HemostasisLowenstein JenzenNo ratings yet
- Epilepsy Management Plan TemplateDocument2 pagesEpilepsy Management Plan TemplateIPNo ratings yet
- Impaire Spontaneous VentilationDocument4 pagesImpaire Spontaneous VentilationSkyla FiestaNo ratings yet
- General Medical Certificate 2018Document1 pageGeneral Medical Certificate 2018sheryarbismal100% (3)
- Adrenal Medulla: By: DR Ismail, Macharia, Karimi, Thitai, Nigel, Muriithi, Maweu, Patel, Oliver FACILITATOR: Prof. KigonduDocument46 pagesAdrenal Medulla: By: DR Ismail, Macharia, Karimi, Thitai, Nigel, Muriithi, Maweu, Patel, Oliver FACILITATOR: Prof. KigonduJustine NyangaresiNo ratings yet
- PheochromocytomaDocument43 pagesPheochromocytomaJason MirasolNo ratings yet
- B17M4L4B PheochromocytomaDocument6 pagesB17M4L4B PheochromocytomaJoaquim RodriguezNo ratings yet
- PheochromocytomaDocument5 pagesPheochromocytomahussain AltaherNo ratings yet
- PHEOCHROMOCYTOMADocument37 pagesPHEOCHROMOCYTOMAYosi OktarinaNo ratings yet
- Pheochromocytoma: - The Incidence of Pheochromocytoma Is Approximately 1Document15 pagesPheochromocytoma: - The Incidence of Pheochromocytoma Is Approximately 1Suman KotwalNo ratings yet
- PHEOCHROMOCYTOMADocument15 pagesPHEOCHROMOCYTOMASteph100% (1)
- 1 s2.0 S0085253815518541 MainDocument6 pages1 s2.0 S0085253815518541 MainaripNo ratings yet
- Pheochromocytoma Presentation, Diagnosis and TreatmentDocument9 pagesPheochromocytoma Presentation, Diagnosis and TreatmentdrSuriana DwiNo ratings yet
- Paraneoplastic Syndromes: Dr. Clara NovenaDocument86 pagesParaneoplastic Syndromes: Dr. Clara NovenaAnggara HNo ratings yet
- Essentials of Diagnosis: Pheochromocytoma & ParagangliomaDocument10 pagesEssentials of Diagnosis: Pheochromocytoma & ParagangliomaAbdul QuyyumNo ratings yet
- Adrenal GlandsDocument116 pagesAdrenal GlandsBrandon AreteNo ratings yet
- LEC 4 Adrenal HyperfunctionDocument39 pagesLEC 4 Adrenal Hyperfunctionalhusien.abd2000No ratings yet
- PHEOCHROMOCYTOMASDocument5 pagesPHEOCHROMOCYTOMASasaaa1No ratings yet
- Pituitary, Thyroid Endocrine 2023Document55 pagesPituitary, Thyroid Endocrine 2023Visura PrabodNo ratings yet
- Pheochromocytoma and HyperaldosteronismDocument18 pagesPheochromocytoma and HyperaldosteronismMouhammad DawoudNo ratings yet
- Pheochromocytoma and Paraganglioma: PearlsDocument14 pagesPheochromocytoma and Paraganglioma: PearlsMohammed FaragNo ratings yet
- Hyperparathyroidism Mancini 100401060921 Phpapp02Document41 pagesHyperparathyroidism Mancini 100401060921 Phpapp02anand787No ratings yet
- Seminar: Jacques W M Lenders, Graeme Eisenhofer, Massimo Mannelli, Karel PacakDocument11 pagesSeminar: Jacques W M Lenders, Graeme Eisenhofer, Massimo Mannelli, Karel PacakAlexandru CozmaNo ratings yet
- Pathology of Endocrine System: Dr. Nesreen Bataineh MD, FrcpathDocument20 pagesPathology of Endocrine System: Dr. Nesreen Bataineh MD, FrcpathQutaybah JahmanyNo ratings yet
- Dr. A. Ramcharan's Firm Thursday 31 Match 2011Document56 pagesDr. A. Ramcharan's Firm Thursday 31 Match 2011Ronald ChongNo ratings yet
- Pheochromocytoma - WikipediaDocument1 pagePheochromocytoma - WikipediaIulian GherasimNo ratings yet
- FeocromocitomaDocument15 pagesFeocromocitomaRaul GascueñaNo ratings yet
- Anxiety Due To General Medical ConditionDocument15 pagesAnxiety Due To General Medical ConditionKatie Anderson100% (1)
- Brain Tumours PresentationDocument19 pagesBrain Tumours PresentationBonfaceNo ratings yet
- TBMDocument47 pagesTBMstephen X-SILVERNo ratings yet
- Anesthetic Management in Conn's Syndrome and PheochromocytomaDocument35 pagesAnesthetic Management in Conn's Syndrome and PheochromocytomaShashikant RamNo ratings yet
- Meeting 7 Endocrine SystemDocument28 pagesMeeting 7 Endocrine SystemNader KhouryNo ratings yet
- Endocrine Pathology - UntadDocument158 pagesEndocrine Pathology - UntadfahrulrozyNo ratings yet
- FeocromocitomaDocument41 pagesFeocromocitomaDauris garcia diazNo ratings yet
- Pheo 51Document13 pagesPheo 51kushalNo ratings yet
- PheochromocytomaDocument6 pagesPheochromocytomaVenkatesh Tammineni100% (1)
- Actualizaciones Oaragangliomas Sociedad EndocrinoDocument9 pagesActualizaciones Oaragangliomas Sociedad EndocrinoCharly FlowNo ratings yet
- 7.1 Pituitary Patho 28Document23 pages7.1 Pituitary Patho 28Namomsa W.No ratings yet
- Disorders of Adrenal Medulla OLUSAYODocument33 pagesDisorders of Adrenal Medulla OLUSAYOIiiNo ratings yet
- 151 English-1Document10 pages151 English-1Michael KaiNo ratings yet
- Cancer and CarcenoidDocument8 pagesCancer and Carcenoidmm7--No ratings yet
- SDL 10 BMS16091064Document5 pagesSDL 10 BMS16091064Jonathan YeohNo ratings yet
- 441 PheochromoDocument48 pages441 Pheochromograyburn_10% (1)
- Adrenal DisordersDocument57 pagesAdrenal Disordersnashadmohammed99No ratings yet
- Nervous System Module (Parasitology)Document13 pagesNervous System Module (Parasitology)NAOGE GEDEFANo ratings yet
- Endocrine TumorsDocument107 pagesEndocrine TumorsBinit BharatiNo ratings yet
- HyperparathyroidismDocument41 pagesHyperparathyroidismShabeel PnNo ratings yet
- Intracranial NeoplasmaDocument21 pagesIntracranial NeoplasmaLuvi PujiNo ratings yet
- 4th Problem Emergency Medicine Group 1Document82 pages4th Problem Emergency Medicine Group 1Jonathan TandajuNo ratings yet
- Adrenal Tumor-Pheochromocytoma 10-10-19Document30 pagesAdrenal Tumor-Pheochromocytoma 10-10-19JessicaNo ratings yet
- Surgical Pathology For Dentistry Students - Surgical Pathology of Thyroid and Adrenal GlandsDocument38 pagesSurgical Pathology For Dentistry Students - Surgical Pathology of Thyroid and Adrenal Glandssorin niky mocanu100% (1)
- Parathyroid Gland and Other Endocrine GlandsDocument35 pagesParathyroid Gland and Other Endocrine GlandsDrRahma Ali HeissNo ratings yet
- Path Lab Name: Onyedika Egbujo No: #671 Topic: PheochromocytomaDocument4 pagesPath Lab Name: Onyedika Egbujo No: #671 Topic: PheochromocytomaOnyedika EgbujoNo ratings yet
- Adrenal Disorders - RaasiDocument39 pagesAdrenal Disorders - RaasiArun kumarNo ratings yet
- Adrenal DisordersDocument36 pagesAdrenal DisordersMalueth AnguiNo ratings yet
- MedulloblastomaDocument29 pagesMedulloblastomaFaizyabNo ratings yet
- 10 1 Paraneoplastic SyndromesDocument31 pages10 1 Paraneoplastic SyndromesTeky WidyariniNo ratings yet
- Disorders of The Adrenal Glands: Adrenal Cortical Adenoma and CarcinomaDocument9 pagesDisorders of The Adrenal Glands: Adrenal Cortical Adenoma and Carcinomahussain AltaherNo ratings yet
- Clinical Seminar On PheochromocytomaDocument9 pagesClinical Seminar On PheochromocytomaParvathy JoshyNo ratings yet
- Pheochromocytoma: Pheochromocytoma: The Facts You Need To KnowDocument5 pagesPheochromocytoma: Pheochromocytoma: The Facts You Need To KnowadityaNo ratings yet
- Disorders of The Adrenal Glands: Adrenal Cortical Adenoma and CarcinomaDocument9 pagesDisorders of The Adrenal Glands: Adrenal Cortical Adenoma and Carcinomahussain AltaherNo ratings yet
- Pheochromocytomas, Paragangliomas and Disorders of the Sympathoadrenal System: Clinical Features, Diagnosis and ManagementFrom EverandPheochromocytomas, Paragangliomas and Disorders of the Sympathoadrenal System: Clinical Features, Diagnosis and ManagementLewis LandsbergNo ratings yet
- A Simple Guide to Pheochromocytoma (Updated), Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Pheochromocytoma (Updated), Diagnosis, Treatment and Related ConditionsNo ratings yet
- Suture & InstrumentsDocument32 pagesSuture & Instrumentsnemo shNo ratings yet
- Arterial ExaminationDocument34 pagesArterial Examinationnemo shNo ratings yet
- 22-Shoulder JointDocument24 pages22-Shoulder Jointnemo shNo ratings yet
- GynecologyPelvic Ultrasound Made Easy Step-By-Step GuideDocument31 pagesGynecologyPelvic Ultrasound Made Easy Step-By-Step Guidenemo shNo ratings yet
- Nursing Care Plan For Disturbed Sleep PatternDocument4 pagesNursing Care Plan For Disturbed Sleep PatternMarife Lipana Reyes100% (3)
- Microbial CarcinogensDocument33 pagesMicrobial CarcinogensJacob ThomasNo ratings yet
- Treatment of Disorders in Childhood and Adolescence Fourth Edition Mitchell J Prinstein Online Ebook Texxtbook Full Chapter PDFDocument69 pagesTreatment of Disorders in Childhood and Adolescence Fourth Edition Mitchell J Prinstein Online Ebook Texxtbook Full Chapter PDFanabaldyrstin100% (7)
- Toxicokinetics: Clinical Toxicology 4 Pharm DDocument23 pagesToxicokinetics: Clinical Toxicology 4 Pharm DFeroze FathimaNo ratings yet
- Case PresentationDocument36 pagesCase Presentationalmas khanNo ratings yet
- Types of PranayamaDocument2 pagesTypes of Pranayamamonsoon2206No ratings yet
- Blunt Trauma AbdomenDocument41 pagesBlunt Trauma AbdomenSanthanu SukumaranNo ratings yet
- Note by Izza - Acute Decompensated Heart FailureDocument3 pagesNote by Izza - Acute Decompensated Heart FailureIzzati N. SariNo ratings yet
- The Added Value of Clinical Hypnosis To FND Treatment: DR Jason Price Consultant Clinical NeuropsychologistDocument21 pagesThe Added Value of Clinical Hypnosis To FND Treatment: DR Jason Price Consultant Clinical Neuropsychologistmeity100% (1)
- Board EamDocument55 pagesBoard Eamjoycevillamor100% (1)
- DR - Elamaran.E Senior Resident Dept. of CTVS, JIPMERDocument43 pagesDR - Elamaran.E Senior Resident Dept. of CTVS, JIPMEREla MaranNo ratings yet
- CDC/NHSN Surveillance Definitions For Specific Types of InfectionsDocument30 pagesCDC/NHSN Surveillance Definitions For Specific Types of InfectionssofiaNo ratings yet
- Drug Study - Ambroxol, AmpicillinDocument3 pagesDrug Study - Ambroxol, AmpicillinPaul John RutaquioNo ratings yet
- Childhood Immunization & Catch Up Immunization-2Document53 pagesChildhood Immunization & Catch Up Immunization-2Haters ExterminatorNo ratings yet
- Pharmacology of Thyroid HormonesDocument56 pagesPharmacology of Thyroid HormonesDr.U.P.Rathnakar.MD.DIH.PGDHMNo ratings yet
- Alzheimer Disease Including Focal Presentations PDFDocument14 pagesAlzheimer Disease Including Focal Presentations PDFpiedrahitasaNo ratings yet
- Summative Test in Health (Drug Education) - 2019Document2 pagesSummative Test in Health (Drug Education) - 2019Melody Joy Amosco100% (2)
- Renasys Ez - Ez Plus User ManualDocument30 pagesRenasys Ez - Ez Plus User ManualRaymundo Olayo EspírituNo ratings yet
- Lesson - 01colour TherapyDocument7 pagesLesson - 01colour TherapyprasadmvkNo ratings yet
- Chronic OsteomyelitisDocument18 pagesChronic OsteomyelitisMar OrdanzaNo ratings yet
- Loa LoaDocument22 pagesLoa LoaphilmonNo ratings yet
- What Is A Migraine?Document7 pagesWhat Is A Migraine?AngelaNo ratings yet
- Dermatology Supplement v2018 PDFDocument39 pagesDermatology Supplement v2018 PDFVenice Jamaila DagcutanNo ratings yet
- Genetic CounselingDocument12 pagesGenetic CounselingChandraNo ratings yet
- Histopathology Requisition FormDocument2 pagesHistopathology Requisition Formr4raheNo ratings yet
- Udem Paru GEADocument36 pagesUdem Paru GEAAndiBoediartoNo ratings yet