Professional Documents
Culture Documents
Dislocation
Dislocation
Uploaded by
Akshata Bansode0 ratings0% found this document useful (0 votes)
5 views12 pagesCopyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
5 views12 pagesDislocation
Dislocation
Uploaded by
Akshata BansodeCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 12
TRAUMATIC JOINT DISLOCATION
• Ms.Akshata vijay Bansode
• Clinical instructor
• K.B.N.C
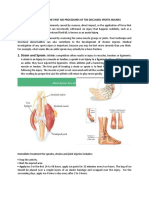
A dislocation is an injury to a joint. It occurs when the surfaces of the
bones forming the joint are dislocated from its anatomic contact. It is
most common in shoulders and fingers. Other sites include elbows,
knees and hips. It is a medical emergency because of associated
disruption of surrounding blood and nerve supplies
Etiology
• 1. Dislocation may be congenital
• 2. Spontaneous or pathologic dislocation might be associated with
some disease.
• 3. Traumatic, i.e. resulting from injury in which joint is disrupted by
force.
Dislocations can occur in contact sports, such as football and hockey,
and in sports in which falls are common such as downhill skiing,
gymnastics and volleyball.
Basketball players and football players also commonly dislocate joints in
their fingers and hands by accidentally striking the ball, the ground or
another player.
A hard blow to a joint during a motor vehicle accident and landing on
an outstretched arm during a fall are other common causes
Risk Factors
1. Susceptibility to falls: Falling increases the chance of a dislocated
joint, if a person use his/her arms to brace for impact or if a person
land forcefully on his/ her body part, such as hip or shoulder
2. Heredity: Some people are born with ligaments that are looser and
more prone to injury than those of other people.
3. Sports participation: Many dislocations occur during high-impact or
contact sports, such as gymnastics, wrestling, basketball and football.
4. Motor vehicle accidents: These are the most common cause of hip
dislocations, especially for people not wearing a seat belt.
Clinical Manifestations
1. Intense pain.
2. Deformity: Visibly deformed or out of place.
3. Change in the length of the extremity.
4. Loss of normal movement.
Diagnostic Evaluation
1. Patient history and physical examination.
2. X-ray confirms dislocation without associated fracture.
Management
1. Immobilization:
a. Immobilize the affected part.
b. Bring displaced parts into normal position as soon as possible.
c. Stabilize reduction until joint structures are healed to prevent
permanently unstable joint or aseptic necrosis of bone.
d. Bandages, splint, plaster casts or traction is maintained.
2. Medication: Analgesics, muscle relaxants and anesthesia are used
during closed reduction.
3. Neurovascular status: Neurovascular status is monitored
4. Exercises: Active and passive exercises can be started gradually. Joint
should be supported during exercise.
Nursing Management
1. Assess for muscle weakness and severity of the weakness
2. Provide assistive devices, e.g. braces, splints, wheel chair to
increase mobility.
3. Range of motion exercise and other physical therapy prevent
contractures and improve muscle strength.
4. 4. Encourage the patient to do activity as much as possible as it
increases independence and helps to maintain muscle function.
5. Respiratory rate and effort should be monitored every 4 hourly.
6. Measures to prevent skin breakdown must be taken.
7. Assess neurovascular status of the extremity before and after
reduction of dislocation.
8. By teaching, ensure proper use of immobilization device after
reduction.
9. Review instructions for activity restrictions and need for
physiotherapy and follow-up.
10. Promote healing during immobilization and prevent further injury.
11. Administer prescribed medicine.
Complications
1. Tearing of the muscles, ligaments and tendons.
2. Nerve or blood vessel damage in or around joint.
3. Susceptibility to reinjury or repeated dislocations
You might also like
- 2 Nursing Foundation II Including Health Assessment Module-Converted - 020222Document17 pages2 Nursing Foundation II Including Health Assessment Module-Converted - 020222Akshata BansodeNo ratings yet
- Safety Practices in Sports and ExerciseDocument19 pagesSafety Practices in Sports and ExerciseRiza Indelible Sibullas80% (5)
- Bacls PDFDocument23 pagesBacls PDFAngelo Domingo0% (1)
- Pfeiffer 5 IM Chapter15Document16 pagesPfeiffer 5 IM Chapter15cjbthegeniusNo ratings yet
- Peh SADocument8 pagesPeh SAlauradeunixNo ratings yet
- 5 Musculoskeletal TraumaDocument102 pages5 Musculoskeletal TraumaMaria Lynne Parambita100% (1)
- Sports Medicine Lecture 1Document23 pagesSports Medicine Lecture 1Manahal SohailNo ratings yet
- Sports InjuriesDocument2 pagesSports InjuriesGuwayNo ratings yet
- Hip ArthroplastyDocument20 pagesHip ArthroplastySandra KitukuNo ratings yet
- QUICK REVISION UNIT 7s 2022-23-1-4Document4 pagesQUICK REVISION UNIT 7s 2022-23-1-4Mr.RandomNo ratings yet
- Fracture Nursing CareDocument6 pagesFracture Nursing CareRizqi LutfiNo ratings yet
- SLM PE 4th QuarterDocument12 pagesSLM PE 4th QuarterRichmond LeeNo ratings yet
- Safety in SportsDocument38 pagesSafety in Sportsjashvaghani10No ratings yet
- Common Injuries and Ilnness 2Document2 pagesCommon Injuries and Ilnness 2SLIDENo ratings yet
- Common Injuries of The Musculoskeletal SystemDocument4 pagesCommon Injuries of The Musculoskeletal SystemJoniele Angelo AninNo ratings yet
- Nursing Care Plan With A FractureDocument11 pagesNursing Care Plan With A FractureHasanah EkaNo ratings yet
- MusculoskelealDocument32 pagesMusculoskelealEbuka AniNo ratings yet
- Ms. Elizabeth D. Cruz E.N., M.A.N.: 9.1 PathophysiologyDocument20 pagesMs. Elizabeth D. Cruz E.N., M.A.N.: 9.1 PathophysiologyAlfadz AsakilNo ratings yet
- Fractures and Low Back Pain: Dr. Lubna DwerijDocument49 pagesFractures and Low Back Pain: Dr. Lubna DwerijNoor MajaliNo ratings yet
- HOPE REVIEWER Last ExamDocument8 pagesHOPE REVIEWER Last Examsunshayneee16No ratings yet
- G11 - Pe 2 - Module 1Document7 pagesG11 - Pe 2 - Module 1John Lois VanNo ratings yet
- Chronic Sports InjuriesDocument22 pagesChronic Sports InjuriesBastosTemitayoStephen78% (9)
- DISLOCATION (Case LC 2)Document7 pagesDISLOCATION (Case LC 2)Fadlan M NasirNo ratings yet
- Pe11 Q2 ReviewerDocument3 pagesPe11 Q2 ReviewerashanticherishNo ratings yet
- Sports InjuriesDocument11 pagesSports Injuriesselinnadiana378No ratings yet
- The Concept of Sports InjuryDocument26 pagesThe Concept of Sports InjuryCharmaine JanorasNo ratings yet
- SHS Lesson 10 Safety Practices in Sports and ExerciseDocument10 pagesSHS Lesson 10 Safety Practices in Sports and ExerciseKylie CadenasNo ratings yet
- Orthopedic NursingDocument19 pagesOrthopedic NursingDa BondadNo ratings yet
- Humerus FractureDocument9 pagesHumerus FracturehelmiNo ratings yet
- FRACTUREDocument16 pagesFRACTUREPriyaNo ratings yet
- Guide English4Document78 pagesGuide English4Paola ChanNo ratings yet
- Skeletal DisorderDocument7 pagesSkeletal Disorderhxqf25mbvvNo ratings yet
- Fractures: Mary Grace B. Gutierrez Resti Mariano Ma. Cindy O. BautistaDocument50 pagesFractures: Mary Grace B. Gutierrez Resti Mariano Ma. Cindy O. BautistaJustin Ahorro-DionisioNo ratings yet
- Elm Grade 11 (Peh)Document28 pagesElm Grade 11 (Peh)Kimberly GonzalesNo ratings yet
- Fractures: Pathophysiology and EtiologyDocument5 pagesFractures: Pathophysiology and EtiologyHafid JuniorNo ratings yet
- Handouts Hope 2Document4 pagesHandouts Hope 2Elmera AmoraNo ratings yet
- Aglugob - Hip Facture 2.0Document18 pagesAglugob - Hip Facture 2.0Miden AlbanoNo ratings yet
- Musculoskeletal TraumaDocument103 pagesMusculoskeletal TraumaJona Kristin EnclunaNo ratings yet
- Self Learning Module P.E. 11 Tyson RamosDocument9 pagesSelf Learning Module P.E. 11 Tyson RamosmailaNo ratings yet
- Russian Language ExerciseDocument11 pagesRussian Language ExerciseCopyright Free VideoNo ratings yet
- 1 What Are Sports InjuriesDocument28 pages1 What Are Sports InjuriesShwetambari PhanseNo ratings yet
- Fracture Case AbstractDocument27 pagesFracture Case AbstractMaribel Briones JuanNo ratings yet
- FractureDocument7 pagesFractureAbigail MangaoangNo ratings yet
- Physiology & Injries in SportsDocument17 pagesPhysiology & Injries in Sportsashvirchatha3No ratings yet
- Types of FracturesDocument10 pagesTypes of Fracturesazeencancer2003No ratings yet
- College of Nursing Adult Nursing Academic Year Lec. Waleed IbrahimDocument6 pagesCollege of Nursing Adult Nursing Academic Year Lec. Waleed Ibrahimمحمد سعد طه احمدNo ratings yet
- Capstone SheetlebDocument58 pagesCapstone Sheetlebapi-675745408No ratings yet
- Sprain: P P P PDocument4 pagesSprain: P P P PJc RocuyanNo ratings yet
- Physical Education Class 12 Study Material Chapter 9Document14 pagesPhysical Education Class 12 Study Material Chapter 9anvi0% (1)
- 2 Safety Practices and Sports Injury ManagementDocument34 pages2 Safety Practices and Sports Injury ManagementGajete, Dnvr Cliedzray L.No ratings yet
- First Aid On TaekwondoDocument5 pagesFirst Aid On TaekwondoJoshua De Leon TuasonNo ratings yet
- Alcantara - Lesson Plan in Physical Education 10Document6 pagesAlcantara - Lesson Plan in Physical Education 10Pau Alcantara IINo ratings yet
- SPRAINS: Overstretching or Tearing The Ligaments Results in A Sprain. Ligaments Are The Bands ofDocument7 pagesSPRAINS: Overstretching or Tearing The Ligaments Results in A Sprain. Ligaments Are The Bands ofPriyanshu KanojiaNo ratings yet
- Common Sports InjuriesDocument35 pagesCommon Sports InjuriesRizalyn TorrevillasNo ratings yet
- Difference Between Sprain and StrainDocument4 pagesDifference Between Sprain and StrainTayyab AliNo ratings yet
- 4 5800869459467963727 PDFDocument38 pages4 5800869459467963727 PDFاحمدNo ratings yet
- Fracture Nursing Care Management: Study GuideDocument5 pagesFracture Nursing Care Management: Study Guidezahwa ayundaNo ratings yet
- Maja Musculo Sceletal-NovaDocument18 pagesMaja Musculo Sceletal-NovaLuka KoloskiNo ratings yet
- Orthopedic SurgeryDocument14 pagesOrthopedic SurgerySajjad LaghariNo ratings yet
- Pe Lesson 5Document35 pagesPe Lesson 5Arselia RubanteNo ratings yet
- Elbow Injury Guidelines for Grappling AthletesFrom EverandElbow Injury Guidelines for Grappling AthletesNo ratings yet
- Respiratorysystem 151130013303 Lva1 App6891Document17 pagesRespiratorysystem 151130013303 Lva1 App6891Akshata BansodeNo ratings yet
- Waste Disposal UnitDocument9 pagesWaste Disposal UnitAkshata BansodeNo ratings yet
- Disaster NursingDocument69 pagesDisaster NursingAkshata BansodeNo ratings yet
- Aa Handing and Taking Over ReportDocument2 pagesAa Handing and Taking Over ReportAkshata BansodeNo ratings yet
- Suctioning ProcedureDocument42 pagesSuctioning ProcedureAkshata Bansode100% (4)
- 1 Applied Nutrition and Dietetics - 020222Document6 pages1 Applied Nutrition and Dietetics - 020222Akshata Bansode50% (2)
- 3 Helth Nursing Informatics Technology - 020222Document5 pages3 Helth Nursing Informatics Technology - 020222Akshata Bansode50% (2)
- Alshata Chapter IIDocument6 pagesAlshata Chapter IIAkshata BansodeNo ratings yet
- SOP Hostel and Mess Commitee FinalDocument10 pagesSOP Hostel and Mess Commitee FinalAkshata BansodeNo ratings yet
- Editorial Commitee NewDocument8 pagesEditorial Commitee NewAkshata BansodeNo ratings yet
- Aa Developing Staffing PatternsDocument14 pagesAa Developing Staffing PatternsAkshata BansodeNo ratings yet
- Script AnchoringDocument5 pagesScript AnchoringAkshata BansodeNo ratings yet
- Pilot Study ReportDocument3 pagesPilot Study ReportAkshata BansodeNo ratings yet
- Fiscal PlaningDocument20 pagesFiscal PlaningAkshata BansodeNo ratings yet
- AA Vision and MissionDocument8 pagesAA Vision and MissionAkshata BansodeNo ratings yet
- Nurse NotesDocument6 pagesNurse NotesAkshata BansodeNo ratings yet
- Care PlanDocument2 pagesCare PlanSiri DevarapalliNo ratings yet
- AA Incident and Night ReportDocument2 pagesAA Incident and Night ReportAkshata BansodeNo ratings yet
- Aa Anecdotal RecordDocument6 pagesAa Anecdotal RecordAkshata BansodeNo ratings yet
- Patent CareDocument10 pagesPatent CareAkshata BansodeNo ratings yet
- Aa Equipments and SuppliesDocument10 pagesAa Equipments and SuppliesAkshata BansodeNo ratings yet
- Community Survey ReportDocument12 pagesCommunity Survey ReportAkshata BansodeNo ratings yet
- AA Enquiary ReportDocument4 pagesAA Enquiary ReportAkshata BansodeNo ratings yet
- AA Duty RoasterDocument6 pagesAA Duty RoasterAkshata Bansode100% (2)
- Kamalnayan Bajaj Nursingcollege, Aurangabad .: Visit Report On Anganwadi at Turkabad TQ Gangapur, Aurangabad DistrictDocument14 pagesKamalnayan Bajaj Nursingcollege, Aurangabad .: Visit Report On Anganwadi at Turkabad TQ Gangapur, Aurangabad DistrictAkshata Bansode78% (9)
- On Ecosystem 12Document10 pagesOn Ecosystem 12Akshata BansodeNo ratings yet
- Review of LiteratureDocument18 pagesReview of LiteratureAkshata BansodeNo ratings yet
- Nursing Research ROLDocument14 pagesNursing Research ROLAkshata BansodeNo ratings yet
- CSF Dynamics in Dandy-Walker SyndromeDocument5 pagesCSF Dynamics in Dandy-Walker SyndromeSergio SaraivaNo ratings yet
- Dr. Trifena - PRESENTASI ESPRO-Application of Ozone Therapy For Holistic Wellness and AntiagingDocument34 pagesDr. Trifena - PRESENTASI ESPRO-Application of Ozone Therapy For Holistic Wellness and AntiagingAdi Sutriwanto PasaribuNo ratings yet
- Paranoid SchizophreniaDocument21 pagesParanoid SchizophreniaRizwan ZafarNo ratings yet
- ANNEX F Employees History and Physical Exam Form 1 - 240205 - 092840Document6 pagesANNEX F Employees History and Physical Exam Form 1 - 240205 - 092840Marion Pierre MateoNo ratings yet
- Maxillofacial - Infection - Dari KikiDrDocument20 pagesMaxillofacial - Infection - Dari KikiDrmashitadyahNo ratings yet
- Cross-Sectional Imaging of Intrahepatic Cholangiocarcinoma: Development, Growth, Spread, and PrognosisDocument12 pagesCross-Sectional Imaging of Intrahepatic Cholangiocarcinoma: Development, Growth, Spread, and PrognosisNikos SerifisNo ratings yet
- Ehy 339Document98 pagesEhy 339Xarisis IoannisNo ratings yet
- Diabetic NephropathyDocument10 pagesDiabetic NephropathySindi Nabila PutriNo ratings yet
- Abdominal CT and TransVag UTZDocument6 pagesAbdominal CT and TransVag UTZWeng Villaverde PampoNo ratings yet
- Kamaljeet Singh - , MediacalDocument3 pagesKamaljeet Singh - , Mediacalafsarkhan85No ratings yet
- Phyllodes TumorDocument6 pagesPhyllodes TumorLuis GuzmánNo ratings yet
- NCP DengueDocument2 pagesNCP DengueJiraGonzalesNo ratings yet
- Misread Chest X Ray Role PlayDocument2 pagesMisread Chest X Ray Role PlayDan Dan ManaoisNo ratings yet
- Coagulopathy of Liver DiseaseDocument5 pagesCoagulopathy of Liver DiseaseAndrea Peláez ChicaNo ratings yet
- CSF ParkinsonDocument4 pagesCSF ParkinsonYunita Christiani BiyangNo ratings yet
- PyelonephritisDocument8 pagesPyelonephritisjellyjohn100% (2)
- Selamawit Seifu 34Document56 pagesSelamawit Seifu 34Alemayehu KebedeNo ratings yet
- Review of Cerebral Malaria Cases in RAHI SchemeDocument8 pagesReview of Cerebral Malaria Cases in RAHI SchemeNanditha ChowhanNo ratings yet
- ParQ Plus Jan 2022 FillableDocument5 pagesParQ Plus Jan 2022 FillableRaechelle DizonNo ratings yet
- SMLE 2018 احدث اسئلة امتحان لأختبار الهيئه السعوديDocument441 pagesSMLE 2018 احدث اسئلة امتحان لأختبار الهيئه السعوديOman Edu100% (6)
- Parkinsons - Disease Curs NR 5Document37 pagesParkinsons - Disease Curs NR 5Iliescu DenisaNo ratings yet
- Beneficial Life Insurance FormDocument1 pageBeneficial Life Insurance FormRanieza CastilloNo ratings yet
- Eating Disorders: Manos, Bencio, Fernandes, ParaisoDocument66 pagesEating Disorders: Manos, Bencio, Fernandes, ParaisoShannen FernandezNo ratings yet
- PROMIS Gastrointestinal Symptoms Scoring ManualDocument32 pagesPROMIS Gastrointestinal Symptoms Scoring ManualAqsha ViazeldaNo ratings yet
- Diagnosis-Pedrosa, Joan ADocument27 pagesDiagnosis-Pedrosa, Joan AJoan Alde PedrosaNo ratings yet
- Circulationaha 122 063399Document12 pagesCirculationaha 122 063399Noel FrancoNo ratings yet
- General Examination For CVSDocument29 pagesGeneral Examination For CVSstudymedic100% (1)
- Blood Groups Assignment AaaDocument3 pagesBlood Groups Assignment AaaLoro JDNo ratings yet