Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
5 views2nd Lecture Anesthesia Physiology
2nd Lecture Anesthesia Physiology
Uploaded by
khayam.n.j.rCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You might also like
- Biology AnswerDocument42 pagesBiology AnswerMuhamad Doris Bagindo Sati50% (10)
- Mock Tests 20 20 Class 4 Science SampleDocument13 pagesMock Tests 20 20 Class 4 Science SampleRueban manohar75% (4)
- 1-26 MIDTERM STUFF and DICTIONARY PARTDocument142 pages1-26 MIDTERM STUFF and DICTIONARY PARThuun_59No ratings yet
- Circulation and Blood Igcse BiologyDocument73 pagesCirculation and Blood Igcse BiologyEllie HousenNo ratings yet
- BioA430 Chapter 2 Vs RGDocument65 pagesBioA430 Chapter 2 Vs RGIbrahim MarmalNo ratings yet
- PHS 211 HMDocument23 pagesPHS 211 HMmetasynthronos748No ratings yet
- Chapter 05 4EDocument41 pagesChapter 05 4Elikhovandy10No ratings yet
- 3010 Adrenal and Parathyroid HormonesDocument21 pages3010 Adrenal and Parathyroid HormonesDenesha KaurNo ratings yet
- Circulatory SystemDocument56 pagesCirculatory SystemillyaniNo ratings yet
- 10 General Anatomy of The Cardiovascular SystemDocument140 pages10 General Anatomy of The Cardiovascular SystemSuzana VoiculescuNo ratings yet
- Ch35 CardiovascularDocument11 pagesCh35 CardiovascularJessie Jennings100% (3)
- Transport in AnimalDocument35 pagesTransport in AnimalbenunosNo ratings yet
- CVS Lectures Corrections 22Document211 pagesCVS Lectures Corrections 22Oluwapelumi DimejiNo ratings yet
- Body Coordination 2023Document73 pagesBody Coordination 2023AbbygailNo ratings yet
- Module 1Document37 pagesModule 1Sharanya BasakNo ratings yet
- Lecture 1.Document27 pagesLecture 1.abdelrazeq zarourNo ratings yet
- Blok: Trauma and Emergency "Shock"Document66 pagesBlok: Trauma and Emergency "Shock"Rina_Fatimah_NuriilaNo ratings yet
- 2.pancreas and Suprarenal GlandsDocument39 pages2.pancreas and Suprarenal Glandsmj4957No ratings yet
- Heart Excitation HandoutDocument10 pagesHeart Excitation HandoutGPearce204No ratings yet
- A&p (B&C) Handout 2015Document50 pagesA&p (B&C) Handout 2015Alisa BrownNo ratings yet
- Clinical EnzymologyDocument38 pagesClinical EnzymologyLloyd Jay LinNo ratings yet
- Body System ChecklistDocument6 pagesBody System Checklistapi-422855075No ratings yet
- WK 1& 2 LectureDocument149 pagesWK 1& 2 LectureElma SekikorolevuNo ratings yet
- CH 26 UrinaryDocument63 pagesCH 26 Urinaryaijaz1inNo ratings yet
- Biochemistry of The Heart and Blood Vessels 2021 3 4Document44 pagesBiochemistry of The Heart and Blood Vessels 2021 3 4jakukNo ratings yet
- Basic Concepts of Human Body FunctionsDocument54 pagesBasic Concepts of Human Body Functionsliliansimba24No ratings yet
- Untitled DocumentDocument3 pagesUntitled DocumentidlydumpfvckNo ratings yet
- Cardiac Muscle Physiology & Cardiac GlycosidesDocument18 pagesCardiac Muscle Physiology & Cardiac GlycosidesEbenezer SamuelNo ratings yet
- Blood Pressure.Document49 pagesBlood Pressure.Sally PujaNo ratings yet
- Asam Basa Dan ElektrolitDocument50 pagesAsam Basa Dan ElektrolitDavid Ithu AgkhuNo ratings yet
- Effects of Exercise On CVSDocument17 pagesEffects of Exercise On CVSDarshan KoiralaNo ratings yet
- Chapter 04Document52 pagesChapter 04api-3743202No ratings yet
- CBL HypertensionDocument23 pagesCBL HypertensionWan AswanNo ratings yet
- Shock: Dr. Naser El-Hammuri Head of The Department of Surgery Hashemite UniversityDocument40 pagesShock: Dr. Naser El-Hammuri Head of The Department of Surgery Hashemite UniversityMohammad Husni BanisalmanNo ratings yet
- Pathophysiology of Heart FailureDocument51 pagesPathophysiology of Heart FailureJoshua ObrienNo ratings yet
- Y10 Heart & CirculationDocument11 pagesY10 Heart & CirculationTri MariyantiNo ratings yet
- Role of Hormones in HumansDocument97 pagesRole of Hormones in HumanshafizamajidNo ratings yet
- Endocrine System: Prepared By: Danish AhmedDocument47 pagesEndocrine System: Prepared By: Danish AhmedHira KhanNo ratings yet
- Shock: Dr. Imam Ghozali., Span.,MkeswDocument70 pagesShock: Dr. Imam Ghozali., Span.,MkeswRiyan SaputraNo ratings yet
- CVS - Regulation of Blood Pressure 21-22Document30 pagesCVS - Regulation of Blood Pressure 21-22ahang.aliNo ratings yet
- Shock: Dr. Imam Ghozali., Span.,MkesDocument66 pagesShock: Dr. Imam Ghozali., Span.,MkesreavondNo ratings yet
- Shock FinalDocument90 pagesShock Finalمجاهد إسماعيل حسن حسينNo ratings yet
- Life's Progression Through Cardiac PhysiologyDocument91 pagesLife's Progression Through Cardiac PhysiologyprofcarleyNo ratings yet
- Effects of Exercise On CVS 21-22Document25 pagesEffects of Exercise On CVS 21-22ahang.aliNo ratings yet
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Cardiovascular SystemDocument58 pagesCardiovascular Systemabromley100% (2)
- 03heart FailureDocument37 pages03heart Failureyonem11615No ratings yet
- CRRT Mod 1 Edwards 9may07Document60 pagesCRRT Mod 1 Edwards 9may07Omar Elsayed RamadanNo ratings yet
- The Endocrine System: HormoneDocument22 pagesThe Endocrine System: HormoneRoxy ExistingNo ratings yet
- Heart FailureDocument4 pagesHeart FailureDane WrightNo ratings yet
- The Urinary System: DR P VijayalakshmiDocument79 pagesThe Urinary System: DR P VijayalakshmiVijaya LakshmiNo ratings yet
- Biomedical Set B AnsDocument20 pagesBiomedical Set B AnskarthikbalajimanoharanNo ratings yet
- Peripheral Vascular Diseases KDocument230 pagesPeripheral Vascular Diseases Kjosephabram051590100% (4)
- Clinical Enzymology: (Clinical Biochemistry of Enzymes)Document10 pagesClinical Enzymology: (Clinical Biochemistry of Enzymes)Dawlat SalamaNo ratings yet
- Enzim Penyakit Jantung: Dr. Evi Kurniawaty, M.SCDocument28 pagesEnzim Penyakit Jantung: Dr. Evi Kurniawaty, M.SCRestu PamanggihNo ratings yet
- Fluid and Electrolyte BalanceDocument41 pagesFluid and Electrolyte BalanceFev BanataoNo ratings yet
- The Circulatory System: The Heart, Blood Vessels, Blood TypesDocument51 pagesThe Circulatory System: The Heart, Blood Vessels, Blood Typescut irnandaNo ratings yet
- Vascular System: - Arteries Arterioles - Capil ExchDocument35 pagesVascular System: - Arteries Arterioles - Capil ExchMikaelle GasparNo ratings yet
- Cardiovascular Physiology - 2Document33 pagesCardiovascular Physiology - 2Luiz Jorge MendonçaNo ratings yet
- Pathophysiology of Heart Failure: Prof. J. HanacekDocument48 pagesPathophysiology of Heart Failure: Prof. J. Hanaceksukarni84sgdNo ratings yet
- ECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!From EverandECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!No ratings yet
- IELTS PowerPoint PresentationDocument43 pagesIELTS PowerPoint Presentationkhayam.n.j.rNo ratings yet
- Methods of Anesthesia - The Choice of A Particular AnestheticDocument17 pagesMethods of Anesthesia - The Choice of A Particular Anesthetickhayam.n.j.rNo ratings yet
- Academic Reading Test 2Document11 pagesAcademic Reading Test 2khayam.n.j.rNo ratings yet
- Lets Go 3 First ExamDocument3 pagesLets Go 3 First Examkhayam.n.j.rNo ratings yet
- Layan Training Center: Name F/Name Class CourseDocument4 pagesLayan Training Center: Name F/Name Class Coursekhayam.n.j.rNo ratings yet
- The Red Cell Histogram PDFDocument9 pagesThe Red Cell Histogram PDFpieterinpretoria391No ratings yet
- Nota Ringkas Sains Bab 1 RespirasiDocument6 pagesNota Ringkas Sains Bab 1 RespirasiZuraina ShaharomNo ratings yet
- Brain ExercisesDocument2 pagesBrain Exercisespaulxe100% (1)
- Vet PathologyDocument128 pagesVet PathologyMegarsaNo ratings yet
- 5851 978-1-5386-4658-8/18/$31.00 ©2019 Ieee Icassp 2019Document5 pages5851 978-1-5386-4658-8/18/$31.00 ©2019 Ieee Icassp 2019Swarnadip SahaNo ratings yet
- Insects Leg - Chandra Kanta Dash - SAUDocument4 pagesInsects Leg - Chandra Kanta Dash - SAUChandra Kanta Dash100% (1)
- Intercellular Communication and Signal TransductionDocument20 pagesIntercellular Communication and Signal TransductionBerkaahh ShoppNo ratings yet
- Focus On Diagnosis of Acute Compartment Syndrome PDFDocument8 pagesFocus On Diagnosis of Acute Compartment Syndrome PDFMuthia DewiNo ratings yet
- N5 Biology All 2018Document48 pagesN5 Biology All 2018Sajida CheemaNo ratings yet
- Antepartum HemorrhageDocument35 pagesAntepartum HemorrhagesubashikNo ratings yet
- Pyschology CAT MKUDocument3 pagesPyschology CAT MKUPeter KNo ratings yet
- Neuroimaging Clinics - Imaging of Head TraumaDocument184 pagesNeuroimaging Clinics - Imaging of Head TraumaSimion Iulian100% (1)
- Veterinary Clinical DiagnosisDocument77 pagesVeterinary Clinical Diagnosismmohammed seidNo ratings yet
- Alambra Et Al - Review & Comments Edited 01-22 EditDocument8 pagesAlambra Et Al - Review & Comments Edited 01-22 EditKenneth_Alambr_1485No ratings yet
- High Yield Biochemistry PDFDocument41 pagesHigh Yield Biochemistry PDFKyle Broflovski100% (2)
- Murthy Et Al 2011 Starch Hydrolysis Modeling Application To Fuel Ethanol ProductionDocument13 pagesMurthy Et Al 2011 Starch Hydrolysis Modeling Application To Fuel Ethanol ProductionMatache GabrielaNo ratings yet
- InstrumentsDocument35 pagesInstrumentsvgmanjunathNo ratings yet
- Daftar Pustaka Kalsium Pada Anak Bandung 2012Document4 pagesDaftar Pustaka Kalsium Pada Anak Bandung 2012haneiyahNo ratings yet
- Sheep Hear Dissection Sp11 BIO 160Document2 pagesSheep Hear Dissection Sp11 BIO 160Kelly TrainorNo ratings yet
- Activity 11 - The Leaf (Instruction Sheet)Document9 pagesActivity 11 - The Leaf (Instruction Sheet)Chris P. BeaconNo ratings yet
- Lesson1 PowerPoint10Document15 pagesLesson1 PowerPoint10chrislazNo ratings yet
- Alimento Del CerebroDocument6 pagesAlimento Del Cerebrodanielagonzalezt5No ratings yet
- The Life of A Flowering PlantDocument19 pagesThe Life of A Flowering PlantMedinaNo ratings yet
- Guidelines HPNDocument46 pagesGuidelines HPNSherif AbobakrNo ratings yet
- Lab1ESR 08Document11 pagesLab1ESR 08Muhamad AfidinNo ratings yet
- HK in Pace CRTDocument87 pagesHK in Pace CRTfraushaiNo ratings yet
- A Simple Method For Individual Anaerobic Threshold As Predictor of Max Lactate Steady State, Baldari2000.pd PDFDocument5 pagesA Simple Method For Individual Anaerobic Threshold As Predictor of Max Lactate Steady State, Baldari2000.pd PDFGil SilvaNo ratings yet
2nd Lecture Anesthesia Physiology
2nd Lecture Anesthesia Physiology
Uploaded by
khayam.n.j.r0 ratings0% found this document useful (0 votes)
5 views44 pagesOriginal Title
2nd Lecture Anesthesia Physiology
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
0 ratings0% found this document useful (0 votes)
5 views44 pages2nd Lecture Anesthesia Physiology
2nd Lecture Anesthesia Physiology
Uploaded by
khayam.n.j.rCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
You are on page 1of 44
Neurophysiology (central nervous system)
By:Dr Ahmad Shah shaiq
• Neurophysiology (central nervous system)
• A basic knowledge of the physiology of the
central nervous system is important for the
anesthesia provider who will be taking care of
patients with diseases of the central nervous
system. This knowledge is also important for
doing a safe anesthetic for operations on the
brain and other central nervous system
structures.
• Important concepts and definitions
• Cerebral (brain) metabolism is concerned with the
amount of oxygen and glucose that the brain uses
for its normal function
• The brain uses 20% of the oxygen that the body
takes in
– The brain uses oxygen at about 50 milliliter per minute
– The brain has very limited oxygen reserves and
unconsciousness occurs after 10 seconds of no blood flow
– Irreversible cell injury occurs after 3 to 8 minutes of no
blood flow or oxygen supply
• Regulation of Cerebral Blood Flow is dependent
on Cerebral Perfusion Pressure (CPP)
• Cerebral perfusion pressure is the difference
between the mean arterial pressure (MAP) and
the higher of either central venous pressure
(CVP) or intracranial pressure (ICP)
– CPP = MAP – ICP or CVP
– Cerebral perfusion pressure (CPP) is normally about
100
• In patients with chronic high blood
pressure the normal function of
autoregulation may be shifted to
higher MAPs and the patient may
require higher than normal MAPs to
supply the brain with acceptable
blood flow
• The blood brain barrier
• Blood vessels in the brain are different from
other blood vessels because the cells that make
up the lining of them are so close together that
only very small molecules (substances) can leave
the blood and enter the brain
– Factors that can effect whether a substance will pass
from the blood into the brain include size, electrical
charge, lipid solubility, and the amount of protein
binding
Physiology of the Autonomic Nervous
System
• Physiology of the Autonomic Nervous System
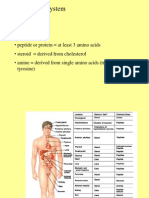
• The autonomic nervous is that part of the nervous
system that sends and receives nerves from many
important body organs (systems). See below
diagram for a general idea of its major functions.
The autonomic nervous is made up of two systems.
These two systems are the sympathetic and the
parasympathetic nervous systems. Normally these
two systems cause changes in the body that are in
opposite direction to the other system.
• The right side of the diagram above shows the nerves
from the sympathetic nervous system leaving the
spinal cord between the first thoracic (T1) and second
lumbar (L2) level of the spinal cord. This is important
because subarachnoid block can block some of these
nerves.
• The left side of the diagram above shows the nerves
from the parasympathetic nervous system leaving the
spinal cord near the brain stem and the sacrum. A
large amount of the information that is sent and
received by the parasympathetic nervous system is
carried in the vagus nerve.
• The sympathetic nervous system causes
the following changes in many body
systems
• cardiac system
– increased heart rate via cardiac fibers from
T1 to T4
• block of these cardiac fibers during subarachnoid
block can cause severe bradycardia (slow heart
rate)
pulmonary system
– relaxation of muscles in walls of small airways causes
bronchodilation
• increases blood glucose level
gastrointestinal system
– slow movement of stomach and intestinal contents through
gastrointestinal system
– decreased production and secretions from stomach,
gallbladder and intestine
• slows digestion
– liver makes and secretes more glucose into the blood stream
• increases blood glucose level
– pancreas produces and secretes less insulin
• urinary system
– the muscle of the bladder relax and
muscle of urethra constricts (tightens)
• this can cause bladder retention of urine
• ocular (eye) system
– pupils dilate (big pupil)
– better far vision
• arterial (circulatory) system
– depending on whether alpha or beta receptors are more
strongly activated, different effects can occur
– arteries to the heart
• alpha receptors cause constriction (narrowing)
• beta receptors cause dilation (widening)
– arteries to skin
• constriction
– arteries to muscle
• alpha receptors cause constriction
• beta receptors cause dilation
– arteries to lung
• constriction
The parasympathetic nervous system
causes the following changes in many
body systems
• cardiac system
– bradycardia (slow heart rate)
• pulmonary system
– contraction of smooth muscles in wall of
airway causes bronchoconstriction
(narrowing) of small airwaysgastrointestinal
system
• faster movement of stomach and intestinal
consents through gastrointestinal system
• increased production and secretion from
stomach, gallbladder, and intestines
• cause faster digestion of meal
– liver stores more glucose
– salivary glands in mouth increase
secretions
• urinary system
– muscle of bladder contract and muscle of
urethra relax
• helps urination
• ocular (eye) system
– small pupils
– better near vision
• arterial (circulatory) system
– the majority of all major arteries dilate (widen
• The following receptors cause responses in
the body when medications are given that
bind to these receptors
• alpha 1
– vasoconstriction
– big pupils
– relaxation of gastrointestinal system
– contraction of urethra
• alpha 2
– depression of the central nervous system
• sedation
– increased strength of each heart beat (contractility)
• beta
• 1
– increased speed of passage of electrical current through
heart
• faster heart rate
• possible risk of abnormal heart rhythm
• beta 2
– vasodilatation
– bronchodilation
– relaxation of gastrointestinal tract
– relaxation of muscles of uterus
– relaxation of muscles of bladder
– breakdown of glucose in the liver
– breakdown of fat for energy
• dopamine
– vasodilatation
• The teaching of how different
medications act on the sympathetic and
parasympathetic nervous systems is to
be taught in separate lectures/chapters
on the specific medications
Cardiac system
• the normal flow of blood from the veins, through
the heart, to the lungs, back to the heart, and
back to the body
• the normal movement of electrical impulses
through the heart that lead to muscle contraction
• normal flow of blood and oxygen to the heart
muscle
• how the cardiovascular system works together to
provide adequate blood pressure for the body
• Another important idea is that the heart
muscle needs both flow and oxygen
• anything that decreases blood flow or oxygen
is bad for the heart
• anything that increases blood flow or oxygen
is good for the heart
• To increase the supply of blood and oxygen to
the heart do the following
• make sure that the blood contains the
maximum of amount of oxygen possible
• remember that blood flow to the
heart muscle occurs during diastole
– slow to normal heart rates allow the
period of diastole to be the longest
– avoid tachycardia in patients with
ischemic heart disease
• heart rates higher that 100 are not tolerated
well in patient with ischemic heart disease
– this causes depolarization and contraction of the
ventricles
• this seen as the qrs complex on the electrocardiogram
– after contraction of the heart muscle, the heart
muscle will repolarize before the next heart beat
• this is seen as the t wave on the electrocardiogram
• a more detailed lecture on electrocardiogram
interpretation and abnormalities will be
discussed in a separate lecture/chapter
• Hepatic (liver) Physiology and
Anesthesia
• The liver is the largest organ in the
body and has many important
functions. Key concepts that are
important to the anesthesia provider
will be discussed.
• Liver blood flow
• The liver has a very significant blood flow
and receives 25 to 30% of the total cardiac
output
• About 1500 milliliter per minute
• About 50% of the hepatic oxygen supply
comes from the hepatic artery
• About 75% of total blood flow comes from
the portal vein
• The liver serves as a reservoir for blood for
the body
• The liver normally contains 450 milliliters of
blood
• In patients with congestive heart failure
this amount of blood in the liver can
increase to 1000 milliliters
• The liver has many functions in normal body
metabolism
• Carbohydrate metabolism
– The liver has a critical role in glucose
metabolism
– The normal liver stores enough glycogen (storage
form of glucose) to keep blood glucose levels
normal for 24 hours
• The liver has the potential to make glucose from
other sources
• It is important to remember that red blood cells,
cells of the kidney, and brain can ONLY use glucose
for energy source
• Drug/medication metabolism
– Almost all medications and many substance
that need to be eliminated from the body
are broken down or metabolized by the
body prior to elimination
– The liver also has a critical role in hormone,
vitamin, and mineral metabolism
– Bile formation and elimination
– Bile formation and elimination is another critical
function of the liver and gallbladder
– Bile is needed for the normal absorption of fats
from the diet
• Problems with bile formation can cause problems with
the absorption of fat soluble vitamins (A, D, E, and K)
• Vitamin K deficiencies can occur in a few days and
normally causes problems with blood clotting
• Blood flow to the liver is normally decreased by regional
and general anesthesia and the surgical procedure
• Effects of Anesthesia on Liver Function
– All volatile anesthetics decrease portal blood flow to the
liver
• Halothane causes the greatest reduction in hepatic blood flow
– Spinal and epidural anesthetics can decrease blood flow to
the liver even if intravascular volume is maintained at an
appropriate level
– Controlled positive pressure ventilation with high airway
pressures can decrease blood flow to the liver
– Surgical procedures near the liver can reduce blood flow
to the liver by up to 60%
• All opioids have been associated with
spasm of the sphincter of oddi and can
cause obstruction of the biliary tree
– Different opioids cause a different
amount of spasm
• Fentanyl > morphine>pentazocine
• Naloxone can release the spasm of the
sphincter of oddi
Standards for Basic Anesthetic
Monitors
• 1. Qualified anesthesia personnel
continuously present in the room
• 2. Pulse oximeter (oxygenation)
• 3. Inspired oxygen analyzer with low
oxygen concentration alarm
• 4. Capnography (ventilation).
• 5. ETCO2 documented post intubation
• 6. Disconnect alarm for ventilator
• 7. ECG (leads II and V5)
• 8. Heart rate and Blood pressure
every 5 minutes (circulation)
• 9. Temperature
Thanks from your
attention
You might also like
- Biology AnswerDocument42 pagesBiology AnswerMuhamad Doris Bagindo Sati50% (10)
- Mock Tests 20 20 Class 4 Science SampleDocument13 pagesMock Tests 20 20 Class 4 Science SampleRueban manohar75% (4)
- 1-26 MIDTERM STUFF and DICTIONARY PARTDocument142 pages1-26 MIDTERM STUFF and DICTIONARY PARThuun_59No ratings yet
- Circulation and Blood Igcse BiologyDocument73 pagesCirculation and Blood Igcse BiologyEllie HousenNo ratings yet
- BioA430 Chapter 2 Vs RGDocument65 pagesBioA430 Chapter 2 Vs RGIbrahim MarmalNo ratings yet
- PHS 211 HMDocument23 pagesPHS 211 HMmetasynthronos748No ratings yet
- Chapter 05 4EDocument41 pagesChapter 05 4Elikhovandy10No ratings yet
- 3010 Adrenal and Parathyroid HormonesDocument21 pages3010 Adrenal and Parathyroid HormonesDenesha KaurNo ratings yet
- Circulatory SystemDocument56 pagesCirculatory SystemillyaniNo ratings yet
- 10 General Anatomy of The Cardiovascular SystemDocument140 pages10 General Anatomy of The Cardiovascular SystemSuzana VoiculescuNo ratings yet
- Ch35 CardiovascularDocument11 pagesCh35 CardiovascularJessie Jennings100% (3)
- Transport in AnimalDocument35 pagesTransport in AnimalbenunosNo ratings yet
- CVS Lectures Corrections 22Document211 pagesCVS Lectures Corrections 22Oluwapelumi DimejiNo ratings yet
- Body Coordination 2023Document73 pagesBody Coordination 2023AbbygailNo ratings yet
- Module 1Document37 pagesModule 1Sharanya BasakNo ratings yet
- Lecture 1.Document27 pagesLecture 1.abdelrazeq zarourNo ratings yet
- Blok: Trauma and Emergency "Shock"Document66 pagesBlok: Trauma and Emergency "Shock"Rina_Fatimah_NuriilaNo ratings yet
- 2.pancreas and Suprarenal GlandsDocument39 pages2.pancreas and Suprarenal Glandsmj4957No ratings yet
- Heart Excitation HandoutDocument10 pagesHeart Excitation HandoutGPearce204No ratings yet
- A&p (B&C) Handout 2015Document50 pagesA&p (B&C) Handout 2015Alisa BrownNo ratings yet
- Clinical EnzymologyDocument38 pagesClinical EnzymologyLloyd Jay LinNo ratings yet
- Body System ChecklistDocument6 pagesBody System Checklistapi-422855075No ratings yet
- WK 1& 2 LectureDocument149 pagesWK 1& 2 LectureElma SekikorolevuNo ratings yet
- CH 26 UrinaryDocument63 pagesCH 26 Urinaryaijaz1inNo ratings yet
- Biochemistry of The Heart and Blood Vessels 2021 3 4Document44 pagesBiochemistry of The Heart and Blood Vessels 2021 3 4jakukNo ratings yet
- Basic Concepts of Human Body FunctionsDocument54 pagesBasic Concepts of Human Body Functionsliliansimba24No ratings yet
- Untitled DocumentDocument3 pagesUntitled DocumentidlydumpfvckNo ratings yet
- Cardiac Muscle Physiology & Cardiac GlycosidesDocument18 pagesCardiac Muscle Physiology & Cardiac GlycosidesEbenezer SamuelNo ratings yet
- Blood Pressure.Document49 pagesBlood Pressure.Sally PujaNo ratings yet
- Asam Basa Dan ElektrolitDocument50 pagesAsam Basa Dan ElektrolitDavid Ithu AgkhuNo ratings yet
- Effects of Exercise On CVSDocument17 pagesEffects of Exercise On CVSDarshan KoiralaNo ratings yet
- Chapter 04Document52 pagesChapter 04api-3743202No ratings yet
- CBL HypertensionDocument23 pagesCBL HypertensionWan AswanNo ratings yet
- Shock: Dr. Naser El-Hammuri Head of The Department of Surgery Hashemite UniversityDocument40 pagesShock: Dr. Naser El-Hammuri Head of The Department of Surgery Hashemite UniversityMohammad Husni BanisalmanNo ratings yet
- Pathophysiology of Heart FailureDocument51 pagesPathophysiology of Heart FailureJoshua ObrienNo ratings yet
- Y10 Heart & CirculationDocument11 pagesY10 Heart & CirculationTri MariyantiNo ratings yet
- Role of Hormones in HumansDocument97 pagesRole of Hormones in HumanshafizamajidNo ratings yet
- Endocrine System: Prepared By: Danish AhmedDocument47 pagesEndocrine System: Prepared By: Danish AhmedHira KhanNo ratings yet
- Shock: Dr. Imam Ghozali., Span.,MkeswDocument70 pagesShock: Dr. Imam Ghozali., Span.,MkeswRiyan SaputraNo ratings yet
- CVS - Regulation of Blood Pressure 21-22Document30 pagesCVS - Regulation of Blood Pressure 21-22ahang.aliNo ratings yet
- Shock: Dr. Imam Ghozali., Span.,MkesDocument66 pagesShock: Dr. Imam Ghozali., Span.,MkesreavondNo ratings yet
- Shock FinalDocument90 pagesShock Finalمجاهد إسماعيل حسن حسينNo ratings yet
- Life's Progression Through Cardiac PhysiologyDocument91 pagesLife's Progression Through Cardiac PhysiologyprofcarleyNo ratings yet
- Effects of Exercise On CVS 21-22Document25 pagesEffects of Exercise On CVS 21-22ahang.aliNo ratings yet
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Cardiovascular SystemDocument58 pagesCardiovascular Systemabromley100% (2)
- 03heart FailureDocument37 pages03heart Failureyonem11615No ratings yet
- CRRT Mod 1 Edwards 9may07Document60 pagesCRRT Mod 1 Edwards 9may07Omar Elsayed RamadanNo ratings yet
- The Endocrine System: HormoneDocument22 pagesThe Endocrine System: HormoneRoxy ExistingNo ratings yet
- Heart FailureDocument4 pagesHeart FailureDane WrightNo ratings yet
- The Urinary System: DR P VijayalakshmiDocument79 pagesThe Urinary System: DR P VijayalakshmiVijaya LakshmiNo ratings yet
- Biomedical Set B AnsDocument20 pagesBiomedical Set B AnskarthikbalajimanoharanNo ratings yet
- Peripheral Vascular Diseases KDocument230 pagesPeripheral Vascular Diseases Kjosephabram051590100% (4)
- Clinical Enzymology: (Clinical Biochemistry of Enzymes)Document10 pagesClinical Enzymology: (Clinical Biochemistry of Enzymes)Dawlat SalamaNo ratings yet
- Enzim Penyakit Jantung: Dr. Evi Kurniawaty, M.SCDocument28 pagesEnzim Penyakit Jantung: Dr. Evi Kurniawaty, M.SCRestu PamanggihNo ratings yet
- Fluid and Electrolyte BalanceDocument41 pagesFluid and Electrolyte BalanceFev BanataoNo ratings yet
- The Circulatory System: The Heart, Blood Vessels, Blood TypesDocument51 pagesThe Circulatory System: The Heart, Blood Vessels, Blood Typescut irnandaNo ratings yet
- Vascular System: - Arteries Arterioles - Capil ExchDocument35 pagesVascular System: - Arteries Arterioles - Capil ExchMikaelle GasparNo ratings yet
- Cardiovascular Physiology - 2Document33 pagesCardiovascular Physiology - 2Luiz Jorge MendonçaNo ratings yet
- Pathophysiology of Heart Failure: Prof. J. HanacekDocument48 pagesPathophysiology of Heart Failure: Prof. J. Hanaceksukarni84sgdNo ratings yet
- ECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!From EverandECG & EKG Interpretation: How to interpret ECG & EKG, including rhythms, arrhythmias, and more!No ratings yet
- IELTS PowerPoint PresentationDocument43 pagesIELTS PowerPoint Presentationkhayam.n.j.rNo ratings yet
- Methods of Anesthesia - The Choice of A Particular AnestheticDocument17 pagesMethods of Anesthesia - The Choice of A Particular Anesthetickhayam.n.j.rNo ratings yet
- Academic Reading Test 2Document11 pagesAcademic Reading Test 2khayam.n.j.rNo ratings yet
- Lets Go 3 First ExamDocument3 pagesLets Go 3 First Examkhayam.n.j.rNo ratings yet
- Layan Training Center: Name F/Name Class CourseDocument4 pagesLayan Training Center: Name F/Name Class Coursekhayam.n.j.rNo ratings yet
- The Red Cell Histogram PDFDocument9 pagesThe Red Cell Histogram PDFpieterinpretoria391No ratings yet
- Nota Ringkas Sains Bab 1 RespirasiDocument6 pagesNota Ringkas Sains Bab 1 RespirasiZuraina ShaharomNo ratings yet
- Brain ExercisesDocument2 pagesBrain Exercisespaulxe100% (1)
- Vet PathologyDocument128 pagesVet PathologyMegarsaNo ratings yet
- 5851 978-1-5386-4658-8/18/$31.00 ©2019 Ieee Icassp 2019Document5 pages5851 978-1-5386-4658-8/18/$31.00 ©2019 Ieee Icassp 2019Swarnadip SahaNo ratings yet
- Insects Leg - Chandra Kanta Dash - SAUDocument4 pagesInsects Leg - Chandra Kanta Dash - SAUChandra Kanta Dash100% (1)
- Intercellular Communication and Signal TransductionDocument20 pagesIntercellular Communication and Signal TransductionBerkaahh ShoppNo ratings yet
- Focus On Diagnosis of Acute Compartment Syndrome PDFDocument8 pagesFocus On Diagnosis of Acute Compartment Syndrome PDFMuthia DewiNo ratings yet
- N5 Biology All 2018Document48 pagesN5 Biology All 2018Sajida CheemaNo ratings yet
- Antepartum HemorrhageDocument35 pagesAntepartum HemorrhagesubashikNo ratings yet
- Pyschology CAT MKUDocument3 pagesPyschology CAT MKUPeter KNo ratings yet
- Neuroimaging Clinics - Imaging of Head TraumaDocument184 pagesNeuroimaging Clinics - Imaging of Head TraumaSimion Iulian100% (1)
- Veterinary Clinical DiagnosisDocument77 pagesVeterinary Clinical Diagnosismmohammed seidNo ratings yet
- Alambra Et Al - Review & Comments Edited 01-22 EditDocument8 pagesAlambra Et Al - Review & Comments Edited 01-22 EditKenneth_Alambr_1485No ratings yet
- High Yield Biochemistry PDFDocument41 pagesHigh Yield Biochemistry PDFKyle Broflovski100% (2)
- Murthy Et Al 2011 Starch Hydrolysis Modeling Application To Fuel Ethanol ProductionDocument13 pagesMurthy Et Al 2011 Starch Hydrolysis Modeling Application To Fuel Ethanol ProductionMatache GabrielaNo ratings yet
- InstrumentsDocument35 pagesInstrumentsvgmanjunathNo ratings yet
- Daftar Pustaka Kalsium Pada Anak Bandung 2012Document4 pagesDaftar Pustaka Kalsium Pada Anak Bandung 2012haneiyahNo ratings yet
- Sheep Hear Dissection Sp11 BIO 160Document2 pagesSheep Hear Dissection Sp11 BIO 160Kelly TrainorNo ratings yet
- Activity 11 - The Leaf (Instruction Sheet)Document9 pagesActivity 11 - The Leaf (Instruction Sheet)Chris P. BeaconNo ratings yet
- Lesson1 PowerPoint10Document15 pagesLesson1 PowerPoint10chrislazNo ratings yet
- Alimento Del CerebroDocument6 pagesAlimento Del Cerebrodanielagonzalezt5No ratings yet
- The Life of A Flowering PlantDocument19 pagesThe Life of A Flowering PlantMedinaNo ratings yet
- Guidelines HPNDocument46 pagesGuidelines HPNSherif AbobakrNo ratings yet
- Lab1ESR 08Document11 pagesLab1ESR 08Muhamad AfidinNo ratings yet
- HK in Pace CRTDocument87 pagesHK in Pace CRTfraushaiNo ratings yet
- A Simple Method For Individual Anaerobic Threshold As Predictor of Max Lactate Steady State, Baldari2000.pd PDFDocument5 pagesA Simple Method For Individual Anaerobic Threshold As Predictor of Max Lactate Steady State, Baldari2000.pd PDFGil SilvaNo ratings yet