Professional Documents
Culture Documents
Presentation 2
Presentation 2
Uploaded by
amosa2270 ratings0% found this document useful (0 votes)
3 views21 pagesCopyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
3 views21 pagesPresentation 2
Presentation 2
Uploaded by
amosa227Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 21
• Thyroid disease is common, affecting approximately
5% to 15% of the general population.
• Females are three to four times more likely than
males to develop any type of thyroid disease.
• The typical thyroid disorders are
Hypothyroidism
Hyperthyroidism
Nodular disease
Thyroid cancer
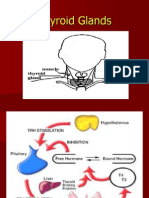
• Triiodothyronine (T3) and thyroxine (T4) are the two
biologically active thyroid hormones produced by the
thyroid gland in response to hormones released by
the pituitary and hypothalamus.
• Thyroid hormones affect the function of virtually
every organ system
Hypothyroidism
• Hypothyroidism is a clinical syndrome that
results from a deficiency of thyroid hormone.
• The prevalence of hypothyroidism is 1.4% to
2% in females and 0.1% to 0.2% in males.
• The incidence increases in persons older than
60 years to 6% of women and 2.5% of men
• Classification a. Hashimoto disease: Most common
hypothyroid disorder in areas with iodine sufficiency i.
Autoimmune-induced thyroid injury resulting in decreased
thyroid secretion ii. Disproportionately affects women
• b. Iatrogenic: Thyroid resection or radioiodine ablative
therapy for hyperthyroidism
• c. Iodine deficiency most common cause worldwide
• d. Secondary causes.I Pituitary insufficiency (failure to
produce adequate TSH secretion, called by some a central
or secondary hypothyroidism) ii. Drug induced (e.g.,
amiodarone, lithium)
Hashimoto's disease
• Hashimoto's disease, an autoimmune
disorder, caused by destruction of thyroid
cells by circulating thyroid antibodies
produces an underlying defect or block in the
intrathyroidal, organo-binding of iodide.
Symptoms
• General: weakness, tiredness, lethargy, fatigue
• Cold intolerance
• Headache
• Loss of taste/smell .
• Deafness
• Hoarseness
• Modest weight gain Muscle cramps, aches, pains
• Dyspnea
• Slow speech
• Constipation
• Menorrhagia
Diagnosis
• Low free T4 serum concentrations b. Elevated
TSH concentrations, typically seen as first
laboratory abnormality, usually greater than
10 mIU/L (normal or low if central
hypothyroidism is the cause
Treatment of Hypothyroidism
• Levothyroxine (L-thyroxine) is the preferred thyroid
replacement preparation.
• ) Initial (1) In otherwise healthy adults, 1.6 mcg/kg (use ideal
body weight) per day (2) In patients age 50–60, consider 50
mcg/day. (3) In those with existing cardiovascular disease,
consider 12.5–25 mcg/day.
• Adverse effects (a) Hyperthyroidism (b) Cardiac
abnormalities (tachyarrhythmias, angina, myocardial
infarction) (c) Linked to risk of fractures (usually at higher
dosages or over-supplementation) v. Efficacy: If levothyroxine
is properly dosed, most patients will maintain TSH and free T
• In myxedema coma, intravenous (IV) therapy
with large initial doses of L-thyroxine (e.g., 400
mcg) is necessary to increase the active free
hormone level by saturating the empty
thyroid-binding sites and to prevent the 60%
to 70% mortality rate.
• In subclinical hypothyroidism, it is
controversial whether T4 replacement therapy
is benefi
• Once a euthyroid state is attained, laboratory
tests can be monitored every 3 to 6 months for
the first year and then yearly thereafter.
• Medications that interfere with T4 absorption
(e.g., iron, aluminum-containing products,
some calcium preparations, cholesterol resin
and phosphate binders, raloxifene) should not
be
coadministered with T4.
HYPERTHYROIDISM
• Classification
• a. Toxic diffuse goiter (Graves disease): Most common
hyperthyroid disorder i. Autoimmune disorder ii. Thyroid-
stimulating antibodies directed at thyrotropin receptors mimic
TSH and stimulate triiodothyronine (T3 ) and T4 production.
• b. Pituitary adenomas: Produce excessive TSH secretion that
does not respond to normal T3 negative feedback
• c. Toxic adenoma: Nodule in thyroid, autonomous of pituitary,
and TSH
• d. Toxic multinodular goiter (Plummer disease): Several
autonomous follicles that, if large enough, cause excessive
thyroid hormone secretion
• Drug induced (e.g., excessive exogenous
thyroid hormone dosages, amiodarone
therapy.
• . Diagnosis
• a. Elevated free T4 serum concentrations
• b. Suppressed TSH concentration
Clinical presentation
• a. Weight loss or increased appetite
• b. Lid lag c
• . Heat intolerance
• d. Goiter
• e. Fine hair
• f. Heart palpitations or tachycardia g. Nervousness,
anxiety, insomnia h
• . Menstrual disturbances (lighter or more infrequent
menstruation, amenorrhea) caused by hypermetabolism
of estrogen i. Sweating or warm, moist ski
Therapy goals
• a. Minimize or eliminate symptoms, improve
quality of life b. Minimize long-term damage
to organs (heart disease, arrhythmias, sudden
cardiac death, bone demineralization, and
fractures)
• Thioureas (i.e., propylthiouracil, methimazole) i.
Mechanism of action: Inhibits iodination and synthesis
of thyroid hormones; propylthiouracil can block T4 /T3
conversion in the periphery as well at high doses ii.
Dosing (a) Propylthiouracil (1) Initial: 50–150 mg by
mouth three times daily (2) Once euthyroid, can
reduce to 50 mg two or three times daily (3)
Recommended over methimazole in the first trimester
of pregnancy because of the risk of embryopathy; can
change to methimazole in second trimester
• Methimazole (1) Preferred agent for Graves
disease according to the American Association
of Clinical Endocrinologists (AACE) and the
American Thyroid Association for most
patients (2) Initial: 10–30 mg by mouth once
daily (use higher dose in those with higher
baseline free T4 concentrations) (3) Once
euthyroid, may reduce to 5–10 mg/day
Adverse effects
• Hepatotoxicity risk (boxed warning for PTU): Consider
baseline liver function tests Routine evaluation of liver
function while receiving antithyroid agents has not been
shown to prevent severe hepatotoxicity.
• (b) Rash (, lupus-like symptoms
• (d) Fever
• (e) Agranulocytosis early in therapy (usually within 3
months): Guidelines recommend a baseline complete
blood cell count; no routine monitoring recommended.
Can repeat if patient becomes febrile or develops
pharyng
• Nonselective β-blockers (primarily propranolol;
sometimes nadolol)
• . Mechanism of action: Blocks many
hyperthyroidism manifestations mediated by β-
adrenergic receptors; also may block (less active)
T4 conversion to (more active) T3 when used at
high doses
• ii. Propranolol dosing (a) Initial: 20–40 mg by
mouth three or four times daily (b) Maximal: 240–
480 mg/day.
• Iodines and iodides (e.g., Lugol’s solution, saturated solution of
potassium iodide) i. Mechanism of action: Inhibits the release
of stored thyroid hormone. Minimal effect on hormone
synthesis. Helps decrease vascularity and size of gland before
surgery ii. Dosing (a) Lugol’s solution (6.3–8 mg of iodide per
drop) (b) Saturated solution of potassium iodide (38–50 mg of
iodide per drop) (c) Potassium iodide tablets: 130-mg tablets
contain 100 mg of iodide. (d) Usual daily dose: 120–400 mg
mixed with juice or water, split three times daily iii. Adverse
effects (a) Hypersensitivity (b) Metallic taste (c) Soreness or
burning in mouth or tongue (d) Do not use in the days before
ablative iodine therapy (may reduce uptake of radioactive
You might also like
- The Global Pharmaceutical IndustryDocument28 pagesThe Global Pharmaceutical IndustryOmolarge100% (1)
- Anti Inflammation Cook Book PDFDocument69 pagesAnti Inflammation Cook Book PDFinmatxetxuNo ratings yet
- An Ethnobotanical Perspective On AyahuascaDocument7 pagesAn Ethnobotanical Perspective On AyahuascaLucho DiazNo ratings yet
- Seminar ActivityDocument2 pagesSeminar ActivityStephen YorNo ratings yet
- Lepra ReactionDocument24 pagesLepra ReactionSWAPAN KUMAR SARKAR100% (2)
- The Feasibility of Using Hibiscus RosaDocument20 pagesThe Feasibility of Using Hibiscus RosaChristianjames DiamanteNo ratings yet
- Duck RaisingDocument12 pagesDuck RaisingRosel Gonzalo-Aquino60% (10)
- Lect 5Document26 pagesLect 5eslambasuony98No ratings yet
- Therapeutics: Thyroid DisordersDocument24 pagesTherapeutics: Thyroid DisordersSharas FarhadNo ratings yet
- Thyroid DisorderDocument60 pagesThyroid DisorderThe AbyssinicansNo ratings yet
- PATIENT WITH ENDOCRINE DYSFUNCTION THYROID .pptx1Document52 pagesPATIENT WITH ENDOCRINE DYSFUNCTION THYROID .pptx1sembakarani thevagumaranNo ratings yet
- Lec#15+16 Thyroid DisordersDocument82 pagesLec#15+16 Thyroid DisordersKhaldoun AlmomaniNo ratings yet
- 15 2020 Thyroid - Antithyroid Drugs - SlidesDocument26 pages15 2020 Thyroid - Antithyroid Drugs - Slidesالبيان البيانNo ratings yet
- Thyroid DisordersDocument34 pagesThyroid DisordersAbdulhameed Mohamed100% (1)
- Thyroid and Antithyroid Agent-VDocument60 pagesThyroid and Antithyroid Agent-VVine100% (1)
- Drug Management of Thyroid DiseaseDocument22 pagesDrug Management of Thyroid DiseaseHassan.shehri100% (6)
- Hyperthyroid Is MDocument38 pagesHyperthyroid Is MMellanie B. VictoriaNo ratings yet
- Thyroid Hormones & DrugsDocument51 pagesThyroid Hormones & DrugsSUTHANNo ratings yet
- Hyperthyroidism: by TemesgenDocument33 pagesHyperthyroidism: by TemesgenTemesgen100% (2)
- Thyroid Disorders: Aromokunola Boluwaji Peter (B.Pharm, Ife)Document18 pagesThyroid Disorders: Aromokunola Boluwaji Peter (B.Pharm, Ife)boluwaji aromokunolaNo ratings yet
- Thyroid DisordersDocument55 pagesThyroid DisordersNsubuga Ivan100% (1)
- Lesson 6 Thyroid and Antithyroid DrugsDocument28 pagesLesson 6 Thyroid and Antithyroid DrugstheintrovNo ratings yet
- Thyroid and Antithyroid Drugs... HaftomDocument40 pagesThyroid and Antithyroid Drugs... Haftomkaleab AlemayehuNo ratings yet
- Drug Induced Thyroid ProblemsDocument33 pagesDrug Induced Thyroid ProblemsJoisy AloorNo ratings yet
- 2 TSHDocument7 pages2 TSHNashat SaadiNo ratings yet
- Internal Med. EndoDocument35 pagesInternal Med. EndoEdwin OkonNo ratings yet
- Endocrinology L8: Introduction To Thyroid Disease and HyperthyroidismDocument30 pagesEndocrinology L8: Introduction To Thyroid Disease and HyperthyroidismSecret ManNo ratings yet
- 02 Lecture 10 Anti-Thyroid Drugs (DR Thatcher Pod Pharm 2022)Document36 pages02 Lecture 10 Anti-Thyroid Drugs (DR Thatcher Pod Pharm 2022)sahilaminNo ratings yet
- Thyroid DisordersDocument62 pagesThyroid Disorderslibentadesse57No ratings yet
- Thyroid and Parathyroid GlandsDocument133 pagesThyroid and Parathyroid GlandsmunafalmahdiNo ratings yet
- Interpretation of Laboratory Thyroid Function Tests: The "Hidden" Health ProblemDocument38 pagesInterpretation of Laboratory Thyroid Function Tests: The "Hidden" Health Problemalanoud.877No ratings yet
- Thyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrDocument57 pagesThyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrpurnaNo ratings yet
- Thyroid PresentationDocument38 pagesThyroid Presentation천사자No ratings yet
- Thyroid Gland L-Thyroxine (T4) Vs Triiodothyronine (T3) : Follicular CellsDocument7 pagesThyroid Gland L-Thyroxine (T4) Vs Triiodothyronine (T3) : Follicular CellsPrincess Noreen SavellanoNo ratings yet
- Thyroid and ParathyroidDocument29 pagesThyroid and Parathyroidpranutan739No ratings yet
- Management and Medications in Thyroid Strom and Myxoedema ComaDocument41 pagesManagement and Medications in Thyroid Strom and Myxoedema ComaBhavesh kunvarNo ratings yet
- Thyroid Gland Diseases in ChildrenDocument29 pagesThyroid Gland Diseases in ChildrenadinayNo ratings yet
- Hyperthyroidism and HypothyroidismDocument59 pagesHyperthyroidism and HypothyroidismJun AmaroNo ratings yet
- Hypothyroidism: Regulation of Thyroid HormoneDocument4 pagesHypothyroidism: Regulation of Thyroid HormoneAmer Abdulla SachitNo ratings yet
- Module I 2 - Thyroid Gland DisordersDocument43 pagesModule I 2 - Thyroid Gland Disordersaysha jasim100% (1)
- Theme 2: Thyroid Diseases: Study GoalsDocument9 pagesTheme 2: Thyroid Diseases: Study GoalsOlesyaNo ratings yet
- Sophie Keyte Bvms (Hons) Mvetmed (Dist) Fhea Dipacvim Mrcvs Sophie - Keyte@Bristol - Ac.UkDocument24 pagesSophie Keyte Bvms (Hons) Mvetmed (Dist) Fhea Dipacvim Mrcvs Sophie - Keyte@Bristol - Ac.UkStefana UrsuNo ratings yet
- Makalah Case 2 Grave DiseaseDocument8 pagesMakalah Case 2 Grave Diseasesalsabila firdausiaNo ratings yet
- Thyroid CrisisDocument34 pagesThyroid CrisisRidyah Ning TyasNo ratings yet
- Thyroid StormDocument3 pagesThyroid StormSuprit SnNo ratings yet
- Trachea: Thyroid Agents Thyroid Gland Is Located in The Middle of The Neck and SurroundsDocument10 pagesTrachea: Thyroid Agents Thyroid Gland Is Located in The Middle of The Neck and SurroundsMIR SARTAJNo ratings yet
- Thyroid & Anti-Thyroid DrugsDocument59 pagesThyroid & Anti-Thyroid DrugsNiranjanNo ratings yet
- Diagnosis and Management of Hyperthyroidism, A Rational ApproachDocument35 pagesDiagnosis and Management of Hyperthyroidism, A Rational ApproachANCHAL SHARMANo ratings yet
- Thyroiddisease 190216062020Document42 pagesThyroiddisease 190216062020Manikandan Vp100% (1)
- THYROTOXICOSISDocument20 pagesTHYROTOXICOSISfig8fashion1No ratings yet
- Thyroid PharmacologyDocument26 pagesThyroid PharmacologyVikrant GholapNo ratings yet
- 3 ThyroidDocument60 pages3 ThyroidyeabsraNo ratings yet
- ThyrotoxicosisDocument105 pagesThyrotoxicosisAli Murtaza Abbas100% (1)
- Thyroid Emergencies-Dr. AM IyagbaDocument13 pagesThyroid Emergencies-Dr. AM IyagbaDr. Amb. Monday ZaccheausNo ratings yet
- Hypothyroid in Pregnancy Andi CakraDocument32 pagesHypothyroid in Pregnancy Andi CakraCakraEkky100% (1)
- Thiroid DisordersDocument11 pagesThiroid Disordersرعد النميريNo ratings yet
- Thyroid Disorders: Dr. Lubna DwerijDocument52 pagesThyroid Disorders: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Thyroid and Parathyroid AgentsDocument28 pagesThyroid and Parathyroid AgentsMary Faith Kiat-ongNo ratings yet
- Hypothyroidism 2Document50 pagesHypothyroidism 2Ziaur rabbi sakilNo ratings yet
- Thyroid Gland An Diseases of Thyroid D Gland: Omc LectureDocument59 pagesThyroid Gland An Diseases of Thyroid D Gland: Omc LectureEdward MakemboNo ratings yet
- Mbs127 Slide Hyperthyroidism 1Document46 pagesMbs127 Slide Hyperthyroidism 1revita262No ratings yet
- Hypo Thyroid Is MDocument27 pagesHypo Thyroid Is Mdhiraj parmarNo ratings yet
- Hyperthyroidism: A Practical Approach To Diagnosis and ManagementDocument70 pagesHyperthyroidism: A Practical Approach To Diagnosis and ManagementMutiara Manuella TambaNo ratings yet
- Disorders of The Thyroid GandDocument167 pagesDisorders of The Thyroid GandWendy Figueroa MijaresNo ratings yet
- Askep GGN ThyroidDocument26 pagesAskep GGN ThyroidTsaalits MuharrorohNo ratings yet
- Hyperthyroidism, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandHyperthyroidism, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 2 out of 5 stars2/5 (2)
- Case Scenerio GlomerulonephritisDocument4 pagesCase Scenerio GlomerulonephritisEllen AngelNo ratings yet
- Nursing Care PlanDocument10 pagesNursing Care PlanIsabelle Madrid100% (1)
- 2 ChapterDocument16 pages2 ChapterAjoy SharmaNo ratings yet
- Review Article: Cluster Headache-Acute and Prophylactic TherapyDocument24 pagesReview Article: Cluster Headache-Acute and Prophylactic TherapyPurna Adi PutraNo ratings yet
- FCPHM (SA) Regulations 23-1-2017Document23 pagesFCPHM (SA) Regulations 23-1-2017matentenNo ratings yet
- GINA 2016 Teaching Slide SetDocument171 pagesGINA 2016 Teaching Slide SetAndra DaNo ratings yet
- HahayysDocument30 pagesHahayys2BGrp3Plaza, Anna MaeNo ratings yet
- Benign Prostatic Hyperplasia (BPH) : Hyperplasia: Diagnosis and Treatment (1994) Was The Starting Point ForDocument14 pagesBenign Prostatic Hyperplasia (BPH) : Hyperplasia: Diagnosis and Treatment (1994) Was The Starting Point ForAnemiaHemolyticNo ratings yet
- College of Nursing: Pharmacological ManagementDocument2 pagesCollege of Nursing: Pharmacological ManagementJOHN PEARL FERNANDEZNo ratings yet
- Swarnaprashana PDFDocument9 pagesSwarnaprashana PDFAnuroop MondruNo ratings yet
- Seminar 5 - Traumatic Dislocation and Common Soft Tissue Injury - 2Document149 pagesSeminar 5 - Traumatic Dislocation and Common Soft Tissue Injury - 2Star CruiseNo ratings yet
- GENESISDocument4 pagesGENESISmonirul islam shohanNo ratings yet
- Corticosteroids 24613Document33 pagesCorticosteroids 24613NOorulain HyderNo ratings yet
- The Homoeopathic Concise Repertory PDFDocument28 pagesThe Homoeopathic Concise Repertory PDFShrutika MatteNo ratings yet
- I'll See You Tomorrow: Ayza Bolanos Autobiographical Reading and Writing Brett Williams 09 December 2015Document30 pagesI'll See You Tomorrow: Ayza Bolanos Autobiographical Reading and Writing Brett Williams 09 December 2015api-357172052No ratings yet
- Respondant MemorialDocument19 pagesRespondant MemorialSunayana Basu0% (1)
- Pulmonary Embolism: Presented By: Miss. M.K.Kaku Nursing TutorDocument9 pagesPulmonary Embolism: Presented By: Miss. M.K.Kaku Nursing TutorKaku ManishaNo ratings yet
- UrinalysisDocument172 pagesUrinalysisRonelene GatoNo ratings yet
- Pharmacokinetics: of OphthalmicDocument4 pagesPharmacokinetics: of OphthalmicWina Siska Purnama BurmanNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaSalwiyadiNo ratings yet
- CAMBRA: Best Practices in Dental Caries Management: 3 CE CreditsDocument8 pagesCAMBRA: Best Practices in Dental Caries Management: 3 CE CreditsDino MainoNo ratings yet
- Touch For Socioemotional and Physical Well-BeingDocument17 pagesTouch For Socioemotional and Physical Well-BeingcarlyNo ratings yet
- 10.1016/j.ymgme.2016.11.045: Abstracts / Molecular Genetics and Metabolism 120 (2016) S17 - S145 S29Document2 pages10.1016/j.ymgme.2016.11.045: Abstracts / Molecular Genetics and Metabolism 120 (2016) S17 - S145 S29Larisa IliescuNo ratings yet