Professional Documents
Culture Documents
Thyroiditis
Thyroiditis
Uploaded by
marselia230 ratings0% found this document useful (0 votes)
5 views12 pagesOriginal Title
Thyroiditis (1)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
5 views12 pagesThyroiditis
Thyroiditis
Uploaded by
marselia23Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 12
Subacute Thyroiditis
• Subacute thyroiditis (De Quervain's thyroiditis or granulomatous
thyroiditis) is an acute inflammatory disorder of the thyroid
gland most likely due to viral infection.
• A number of viruses, including coxsackievirus, and
adenoviruses, have been implicated, either by finding the virus
in biopsy specimens taken from the gland or by demonstration
of rising titers of viral antibodies in the blood during the course
of the infection.
• Pathologic examination reveals moderate thyroid enlargement
and a mild inflammatory reaction involving the capsule.
• Histologic features include destruction of thyroid parenchyma
and the presence of many large phagocytic cells, including giant
cells. Subacute thyroiditis is more common in the summer
months, in women, and in individuals who are HLA-Bw35
positive.
Clinical Signs
• Subacute thyroiditis usually presents with fever, malaise, and
soreness in the anterior neck, which may extend up to the
angle of the jaw or toward the ear lobes on one or both sides
of the neck.
• Initially, the patient may have symptoms of hyperthyroidism,
with palpitations, nervousness, and sweats. There is no
ophthalmopathy.
• On physical examination, the gland is exquisitely tender, so
that the patient objects to pressure on it. There are no signs of
local redness or heat suggestive of abscess formation. Clinical
signs of thyrotoxicosis, including tachycardia, tremor, and
hyperreflexia, may be present.
Laboratory findings
• Initially, FT4 and T3 are elevated, whereas serum TSH
and RAIU are extremely low. Because the thyroid
hormone levels in the blood are a reflection of
leakage of glandular hormonal stores, serum FT4
levels are elevated disproportionately to serum T3
levels.
• Thyroid autoantibodies are usually not detectable in
serum. As the disease progresses, FT4 and T3 drops,
TSH rises, and symptoms of hypothyroidism are
noted.
Treatment
• In many cases, only symptomatic treatment is necessary (aspirin
or other nonsteroidal anti-inflammatory drugs). In severe cases
or in patients who do not respond to nonsteroidal agents, a
glucocorticoid such as prednisone, 20 mg three times daily for
7–10 days, may be necessary to reduce the inflammation.
• Beta-adrenergic blocking agents can be employed during the
hyperthyroid phase to treat bothersome symptoms of
hyperthyroidism.
• T4, 0.1–0.15 mg once daily, may be indicated during the
hypothyroid phase of the illness if hypothyroid symptoms are
present. T4 therapy may also prevent exacerbations of
inflammation due to elevated TSH levels.
Chronic Thyroiditis
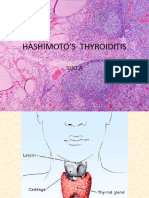
Hashimoto’s thyroidit
• Chronic thyroiditis (Hashimoto's thyroiditis, lymphocytic
thyroiditis) is the most common cause of hypothyroidism and
goiter. It is certainly the major cause of goiter in children and
young adults and is the cause of "idiopathic myxedema," which
represents an end stage of Hashimoto's thyroiditis, with total
destruction of the gland.
• Riedel's thyroiditis may be a very rare variant of Hashimoto's
thyroiditis, with extensive fibrosis extending outside the gland and
involving overlying muscle and surrounding tissues. Riedel's
struma presents as a stony-hard mass that must be differentiated
from thyroid cancer. It is also associated with fibrosis in other
parts of the body including the mediastinum and retroperitoneum
Etiology & Pathogenesis
• Hashimoto's thyroiditis is thought to be an immunologic
disorder in which lymphocytes become sensitized to
thyroidal antigens and autoantibodies are formed that
react with these antigens (see Thyroid Autoimmunity,
above). In Hashimoto's thyroiditis, the three most
important thyroid autoantibodies are thyroglobulin
antibody, TPO Ab, and TSH-R blocking antibody. During
the early phases of Hashimoto's thyroiditis,
thyroglobulin antibody is markedly elevated, and TPO Ab
is slightly elevated. Later, thyroglobulin antibody may
disappear, but TPO Ab is present for many years
Symptomps and Signs
• Hashimoto's thyroiditis usually presents with
goiter in a patient who is euthyroid or has mild
hypothyroidism. The female: male sex
distribution is about 4:1. The process is
painless, and the patient may be unaware of
the goiter unless it becomes very large. Older
patients may present with severe
hypothyroidism with only a small, firm
atrophic thyroid gland (idiopathic myxedema).
Laboratory findings
• Circulating thyroid hormone levels are usually
normal or low, and if low, TSH will be elevated.
• The most striking laboratory finding is the high
titer of autoantibodies to thyroidal antigens in
the serum. Serum tests for either
thyroglobulin antibody or TPO Ab are positive
in most patients with Hashimoto's thyroiditis.
Complications
• The major complication of Hashimoto's
thyroiditis is progressive hypothyroidism. Most
patients with Hashimoto's thyroiditis initially
have a small goiter and "subclinical
hypothyroidism," which is defined as normal
serum levels of FT4 and T3, but mildly elevated
serum TSH levels.
Complications
• Rarely, a patient with Hashimoto's thyroiditis
may develop lymphoma of the thyroid gland.
Although the etiology of thyroid lymphoma is
unknown, Hashimoto's thyroiditis is a definite
risk factor.
• Thyroid lymphoma is characterized by rapid
growth of the gland despite continued T4
therapy; the diagnosis of lymphoma must be
made by surgical biopsy.
Treatment
• The indications for treatment of Hashimoto's thyroiditis are
goiter or hypothyroidism; a patient with a positive thyroid
antibody test alone does not require therapy.
• Surgery is rarely indicated for Hashimoto's thyroiditis but
occasionally is performed if a goiter does not regress and
continues to cause compressive symptoms.
• The treatment of subclinical hypothyroidism is a matter of
debate but is often instituted because of mild symptoms;
positive antithyroid antibody titers, which predicts a high
chance of progression to hypothyroidism over time.
• Sufficient T4 is given to normalize TSH and allow regression of
the goiter.
You might also like
- D&D Name ListDocument21 pagesD&D Name ListFun McBunsNo ratings yet
- A Case Presentation On Multinodular GoitreDocument27 pagesA Case Presentation On Multinodular Goitrecnsatish86% (7)
- Living and Nonliving Things PDFDocument2 pagesLiving and Nonliving Things PDFRelingado GraceNo ratings yet
- Thyroid StormDocument11 pagesThyroid StormAndrew UtamaNo ratings yet
- Thyroid Disorders in PregnancyDocument46 pagesThyroid Disorders in PregnancyMara Medina - BorleoNo ratings yet
- Send in The Clones - A Cultural Study of The Tribute Band (Studies in Popular Music) by Georgina GregoryDocument183 pagesSend in The Clones - A Cultural Study of The Tribute Band (Studies in Popular Music) by Georgina GregoryMatias Sandes100% (1)
- HARP Character Sheet PDFDocument4 pagesHARP Character Sheet PDFBarbarianYNo ratings yet
- Gerald Martin About CASDocument16 pagesGerald Martin About CASJuanpklllllllcamargoNo ratings yet
- ThyroidDocument31 pagesThyroidAmmar HattemNo ratings yet
- Clinical Science HashimotoDocument36 pagesClinical Science HashimotoImartaNo ratings yet
- ThyrotoxicosisDocument15 pagesThyrotoxicosischrysandre100% (1)
- Hyperthyroidism and HypothyroidismDocument59 pagesHyperthyroidism and HypothyroidismJun AmaroNo ratings yet
- Endocrine System - Internal MedicineDocument39 pagesEndocrine System - Internal MedicineDaanishNo ratings yet
- Thyrotoxicosis Seb 4Document35 pagesThyrotoxicosis Seb 4Bersisa chalchisaNo ratings yet
- Hashimoto and Grave DiseaseDocument9 pagesHashimoto and Grave DiseaseNadia ElaizaNo ratings yet
- Hashimoto's ThyroiditisDocument18 pagesHashimoto's Thyroiditisabdulrahmanbelewa96No ratings yet
- Hypothyroidism: Prepared By: Angel Shwaihat Enas Khamaiseh Supervised By: Dr. Khalil Al SoutariDocument33 pagesHypothyroidism: Prepared By: Angel Shwaihat Enas Khamaiseh Supervised By: Dr. Khalil Al Soutariraed faisalNo ratings yet
- Grave's Disease EDITEDDocument39 pagesGrave's Disease EDITEDLadipo Temitope AyodejiNo ratings yet
- Thyroiditis: o o o o o oDocument10 pagesThyroiditis: o o o o o omagisasamundoNo ratings yet
- Tiroiditis Subakut PDFDocument8 pagesTiroiditis Subakut PDFAdeh MahardikaNo ratings yet
- ThyrotoxicosisDocument105 pagesThyrotoxicosisAli Murtaza Abbas100% (1)
- Thyroid Function TestDocument28 pagesThyroid Function TestDhinesh Muthusamy100% (1)
- Thyroid DiseaseDocument72 pagesThyroid Diseaseluna zeidNo ratings yet
- Internal Med. EndoDocument35 pagesInternal Med. EndoEdwin OkonNo ratings yet
- Thyroid Storm May Be The Initial Presentation Of: Thyrotoxicosis in Undiagnosed Children, Particularly in NeonatesDocument8 pagesThyroid Storm May Be The Initial Presentation Of: Thyrotoxicosis in Undiagnosed Children, Particularly in NeonatesLolla MorsiNo ratings yet
- Thyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrDocument57 pagesThyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrpurnaNo ratings yet
- Thyroid Function TestDocument21 pagesThyroid Function TestPat JacintoNo ratings yet
- HypertyroidismDocument46 pagesHypertyroidismenriNo ratings yet
- Thyroid Gland Diseases in ChildrenDocument29 pagesThyroid Gland Diseases in ChildrenadinayNo ratings yet
- HPERTHYROIDISMDocument4 pagesHPERTHYROIDISMSalwa KaramanNo ratings yet
- Hashimotosthyroiditis 170825171347Document25 pagesHashimotosthyroiditis 170825171347abdulrahmanbelewa96No ratings yet
- Lecture (1). THDocument34 pagesLecture (1). THyoussef hossamNo ratings yet
- Lec#15+16 Thyroid DisordersDocument82 pagesLec#15+16 Thyroid DisordersKhaldoun AlmomaniNo ratings yet
- Hypo Thyroid Is MDocument27 pagesHypo Thyroid Is Mdhiraj parmarNo ratings yet
- THYROTOXICOSISDocument20 pagesTHYROTOXICOSISfig8fashion1No ratings yet
- Background: Excessive Release of Thyroid Hormones (THS) Hypertension Congestive Heart FailureDocument8 pagesBackground: Excessive Release of Thyroid Hormones (THS) Hypertension Congestive Heart FailureIkmal HazliNo ratings yet
- Graves' Disease: Bella I. Putri 16-025Document29 pagesGraves' Disease: Bella I. Putri 16-025anon_414347743No ratings yet
- Hyperthyroidism .... 2Document13 pagesHyperthyroidism .... 2guptaavni0000No ratings yet
- Thyroid Disorders Chapter 20 Hal 176 Dipiro Edisi 9Document7 pagesThyroid Disorders Chapter 20 Hal 176 Dipiro Edisi 9Nila LutfiNo ratings yet
- Thyroid GlandDocument59 pagesThyroid Glandbessan alfqeatNo ratings yet
- ThyroidDocument96 pagesThyroidNimer Abdelhadi AliNo ratings yet
- Kuliah HyperthyroidDocument18 pagesKuliah HyperthyroidFreddyNo ratings yet
- Main Thyroid DiseasesDocument25 pagesMain Thyroid DiseasesPurnima ChoudhuryNo ratings yet
- Types: HyperthyroidismDocument12 pagesTypes: HyperthyroidismArunNo ratings yet
- Thyroid DisordersDocument22 pagesThyroid DisordersNimer Abdelhadi AliNo ratings yet
- Bening Disease of Thyroid GlandDocument85 pagesBening Disease of Thyroid GlandKarishma MishraNo ratings yet
- Etiology-Hypothyroidism: Chronic Autoimmune ThyroiditisDocument4 pagesEtiology-Hypothyroidism: Chronic Autoimmune ThyroiditisNungky KusumaNo ratings yet
- Hypothyroidism Evaluation of Thyroid FunctionDocument9 pagesHypothyroidism Evaluation of Thyroid FunctionJJ hidden objectNo ratings yet
- HipotiroidismDocument62 pagesHipotiroidismMuhammad Nur DelaphanEnamNo ratings yet
- #30 Thyroid and Thyroid TestingDocument25 pages#30 Thyroid and Thyroid TestingasclswisconsinNo ratings yet
- EndocrinologyDocument39 pagesEndocrinologySoumyajit Ray ChaudhuriNo ratings yet
- Hyperthyroidism-Dr. A.M IyagbaDocument42 pagesHyperthyroidism-Dr. A.M IyagbaDr. Amb. Monday ZaccheausNo ratings yet
- Therapeutics: Thyroid DisordersDocument24 pagesTherapeutics: Thyroid DisordersSharas FarhadNo ratings yet
- Thyroiditis: Uaepong Limpapanasit 23/5/54Document36 pagesThyroiditis: Uaepong Limpapanasit 23/5/54Rapid MedicineNo ratings yet
- ThyrotoxicosisDocument42 pagesThyrotoxicosisShaw Khan100% (7)
- Wo Week 4 (Hyperthyroidism)Document12 pagesWo Week 4 (Hyperthyroidism)Theddyon BhenlieNo ratings yet
- Nodul Tiroid Tiroiditis CA Tiroid-2Document61 pagesNodul Tiroid Tiroiditis CA Tiroid-2iraNo ratings yet
- Interpretation of Laboratory Thyroid Function Tests: The "Hidden" Health ProblemDocument38 pagesInterpretation of Laboratory Thyroid Function Tests: The "Hidden" Health Problemalanoud.877No ratings yet
- Disorders of The Thyroid GandDocument167 pagesDisorders of The Thyroid GandWendy Figueroa MijaresNo ratings yet
- Subacute, Silent, and Postpartum Thyroiditis 2012Document11 pagesSubacute, Silent, and Postpartum Thyroiditis 2012YoaNnita GoMezNo ratings yet
- Hperthyroidism 1Document4 pagesHperthyroidism 1Salwa KaramanNo ratings yet
- Hyperthyroidism Vs HypothyroidismDocument12 pagesHyperthyroidism Vs Hypothyroidismazizan hannyNo ratings yet
- Hyperthyroidism and Thyrotoxicosis: Practice EssentialsDocument39 pagesHyperthyroidism and Thyrotoxicosis: Practice Essentialssyl viNo ratings yet
- Benign Thyroid DiseasesDocument8 pagesBenign Thyroid DiseasesBkas GrgNo ratings yet
- Hashimoto Thyroiditis, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandHashimoto Thyroiditis, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Haddad v. Indiana Pacers Et Al - Document No. 82Document17 pagesHaddad v. Indiana Pacers Et Al - Document No. 82Justia.com100% (1)
- CIS534 Week #10 Term Paper Designing A Secure NetworkDocument8 pagesCIS534 Week #10 Term Paper Designing A Secure NetworkLouis DeWeaver IIINo ratings yet
- BS en 00408-2010 PDFDocument40 pagesBS en 00408-2010 PDFShan Sandaruwan Abeywardene100% (2)
- Error Code Analysis Flow (Mechanism) : 10300 IP Sensor Logical InconsistencyDocument1 pageError Code Analysis Flow (Mechanism) : 10300 IP Sensor Logical InconsistencyElvira RodNo ratings yet
- The Field of Engineering ManagementDocument15 pagesThe Field of Engineering ManagementBelle SolaceNo ratings yet
- Sample Size CalculationDocument2 pagesSample Size CalculationAljon AgustinNo ratings yet
- 4987-2007 Network of RaingaugeDocument7 pages4987-2007 Network of RaingaugeIshwari TiwariNo ratings yet
- CV RohitDocument4 pagesCV RohitRohit GandhiNo ratings yet
- Definition of Good GovernanceDocument3 pagesDefinition of Good GovernanceHaziq KhanNo ratings yet
- JCR 2019 PDFDocument385 pagesJCR 2019 PDFpervezkanjuNo ratings yet
- Stalwar DX LiteratureDocument2 pagesStalwar DX LiteratureAnonymous cbXdPkXoNo ratings yet
- Balancing Pool FOIPSDocument330 pagesBalancing Pool FOIPSTeamWildroseNo ratings yet
- Product Category LifecyclesDocument13 pagesProduct Category LifecyclesAdam Andrew OngNo ratings yet
- Biochemistry Lab ManualDocument11 pagesBiochemistry Lab ManualShela MalubagNo ratings yet
- Rabagia - MatenTertiary Tectonic and Sedimentological Evolution of The South Carpathians Foredeep: Tectonic Versus Eustatic Controlco (1999)Document22 pagesRabagia - MatenTertiary Tectonic and Sedimentological Evolution of The South Carpathians Foredeep: Tectonic Versus Eustatic Controlco (1999)Lex AlexaNo ratings yet
- R. Molski, Polish Antitrust Law in Its Fight Against Cartels - Awaiting A BreakthroughDocument28 pagesR. Molski, Polish Antitrust Law in Its Fight Against Cartels - Awaiting A Breakthroughcsair1No ratings yet
- Discrete Prob Practice QsDocument8 pagesDiscrete Prob Practice QsAitzul SchkohNo ratings yet
- FFT Tutorial: 1 Getting To Know The FFTDocument6 pagesFFT Tutorial: 1 Getting To Know The FFTDavid NasaelNo ratings yet
- A Study On Consumer Behaviour in Real Estate SectorDocument94 pagesA Study On Consumer Behaviour in Real Estate SectorNadeem khan100% (2)
- Self Incompatibility: Dr. L.K.GangwarDocument38 pagesSelf Incompatibility: Dr. L.K.GangwarSiddhant Singh100% (1)
- Francisco QuisumbingDocument1 pageFrancisco QuisumbingILubo AkNo ratings yet
- MTB-Lesson 3Document4 pagesMTB-Lesson 3Clavillas GrachelleNo ratings yet
- Theories of MotivationDocument9 pagesTheories of MotivationJeffrey ManzanoNo ratings yet
- REINVENTING EDEN. The Fate of Nature in Western Culture. Carolyn Merchant, Second Edition (Updated With A New Foreword and Afterword), 2013Document334 pagesREINVENTING EDEN. The Fate of Nature in Western Culture. Carolyn Merchant, Second Edition (Updated With A New Foreword and Afterword), 2013Francis RijnaNo ratings yet